Abstract
Background
Wernicke encephalopathy is caused by thiamine (vitamin B1) deficiency. It is generally considered to be a disease of adult alcoholics. However, it is known to occur in the pediatric population and in non-alcoholic conditions.
Data sources
We searched PubMed with the key words Wernicke, thiamine, pediatric, children and adolescents and selected publications that were deemed appropriate.
Results
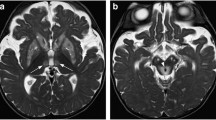
The global prevalence rates of hunger, poverty and resultant nutrient deprivation have decreased in the 21st century. However, several scenarios which may predispose to Wernicke encephalopathy may be increasingly prevalent in children and adolescents such as malignancies, intensive care unit stays and surgical procedures for the treatment of obesity. Other predisposing conditions include magnesium deficiency and defects in the SLC19A3 gene causing thiamine transporter-2 deficiency. The classic triad consists of encephalopathy, oculomotor dysfunction and gait ataxia but is not seen in a majority of patients. Treatment should be instituted immediately when the diagnosis is suspected clinically without waiting for laboratory confirmation. Common magnetic resonance findings include symmetric T2 hyperintensities in dorsal medial thalamus, mammillary bodies, periaqueductal gray matter, and tectal plate.
Conclusions
Wernicke encephalopathy is a medical emergency. Delay in its recognition and treatment may lead to significant morbidity, irreversible neurological damage or even death. This article aims to raise the awareness of this condition among pediatricians.
Similar content being viewed by others
References
Wernicke C. Die akute haemorrhagische polioencephalitis superior. In: Lehrbuch der Gehirnkrankheiten für Aerzte und Studirende, Bd II. Kassel: Fisher Verlag, 1881: 229–242.
Victor M, Adams RA, Collins GH. The Wernicke-Korsakoff syndrome and related disorders due to alcoholism and malnutrition. Philadelphia: FA Davis, 1989.
Martin PR, Singleton CK, Hiller-Sturmhöfel S. The role of thiamine deficiency in alcoholic brain disease. Alcohol Res Health 2003;27:134–142.
Blass JP, Gibson GE. Abnormality of a thiamin-requiring enzyme in patients with Wernicke-Korsakoff syndrome. N Engl J Med 1977;297:1367–1370.
Mukherjee AB, Svoronos S, Ghazanfari A, Martin PR, Fisher A, Roecklein B, et al. Transketolase abnormality in cultured fibroblasts from familial chronic alcoholic men and their male offspring. J Clin Invest 1987;79:1039–1043.
Torvik A. Two types of brain lesions in Wernicke’s encephalopathy. Neuropathol Appl Neurobiol 1985;11:179–190.
Pihko H, Saarinen U, Paetau A. Wernicke encephalopathy—a preventable cause of death: report of 2 children with malignant disease. Pediatr Neurol 1989;5:237–242.
Vasconcelos MM, Silva KP, Vidal G, Silva AF, Domingues RC, Berditchevsky CR. Early diagnosis of pediatric Wernicke’s encephalopathy. Pediatr Neurol 1999;20:289–294.
Zuccoli G, Siddiqui N, Bailey A, Bartoletti SC. Neuroimaging findings in pediatric Wernicke encephalopathy: a review. Neuroradiology 2010;52:523–529.
Guerrero RM. Wernicke syndrome due to vitamin B deficiency; report of the disease in two infants. Am J Dis Child 1949;78:88–96.
Davis RA, Wolf A. Infantile beriberi associated with Wernicke encephalopathy. Pediatrics 1958;21:409–420.
Seear MD, Norman MG. Two cases of Wernicke encephalopathy in children: an underdiagnosed complication of poor nutrition. Ann Neurol 1988;24:85–87.
Cochrane WA, Collins-Willims C, Donohue WL. Superior hemorrhagic polioencephalitis (Wernicke disease) occurring in an infant-probably due to thiamine deficiency from use of a soya bean product. Pediatrics 1961;28:771–777.
