Abstract
Context
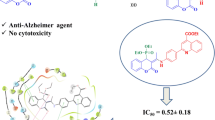
Alzheimer’s disease (AD) is a chronic progressive neurodegenerative syndrome, which adversely disturbs cognitive abilities as well as intellectual processes and frequently occurs in the elderly. Inhibition of cholinesterase is a valuable approach to upsurge acetylcholine concentrations in the brain and persuades the development of multi-targeted ligands against cholinesterases.
Methods
The current study aims to determine the binding potential accompanied by antioxidant and anti-inflammatory activities of stilbenes-designed analogs against both cholinesterases (Acetylcholinesterase and butyrylcholinesterase) and neurotrophin targets for effective AD therapeutics. Docking results have shown that the WS6 compound exhibited the least binding energy − 10.1 kcal/mol with Acetylcholinesterase and − 7.8 kcal/mol with butyrylcholinesterase. The WS6 also showed a better binding potential with neurotrophin targets that are Brain-derived Neurotrophic Factor, Neurotrophin 4, Nerve Growth Factor, and Neurotrophin 3. The tested compounds particularly WS6 revealed significant antioxidant and anti-inflammatory activities through the comparative docking analysis with Fluorouracil and Melatonin as control drugs of antioxidants while Celecoxib and Anakinra as anti-inflammatory. The bioinformatics approaches including molecular docking calculations followed by the pharmacokinetics analysis and molecular dynamic simulations were accomplished to explore the capabilities of designed stilbenes as effective and potential leads. Root mean square deviation, root mean square fluctuations, and MM-GBSA calculations were performed through molecular dynamic simulations to extract the structural and residual variations and binding free energies through the 50-ns time scale.







Similar content being viewed by others
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on request.
References
Wan Y-W, Al-Ouran R, Mangleburg CG, Perumal TM, Lee TV, Allison K, Swarup V, Funk CC, Gaiteri C, Allen M (2020) Meta-analysis of the Alzheimer’s disease human brain transcriptome and functional dissection in mouse models. Cell Rep 32:107908
De Virgilio A, Greco A, Fabbrini G, Inghilleri M, Rizzo MI, Gallo A, Conte M, Rosato C, Appiani MC, De Vincentiis M (2016) Parkinson’s disease: autoimmunity and neuroinflammation. Autoimmun Rev 15:1005–1011
McColgan P, Tabrizi SJ (2018) Huntington’s disease: a clinical review. Eur J Neurol 25:24–34
Sangeet S, Khan A (2021) In-silico studies of Neurocognitive and Neuropharmacological effect of Bacopa monnieri (L.). bioRxiv
Verdile G, Keane KN, Cruzat VF, Medic S, Sabale M, Rowles J, Wijesekara N, Martins RN, Fraser PE, Newsholme P (2015) Inflammation and oxidative stress: the molecular connectivity between insulin resistance, obesity, and Alzheimer’s disease. Mediators of inflammation 2015
Cho T, Ryu JK, Taghibiglou C, Ge Y, Chan AW, Liu L, Lu J, McLarnon JG, Wang YT (2013) Long-term potentiation promotes proliferation/survival and neuronal differentiation of neural stem/progenitor cells. PLoS One 8:e76860
