Abstract
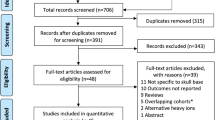
The management of base of skull (BS) chordomas is a neurosurgical conundrum owing to their close proximity to the critical neurovascular structures. Surgical resection is the gold standard treatment followed by adjuvant radiotherapy which includes photon therapy, proton beam therapy (PBT), gamma knife radiosurgery, etc. PBT has become an unparalleled therapeutic modality in the management of BS chordomas. The aim of this systematic review was to assess the outcomes in BS chordoma patients who received PBT as a primary or adjuvant therapy. PubMed and Cochrane databases were screened till May 2022. Following the PRISMA guidelines, studies were reviewed thoroughly, and the data of the included study was extracted. Statistical analysis was performed using the SAS 9.4 with P value < .05 considered as significant. Sixteen studies with 752 patients were included. The majority of the patients were adults (> 18 years) with a male:female ratio of 1.2. The most common clinical features were cranial nerve (3rd, 6th, or 12th) palsy and hearing impairment. Ninety-five percent of the patients underwent surgical resection before PBT. The mean PBT dose received was 74.02 cGe (cobalt gray equivalent). Eighty percent of the patients showed a positive response to the therapy defined in terms of tumor regression. Five-year local control (LC), overall survival (OS), and progression-free survival (PFS) were calculated as 76.6%, 79.6%, and 89%, respectively. Statistical analysis revealed none of the factors had any significant association with 5-year LC. PBT is a growing therapeutic technique that has revolutionized the treatment of BS chordomas.


Similar content being viewed by others
Data Availability
Not applicable.
References
McMaster ML, Goldstein AM, Bromley CM, Ishibe N, Parry DM (2001) Chordoma: incidence and survival patterns in the United States, 1973–1995. Cancer Causes Control 12(1):1–11. https://doi.org/10.1023/a:1008947301735
Healey JH, Lane JM (1989) Chordoma: a critical review of diagnosis and treatment. Orthop Clin North Am 20(3):417–426
Tenny S, Varacallo M. Chordoma. [Updated 2022 Feb 12]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430846/
Koutourousiou M, Snyderman CH, Fernandez-Miranda J, Gardner PA (2011) Skull base chordomas. Otolaryngol Clin North Am 44(5):1155–1171. https://doi.org/10.1016/j.otc.2011.06.002
Wang L, Wu Z, Tian K et al (2017) Clinical features and surgical outcomes of patients with skull base chordoma: a retrospective analysis of 238 patients. J Neurosurg 127(6):1257–1267. https://doi.org/10.3171/2016.9.JNS16559
Kishimoto R, Omatsu T, Hasegawa A, Imai R, Kandatsu S, Kamada T (2012) Imaging characteristics of metastatic chordoma. Jpn J Radiol 30(6):509–516. https://doi.org/10.1007/s11604-012-0086-3
Habrand JL, Datchary J, Bolle S et al (2016) Chordoma in children: case-report and review of literature. Rep Pract Oncol Radiother 21(1):1–7. https://doi.org/10.1016/j.rpor.2015.10.007
Mobley BC, McKenney JK, Bangs CD et al (2010) Loss of SMARCB1/INI1 expression in poorly differentiated chordomas. Acta Neuropathol 120(6):745–753. https://doi.org/10.1007/s00401-010-0767-x
Yadav R, Sharma MC, Malgulwar PB et al (2014) Prognostic value of MIB-1, p53, epidermal growth factor receptor, and INI1 in childhood chordomas. Neuro Oncol 16(3):372–381. https://doi.org/10.1093/neuonc/not228
al-Mefty O, Borba LA (1997) Skull base chordomas: a management challenge. J Neurosurg 86(2):182–189. https://doi.org/10.3171/jns.1997.86.2.0182
Stacchiotti S, Sommer J, Chordoma Global Consensus Group (2015) Building a global consensus approach to chordoma: a position paper from the medical and patient community. Lancet Oncol 16(2):e71–e83. https://doi.org/10.1016/S1470-2045(14)71190-8
Weber DC, Rutz HP, Pedroni ES et al (2005) Results of spot-scanning proton radiation therapy for chordoma and chondrosarcoma of the skull base: the Paul Scherrer Institut experience. Int J Radiat Oncol Biol Phys 63(2):401–409. https://doi.org/10.1016/j.ijrobp.2005.02.023
Hoch BL, Nielsen GP, Liebsch NJ, Rosenberg AE (2006) Base of skull chordomas in children and adolescents: a clinicopathologic study of 73 cases. Am J Surg Pathol 30(7):811–818. https://doi.org/10.1097/01.pas.0000209828.39477.ab
