Abstract
Objective
Adult-onset Still’s disease (AOSD) is a systemic inflammatory disorder with clinical heterogeneity. Although tocilizumab (TCZ), an interleukin (IL)-6 receptor inhibitor, is an effective treatment for AOSD, the evidence regarding its efficacy on systemic or articular subtypes is conflicting. Furthermore, the predictors of therapeutic response are still elusive and worthy of exploration.
Methods
This two-center retrospective study analyzed the effectiveness and safety profile of TCZ treatment in 28 patients with refractory AOSD. The 28-joint disease activity score (DAS28) and systemic activity score were assessed before and during TCZ treatment period at weeks 12, 24, 36, and 48. Plasma levels of proinflammatory cytokines at baseline were determined using ELISA method.
Results
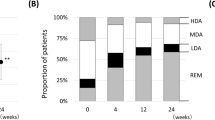
Among the systemic subtype patients, 10 (58.8%), 13 (76.5%), 14 (82.4%), and 15 (88.2%) patients achieved complete remission at week 12, 24, 36, and 48, respectively, in comparison to 2 (22.2%), 5 (55.6%), 6 (66.7%), and 7 (77.8%) who achieved disease remission (DAS28 < 2.6) at weeks 12, 24, 36, and 48, respectively, among articular subtype patients. The systemic activity scores and inflammatory parameters were significantly decreased after 12-week TCZ therapy, and TCZ could significantly reduce corticosteroid dose in AOSD patients. Multivariate analysis reveals that baseline IL-18 level is a significant predictor of poor therapeutic response at week 24 (odds ratio 7.86, p < 0.05).
Conclusion
AOSD patients refractory to high-dose corticosteroids and methotrexate may respond well to TCZ treatment with a steroid-sparing effect and an acceptable safety. A high baseline IL-18 level may be a predictor of poor therapeutic response.
Key Points • Tocilizumab may be effective and well-tolerated in refractory AOSD patients regardless of disease subtypes. • High plasma levels of IL-18 may predict poor response to tocilizumab in AOSD patients. |


Similar content being viewed by others
References
Ohta A, Yamaguchi M, Kaneoka H, Nagayoshi T, Hiida M (1987) Adult Still’s disease: review of 228 cases from the literature. J Rheumatol 14(6):1139–1146
Kadavath S, Efthimiou P (2015) Adult-onset Still’s disease-pathogenesis, clinical manifestations, and new treatment options. Ann Med 47(1):6–14. https://doi.org/10.3109/07853890.2014.971052
Lenert A, Yao Q (2016) Macrophage activation syndrome complicating adult onset Still’s disease: a single center case series and comparison with literature. Semin Arthritis Rheum 45(6):711–716. https://doi.org/10.1016/j.semarthrit.2015.11.002
Yoo DH (2017) Treatment of adult-onset Still’s disease: up to date. Expert Rev Clin Immunol 13(9):849–866. https://doi.org/10.1080/1744666X.2017.1332994
Castaneda S, Blanco R, Gonzalez-Gay MA (2016) Adult-onset Still’s disease: advances in the treatment. Best Pract Res Clin Rheumatol 30(2):222–238. https://doi.org/10.1016/j.berh.2016.08.003
Kalyoncu U, Solmaz D, Emmungil H et al (2016) Response rate of initial conventional treatments, disease course, and related factors of patients with adult-onset Still’s disease: data from a large multicenter cohort. J Autoimmun 69:59–63. https://doi.org/10.1016/j.jaut.2016.02.010
Choi JH, Suh CH, Lee YM et al (2003) Serum cytokine profiles in patients with adult onset Still’s disease. J Rheumatol 30(11):2422–2427
Kawaguchi Y, Terajima H, Harigai M, Hara M, Kamatani N (2001) Interleukin-18 as a novel diagnostic marker and indicator of disease severity in adult-onset Still’s disease. Arthritis Rheum 44(7):1716–1717. https://doi.org/10.1002/1529-0131(200107)44:7%3c1716::AID-ART298%3e3.0.CO;2-I