Fitzsimons CP, Van Bodegraven E, Schouten M, Lardenoije R, Kompotis K, Kenis G, Van Den Hurk M, Boks MP, Biojone C, Joca S (2014) Epigenetic regulation of adult neural stem cells: implications for Alzheimer’s disease. Mol Neurodegener 9:1–21
Chao MV (2003) Neurotrophins and their receptors: a convergence point for many signalling pathways. Nat Rev Neurosci 4:299–309
Simmons DA (2017) Modulating neurotrophin receptor signaling as a therapeutic strategy for Huntington’s disease. J Huntingt Dis 6:303–325
Low LE, Wang Q, Chen Y, Lin P, Yang S, Gong L, Lee J, Siva SP, Goh B-H, Li F (2021) Microenvironment-tailored nanoassemblies for the diagnosis and therapy of neurodegenerative diseases. Nanoscale 13:10197–10238
Jiang Y, Fay JM, Poon CD, Vinod N, Zhao Y, Bullock K, Qin S, Manickam DS, Yi X, Banks WA (2018) Nanoformulation of Brain-Derived Neurotrophic Factor with Target Receptor-Triggered-Release in the Central Nervous System. Adv Func Mater 28:1703982
Goedert M, Spillantini MG (2006) A century of Alzheimer’s disease. science 314:777–781
Patterson C (2018) World Alzheimer Report 2018: the state of the art of dementia research: new frontiers. Alzheimer’s Disease International (ADI): London, UK
Talesa VN (2001) Acetylcholinesterase in Alzheimer’s disease. Mech Ageing Dev 122:1961–1969
Greenough MA, Camakaris J, Bush AI (2013) Metal dyshomeostasis and oxidative stress in Alzheimer’s disease. Neurochem Int 62:540–555
Selkoe DJ (2003) Folding proteins in fatal ways. Nature 426:900–904
Lamie PF, Abdel-Fattah MM, Philoppes JN (2022) Design and synthesis of new indole drug candidates to treat Alzheimer’s disease and targeting neuro-inflammation using a multi-target-directed ligand (MTDL) strategy. J Enzyme Inhib Med Chem 37:2660–2678
Bonda DJ, Wang X, Perry G, Nunomura A, Tabaton M, Zhu X, Smith MA (2010) Oxidative stress in Alzheimer disease: a possibility for prevention. Neuropharmacology 59:290–294
Schelterns P, Feldman H (2003) Treatment of Alzheimer’s disease; current status and new perspectives. Lancet Neurol 2:539–547
Gold PE (2003) Acetylcholine modulation of neural systems involved in learning and memory. Neurobiol Learn Mem 80:194–210
Thompson S, Lanctôt KL, Herrmann N (2004) The benefits and risks associated with cholinesterase inhibitor therapy in Alzheimer’s disease. Expert Opin Drug Saf 3:425–440
Khan MB, Khan MM, Khan A, Ahmed ME, Ishrat T, Tabassum R, Vaibhav K, Ahmad A, Islam F (2012) Naringenin ameliorates Alzheimer’s disease (AD)-type neurodegeneration with cognitive impairment (AD-TNDCI) caused by the intracerebroventricular-streptozotocin in rat model. Neurochem Int 61:1081–1093
da Silva AA, Goncalves RC (2010) Reactive oxygen species and the respiratory tract diseases of large animals/Especies reativas do oxigenio e as doencas respiratorias em grandes animais. Ciência Rural 40:994–1003
de Almeida RB, Barbosa DB, Bomfim do MR, Amparo JA, Andrade BS, Costa SL, Campos JM, Cruz JN, Santos CB, Leite FH (2023) Identification of a Novel Dual Inhibitor of Acetylcholinesterase and Butyrylcholinesterase: In Vitro and In Silico Studies. Pharmaceuticals 16:95
Tahir RA, Sehgal SA, Khattak NA, Khan Khattak JZ, Mir A (2013) Tumor necrosis factor receptor superfamily 10B (TNFRSF10B): an insight from structure modeling to virtual screening for designing drug against head and neck cancer. Theor Biol Med Model 10:38. https://doi.org/10.1186/1742-4682-10-38