Rutz HP, Weber DC, Goitein G et al (2008) Postoperative spot-scanning proton radiation therapy for chordoma and chondrosarcoma in children and adolescents: initial experience at Paul Scherrer Institute. Int J Radiat Oncol Biol Phys 71(1):220–225. https://doi.org/10.1016/j.ijrobp.2007.09.014
Pehlivan B, Ares C, Lomax AJ et al (2012) Temporal lobe toxicity analysis after proton radiation therapy for skull base tumors. Int J Radiat Oncol Biol Phys 83(5):1432–1440. https://doi.org/10.1016/j.ijrobp.2011.10.042
Korchi AM, Garibotto V, Lovblad KO, Haller S, Weber DC (2013) Radiologic patterns of necrosis after proton therapy of skull base tumors. Can J Neurol Sci 40(6):800–806. https://doi.org/10.1017/s0317167100015924
Deraniyagala RL, Yeung D, Mendenhall WM et al (2014) Proton therapy for skull base chordomas: an outcome study from the University of Florida proton therapy institute. J Neurol Surg B Skull Base 75(1):53–57. https://doi.org/10.1055/s-0033-1354579
McDonald MW, Linton OR, Moore MG, Ting JY, Cohen-Gadol AA, Shah MV (2016) Influence of residual tumor volume and radiation dose coverage in outcomes for clival chordoma. Int J Radiat Oncol Biol Phys 95(1):304–311. https://doi.org/10.1016/j.ijrobp.2015.08.011
Weber DC, Malyapa R, Albertini F et al (2016) Long term outcomes of patients with skull-base low-grade chondrosarcoma and chordoma patients treated with pencil beam scanning proton therapy. Radiother Oncol 120(1):169–174. https://doi.org/10.1016/j.radonc.2016.05.011
Tsitouras V, Wang S, Dirks P et al (2016) Management and outcome of chordomas in the pediatric population: the Hospital for Sick Children experience and review of the literature. J Clin Neurosci 34:169–176. https://doi.org/10.1016/j.jocn.2016.06.003
Ramm-Pettersen J, Frič R, Berg-Johnsen J (2017) Long-term follow-up after endoscopic trans-sphenoidal surgery or initial observation in clivus chordomas. Acta Neurochir (Wien) 159(10):1849–1855. https://doi.org/10.1007/s00701-017-3236-7
Gatfield ER, Noble DJ, Barnett GC et al (2018) Tumour volume and dose influence outcome after surgery and high-dose photon radiotherapy for chordoma and chondrosarcoma of the skull base and spine. Clin Oncol (R Coll Radiol) 30(4):243–253. https://doi.org/10.1016/j.clon.2018.01.002
Takagi M, Demizu Y, Nagano F et al (2018) Treatment outcomes of proton or carbon ion therapy for skull base chordoma: a retrospective study. Radiat Oncol 13(1):232. https://doi.org/10.1186/s13014-018-1173-0
Hottinger AL, Bojaxhiu B, Ahlhelm F et al (2020) Prognostic impact of the “Sekhar grading system for cranial chordomas” in patients treated with pencil beam scanning proton therapy: an institutional analysis. Radiat Oncol 15(1):96. https://doi.org/10.1186/s13014-020-01547-x
Iannalfi A, D’Ippolito E, Riva G et al (2021) 2020 Proton and carbon ion radiotherapy in skull base chordomas: a prospective study based on a dual particle and a patient-customized treatment strategy [published correction appears in Neuro Oncol. Neuro Oncol 22(9):1348–1358. https://doi.org/10.1093/neuonc/noaa067
Basler L, Poel R, Schröder C et al (2020) Dosimetric analysis of local failures in skull-base chordoma and chondrosarcoma following pencil beam scanning proton therapy. Radiat Oncol 15(1):266. https://doi.org/10.1186/s13014-020-01711-3
Metcalfe C, Muzaffar J, Kulendra K et al (2021) Chordomas and chondrosarcomas of the skull base: treatment and outcome analysis in a consecutive case series of 24 patients. World J Surg Oncol 19(1):68. https://doi.org/10.1186/s12957-021-02178-6
Rutkowski MJ, Birk HS, Wood MD et al (2017) Metastatic clival chordoma: a case report of multiple extraneural metastases following resection and proton beam radiotherapy in a 5-year old boy. J Neurosurg Pediatr 19(5):531–537. https://doi.org/10.3171/2017.1.PEDS16549
Forsyth PA, Cascino TL, Shaw EG et al (1993) Intracranial chordomas: a clinicopathological and prognostic study of 51 cases. J Neurosurg 78(5):741–747. https://doi.org/10.3171/jns.1993.78.5.0741
Tamura T, Sato T, Kishida Y et al (2015) Outcome of clival chordomas after skull base surgeries with mean follow-up of 10 years. Fukushima J Med Sci 61(2):131–140. https://doi.org/10.5387/fms.2015-12
