Abstract
Background
Longitudinal data are limited on systemic lupus erythematosus (SLE) hospitalizations. We aim to study longitudinal trends of SLE hospitalizations in the last 2 decades in the United States (U.S).
Methods
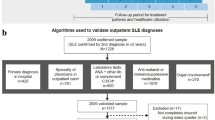
Data were obtained from the National Inpatient Sample database (NIS). We performed a 21-year longitudinal trend analysis of NIS 1998–2018. We searched for hospitalizations for adult patients with a “principal” diagnosis of SLE (SLE flare group) and those with “any” diagnosis of SLE (all SLE hospitalization group) using ICD codes. All non-SLE hospitalizations for adult patients were used as the control. Multivariable logistic and linear regression were used appropriately to calculate adjusted p-trend for the outcomes of interest.
Results
Incidence of SLE flare hospitalization reduced from 4.1 to 3.2 per 100,000 U.S persons from 1998 to 2018 (adjusted p-trend < 0.0001). The proportion of all hospitalized patients with SLE admitted principally for SLE reduced from 11.3% in 1998 to 5.7% in 2018 (adjusted p-tend < 0.0001). The proportion of hospitalized blacks in the SLE flare and all SLE hospitalization groups increased from 37.7% and 26.9% in 1998 to 44.7% and 30.7% in 2018 respectively (adjusted p-trend < 0.0001). The proportion of hospitalized Hispanics and Asians disproportionally increased in SLE flare hospitalizations compared to the control group.
Conclusion
The incidence of hospitalization for SLE flare has reduced in the last 2 decades in the U.S. The proportion of hospitalized patients with SLE admitted principally for SLE has reduced significantly over time. However, the burden of SLE hospitalizations among ethnic minorities has increased over time.
Key Points • The incidence of hospitalization for SLE flare has reduced in the last 2 decades in the U.S. • The proportion of hospitalized patients with SLE admitted principally for SLE has reduced significantly over time. • The burden of SLE hospitalizations among ethnic minorities such as blacks has increased over time. |


Similar content being viewed by others
References
Anastasiou C, Trupin L, Glidden DV, Li J, Gianfrancesco M, Shiboski S, Schmajuk G, Yazdany J (2021) Mortality among hospitalized individuals with systemic lupus erythematosus in the US between 2006 and 2016. Arthritis Care Res 73(10):1444–1450. https://doi.org/10.1002/acr.24356
HCUP databases. https://www.hcup-us.ahrq.gov. Assessed 14 October 2022
HCUP method series. https://www.hcup-us.ahrq.gov/reports/methods/TrendReport2005_1.pdf. Assessed 14 October 2022
United States Census Bureu. https://www.census.gov/data.html. Assessed 14 October 2022
Medical expenditure panel survey-based factor for hospital care. https://www.meps.ahrq.gov/mepsweb/. Assessed 14 October 2022
Lupus | CDC. https://www.cdc.gov/lupus/index.htm. Assessed 14 October 2022
Li S, Gong T, Peng Y, Nieman KM, Gilbertson DT (2020) Prevalence and incidence of systemic lupus erythematosus and associated outcomes in the 2009–2016 US Medicare population. Lupus 29(1):15–26. https://doi.org/10.1177/0961203319888691
Barber M, Drenkard C, Falasinnu T, Hoi A, Mak A, Kow NY, Svenungsson E, Peterson J, Clarke AE, Ramsey-Goldman R (2021) Global epidemiology of systemic lupus erythematosus. Nat Rev Rheumatol 17(9):515–532. https://doi.org/10.1038/s41584-021-00668-1
Alarcón GS, Calvo-Alén J, McGwin G Jr, Uribe AG, Toloza SM, Roseman JM, Fernández M, Fessler BJ, Vilá LM, Ahn C, Tan FK, Reveille JD, LUMINA Study Group (2006) Systemic lupus erythematosus in a multiethnic cohort: LUMINA XXXV. Predictive factors of high disease activity over time. Ann Rheum Dis 65(9):1168–1174. https://doi.org/10.1136/ard.200X.046896
González LA, Toloza SM, McGwin G Jr, Alarcón GS (2013) Ethnicity in systemic lupus erythematosus (SLE): its influence on susceptibility and outcomes. Lupus 22(12):1214–1224. https://doi.org/10.1177/0961203313502571
Maidhof W, Hilas O (2012) Lupus: an overview of the disease and management options. P T: Peer-Revi J Form Manag 37(4):240–249
Hannah J, Galloway J, Kaul A (2019) Changing hospitalization trends for systemic lupus erythematosus and rheumatoid arthritis in England. Lupus 28(7):906–913. https://doi.org/10.1177/0961203319853357
Piga M, Casula L, Perra D, Sanna S, Floris A, Antonelli A, Cauli A, Mathieu A (2016) Population-based analysis of hospitalizations in a West-European region revealed major changes in hospital utilization for patients with systemic lupus erythematosus over the period 2001–2012. Lupus 25(1):28–37. https://doi.org/10.1177/0961203315596597
Menard LC, Habte S, Gonsiorek W, Lee D, Banas D, Holloway DA, Manjarrez-Orduno N, Cunningham M, Stetsko D, Casano F, Kansal S, Davis PM, Carman J, Zhang CK, Abidi F, Furie R, Nadler SG, Suchard SJ (2016) B cells from African American lupus patients exhibit an activated phenotype. JCI insight 1(9):e87310. https://doi.org/10.1172/jci.insight.87310
Dubey AK, Handu SS, Dubey S, Sharma P, Sharma KK, Ahmed QM (2011) Belimumab: first targeted biological treatment for systemic lupus erythematosus. J Pharmacol Pharmacother 2(4):317–319. https://doi.org/10.4103/0976-500X.85930
Hasan B, Fike A, Hasni S (2022) Health disparities in systemic lupus erythematosus-a narrative review. Clin Rheumatol 41(11):3299–3311. https://doi.org/10.1007/s10067-022-06268-y
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Edigin, E., Trang, A., Ojemolon, P.E. et al. Longitudinal trends of systemic lupus erythematous hospitalizations in the United States: a two-decade population-based study. Clin Rheumatol 42, 695–701 (2023). https://doi.org/10.1007/s10067-022-06418-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-022-06418-2