Abstract
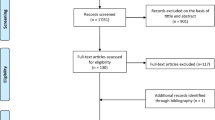
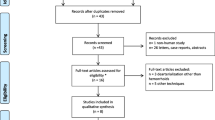
Laser hemorrhoidoplasty (LHP) is known as a new minimally invasive and painless procedure for symptomatic hemorrhoids. However, Milligan-Morgan (MM) may offer the best result of long-term cure rates. In this study, we aim to compare the efficacy between LHP and MM for hemorrhoidal disease treatment. Using specific keywords, we comprehensively go through the potential articles on PubMed, Europe PMC, and Google Scholar sources until April 19, 2022. All published studies on LHP and MM hemorrhoidectomy were collected. Statistical analysis was done by using Review Manager 5.4 software. Twelve studies with a total of 1756 patients with hemorrhoid grades II–IV were included for the analysis. Our pooled analysis revealed that LHP was associated with shorter operative time (p < 0.00001), shorter length of hospital stay (p = 0.0005), lower risk of urinary retention (p = 0.005) and anal stenosis (p = 0.0004), and lower VAS 24-h post-operative (p < 0.00001) when compared with MM. However, LHP and MM did not differ in terms of recurrence rate (p = 0.70). LHP was superior to MM procedure in terms of shortening the recovery time and minimizing post-operative complications for patients with hemorrhoidal disease.



Similar content being viewed by others
Data availability
The authors confirm that the data supporting the findings of this study are available within the article.
References
Zhang G, Liang R, Wang J, Ke M, Chen Z, Huang J et al (2020) Network meta-analysis of randomized controlled trials comparing the procedure for prolapse and hemorrhoids, Milligan-Morgan hemorrhoidectomy and tissue-selecting therapy stapler in the treatment of grade III and IV internal hemorrhoids(Meta-analysis). Int J Surg 74:53–60. https://doi.org/10.1016/j.ijsu.2019.12.027
Abbas ST, Raza A, Muhammad ChI, Hameed T, Hasham N, Arshad N (2020) Comparison of mean pain score using topical and oral metronidazole in post Milligan Morgan hemorrhoidectomy patient; a randomized controlled trial. Pak J Med Sci 36(5):867–871. https://doi.org/10.12669/pjms.36.5.1796
Balciscueta Z, Balciscueta I, Uribe N (2021) Post-hemorrhoidectomy pain: can surgeons reduce it? A systematic review and network meta-analysis of randomized trials. Int J Colorectal Dis 36(12):2553–2566. https://doi.org/10.1007/s00384-021-04013-6
Danys D, Pacevicius J, Makunaite G, Palubeckas R, Mainelis A, Markevicius N et al (2020) Tissue coagulation in laser hemorrhoidoplasty - an experimental study. Open Med (Wars) 8(15):185–189. https://doi.org/10.1515/med-2020-0027
Longchamp G, Liot E, Meyer J, Toso C, Buchs NC, Ris F (2021) Non-excisional laser therapies for hemorrhoidal disease: a systematic review of the literature. Lasers Med Sci 36(3):485–496. https://doi.org/10.1007/s10103-020-03142-8
Poskus T, Danys D, Makunaite G, Mainelis A, Mikalauskas S, Poskus E et al (2020) Results of the double-blind randomized controlled trial comparing laser hemorrhoidoplasty with sutured mucopexy and excisional hemorrhoidectomy. Int J Colorectal Dis 35(3):481–490. https://doi.org/10.1007/s00384-019-03460-6
De Nardi P, Tamburini AM, Gazzetta PG, Lemma M, Pascariello A, Asteria CR (2016) Hemorrhoid laser procedure for second- and third-degree hemorrhoids: results from a multicenter prospective study. Tech Coloproctol 20(7):455–459. https://doi.org/10.1007/s10151-016-1479-6
Gupta K, Agarwal N, Mital K (2021) Clinical outcomes in patients with hemorrhoids treated by finger guided hemorrhoidal artery ligation with laser hemorrhoidoplasty: a retrospective cohort study. JAMMR 33(18):143–152. https://doi.org/10.9734/jammr/2021/v33i1831064
