Abstract
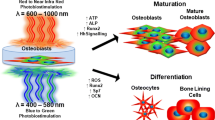
Low-level laser therapy (LLLT)-induced photobiomodulation (PBM) stimulates bone tissue regeneration by inducing osteoblast differentiation and mitochondrial activation. However, the role of reactive oxygen species (ROS) in this process remains controversial. The aim of this systematic review was to collect and analyze the available literature on the cellular and molecular effects of LLLT on osteoblasts and the role of ROS in this process. A search was conducted in PubMed, ScienceDirect, Scopus, and Web of Science. Studies published in English over the past 15 years were selected. Fourteen articles were included with moderate (n = 9) and low risk of bias (n = 5). Thirteen studies reported the use of diode lasers with wavelengths (λ) between 635 and 980 nm. One study used an Nd:YAG laser (λ1064 nm). The most commonly used λ values were 808 and 635 nm. The energy densities ranged from 0.378 to 78.75 J/cm2, and irradiation times from 1.5 to 300 s. Most studies found increases in proliferation, ATP synthesis, mitochondrial activity, and osteoblastic differentiation related to moderate and dose-dependent increases in intracellular ROS levels. Only two studies reported no significant changes. The data presented heterogeneity owing to the variety of LLLT protocols. Although several studies have shown a positive role of ROS in the induction of proliferation, migration, and differentiation of different cell types, further research is required to determine the specific role of ROS in the osteoblastic cell response and the molecular mechanisms involved in triggering previously reported cellular events.

Similar content being viewed by others
References
Scheinin A, Kantola S (1969) Laser-induced effects on tooth structure I. Crater Production With A CO2-Laser. Acta Odontol Scan 27(2):173–179
Spanemberg JC, Figueiredo MA, Cherubini K, Salum FG (2016) Low-level laser therapy: a review of its applications in the management of oral mucosal disorders. Altern Ther Health Med 22(6):24–31
Ahrabi B, Tavirani MR, Khoramgah MS, Noroozian M, Darabi S, Khoshsirat S et al (2019) The effect of photobiomodulation therapy on the differentiation, proliferation, and migration of the mesenchymal stem cell: a review. J Lasers Med Sci 10(Suppl 1):96
Deana AM, de Souza AM, Teixeira VP, Mesquita-Ferrari RA, Bussadori SK, Fernandes KPS (2018) The impact of photobiomodulation on osteoblast-like cell: a review. Lasers Med Sci 33(5):1147–1158
Incerti Parenti S, Tschon M, Sartori M, Visani A, Aroni E, Fini M et al (2020) Evidence from systematic reviews on photobiomodulation of human bone and stromal cells: Where do we stand? Arch Biochem Biophys 685:108333
Jawad MM, Husein A, Azlina A, Alam MK, Hassan R, Shaari R (2013) Effect of 940 nm low-level laser therapy on osteogenesis in vitro. J Biomed Opt 18(12):128001
Tani A, Chellini F, Giannelli M, Nosi D, Zecchi-Orlandini S, Sassoli C (2018) Red (635 nm), Near-Infrared (808 nm) and Violet-Blue (405 nm) Photobiomodulation potentiality on human osteoblasts and mesenchymal stromal cells: a morphological and molecular in vitro study. Int J Mol Sci 19:7–1946
Sharma P, Jha AB, Dubey RS, Pessarakli MJ (2012) Reactive oxygen species, oxidative damage, and antioxidative defense mechanism in plants under stressful conditions. J Bot 2012:1–26
Chung H, Dai T, Sharma SK, Huang Y-Y, Carroll JD, Hamblin MR (2012) The nuts and bolts of low-level laser (light) therapy. Ann Biomed Eng 40(2):516–533
Rupel K, Zupin L, Colliva A, Kamada A, Poropat A, Ottaviani G et al (2018) Photobiomodulation at multiple wavelengths differentially modulates oxidative stress in vitro and in vivo. Oxid Med Cell Longev 2018:6510159