Chen DY, Chen YM, Lan JL, Lin CC, Chen HH, Hsieh CW (2010) Potential role of Th17 cells in the pathogenesis of adult-onset Still’s disease. Rheumatology (Oxford) 49(12):2305–2312. https://doi.org/10.1093/rheumatology/keq284
Hsieh CW, Chen YM, Lin CC et al (2017) Elevated expression of the NLRP3 inflammasome and its correlation with disease activity in adult-onset Still disease. J Rheumatol 44(8):1142–1150. https://doi.org/10.3899/jrheum.161354
Feist E, Mitrovic S, Fautrel B (2018) Mechanisms, biomarkers and targets for adult-onset Still’s disease. Nat Rev Rheumatol 14(10):603–618. https://doi.org/10.1038/s41584-018-0081-x
Inoue N, Shimizu M, Tsunoda S, Kawano M, Matsumura M, Yachie A (2016) Cytokine profile in adult-onset Still’s disease: comparison with systemic juvenile idiopathic arthritis. Clin Immunol 169:8–13. https://doi.org/10.1016/j.clim.2016.05.010
Sfriso P, Bindoli S, Galozzi P (2018) Adult-onset Still’s disease: molecular pathophysiology and therapeutic advances. Drugs 78(12):1187–1195. https://doi.org/10.1007/s40265-018-0956-9
Puechal X, DeBandt M, Berthelot JM et al (2011) Tocilizumab in refractory adult Still’s disease. Arthritis Care Res (Hoboken) 63(1):155–159. https://doi.org/10.1002/acr.20319
de Boysson H, Fevrier J, Nicolle A, Auzary C, Geffray L (2013) Tocilizumab in the treatment of the adult-onset Still’s disease: current clinical evidence. Clin Rheumatol 32(1):141–147. https://doi.org/10.1007/s10067-012-2105-2
Ortiz-Sanjuan F, Blanco R, Calvo-Rio V et al (2014) Efficacy of tocilizumab in conventional treatment-refractory adult-onset Still’s disease: multicenter retrospective open-label study of thirty-four patients. Arthritis Rheumatol 66(6):1659–1665. https://doi.org/10.1002/art.38398
Nishina N, Kaneko Y, Kameda H, Takeuchi T (2015) The effect of tocilizumab on preventing relapses in adult-onset Still’s disease: a retrospective, single-center study. Mod Rheumatol 25(3):401–404. https://doi.org/10.3109/14397595.2014.973659
Bannai E, Yamashita H, Kaneko S et al (2016) Successful tocilizumab therapy in seven patients with refractory adult-onset Still’s disease. Mod Rheumatol 26(2):297–301. https://doi.org/10.3109/14397595.2014.899178
Song ST, Kim JJ, Lee S et al (2016) Efficacy of tocilizumab therapy in Korean patients with adult-onset Still’s disease: a multicentre retrospective study of 22 cases. Clin Exp Rheumatol 34(6 Suppl 102):S64–S71
Li T, Gu L, Wang X et al (2017) A pilot study on tocilizumab for treating refractory adult-onset Still’s disease. Sci Rep 7(1):13477. https://doi.org/10.1038/s41598-017-13639-y
Wang CY, Guo SH, Wang LP, Shen HL (2019) Refractory adult-onset Still disease treated by tocilizumab combined with methotrexate: a STROBE-compliant article. Medicine (Baltimore) 98(32):e16682. https://doi.org/10.1097/MD.0000000000016682
Castaneda S, Martinez-Quintanilla D, Martin-Varillas JL, Garcia-Castaneda N, Atienza-Mateo B, Gonzalez-Gay MA (2019) Tocilizumab for the treatment of adult-onset Still’s disease. Expert Opin Biol Ther 19(4):273–286. https://doi.org/10.1080/14712598.2019.1590334
Ma Y, Wu M, Zhang X et al (2018) Efficacy and safety of tocilizumab with inhibition of interleukin-6 in adult-onset Still’s disease: a meta-analysis. Mod Rheumatol 28(5):849–857. https://doi.org/10.1080/14397595.2017.1416924
Kaneko Y, Kameda H, Ikeda K et al (2018) Tocilizumab in patients with adult-onset Still’s disease refractory to glucocorticoid treatment: a randomised, double-blind, placebo-controlled phase III trial. Ann Rheum Dis 77(12):1720–1729. https://doi.org/10.1136/annrheumdis-2018-213920