Tahir RA, Hassan F, Kareem A, Iftikhar U, Sehgal SA (2019) Ligand-Based Pharmacophore Modeling and Virtual Screening to Discover Novel CYP1A1 Inhibitors. Curr Top Med Chem 19:2782–2794. https://doi.org/10.2174/1568026619666191112104217
Tahir RA, Sehgal SA (2018) Pharmacoinformatics and Molecular Docking Studies Reveal Potential Novel Compounds Against Schizophrenia by Target SYN II. Comb Chem High Throughput Screen 21:175–181. https://doi.org/10.2174/1386207321666180213092018
Tahir RA, Wu H, Javed N, Khalique A, Khan SAF, Mir A, Ahmed MS, Barreto GE, Qing H, Ashraf GM et al (2019) Pharmacoinformatics and molecular docking reveal potential drug candidates against Schizophrenia to target TAAR6. J Cell Physiol 234:13263–13276. https://doi.org/10.1002/jcp.27999
Sehgal SA, Hammad MA, Tahir RA, Akram HN, Ahmad F (2018) Current Therapeutic Molecules and Targets in Neurodegenerative Diseases Based on in silico Drug Design. Curr Neuropharmacol 16:649–663. https://doi.org/10.2174/1570159X16666180315142137
Tahir RA, Wu H, Rizwan MA, Jafar TH, Saleem S, Sehgal SA (2018) Immunoinformatics and molecular docking studies reveal potential epitope-based peptide vaccine against DENV-NS3 protein. J Theor Biol 459:162–170. https://doi.org/10.1016/j.jtbi.2018.10.005
Waqas M, Haider A, Rehman A, Qasim M, Umar A, Sufyan M, Akram HN, Mir A, Razzaq R, Rasool D et al (2021) Immunoinformatics and Molecular Docking Studies Predicted Potential Multiepitope-Based Peptide Vaccine and Novel Compounds against Novel SARS-CoV-2 through Virtual Screening. Biomed Res Int 2021:1596834. https://doi.org/10.1155/2021/1596834
Rose PW, Beran B, Bi C, Bluhm WF, Dimitropoulos D, Goodsell DS, Prlić A, Quesada M, Quinn GB, Westbrook JD (2010) The RCSB Protein Data Bank: redesigned web site and web services. Nucleic Acids Res 39:D392–D401
Pettersen EF, Goddard TD, Huang CC, Couch GS, Greenblatt DM, Meng EC, Ferrin TE (2004) UCSF Chimera—a visualization system for exploratory research and analysis. J Comput Chem 25:1605–1612
MOE (2013) Molecular Operating Environment (MOE).
Zielesny A (2005) Chemistry Software Package ChemOffice Ultra 2005ACS Publications.
Trott O, Olson AJ (2010) AutoDock Vina: improving the speed and accuracy of docking with a new scoring function, efficient optimization, and multithreading. J Comput Chem 31:455–461
Lima AdM, Siqueira AS, Möller MLS, Souza RCd, Cruz JN, Lima ARJ, Silva RCd, Aguiar DCF, Junior JLdSGV, Gonçalves EC (2022) In silico improvement of the cyanobacterial lectin microvirin and mannose interaction. J Biomol Struct Dyn 40:1064–1073
Almeida VM, Dias ÊR, Souza BC, Cruz JN, Santos CB, Leite FH, Queiroz RF, Branco A (2022) Methoxylated flavonols from Vellozia dasypus Seub ethyl acetate active myeloperoxidase extract: in vitro and in silico assays. J Biomol Struct Dyn 40:7574–7583
Bowers KJ, Chow DE, Xu H, Dror RO, Eastwood MP, Gregersen BA, Klepeis JL, Kolossvary I, Moraes MA, Sacerdoti FD (2006) Scalable algorithms for molecular dynamics simulations on commodity clustersSC’06: Proceedings of the 2006 ACM/IEEE Conference on Supercomputing IEEE, pp. 43–43.
