Abstract
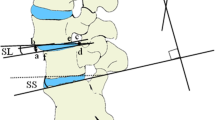
The disc angle at the fused segment is extended in operative prone position, but eventually returns to preoperative neutral position within 6 months to 1 year. This study aimed to assess pedicle screw (PS) shift without loosening to identify the mechanism of the change in disc angle after posterior fusion for degenerative lumbar spondylolisthesis (DLS). Sixty-three consecutive patients who underwent facet fusion for L4 single-level DLS were retrospectively reviewed using computed tomography (CT) immediately after surgery and 6 months postoperatively. Twenty-two patients (88 PSs) in whom the disc angle had decreased by more than 4° at 6-month postoperative radiographic follow-up were selected to more readily identify and quantify PS shift. Six patients with PS loosening and/or nonunion were excluded. We reconstructed a CT plane, vertical to the cranial endplate of the vertebrae and passing through the cannula used for percutaneous PSs. Angle α, which is formed by the cranial endplate and the cannula on this plane, was measured. A change in angle α of more than 2° between the immediate postoperative period and the 6-month follow-up was defined as a PS shift. Angle α did not change by more than 2° in any of the 44 PSs in the upper vertebrae of the fused segment. In the lower vertebrae, angle α changed by more than 2° in 22 of 44 PSs. The change in angle α in the lower vertebrae (average, 2.3°) was significantly greater than that in the upper vertebrae (average, 0.2°) (P < 0.0001). The change in the disc angle was not relevant to clinical outcomes assessed by the Japanese Orthopaedic Association Back Pain Evaluation Questionnaire, the Roland-Morris Disability Questionnaire, and the visual analogue scale. The disc angle at the fused segment returned to preoperative neutral position due to PS shift without loosening, mainly in the lower vertebrae. PS shift is caused by bone remodeling in response to biomechanical load, similar to that in orthodontic tooth movement. As PS has limited ability to maintain a lordotic disc angle, even with the insertion of a cage, lumbar alignment will return to preoperative neutral position owing to cage subsidence or adjacent segment disease. These findings might indicate that it is not necessary to correct the spinal alignment for DLS.








Similar content being viewed by others
References
Bondemark L (1998) Interdental bone changes after orthodontic treatment: a 5-year longitudinal study. Am J Orthod Dentofac Orthop 114:25–31
Cakir B, Richter M, Käfer W, Wieser M, Puhl W, Schmidt R (2006) Evaluation of lumbar spine motion with dynamic X-ray–a reliability analysis. Spine 31:1258–1264
Fukui M, Chiba K, Kawakami M, Kikuchi S, Konno S, Miyamoto M, Seichi A, Shimamura T, Shirado O, Taguchi T, Takahashi K, Takeshita K, Tani T, Toyama Y, Yonenobu K, Wada E, Tanaka T, Hirota Y, Subcommittee of the Clinical Outcome Committee of the Japanese Orthopaedic Association on Low Back Pain and Cervical Myelopathy Evaluation (2009) JOA back pain evaluation questionnaire (JOABPEQ)/JOA cervical myelopathy evaluation questionnaire (JOACMEQ). The report on the development of revised versions April 16, 2007. J Orthop Sci 14:348–365
Huang H, Williams RC, Kyrkanides S (2014) Accelerated orthodontic tooth movement: molecular mechanisms. Am J Orthod Dentofac Orthop 146:620–632
Jain S, Modi HN, Suh SW, Yang JH, Hong JY (2009) Pedicle shifting or migration as one of the causes of curve progression after posterior fusion: an interesting case report and review of literature. J Pediatr Orthop B 18:369–374
Janson G, Bombonatti R, Brandão AG, Henriques JF, de Freitas MR (2003) Comparative radiographic evaluation of the alveolar bone crest after orthodontic treatment. Am J Orthod Dentofac Orthop 124:157–164
Jiang SD, Wu QZ, Lan SH, Dai LY (2012) Reliability of the measurement of thoracolumbar burst fracture kyphosis with Cobb angle, Gardner angle, and sagittal index. Arch Orthop Trauma Surg 132:221–225
Kaito T, Hosono N, Mukai Y, Makino T, Fuji T, Yonenobu K (2010) Induction of early degeneration of the adjacent segment after posterior lumbar interbody fusion by excessive distraction of lumbar disc space. J Neurosurg Spine 12:671–679
Kotwal S, Kawaguchi S, Lebl D, Hughes A, Huang R, Sama A, Cammisa F, Girardi F (2015) Minimally invasive lateral lumbar interbody fusion: clinical and radiographic outcome at a minimum 2-year follow-up. J Spinal Disord Tech 28:119–125
Le TV, Baaj AA, Dakwar E, Burkett CJ, Murray G, Smith DA, Uribe JS (2012) Subsidence of polyetheretherketone intervertebral cages in minimally invasive lateral retroperitoneal transpsoas lumbar interbody fusion. Spine 37:1268–1273
Malham GM, Ellis NJ, Parker RM, Seex KA (2012) Clinical outcome and fusion rates after the first 30 extreme lateral interbody fusions. Sci World J 2012:246989
Miyashita T, Ataka H, Kato K, Tanno T (2015) Good clinical outcomes and fusion rate of facet fusion with a percutaneous pedicle screw system for degenerative lumbar spondylolisthesis. Minimally invasive evolution of posterolateral fusion. Spine 40:E552–E557
Niklas A, Proff P, Gosau M, Römer P (2013) The role of hypoxia in orthodontic tooth movement. Int J Dent 2013:841840
Ogaard B (1988) Marginal bone support and tooth lengths in 19-year-olds following orthodontic treatment. Eur J Orthod 10:180–186
Tanno T, Ataka H, Miyashita T (2008) Long-term results of posterolateral fusion with a pedicle screw system for degenerative lumbar spondylolisthesis in relation to adjacent segment disease. Nihon Sekitsui Sekizuibyou Gakkai zasshi (J Japanese Society Spine Surg Relat Res) 19:617–621
Tsubota K, Adachi T, Tomita Y (2003) Effects of a fixation screw on trabecular structural changes in a vertebral body predicted by remodeling simulation. Ann Biomed Eng 31:733–740
Zainal Ariffin SH, Yamamoto Z, Zainol Abidin IZ, Megat Abdul Wahab R, Zainal Ariffin Z (2011) Cellular and molecular changes in orthodontic tooth movement. Sci World J 11:1788–1803
Acknowledgements
The authors wish to thank Dr. Daisuke Ishigami for information about orthodontic treatment.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of study, formal consent is not required.
Institutional ethics committee approval
This study was approved by the Medical Ethics Committee of Matsudo City General Hospital (#25-13).
Additional information
Permission was granted to reproduce Fig. 1 and Fig. 4 in the Nihon Sekitsui Sekizuibyou Gakkai zasshi (The Journal of the Japanese Society for Spine Surgery and Related Research). 2008; 19: 617–621.
Rights and permissions
About this article
Cite this article
Miyashita, T., Ataka, H., Kato, K. et al. Pedicle screw shift without loosening following instrumented posterior fusion: limitations of pedicle screw fixation. Neurosurg Rev 42, 691–698 (2019). https://doi.org/10.1007/s10143-018-1030-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-018-1030-5