Choi D, Gleeson M (2010) Surgery for chordomas of the craniocervical junction: lessons learned. Skull Base 20(1):41–45. https://doi.org/10.1055/s-0029-1242984
Colli BO, Al-Mefty O (2001) Chordomas of the skull base: follow-up review and prognostic factors. Neurosurg Focus 10(3):E1. https://doi.org/10.3171/foc.2001.10.3.2
Gay E, Sekhar LN, Rubinstein E et al (1995) Chordomas and chondrosarcomas of the cranial base: results and follow-up of 60 patients. Neurosurgery 36(5):887–897. https://doi.org/10.1227/00006123-199505000-00001
Carpentier A, Polivka M, Blanquet A, Lot G, George B (2002) Suboccipital and cervical chordomas: the value of aggressive treatment at first presentation of the disease. J Neurosurg 97(5):1070–1077. https://doi.org/10.3171/jns.2002.97.5.1070
Munzenrider JE, Liebsch NJ (1999) Proton therapy for tumors of the skull base. Strahlenther Onkol 175(Suppl 2):57–63. https://doi.org/10.1007/BF03038890
Suit H, Goldberg S, Niemierko A et al (2003) Proton beams to replace photon beams in radical dose treatments. Acta Oncol 42(8):800–808. https://doi.org/10.1080/02841860310017676
Amichetti M, Cianchetti M, Amelio D, Enrici RM, Minniti G (2009) Proton therapy in chordoma of the base of the skull: a systematic review. Neurosurg Rev 32(4):403–416. https://doi.org/10.1007/s10143-009-0194-4
Matloob SA, Nasir HA, Choi D (2016) Proton beam therapy in the management of skull base chordomas: systematic review of indications, outcomes, and implications for neurosurgeons. Br J Neurosurg 30(4):382–387. https://doi.org/10.1080/02688697.2016.1181154
Alahmari M, Temel Y (2019) Skull base chordoma treated with proton therapy: a systematic review. Surg Neurol Int. 10:96. Published 2019 Jun 7. https://doi.org/10.25259/SNI-213-2019
Di Maio S, Temkin N, Ramanathan D, Sekhar LN (2011) Current comprehensive management of cranial base chordomas: 10-year meta-analysis of observational studies. J Neurosurg 115(6):1094–1105. https://doi.org/10.3171/2011.7.JNS11355
Engelsman M, Schwarz M, Dong L (2013) Physics controversies in proton therapy. Semin Radiat Oncol 23(2):88–96. https://doi.org/10.1016/j.semradonc.2012.11.003
Jiang S, Wang J, Li H et al (2016) Novel hybrid scattering- and scanning-beam proton therapy approach. Int J Part Ther 3(1):37–50. https://doi.org/10.14338/IJPT-15-00014.1
Grosshans DR, Zhu XR, Melancon A et al (2014) Spot scanning proton therapy for malignancies of the base of skull: treatment planning, acute toxicities, and preliminary clinical outcomes. Int J Radiat Oncol Biol Phys 90(3):540–546. https://doi.org/10.1016/j.ijrobp.2014.07.005
Ares C, Hug EB, Lomax AJ et al (2009) Effectiveness and safety of spot scanning proton radiation therapy for chordomas and chondrosarcomas of the skull base: first long-term report. Int J Radiat Oncol Biol Phys 75(4):1111–1118. https://doi.org/10.1016/j.ijrobp.2008.12.055
Benk V, Liebsch NJ, Munzenrider JE, Efird J, McManus P, Suit H (1995) Base of skull and cervical spine chordomas in children treated by high-dose irradiation. Int J Radiat Oncol Biol Phys 31(3):577–581. https://doi.org/10.1016/0360-3016(94)00395-2
Austin AM, Douglass MJJ, Nguyen GT, Penfold SN (2017) A radiobiological Markov simulation tool for aiding decision making in proton therapy referral. Phys Med 44:72–82. https://doi.org/10.1016/j.ejmp.2017.11.013
Schultz C, Goffi-Gomez MV, Pecora Liberman PH, Pellizzon AC, Carvalho AL (2010) Hearing loss and complaint in patients with head and neck cancer treated with radiotherapy. Arch Otolaryngol Head Neck Surg 136(11):1065–1069. https://doi.org/10.1001/archoto.2010.180
Austin AM, Douglass MJJ, Nguyen GT et al (2019) Cost-effectiveness of proton therapy in treating base of skull chordoma. Australas Phys Eng Sci Med 42(4):1091–1098. https://doi.org/10.1007/s13246-019-00810-0
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection and analysis were performed by Bhavya Pahwa, Khalid Medani, and Victor M Lu. The first draft of the manuscript was written by Bhavya Pahwa and Turki Elarjani, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pahwa, B., Medani, K., Lu, V.M. et al. Proton beam therapy for skull base chordomas: a systematic review of tumor control rates and survival rates. Neurosurg Rev 45, 3551–3563 (2022). https://doi.org/10.1007/s10143-022-01880-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-022-01880-7