Altan AB, Bicakci AA, Avunduk MC, Esen H (2015) The effect of dosage on the efficiency of LLLT in new bone formation at the expanded suture in rats. Lasers Med Sci 30(1):255–262
Aras MH, Bozdag Z, Demir T, Oksayan R, Yanik S, Sokucu O (2015) Effects of low-level laser therapy on changes in inflammation and in the activity of osteoblasts in the expanded premaxillary suture in an ovariectomized rat model. Photomed Laser Surg 33(3):136–144
Kalhori KAM, Vahdatinia F, Jamalpour MR, Vescovi P, Fornaini C, Merigo E et al (2019) Photobiomodulation in Oral Medicine. Photobiomodul Photomed Laser Surg 37(12):837–861
de Almeida VL, de Andrade Gois VL, Andrade RN, Cesar CP, de Albuquerque-Junior RL, de Mello RS et al (2016) Efficiency of low-level laser therapy within induced dental movement: a systematic review and meta-analysis. J Photochem Photobiol B 158:258–266
Cericato GO, Bittencourt MA, Paranhos LR (2015) Validity of the assessment method of skeletal maturation by cervical vertebrae: a systematic review and meta-analysis. Dentomaxillofacial Radiol 44(4):20140270
Kushibiki T, Tu Y, Abu-Yousif AO, Hasan T (2015) Photodynamic activation as a molecular switch to promote osteoblast cell differentiation via AP-1 activation. Sci Rep 5:13114
Son JH, Park BS, Kim IR, Sung IY, Cho YC, Kim JS et al (2017) A novel combination treatment to stimulate bone healing and regeneration under hypoxic conditions: photobiomodulation and melatonin. Lasers Med Sci 32(3):533–541
Amaroli A, Agas D, Laus F, Cuteri V, Hanna R, Sabbieti MG et al (2018) The effects of photobiomodulation of 808 nm diode laser therapy at higher fluence on the in vitro osteogenic differentiation of bone marrow stromal cells. Front Physiol 9:123
Ateş GB, Ak A, Garipcan B, Gülsoy M (2018) Indocyanine green-mediated photobiomodulation on human osteoblast cells. Lasers Med Sci 33(7):1591–1599
Kunimatsu R, Gunji H, Tsuka Y, Yoshimi Y, Awada T, Sumi K et al (2018) Effects of high-frequency near-infrared diode laser irradiation on the proliferation and migration of mouse calvarial osteoblasts. Lasers Med Sci 33(5):959–966
Pires Oliveira DAA, De Oliveira RF, Zangaro RA, Soares CP (2008) Evaluation of low-level laser therapy of osteoblastic cells. Photomed Laser Surg 26(4):401–404
Xu Y, Young MJ, Battaglino RA, Morse LR, Fontana CR, Pagonis TC et al (2009) Endodontic antimicrobial photodynamic therapy: safety assessment in mammalian cell cultures. J Endod 35(11):1567–1572
Huang TH, Lu YC, Kao CT (2012) Low-level diode laser therapy reduces lipopolysaccharide (LPS)-induced bone cell inflammation. Lasers Med Sci 27(3):621–627
Migliario M, Pittarella P, Fanuli M, Rizzi M, Renò F (2014) Laser-induced osteoblast proliferation is mediated by ROS production. Lasers Med Sci 29(4):1463–1467
Ballini A, Mastrangelo F, Gastaldi G, Tettamanti L, Bukvic N, Cantore S et al (2015) Osteogenic differentiation and gene expression of dental pulp stem cells under low-level laser irradiation: A good promise for tissue engineering. J Biol Regul Homeost Agents 29(4):813–822
Ateş GB, Can AA, Gülsoy MJ (2017) Investigation of photobiomodulation potentiality by 635 and 809 nm lasers on human osteoblasts. Lasers Med Sci 32(3):591–599
Tsuka Y, Kunimatsu R, Gunji H, Nakajima K, Kimura A, Hiraki T et al (2019) Effects of Nd:YAG low-level laser irradiation on cultured human osteoblasts migration and ATP production: in vitro study. Lasers Med Sci 34(1):55–60