Ferreira LG, Dos Santos RN, Oliva G, Andricopulo AD (2015) Molecular docking and structure-based drug design strategies. Molecules 20:13384–13421
Hildebrand PW, Rose AS, Tiemann JK (2019) Bringing molecular dynamics simulation data into view. Trends Biochem Sci 44:902–913
Shivakumar D, Williams J, Wu Y, Damm W, Shelley J, Sherman W (2010) Prediction of absolute solvation free energies using molecular dynamics free energy perturbation and the OPLS force field. J Chem Theory Comput 6:1509–1519
Liang J-H, Yang L, Wu S, Liu S-S, Cushman M, Tian J, Li N-M, Yang Q-H, Zhang H-A, Qiu Y-J (2017) Discovery of efficient stimulators for adult hippocampal neurogenesis based on scaffolds in dragon’s blood. Eur J Med Chem 136:382–392
Gourie-Devi M (2014) Epidemiology of neurological disorders in India: Review of background, prevalence and incidence of epilepsy, stroke, Parkinson’s disease and tremors. Neurology India 62:588
Li YZ, Yang XL, Yan SL, Sun ZK (2023) Complexity decline of hippocampal CA1 circuit model due to cholinergic deficiency associated with Alzheimer’s disease. Cogn Neurodyn. https://doi.org/10.1007/s11571-023-09958-8
Yang H, Yang XL, Yan SL, Sun ZK (2022) Effect of acetylcholine deficiency on neural oscillation in a brainstem-thalamus-cortex neurocomputational model related with Alzheimer’s disease. Abst Sci Rep 12(1). https://doi.org/10.1038/s41598-022-19304-3
da Costa M, Bernardi J, Costa L, Fiuza T, Brandão R, Ribeiro MF, Amaral JD, Rodrigues CM, Pereira ME (2017) N-acetylcysteine treatment attenuates the cognitive impairment and synaptic plasticity loss induced by streptozotocin. Chem Biol Interact 272:37–46
Silva LB, Ferreira EF, Maryam E-R, Costa GV, Cruz JV, Kimani NM, Costa JS, Bittencourt JA, Cruz JN (2023) Galantamine Based Novel Acetylcholinesterase Enzyme Inhibitors: A Molecular Modeling Design Approach. Molecules 28:1035
Sahay A, Kale A, Joshi S (2020) Role of neurotrophins in pregnancy and offspring brain development. Neuropeptides 83:102075
Hempstead BL (2006) Dissecting the diverse actions of pro-and mature neurotrophins. Curr Alzheimer Res 3:19–24
Vilar M, Mira H (2016) Regulation of neurogenesis by neurotrophins during adulthood: expected and unexpected roles. Front Neurosci 10:26
Sahu MP, Pazos-Boubeta Y, Pajanoja C, Rozov S, Panula P, Castrén E (2019) Neurotrophin receptor Ntrk2b function in the maintenance of dopamine and serotonin neurons in zebrafish. Sci Rep 9:1–13
Autry AE, Bambah-Mukku D (2020) The role of brain-derived neurotrophic factor in neural circuit development and functionSynapse Development and Maturation Elsevier, pp. 443–466.
Allen SJ, Dawbarn D (2006) Clinical relevance of the neurotrophins and their receptors. Clin Sci 110:175–191
Meldolesi J (2017) Neurotrophin receptors in the pathogenesis, diagnosis and therapy of neurodegenerative diseases. Pharmacol Res 121:129–137
Konar A, Shah N, Singh R, Saxena N, Kaul SC, Wadhwa R, Thakur MK (2011) Protective role of Ashwagandha leaf extract and its component withanone on scopolamine-induced changes in the brain and brain-derived cells. PLoS One 6:e27265
Kim KH, Kim MA, Moon E, Kim SY, Choi SZ, Son MW, Lee KR (2011) Furostanol saponins from the rhizomes of Dioscorea japonica and their effects on NGF induction. Bioorg Med Chem Lett 21:2075–2078
Tseng P-T, Chen Y-W, Tu K-Y, Wang H-Y, Chung W, Wu C-K, Hsu S-P, Kuo H-C, Lin P-Y (2016) State-dependent increase in the levels of neurotrophin-3 and neurotrophin-4/5 in patients with bipolar disorder: a meta-analysis. J Psychiatr Res 79:86–92
GómezmezT C-W, Tu K-Y, Wang H-Y, Chung W, Wu C-K, Hsu S-P, Kuo H-C, Lin P-Y (2016) State-dependent increase in the levels of neurotrophin-3 and neurotrophin-4/5 in ’s disease. CNS Neurosci Ther 24:353–363
Yun J, Mullarky E, Lu C, Bosch KN, Kavalier A, Rivera K, Roper J, Chio IIC, Giannopoulou EG, Rago C (2015) Vitamin C selectively kills KRAS and BRAF mutant colorectal cancer cells by targeting GAPDH. Science 350:1391–1396