Franchini S, Dagna L, Salvo F, Aiello P, Baldissera E, Sabbadini MG (2010) Efficacy of traditional and biologic agents in different clinical phenotypes of adult-onset Still’s disease. Arthritis Rheum 62(8):2530–2535. https://doi.org/10.1002/art.27532
Maria AT, Le Quellec A, Jorgensen C, Touitou I, Riviere S, Guilpain P (2014) Adult onset Still’s disease (AOSD) in the era of biologic therapies: dichotomous view for cytokine and clinical expressions. Autoimmun Rev 13(11):1149–1159. https://doi.org/10.1016/j.autrev.2014.08.032
Vercruysse F, Barnetche T, Lazaro E et al (2019) Adult-onset Still’s disease biological treatment strategy may depend on the phenotypic dichotomy. Arthritis Res Ther 21(1):53. https://doi.org/10.1186/s13075-019-1838-6
Yamaguchi M, Ohta A, Tsunematsu T et al (1992) Preliminary criteria for classification of adult Still’s disease. J Rheumatol 19(3):424–430
Rau M, Schiller M, Krienke S, Heyder P, Lorenz H, Blank N (2010) Clinical manifestations but not cytokine profiles differentiate adult-onset Still’s disease and sepsis. J Rheumatol 37(11):2369–2376. https://doi.org/10.3899/jrheum.100247
Prevoo ML, van ’t Hof MA, Kuper HH, van Leeuwen MA, van de Putte LB, van Riel PL (1995) Modified disease activity scores that include twenty-eight-joint counts. Development and validation in a prospective longitudinal study of patients with rheumatoid arthritis. Arthritis Rheum 38(1):44–48. https://doi.org/10.1002/art.1780380107
Smolen JS, Aletaha D, Bijlsma JW et al (2010) Treating rheumatoid arthritis to target: recommendations of an international task force. Ann Rheum Dis 69(4):631–637. https://doi.org/10.1136/ard.2009.123919
CTEP cancer therapy evaluation program (2017) Common Terminology Criteria for Adverse Events (CTCAE) versions 5.0. National Cancer Institute. https://ctep.cancer.gov/protocoldevelopment/electronic_applications/ctc.htm#ctc_50. Accessed 17 August 2021
Cipriani P, Ruscitti P, Carubbi F et al (2014) Tocilizumab for the treatment of adult-onset Still’s disease: results from a case series. Clin Rheumatol 33(1):49–55. https://doi.org/10.1007/s10067-013-2381-5
Yoshida Y, Sakamoto M, Yokota K, Sato K, Mimura T (2011) Tocilizumab improved both clinical and laboratory manifestations except for interleukin-18 in a case of multiple drug-resistant adult-onset Still’s disease. Intern Med 50(16):1757–1760. https://doi.org/10.2169/internalmedicine.50.4771
Kir S, Ozgen M, Zontul S (2021) Adult-onset Still’s disease and treatment results with tocilizumab. Int J Clin Pract 75(3):e13936. https://doi.org/10.1111/ijcp.13936
Mercan R, Bitik B, Tufan A et al (2016) The association between neutrophil/lymphocyte ratio and disease activity in rheumatoid arthritis and ankylosing spondylitis. J Clin Lab Anal 30(5):597–601. https://doi.org/10.1002/jcla.21908
Seo JY, Suh CH, Jung JY, Kim AR, Yang JW, Kim HA (2017) The neutrophil-to-lymphocyte ratio could be a good diagnostic marker and predictor of relapse in patients with adult-onset Still’s disease: a STROBE-compliant retrospective observational analysis. Medicine (Baltimore) 96(29):e7546. https://doi.org/10.1097/MD.0000000000007546
Zhou S, Qiao J, Bai J, Wu Y, Fang H (2018) Biological therapy of traditional therapy-resistant adult-onset Still’s disease: an evidence-based review. Ther Clin Risk Manag 14:167–171. https://doi.org/10.2147/TCRM.S155488
Ortiz-Sanjuan F, Blanco R, Riancho-Zarrabeitia L et al (2015) Efficacy of anakinra in refractory adult-onset Still’s disease: multicenter study of 41 patients and literature review. Medicine (Baltimore) 94(39):e1554. https://doi.org/10.1097/MD.0000000000001554
