Abstract
Objective
This study compared the masses and amounts of intramuscular non-contractile tissue of the trunk and lower extremity muscles, sagittal spinal alignment, and mobility and balance ability between patients with Parkinson’s disease (PD) and older adults.
Methods
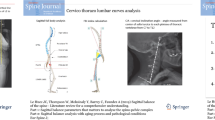
This study included 26 older adults (control [CTR] group) and eight patients with PD (PD group). Muscle thicknesses and echo intensities of the trunk and lower extremity muscles were measured using an ultrasound imaging device. Sagittal spinal alignments in the standing and prone positions were assessed using a Spinal Mouse. Mobility capacity was assessed based on the measurements of usual and maximal walking speeds, timed up-and-go (TUG) time, and five-chair-stand time, while balance ability was assessed based on the measurement of one-legged stance (OLS) time.
Results
Our results showed significantly lower gluteus maximus and tibialis anterior muscle thicknesses, higher thickness of the short head of the biceps femoris muscle, and higher echo intensity of the gluteus maximus muscle in the PD group than in the CTR group. Lumbar lordosis angle in the standing position, usual and maximal walking speeds, and OLS time were significantly lower, while the TUG and five-chair-stand times were significantly higher in the PD group than in the CTR group. The other factors did not differ significantly between groups.
Conclusions
Our results revealed lower masses of the gluteus maximus and tibialis anterior muscles, higher mass of the short head of the biceps femoris muscle, and higher amounts of intramuscular non-contractile tissue of the gluteus maximus muscle in patients with PD.



Similar content being viewed by others
References
Dickson DW (2018) Neuropathology of Parkinson disease. Parkinsonism Relat Disord 46:S30-33
Wirdefeldt K, Adami HO, Cole P, Trichopoulos D, Mandel J (2011) Epidemiology and etiology of Parkinson’s disease: a review of the evidence. Eur J Epidemiol 26:S1-58
Hess CW, Hallett M (2017) The phenomenology of Parkinson’s disease. Semin Neurol 37:109–117
Paul SS, Canning CG, Sherrington C, Fung VS (2012) Reduced muscle strength is the major determinant of reduced leg muscle power in Parkinson’s disease. Parkinsonism Relat Disord 18:974–977
Allen NE, Sherrington C, Canning CG, Fung VS (2010) Reduced muscle power is associated with slower walking velocity and falls in people with Parkinson’s disease. Parkinsonism Relat Disord 16:261–264
Paul SS, Sherrington C, Fung VS, Canning CG (2013) Motor and cognitive impairments in Parkinson disease: relationships with specific balance and mobility tasks. Neurorehabil Neural Repair 27:63–71
Inkster LM, Eng JJ, MacIntyre DL, Stoessl AJ (2003) Leg muscle strength is reduced in Parkinson’s disease and relates to the ability to rise from a chair. Mov Disord 18:157–162
Pang MY, Mak MK (2012) Influence of contraction type, speed, and joint angle on ankle muscle weakness in Parkinson’s disease: implications for rehabilitation. Arch Phys Med Rehabil 93:2352–2359
Wang CK, Chen HL, Lu CH, Chen MH, Chiang PL, Chen YS, Lin WC (2019) Altered body composition of psoas and thigh muscles in relation to frailty and severity of Parkinson’s disease. Int J Environ Res Public Health 16:3667
Ota M, Ikezoe T, Kaneoka K, Ichihashi N (2012) Age-related changes in the thickness of the deep and superficial abdominal muscles in women. Arch Gerontol Geriatr 55:e26-30
Ikezoe T, Mori N, Nakamura M, Ichihashi N (2012) Effects of age and inactivity due to prolonged bed rest on atrophy of trunk muscles. Eur J Appl Physiol 112:43–48
