Abstract
Objective
Wernicke encephalopathy (WE) is a neuropsychiatric syndrome caused by thiamine deficiency. Despite its low sensitivity, brain magnetic resonance imaging (MRI) is the most useful diagnostic technique. Our aim was to investigate whether the timing of the imaging study, and thiamine replacement can influence brain MRI findings in these patients.
Methods
Retrospective observational study of hospitalized patients between January/2008 and December/2020 with a clinical diagnosis of WE. Data from clinical presentation, diagnostic features, therapeutic approach, and outcomes were collected.
Results
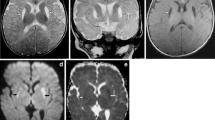
We identified 41 patients (55 ± 13.3 years) with WE. Brain MRI was performed in 36 patients, and one third had T2/FLAIR hyperintensities suggestive of WE. We found an association between a history of poor diet and periventricular hyperintensities (p = 0.023), especially on the ventral surface of the thalamus and the periaqueductal region. It was found that the odds of having a typical imaging of WE decreased by 5.3% for each additional unit (100 mg) of thiamine administered (p = 0.046) (95% CI [0.89, 0.99]). On the other hand, the number of days from clinical presentation was not found to be a viable predictor (p = 0.254) (95% CI [0.88, 1.03]) Recovery was positively correlated with the total dose of thiamine received until discharge (p = 0.020).
Conclusions
MRI hyperintensities seem to be dependent on the timing of thiamine correction and, particularly, on the thiamine dosage prescribed at admission. Nevertheless, thiamine replacement should not be delayed, as its timely prescription is associated with a better prognosis at discharge.



Similar content being viewed by others
Data availability
The data generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Harper C (1983) The incidence of Wernicke’s encephalopathy in Australia–a neuropathological study of 131 cases. J Neurol Neurosurg Psychiatry 46(7):593–598. https://doi.org/10.1136/jnnp.46.7.593
Caine D et al (1997) Operational criteria for the classification of chronic alcoholics: identification of Wernicke’s encephalopathy. J Neurol Neurosurg Psychiatry 62(1):51–60. https://doi.org/10.1136/jnnp.62.1.51
Galvin R et al (2010) EFNS guidelines for diagnosis, therapy and prevention of Wernicke encephalopathy. Eur J Neurol 17(12):1408–1418. https://doi.org/10.1111/j.1468-1331.2010.03153.x
Sinha S et al (2019) Wernicke encephalopathy—clinical pearls. Mayo Clin Proc 94(6):1065–1072. https://doi.org/10.1016/j.mayocp.2019.02.018
Chamorro AJ et al (2017) Differences between alcoholic and nonalcoholic patients with Wernicke encephalopathy: a multicenter observational study. Mayo Clin Proc 92(6):899–907. https://doi.org/10.1016/j.mayocp.2017.02.019
Harper CG, Giles M (1986) Clinical signs in the Wernicke-Korsakoff complex : retrospective analysis of 131 cases diagnosed at necropsy. J Neurol Neurosurg Psychiatry 49(4):341–345. https://doi.org/10.1136/jnnp.49.4.341
Chandrakumar A, Bhardwaj A, T’Jong GW (2019) Review of thiamine deficiency disorders: Wernicke encephalopathy and Korsakoff psychosis. J Basic Clin Physiol Pharmacol 30(2):153–162. https://doi.org/10.1515/jbcpp-2018-0075
Oudman E, Wijnia JW, Oey MJ, van Dam M, Postma A (2021) Wernicke-Korsakoff syndrome despite no alcohol abuse: a summary of systematic reports. J Neurol Sci 426:117482
Manzo, G. et al. (2014) ‘MR imaging findings in alcoholic and nonalcoholic acute Wernicke’s encephalopathy: a review’. BioMed Res Int. https://doi.org/10.1155/2014/503596
Arts NJ, Pitel AL, Kessels RP (2021) The contribution of mamillary body damage to Wernicke’s encephalopathy and Korsakoff’s syndrome. Handb Clin Neurol 180:455–475. https://doi.org/10.1016/B978-0-12-820107-7.00029-X
Harper C, B. R. (1997) ‘Nutritional and metabolic disorders’, in Greenfield’s Neuropatholog. 6th ed. London, UK, pp. 601–52.
Zhong C, Jin L, Fei G (2005) ‘MR imaging of nonalcoholic Wernicke encephalopathy: a follow-up study AJNR. Am J Neuroradiol 26(9):2301–2305
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
Approval for this study was obtained from the local Ethics Committee (REF 74/2018).
Consent to participate and consent for publication
Because of the retrospective observational nature of the study, patient informed consent was waived by the local ethics committee.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Silva, A.R., Almeida-Xavier, S., Lopes, M. et al. Is there a time window for MRI in Wernicke encephalopathy — a decade of experience from a tertiary hospital. Neurol Sci 44, 703–708 (2023). https://doi.org/10.1007/s10072-022-06477-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-022-06477-y