White PA, Oliveira RC, Oliveira AP, Serafini MR, Araújo AA, Gelain DP, Moreira JC, Almeida JR, Quintans JS, Quintans-Junior LJ (2014) Antioxidant activity and mechanisms of action of natural compounds isolated from lichens: a systematic review. Molecules 19:14496–14527
Reuter S, Gupta SC, Chaturvedi MM, Aggarwal BB (2010) Oxidative stress, inflammation, and cancer: how are they linked? Free Radical Biol Med 49:1603–1616
Dharmaraja AT (2017) Role of reactive oxygen species (ROS) in therapeutics and drug resistance in cancer and bacteria. J Med Chem 60:3221–3240
Yaribeygi H, Panahi Y, Javadi B, Sahebkar A (2018) The underlying role of oxidative stress in neurodegeneration: a mechanistic review. CNS & Neurological Disorders-Drug Targets (Formerly Current Drug Targets-CNS & Neurological Disorders) 17: 207–215
Chiurchiù V, Orlacchio A, Maccarrone M (2016) Is modulation of oxidative stress an answer? The state of the art of redox therapeutic actions in neurodegenerative diseases. Oxidative medicine and cellular longevity 2016
Agostinho P, Cunha RA, Oliveira C (2010) Neuroinflammation, oxidative stress and the pathogenesis of Alzheimer’s disease. Curr Pharm Des 16:2766–2778
Wang W-Y, Tan M-S, Yu J-T, Tan L (2015) Role of pro-inflammatory cytokines released from microglia in Alzheimer’s disease. Ann Trans Med 3
Aborode AT, Pustake M, Awuah WA, Alwerdani M, Shah P, Yarlagadda R, Ahmad S, Silva Correia IF, Chandra A, Nansubuga EP (2022) Targeting oxidative stress mechanisms to treat Alzheimer’s and Parkinson’s disease: a critical review. Oxidative Med Cell Longev 2022
Song Y, Zhu X-Y, Zhang X-M, Xiong H (2022) Targeted Mitochondrial Epigenetics: A New Direction in Alzheimer’s Disease Treatment. Int J Mol Sci 23:9703
Song J, Jia Y, Li J, Ding R, Yuan Y, Cai J, Su Y, Hua Q, Zhang Z (2022) LiuweiDihuang improved cognitive functions in SAMP8 mice by inhibiting COX-2 expression and subsequent neuroinflammation. J Ethnopharmacol 296:115491
Fang Y, Xia W, Cheng B, Hua P, Zhou H, Gu Q, Xu J (2018) Design, synthesis, and biological evaluation of compounds with a new scaffold as anti-neuroinflammatory agents for the treatment of Alzheimer’s disease. Eur J Med Chem 149:129–138
Tahir RA, Bashir A, Yousaf MN, Ahmed A, Dali Y, Khan S, Sehgal SA (2020) In Silico identification of angiotensin-converting enzyme inhibitory peptides from MRJP1. PloS One 15:e0228265
Tahir RA, Hassan F, Kareem A, Iftikhar U, Sehgal SA (2019) Ligand-based pharmacophore modeling and virtual screening to discover novel CYP1A1 inhibitors. Curr Top Med Chem 19:2782–2794
Hassan Baig M, Ahmad K, Roy S, Mohammad Ashraf J, Adil M, Haris Siddiqui M, Khan S, Amjad Kamal M, Provazník I, Choi I (2016) Computer aided drug design: Success and limitations. Curr Pharma Design 22:572–581
Funding
This work was supported by the National Natural Science Foundation of China (Grant Nos. 92049102, 32070954, 82001167, 81870844). We thank the Biological and Medical Engineering Core Facilities of the Beijing Institute of Technology for their support.
Author information
Authors and Affiliations
Contributions
Contributions based on CRediT taxonomy: Sundas Firdoos: conceptualization, writing — original draft, writing — review and editing, methodology, investigation; Rongji Dai: supervision, writing — review and editing, methodology, investigation; Rana Adnan Tahir: methodology, writing — review and editing, investigation; Zahid Younas Khan: methodology, writing — review and editing; Hui Li, Jun Zhang and Junjun Ni: writing — review and editing; Zhenzhen Quan: methodology, investigation, resources, writing — review and editing; Hong Qing: methodology, investigation, writing — review and editing, funding acquisition, supervision.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Firdoos, S., Dai, R., Tahir, R.A. et al. In silico identification of novel stilbenes analogs for potential multi-targeted drugs against Alzheimer’s disease. J Mol Model 29, 209 (2023). https://doi.org/10.1007/s00894-023-05609-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00894-023-05609-1