Abstract
Objective
This study aimed to examine the influence of immediate loading on the dynamic changes of bone metabolism around dental implants using a high-resolution semiconductor sodium 18F-fluoride (Na18F)-PET.
Methods
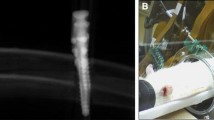
Tibiae of 12 adult male rats were divided into 4 groups: immediate loading (IL), no loading (NL), bone defect (BD), and control (CTR). For the IL group, a 4.0-N load was applied continuously by two closed-coil springs attached between two implants in tibia. Each rat received an intravenous injection of Na18F and was scanned by high-resolution Na18F-PET at day 1 and then at weeks 1, 2, 3, 4, 5, 6, and 8 after surgery. Bone metabolism around the implant was evaluated by standardized uptake value (SUV), which indicates the outcome of Na18F accumulation. CT scanning was also performed, and PET and CT images were superposed to determine the anatomical orientation in PET images.
Results
Bone metabolism peaked at 7 days after surgery and then gradually decreased in all three test groups (IL, NL, and BD). SUVs of all three test groups were significantly higher than the baseline at 1, 2, 3, and 4 weeks after surgery, with SUVs in the IL group returning to baseline levels earlier than those in the NL and BD groups.
Conclusions
Fluorine integrates preferentially with the initial low-calcified bone; thus, our results suggest that immediate loading promotes the calcification of the bone tissue in the early stage on peri-implant bone formation.
Clinical relevance
Na18F-PET allows for an estimate of bone metabolism change around the implant.



Similar content being viewed by others
References
Attard NJ, Zarb GA (2005) Immediate and early implant loading protocols: a literature review of clinical studies. J Prosthet Dent 94:242–258
Suito H, Tomotake Y, Watanabe M, Nagao D, Ishida Y, Ichikawa T (2011) Survival of immediate implant restoration: a retrospective study through 9-year-observation. J Prosthodont Res 55:141–145
Brunski JB (1999) In vivo bone response to biomechanical loading at the bone/dental-implant interface. Adv Dent Res 13:99–119
Rismanchian M, Movahedian B, Khalighinejad N, Badrian H, Mohammad Razavi S, Nekouie A (2012) Comparative evaluation of two types of immediately loaded implants using biomechanical and histomorphometric tests: an animal case study. ISRN Dent 2012:328945
Ogawa T, Vandamme K, Zhang X, Naert I, Possemiers T, Chaudhari A, Sasaki K, Duyck J (2014) Stimulation of titanium implant osseointegration through high-frequency vibration loading is enhanced when applied at high acceleration. Calcif Tissue Int 95(5):467–475
Schwartz Z, Shani J, Soskolne WA, Touma H, Amir D, Sela J (1993) Uptake and biodistribution of technetium-99m-MD32P during rat tibial bone repair. J Nucl Med 34:104–108
Blau M, Ganatra R, Bender MA (1972) 18 F-fluoride for bone imaging. Semin Nucl Med 2:31–37
Ogawa T, Zhang X, Naert I, Vermaelen P, Deroose CM, Sasaki K, Duyck J (2011) The effect of whole-body vibration on peri-implant bone healing in rats. Clin Oral Implants Res 22:302–307
Sasaki H, Koyama S, Yokoyama M, Yamaguchi K, Itoh M, Sasaki K (2008) Bone metabolic activity around dental implants under loading observed using bone scintigraphy. Int J Oral Maxillofac Implants 23:827–834
Yamamoto M, Ogawa T, Yokoyama M, Koyama S, Sasaki K (2014) Influence of immediate and early loading on bone metabolic activity around dental implants in rat tibiae. Clin Oral Implants Res 25(9):1084–1090
Ishii K, Kikuchi Y, Matsuyama S, Kanai Y, Kotani K, Ito T et al (2007) First achievement of less than 1 mm FWHM resolution in practical semiconductor animal PET scanner. Nuclear Instruments and Methods in Physics Research Section A: Accelerators, Spectrometers, Detectors and Associated Equipment 576:435–440