Yoo DH (2019) Biologics for the treatment of adult-onset Still’s disease. Expert Opin Biol Ther 19(11):1173–1190. https://doi.org/10.1080/14712598.2019.1652591
Ichida H, Kawaguchi Y, Sugiura T et al (2014) Clinical manifestations of adult-onset Still’s disease presenting with erosive arthritis: association with low levels of ferritin and interleukin-18. Arthritis Care Res (Hoboken) 66(4):642–646. https://doi.org/10.1002/acr.22194
Nam SW, Kang SM, Lee JH, Yoo DH (2021) Different features of interleukin-37 and interleukin-18 as disease activity markers of adult-onset Still’s disease. J Clin Med 10(5):910. https://doi.org/10.3390/jcm10050910
Jung KH, Kim JJ, Lee JS et al (2014) Interleukin-18 as an efficient marker for remission and follow-up in patients with inactive adult-onset Still’s disease. Scand J Rheumatol 43(2):162–169. https://doi.org/10.3109/03009742.2013.824023
Tsuchida Y, Sumitomo S, Shoda H, Kubo K, Fujio K, Yamamoto K (2017) Macrophage activation syndrome associated with tocilizumab treatment in adult-onset Still’s disease. Mod Rheumatol 27(3):556–557. https://doi.org/10.1080/14397595.2016.1221875
Kobayashi M, Takahashi Y, Yamashita H, Kaneko H, Mimori A (2011) Benefit and a possible risk of tocilizumab therapy for adult-onset Still’s disease accompanied by macrophage-activation syndrome. Mod Rheumatol 21(1):92–96. https://doi.org/10.1007/s10165-010-0348-9
Wang R, Li T, Ye S et al (2020) Macrophage activation syndrome associated with adult-onset Still’s disease: a multicenter retrospective analysis. Clin Rheumatol 39(8):2379–2386. https://doi.org/10.1007/s10067-020-04949-0
Yamabe T, Ohmura SI, Uehara K, Naniwa T (2021) Macrophage activation syndrome in patients with adult-onset Still’s disease under tocilizumab treatment: a single-center observational study. Mod Rheumatol:1–8. https://doi.org/10.1080/14397595.2021.1899565
Ruscitti P, Iacono D, Ciccia F et al (2018) Macrophage activation syndrome in patients affected by adult-onset Still disease: analysis of survival rates and predictive factors in the Gruppo Italiano di Ricerca in Reumatologia Clinica e Sperimentale Cohort. J Rheumatol 45(6):864–872. https://doi.org/10.3899/jrheum.170955
Acknowledgements
The authors thank Shiow-Jiuan Wey, MD, of the Chung Shan Medical University Hospital, Taiwan, for manuscript editing. The authors also thank the Biostatistics Task Force of Taichung Veterans General Hospital, Taichung, Taiwan.
Author information
Authors and Affiliations
Contributions
K-TT and C-WH contributed equally on this work, conceived the study, acquired the clinical data, performed the data analysis, and drafted and revised the manuscript. Both Y-MC, S-HC, and H-HC performed the clinical assessment as well as data acquisition and statistical analysis. P-HH and J-LL performed the clinical assessments on study subjects and conducted the analysis of data. D-YC conceived and designed the study, generated the original hypothesis, acquired the clinical data, performed the data analysis, and also revised the manuscript.
Corresponding author
Ethics declarations
Disclosures
None.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tang, KT., Hsieh, CW., Chen, HH. et al. The effectiveness of tocilizumab in treating refractory adult-onset Still’s disease with dichotomous phenotypes: IL-18 is a potential predictor of therapeutic response. Clin Rheumatol 41, 557–566 (2022). https://doi.org/10.1007/s10067-021-05921-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-021-05921-2