Trigui A, Rejab H, Akrout A, Trabelsi J, Zouari A, Majdoub Y et al (2022) Laser utility in the treatment of hemorrhoidal pathology: a review of literature. Lasers Med Sci 37(2):693–699. https://doi.org/10.1007/s10103-021-03333-x
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA 283(15):2008–12. https://doi.org/10.1001/jama.283.15.2008
Moher D, Liberati A, Tetzlaff J, Altman DG, PRISMA Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535. https://doi.org/10.1136/bmj.b2535
Huang J, Wang X, Chen X, Song Q, Liu W, Lu L (2016) Perioperative antibiotics to prevent acute endophthalmitis after ophthalmic surgery: a systematic review and meta-analysis. PLoS One 11(11):e0166141. https://doi.org/10.1371/journal.pone.0166141
Margulis AV, Pladevall M, Riera-Guardia N, Varas-Lorenzo C, Hazell L, Berkman ND et al (2014) Quality assessment of observational studies in a drug-safety systematic review, comparison of two tools: the Newcastle-Ottawa Scale and the RTI item bank. Clin Epidemiol 10(6):359–368. https://doi.org/10.2147/CLEP.S66677
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135. https://doi.org/10.1186/1471-2288-14-135
Abdulkarim A, Misoi B, Gathege D (2020) Laser hemorrhoidoplasty: experience at Aga Khan University Hospital. Ann Afr Surg 17(2):76–79. https://doi.org/10.4314/aas.v17i2.8
Alsisy AA, Alkhateep YM, Salem IEI (2019) Comparative study between intrahemorrhoidal diode laser treatment and Milligan-Morgan hemorrhoidectomy. Menoufia Med J 32:560–565. https://doi.org/10.4103/mmj.mmj_101_18
Eskandaros MS, Darwish AA (2020) Comparative study between Milligan-Morgan hemorrhoidectomy, stapled hemorrhoidopexy, and laser hemorrhoidoplasty in patients with third degree hemorrhoids: a prospective study. Egypt J Surg 39:352–363. https://doi.org/10.4103/ejs.ejs_214_19
Hassan A, El-Shemy GG (2021) Laser hemorrhoidoplasty versus open hemorrhoidectomy in Upper Egypt. AIMJ 2(2):84–89. https://doi.org/10.21608/aimj.2021.57763.1397
Khan HM, Gowda VSS, Ramesh BS, Sandeep D (2021) A comparative evaluation of laser hemorrhoidoplasty versus open surgical hemorrhoidectomy treatment of grade III and IV hemorrhoids. A prospective observational study. J Clin Invest Surg 6(1):30–36
Maloku H, Gashi Z, Lazovic R, Islami H, Juniku-Shkololli A (2014) Laser hemorrhoidoplasty procedure vs open surgical hemorrhoidectomy: a trial comparing 2 treatments for hemorrhoids of third and fourth degree. Acta Inform Med 22(6):365–367. https://doi.org/10.5455/aim.2014.22.365-367
Maloku H, Lazovic R, Terziqi H (2019) Laser hemorrhoidoplasty versus Milligan-Morgan hemorrhoidectomy – short-term outcome. Vojnosanit Pregl 76(1):8–12. https://doi.org/10.2298/VSP170125070M
Mohammed AF, Al-Sultani DAH, Janabi HMF (2019) A comparative study between laser hemorrhoidoplasty procedure and conventional hemorrhoidectomy. JUBPAS 27(1):69–86. https://doi.org/10.29196/jubpas.v27i1.2065
Naderan M, Shoar S, Nazari M, Elsayed A, Mahmoodzadeh H, Khorgami Z (2017) A randomized controlled trial comparing laser intra-hemorrhoidal coagulation and Milligan-Morgan hemorrhoidectomy. J Invest Surg 30(5):325–331. https://doi.org/10.1080/08941939.2016.1248304
Nagdy MA (2022) Comparative study between Milligan Morgan haemorrhoidectomy and laser ablation for the management of third and fourth degree of hemorrhoids. AIMJ 3(3):49–58. https://doi.org/10.21608/aimj.2022.109601.1704
Shabahang H, Maddah G, Mofidi A, Nooghabi MJ, Khaniki SH (2019) A randomized clinical trial of laser hemorrhoidoplasty vs Milligan and Morgan hemorrhoidectomy. World J Lap Surg 12(2):59–63. https://doi.org/10.5005/jp-journals-10033-1373
Yahya WN, Refaat DO, AbdElhady WA, Elsayed WA (2022) Comparison between laser hemorrhoidoplasty procedure and conventional open surgical hemorrhoidectomy. EJHM 86(1):112–116. https://doi.org/10.21608/ejhm.2022.210781