Ikezoe T, Mori N, Nakamura M, Ichihashi N (2011) Atrophy of the lower limbs in elderly women: is it related to walking ability? Eur J Appl Physiol 111:989–995
Ikezoe T, Mori N, Nakamura M, Ichihashi N (2011) Age-related muscle atrophy in the lower extremities and daily physical activity in elderly women. Arch Gerontol Geriatr 53:e153-157
Ota M, Ikezoe T, Kato T, Tateuchi H, Ichihashi N (2020) Age-related changes in muscle thickness and echo intensity of trunk muscles in healthy women: comparison of 20–60s age groups. Eur J Appl Physiol 120:1805–1814
Ikezoe T, Asakawa Y, Fukumoto Y, Tsukagoshi R, Ichihashi N (2012) Associations of muscle stiffness and thickness with muscle strength and muscle power in elderly women. Geriatr Gerontol Int 12:86–92
Miyatani M, Kanehisa H, Ito M, Kawakami Y, Fukunaga T (2004) The accuracy of volume estimates using ultrasound muscle thickness measurements in different muscle groups. Eur J Appl Physiol 91:264–272
Reimers K, Reimers CD, Wagner S, Paetzke I, Pongratz DE (1993) Skeletal muscle sonography: a correlative study of echogenicity and morphology. J Ultrasound Med 12:73–77
Pillen S, Tak RO, Zwarts MJ, Lammens MM, Verrijp KN, Arts IM, van der Laak JA, Hoogerbrugge PM, van Engelen BG, Verrips A (2009) Skeletal muscle ultrasound: correlation between fibrous tissue and echo intensity. Ultrasound Med Biol 35:443–446
Fukumoto Y, Ikezoe T, Yamada Y, Tsukagoshi R, Nakamura M, Mori N, Kimura M, Ichihashi N (2012) Skeletal muscle quality assessed from echo intensity is associated with muscle strength of middle-aged and elderly persons. Eur J Appl Physiol 112:1519–1525
Hoehn MM, Yahr MD (1967) Parkinsonism: onset, progression and mortality. Neurology 17:427–442
Movement Disorder Society Task Force on Rating Scales for Parkinson’s Disease (2003) The Unified Parkinson’s Disease Rating Scale (UPDRS): status and recommendations. Mov Disord 18:738–750
Louis ED, Lynch T, Marder K, Fahn S (1996) Reliability of patient completion of the historical section of the Unified Parkinson’s Disease Rating Scale. Mov Disord 11:185–192
Siderowf A, McDermott M, Kieburtz K, Blindauer K, Plumb S, Shoulson I, Parkinson Study Group (2002) Test-retest reliability of the unified Parkinson’s disease rating scale in patients with early Parkinson’s disease: results from a multicenter clinical trial. Mov Disord 17:758–763
Masaki M, Ikezoe T, Fukumoto Y, Minami S, Tsukagoshi R, Sakuma K, Ibuki S, Yamada Y, Kimura M, Ichihashi N (2015) Association of sagittal spinal alignment with thickness and echo intensity of lumbar back muscles in middle-aged and elderly women. Arch Gerontol Geriatr 61:197–201
Moreau NG, Teefey SA, Damiano DL (2009) In vivo muscle architecture and size of the rectus femoris and vastus lateralis in children and adolescents with cerebral palsy. Dev Med Child Neurol 51:800–806
Umegaki H, Ikezoe T, Nakamura M, Nishishita S, Kobayashi T, Fujita K, Tanaka H, Ichihashi N (2015) The effect of hip rotation on shear elastic modulus of the medial and lateral hamstrings during stretching. Man Ther 20:134–137
Ikezoe T, Nakamura M, Shima H, Asakawa Y, Ichihashi N (2015) Association between walking ability and trunk and lower-limb muscle atrophy in institutionalized elderly women: a longitudinal pilot study. J Physiol Anthropol 34:31
Hebert JJ, Koppenhaver SL, Parent EC, Fritz JM (2009) A systematic review of the reliability of rehabilitative ultrasound imaging for the quantitative assessment of the abdominal and lumbar trunk muscles. Spine (Phila Pa 1976) 34:E848-856
Guermazi M, Ghroubi S, Kassis M, Jaziri O, Keskes H, Kessomtini W, Ben Hammouda I, Elleuch MH (2006) Validity and reliability of Spinal Mouse to assess lumbar flexion. Ann Readapt Med Phys 49:172–177