Peters TE, Parvin M, Petersen C, Faircloth VC, Levine RL. A case report of Wernicke’s encephalopathy in a pediatric patient with anorexia nervosa-restricting type. J Adolesc Health 2007;40:376–383.
Watanabe S, Yamakura S, Hirano K, Okumura Y, Aiba H. Case of infantile autism with pediatric Wernicke’s encephalopathy due to severe eating disorder. No To Hattatsu 2009;41:43–46. [In Japanese]
Gropman AL, Gaillard WD, Campbell P, Charya SV. Wernicke’s encephalopathy due to self starvation in a child. Lancet 1998;351:1704–1705.
Tanphaichitr V. Thiamine. In: Shils ME, Olson JA, Shike M, Ross AC, eds. Modern nutrition in health and disease, 9th ed. Baltimore: Williams & Wilkins, 1999: 381–389.
Friel JK, Andrews WL, Simmons BS, L’Abbe MR, Mercer C, MacDonald A, et al. Evaluation of full-term infants fed an evaporated milk formula. Acta Paediatr 1997;86:448–453.
Zeljko K, Darija VB, Dina LK, Marko B. Wernicke’s encephalopathy during parenteral nutrition in a Crohn’s disease patient. Nutrition 2011;27:503–504.
Basit S, Elsås T, Kvistad KA, Høsøien LS. Wernicke’s encephalopathy because of pancreatitis in a young boy. Acta Ophthalmol 2011;89:e656–e657.
Bohnert B. Wernicke’s encephalopathy in gastropancreatic disease with pyloric stenosis. Dtsch Med Wochenschr 1982;107:1722–1725. [In German]
Shah N, Wolff JA. Thiamine deficiency: Probable Wernicke’s encephalopathy successfully treated in a child with acute lymphocytic leukemia. Pediatrics 1973;51:750–751.
Onodera N, Nakahata T, Tanaka H, Ito R, Honda T. Successful treatment of Wernicke’s encephalopathy in a boy with acute mixed lineage leukemia. Acta Paediatr Jpn 1998;40:271–274.
Lim YJ, Kim HJ, Lee YJ, Seol IJ, Lee YH. Clinical features of encephalopathy in children with cancer requiring cranial magnetic resonance imaging. Pediatr Neurol 2011;44:433–438.
Mintz M. Clinical comparison of adult and pediatric NeuroAIDS. Adv Neuroimmunol 1994;4:207–221.
Nishida M, Sato H, Kobayashi N, Morimoto M, Hamaoka K. Wernicke’s encephalopathy in a patient with nephrotic syndrome. Eur J Pediatr 2009;168:731–734.
Baracco R, Ku L, Adabala M, Jain A, Valentini RP, Mattoo TK, et al. An adolescent on peritoneal dialysis with acute encephalopathy. Pediatr Nephrol 2013;28:1221–1225.
Han JW, Lim S, Shin HS, Park HJ, Jung WJ, Kwon SY, et al. Two cases of Wernicke encephalopathy in young age patients receiving allogeneic hematopoietic stem cell transplantation. Yonsei Med J 2012;53:1049–1053.
Muwakkit S, Al-Aridi C, Saab R, Hourani R, Yazbeck N, Abboud M. Wernicke encephalopathy during total parenteral nutrition in a child with acute lymphoblastic leukemia and acute pancreatitis. Neuropediatrics 2009;40:249–251.
Hahn JS, Berquist W, Alcorn DM, Chamberlain L, Bass D. Wernicke encephalopathy and beriberi during total parenteral nutrition attributable to multivitamin infusion shortage. Pediatrics 1998;101:E10.
Perko R, Harreld JH, Helton KJ, Sabin ND, Haidar CE, Wright KD. What goes around comes around? Wernicke encephalopathy and the nationwide shortage of intravenous multivitamins revisited. J Clin Oncol 2012;30:e318–e320.