Gentleman E, Stevens MM, Hill RG, Brauer DS (2013) Surface properties and ion release from fluoride-containing bioactive glasses promote osteoblast differentiation and mineralization in vitro. Acta Biomater 9:5771–5779
Bi Y, Gao Y, Ehirchiou D et al (2010) Bisphosphonates cause osteonecrosis of the jaw-like disease in mice. Am J Pathol 177:280–290
Iwasashi M, Funayama T, Watanabe A, Noguchi H, Tsukanishi T, Suetsugu Y, Makihara T, Ochiai N, Yamazaki M, Sakane M (2015) Bone regeneration and remodeling within a unidirectional porous hydroxyapatite bone substitute at a cortical bone defect site: histological analysis at one and two years after implantation. Materials 8:4884–4894
Singer JD, Willett JB (2003) Applied longitudinal data analysis: modeling change and event occurrence. Part I. Oxford University Press, New York
Alsabeeha N, Atieh M, Payne AG (2010) Loading protocols for mandibular implant overdentures: a systematic review with meta-analysis. Clin Implant Dent Relat Res 12(Suppl 1):e28–e38
Grant FD, Fahey FH, Packard AB, Davis RT, Alavi A, Treves ST (2008) Skeletal PET with 18F-fluoride: applying new technology to an old tracer. J Nucl Med 49:68–78
Cheng C, Alt V, Pan L, Thormann U, Schnettler R, Strauss LG, Heinemann S, Schumacher M, Gelinsky M, Nies B, Dimitrakopoulou-Strauss A (2014) Application of F-18-sodium fluoride (NaF) dynamic PET-CT (dPET-CT) for defect healing: a comparison of biomaterials in an experimental osteoporotic rat model. Med Sci Monit 20:1942–1949
Toegel S, Hoffmann O, Wadsak W, Ettlinger D, Mien LK, Wiesner K, Nguemo J, Viernstein H, Kletter K, Dudczak R, Mitterhauser M (2006) Uptake of bone-seekers is solely associated with mineralisation! A study with 99mTc-MDP, 153Sm-EDTMP and 18F-fluoride on osteoblasts. Eur J Nucl Med Mol Imaging 33:491–494
Chen ZF, Darvell BW, Leung VW (2004) Hydroxyapatite solubility in simple inorganic solutions. Arch Oral Biol 49:359–367
Czernin J, Satyamurthy N, Schiepers C (2010) Molecular mechanisms of bone 18F-NaF deposition. J Nucl Med 51:1826–1829
Blake GM, Park-Holohan SJ, Cook GJ, Fogelman I (2001) Quantitative studies of bone with the use of 18F-fluoride and 99mTc-methylene diphosphonate. Semin Nucl Med 31:28–49
Acknowledgements
The authors are grateful to Dr. Hisashi Shinoda, a professor emeritus at Tohoku University Graduate School of Dentistry, for the important scientific advice. The authors are also grateful to Dr. Jun Aida, from the Department of International and Community Oral Health, Tohoku University Graduate School of Dentistry, for the assistance with statistical analysis. We also acknowledge the Research Team for Neuroimaging, Tokyo Metropolitan Institute of Gerontology, who lent facilities willingly as coworkers. The authors express gratitude to Hitachi Aloka Medical, for their support and use of the CT imaging scanner and fusion technology.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
This work was partially supported by Grants-in-Aid for Scientific Research (B) (grant no. 24390428), Grant-in-Aid for Young Scientists (B) (grant no. 24792130) from the Ministry of Education, Culture, Sports, Science and Technology, Japan and Research Seeds Quest Program (grant no. J110001441) from Japan Science and Technology Agency.
Ethical approval
This article does not contain any studies with human participants. Ethical approval (2012CrA-4) was provided by the Institutional Animal Use and Care Committee of Tohoku University.
Informed consent
For this type of study, formal consent is not required.
Additional information
Y.M. and T.O. equally contributed to this work.
Rights and permissions
About this article
Cite this article
Matsuo, Y., Ogawa, T., Yamamoto, M. et al. Evaluation of peri-implant bone metabolism under immediate loading using high-resolution Na18F-PET. Clin Oral Invest 21, 2029–2037 (2017). https://doi.org/10.1007/s00784-016-1992-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-016-1992-z