Kellis E, Adamou G, Tzilios G, Emmanouilidou M (2008) Reliability of spinal range of motion in healthy boys using a skin-surface device. J Manipulative Physiol Ther 31:570–576
Masaki M, Ikezoe T, Kamiya M, Araki K, Isono R, Kato T, Kusano K, Tanaka M, Sato S, Hirono T, Kita K, Tsuboyama T, Ichihashi N (2018) Association of activities of daily living with load during step ascent motion in nursing home-residing elderly individuals: an observational study. Am J Phys Med Rehabil 97:715–720
Yoshiko A, Kaji T, Kozuka T, Sawazaki T, Akima H (2021) Evaluation of rehabilitation exercise effects by using gradation-based skeletal muscle echo intensity in older individuals: a one-group before-and-after trial study. BMC Geriatr 21:485
Sofuwa O, Nieuwboer A, Desloovere K, Willems AM, Chavret F, Jonkers I (2005) Quantitative gait analysis in Parkinson’s disease: comparison with a healthy control group. Arch Phys Med Rehabil 86:1007–1013
Cioni M, Richards CL, Malouin F, Bedard PJ, Lemieux R (1997) Characteristics of the electromyographic patterns of lower limb muscles during gait in patients with Parkinson’s disease when OFF and ON L-Dopa treatment. Ital J Neurol Sci 18:195–208
Stevens-Lapsley J, Kluger BM, Schenkman M (2012) Quadriceps muscle weakness, activation deficits, and fatigue with Parkinson disease. Neurorehabil Neural Repair 26:533–541
Doherty KM, van de Warrenburg BP, Peralta MC, Silveira-Moriyama L, Azulay JP, Gershanik OS, Bloem BR (2011) Postural deformities in Parkinson’s disease. Lancet Neurol 10:538–549
Ashour R, Jankovic J (2006) Joint and skeletal deformities in Parkinson’s disease, multiple system atrophy, and progressive supranuclear palsy. Mov Disord 21:1856–1863
Margraf NG, Rohr A, Granert O, Hampel J, Drews A, Deuschl G (2015) MRI of lumbar trunk muscles in patients with Parkinson’s disease and camptocormia. J Neurol 262:1655–1664
Cole MH, Naughton GA, Silburn PA (2017) Neuromuscular impairments are associated with impaired head and trunk stability during gait in Parkinson fallers. Neurorehabil Neural Repair 31:34–47
Mak MK, Pang MY (2009) Balance confidence and functional mobility are independently associated with falls in people with Parkinson’s disease. J Neurol 256:742–749
Thompson M, Medley A (1998) Performance of individuals with Parkinson’s disease on the timed up & go. J Neurol Phys Ther 22:16–21
Kawami Y, Marumoto K, Shiomi Y, Okinishi M, Kozuki T, Oyabu H, Yokoyama K, Nikaido Y, Akisue T (2018) The effect of comprehensive physiotherapy-based rehabilitation on stooped posture in Parkinson’s disease. J Phys Ther Sci 30:1440–1445
Scandalis TA, Bosak A, Berliner JC, Helman LL, Wells MR (2001) Resistance training and gait function in patients with Parkinson’s disease. Am J Phys Med Rehabil 80:38–43
Yang WC, Wang HK, Wu RM, Lo CS, Lin KH (2016) Home-based virtual reality balance training and conventional balance training in Parkinson’s disease: a randomized controlled trial. J Formos Med Assoc 115:734–743
Lorefält B, Toss G, Granérus AK (2009) Weight loss, body fat mass, and leptin in Parkinson’s disease. Mov Disord 24:885–890
Acknowledgements
The authors wish to thank all of the individuals who participated in the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Masaki, M., Kasahara, M., Takeuchi, M. et al. Comparison of the mass and amount of intramuscular non-contractile tissue of the trunk and lower extremity muscles between patients with Parkinson’s disease and community-dwelling older adults. Neurol Sci 43, 3629–3640 (2022). https://doi.org/10.1007/s10072-021-05828-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05828-5