Abdelgawad LM, Abdelaziz AM, Sabry D, Abdelgwad MJ (2020) Influence of photobiomodulation and vitamin D on osteoblastic differentiation of human periodontal ligament stem cells and bone-like tissue formation through enzymatic activity and gene expression. BioMol Concepts 11(1):172–181
Cavalcanti M, Maria DA, de Isla N, Leal ECP, Joensen J, Bjordal JM et al (2015) Evaluation of the proliferative effects induced by low-level laser therapy in bone marrow stem cell culture. Photomed Laser Surg 33(12):610–616
Amaroli A, Colombo E, Zekiy A, Aicardi S, Benedicenti S, De Angelis N (2020) Interaction between laser light and osteoblasts: photobiomodulation as a trend in the management of socket bone preservation—a review. Biology (Basel) 9(11):409
Fávaro-Pípi E, Ribeiro DA, Ribeiro JU, Bossini P, Oliveira P, Parizotto NA et al (2011) Low-level laser therapy induces differential expression of osteogenic genes during bone repair in rats. Photomed Laser Surg 29(5):311–317
Wu Y-h, Wang J, Gong D-x, Gu H-y, Hu S-s, Zhang HJ (2012) Effects of low-level laser irradiation on mesenchymal stem cell proliferation: a microarray analysis. Lasers Med Sci 27(2):509–519
Dhar A, Young MR, Colburn NH (2002) The role of AP-1, NF-κB and ROS/NOS in skin carcinogenesis: the JB6 model is predictive. Mol Cell Biochem 234(1):185–193
Gazon H, Barbeau B, Mesnard JM, Peloponese JM (2018) Hijacking of the AP-1 signaling pathway during development of ATL. Front Microbiol 8:2686
Tschon M, Incerti-Parenti S, Cepollaro S, Checchi L, Fini M (2015) Photobiomodulation with low-level diode laser promotes osteoblast migration in an in vitro micro wound model. J Biomed Opt 20(7):78002
Son Y, Cheong YK, Kim NH, Chung HT, Kang DG, Pae HO (2011) Mitogen-activated protein kinases and reactive oxygen species: how can ROS activate MAPK pathways? J Signal Transduct 2011:792639
Zhang J, Xing D, Gao XJ (2008) Low-power laser irradiation activates Src tyrosine kinase through reactive oxygen species-mediated signaling pathway. J Cell Physiol 217(2):518–528
Zhang L, Xing D, Gao X, Wu SJ (2009) Low-power laser irradiation promotes cell proliferation by activating PI3K/Akt pathway. J Cell Physiol 219(3):553–562
AlGhamdi KM, Kumar A, Moussa NA (2012) Low-level laser therapy: a useful technique for enhancing the proliferation of various cultured cells. Lasers Med Sci 27(1):237–249
Arakaki N, Yamashita A, Niimi S, Yamazaki TJ (2013) Involvement of reactive oxygen species in osteoblastic differentiation of MC3T3-E1 cells accompanied by mitochondrial morphological dynamics. Biomed Res 34(3):161–166
Sun Y, Liu W-Z, Liu T, Feng X, Yang N, Zhou HF (2015) Signaling pathway of MAPK/ERK in cell proliferation, differentiation, migration, senescence and apoptosis. J Recept Signal Transduct Res 35(6):600–604
Kumar Rajendran N, George BP, Chandran R, Tynga IM, Houreld N, Abrahamse H (2019) The influence of light on reactive oxygen species and NF-кB in disease progression. Antioxidants (Basel) 8(12):640
Zhang B, Xie QY, Quan Y, Pan XM, Liao DF (2015) Reactive oxygen species induce cell death via Akt signaling in rat osteoblast-like cell line ROS 17/2.8. Toxicol Ind Health 31(12):1236–1242
Jha N, Ryu JJ, Choi EH (2017) Generation and role of reactive oxygen and nitrogen species induced by plasma, lasers, chemical agents, and other systems in dentistry. Oxid Med Cell Longev 2017:7542540
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Garzón, J., Baldion, P.A., Grajales, M. et al. Response of osteoblastic cells to low-level laser treatment: a systematic review. Lasers Med Sci 37, 3031–3049 (2022). https://doi.org/10.1007/s10103-022-03587-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-022-03587-z