Jain A, Lew C, Aksakal G, Hiscock R, Mirbagheri N (2022) Laser hemorrhoidoplasty in the treatment of symptomatic hemorrhoids: a pilot Australian study. Ann Coloproctol. https://doi.org/10.3393/ac.2022.00164.0023
Koh FH, Foo FJ, Ho L, Sivarajah SS, Tan WJ, Chew MH (2020) Study protocol for the use of conventional open haemorrhoidectomy versus laser haemorrhoidoplasty in the treatment of symptomatic haemorrhoids: a randomized controlled trial. Eur Surg Res 61(6):201–208. https://doi.org/10.1159/000513844
Suh YJ, Ha HK, Oh HK, Shin R, Jeong SY, Park KJ (2013) Rectal perforation caused by anal stricture after hemorrhoid treatment. Ann Coloproctol 29(1):28–30. https://doi.org/10.3393/ac.2013.29.1.28
Roervik HD, Heiner Campos A, Ilum L, Herlak Styr KF, McKinstrey GK, Brandstrup B et al (2019) Minimal open hemorrhoidectomy. Tech Coloproctol 23(1):73–77. https://doi.org/10.1007/s10151-018-1915-x
Brusciano L, Gambardella C, Terracciano G, Gualtieri G, Schiano di Visconte M, Tolone S et al (2020) Postoperative discomfort and pain in the management of hemorrhoidal disease: laser hemorrhoidoplasty, a minimal invasive treatment of symptomatic hemorrhoids. Updates Surg 72(3):851–857. https://doi.org/10.1007/s13304-019-00694-5
Leventoglu S, Mentes B, Balci B, Kebiz HC (2022) New techniques in hemorrhoidal disease but the same old problem: anal stenosis. Medicina (Kaunas) 58(3):362. https://doi.org/10.3390/medicina58030362
Erzurumlu K, Karabulut K, Özbalcı GS, Tarım İA, Lap G, Güngör B (2017) The whitehead operation procedure: is it a useful technique? Turk J Surg 33(3):190–194. https://doi.org/10.5152/turkjsurg.2017.3483
Eberspacher C, Mascagni P, Zeri KP, Fralleone L, Naldini G, Mascagni D (2021) Self-mechanical anal dilatation: a simple trick to minimize postoperative pain and stenosis following hemorrhoidectomy with radiofrequency. Front Surg 30(8):711958. https://doi.org/10.3389/fsurg.2021.711958
Asfar S (2018) Anoplasty for post-hemorrhoidectomy low anal stenosis: a new technique. World J Surg 42(9):3015–3020. https://doi.org/10.1007/s00268-018-4561-6
Katdare MV, Ricciardi R (2010) Anal stenosis. Surg Clin North Am 90(1):137–45. https://doi.org/10.1016/j.suc.2009.10.002
Faes S, Pratsinis M, Hasler-Gehrer S, Keerl A, Nocito A (2019) Short- and long-term outcomes of laser haemorrhoidoplasty for grade II-III haemorrhoidal disease. Colorectal Dis 21(6):689–696. https://doi.org/10.1111/codi.14572
Author information
Authors and Affiliations
Contributions
• Study conception and design: Hendry Lie, Evelyn Franca Caesarini, Antonius Agung Purnama, Andry Irawan, Taufik Sudirman, Wifanto Saditya Jeo, Bernardus Parish Budiono, Erik Prabowo, M Iqbal Rivai, Ryanto Karobuana Sitepu
• Acquisition of data: Hendry Lie, Evelyn Franca Caesarini, Antonius Agung Purnama, Andry Irawan, Taufik Sudirman
• Analysis and interpretation of data: Wifanto Saditya Jeo, Bernardus Parish Budiono, Erik Prabowo, M Iqbal Rivai, Ryanto Karobuana Sitepu
• Drafting of manuscript: Hendry Lie, Evelyn Franca Caesarini, Antonius Agung Purnama, Andry Irawan, Taufik Sudirman
• Critical revision of manuscript: Wifanto Saditya Jeo, Bernardus Parish Budiono, Erik Prabowo, M Iqbal Rivai, Ryanto Karobuana Sitepu
Corresponding author
Ethics declarations
Ethics approval
Not applicable for this type of study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Lie, H., Caesarini, E.F., Purnama, A.A. et al. Laser hemorrhoidoplasty for hemorrhoidal disease: a systematic review and meta-analysis. Lasers Med Sci 37, 3621–3630 (2022). https://doi.org/10.1007/s10103-022-03643-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-022-03643-8