McLean J, Manchip S. Wernicke’s encephalopathy induced by magnesium depletion. Lancet 1999;353:1768.
Pérez-Dueñas B, Serrano M, Rebollo M, Muchart J, Gargallo E, Dupuits C, et al. Reversible lactic acidosis in a newborn with thiamine transporter-2 deficiency. Pediatrics 2013;131: e1670–e1675.
Kono S, Miyajima H, Yoshida K, Togawa A, Shirakawa K, Suzuki H. Mutations in a thiamine-transporter gene and Wernicke’s-like encephalopathy. N Engl J Med 2009;360:1792–1794.
Sechi G, Serra A. Wernicke’s encephalopathy: new clinical settings and recent advances in diagnosis and management. Lancet Neurol 2007;6:442–455.
Cefalo MG, Ioris MA, Cacchione A, Longo D, Staccioli S, Arcioni F, et al. Wernicke encephalopathy in pediatric neurooncology: presentation of 2 cases and review of literature. J Child Neurol 2013 Nov 28. [Epub ahead of print]
Leigh D, McBurney A, McIlwain H. Erythrocyte transketolase activity in the Wernicke-Korsakoff syndrome. Br J Psychiatry 1981;139:153–156.
Doolman R, Dinbar A, Sela BA. Improved measurement of transketolase activity in the assessment of “TPP effect”. Eur J Clin Chem Clin Biochem 1995;33:445–446.
Kuriyama M, Yokomine R, Arima H, Hamada R, Igata A. Blood vitamin B1, transketolase and thiamine pyrophosphate (TPP) effect in beriberi patients, with studies employing discriminant analysis. Clin Chim Acta 1980;108:159–168.
Ming X, Wang MM, Zee D, Katz RM, Freeman JM. Wernicke’s encephalopathy in a child with prolonged vomiting. J Child Neurol 1998;13:187–189.
Fattal-Valevski A, Kesler A, Sela BA, Nitzan-Kaluski D, Rotstein M, Mesterman R, et al. Outbreak of life-threatening thiamine deficiency in infants in Israel caused by a defective soybased formula. Pediatrics 2005;115:e233–e238.
Zuccoli G, Santa Cruz D, Bertolini M, Rovira A, Gallucci M, Carollo C, et al. MR imaging findings in 56 patients with Wernicke encephalopathy: nonalcoholics may differ from alcoholics. AJNR Am J Neuroradiol 2009;30:171–176.
Zuccoli G, Pipitone N. MR Imaging: an increasingly important tool in the early diagnosis of Wernicke encephalopathy. AJNR Am J Neuroradiol 2012;33:E92.
Coe M, Carfagnini F, Tani G, Ambrosetto P. Wernicke’s encephalopathy in a child: case report and MRI findings. Pediatr Radiol 2001;31:167–168.
Sparacia G, Banco A, Lagalla R. Reversible MRI abnormalities in an unusual paediatric presentation of Wernicke’s encephalopathy. Pediatr Radiol 1999;29:581–584.
Zhong C, Jin L, Fei G. MR Imaging of nonalcoholic Wernicke encephalopathy: a follow-up study. AJNR Am J Neuroradiol 2005;26:2301–2305.
Kornreich L, Bron-Harlev E, Hoffmann C, Schwarz M, Konen O, Schoenfeld T, et al. Thiamine deficiency in infants: MR findings in the brain. AJNR Am J Neuroradiol 2005;26:1668–1674.
Rodan LH, Mishra N, Tein I. MR spectroscopy in pediatric Wernicke encephalopathy. Neurology 2013;80:969.
Seear M, Lockitch G, Jacobson B, Quigley G, MacNab A. Thiamine, riboflavin and pyridoxine deficiencies in a population of critically ill children. J Pediatr 1992;121:533–538.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lallas, M., Desai, J. Wernicke encephalopathy in children and adolescents. World J Pediatr 10, 293–298 (2014). https://doi.org/10.1007/s12519-014-0506-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-014-0506-9