Abstract
Background and objectives
Mechanical thrombectomy (MT) has been established as the gold standard of treatment for patients with Acute Ischemic Stroke (AIS) who present up to 6 h after the onset of the stroke. Recently, the DEFUSE-3 and DAWN trials established the safety of starting the MT procedure up to 16 and 24 h after the patient was last seen well, respectively. The purpose of this study is to assess the safety and functional effects of thrombectomy in individuals with AIS detected at a late stage (> 24 h).
Materials and methods
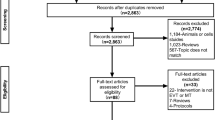
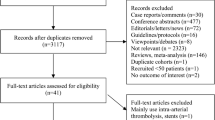
PubMed, Web of Science, Embase, and Cochrane databases were thoroughly searched for research on MT in patients in the extremely late time window after AIS. The primary outcomes were symptomatic cerebral hemorrhage, 90-day mortality, Thrombolysis in Cerebral Infarction (TICI) 2b-3, and Modified Rankin Scale (mRS) 0–2.
Results
Our study included fifteen studies involving a total of 1,221 patients who presented with AIS and an extended time window. The primary outcome of interest was the favorable functional outcome, mRS 0–2 at 90 days. The pooled proportion for this outcome was 45% (95% confidence interval 34–58%). Other outcomes included the TICI 2b or 3 (successful recanalization), which was reported in 12 studies and had a 79% incidence in the study population (95% CI 68–87%). Complications included: symptomatic intracranial hemorrhage (sICH), which revealed an incidence of 7% in the study population (95% CI 5–10%); and 90-day mortality, which reported a 27% incidence (95% CI 24–31%). In addition, we conducted a comparative analysis between endovascular treatment and standard medical therapy.
Conclusion
Our meta-analysis provides evidence that supports the need of further randomized and prospective clinical trials to better assess the effectiveness and safety of MT in these patients.












Similar content being viewed by others
Data availability
This meta-analysis used data from previously published studies, therefore all data and study materials are public domain. The meta-analysis authors do not have patient-level data from the various studies. Researchers interested in individual-level data from this meta-analysis should contact each study's corresponding author.
Abbreviations
- AIS:
-
Acute Ischemic Stroke
- ASPECT:
-
Alberta Stroke Program Early CT Score
- LVO:
-
Large vessel occlusion
- mRS:
-
Modified Rankin Score
- MT:
-
Mechanical thrombectomy
- NIHSS:
-
National Institute of Health Stroke Scale
- PRISMA:
-
Preferred reporting items for systematic reviews and meta-analyses
- PROSPERO:
-
International Prospective Register of Systematic Reviews
- sICH:
-
Symptomatic intracranial hemorrhage
- SMT:
-
Standard medical treatment
- TICI:
-
Thrombolysis in Cerebral Infarction
References
Albers GW, Marks MP, Kemp S et al (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med 378:708–718
Casetta I, Fainardi E, Pracucci G et al (2022) Endovascular treatment beyond 24 hours from the onset of acute ischemic stroke: the Italian Registry of Endovascular Thrombectomy in Acute Stroke (IRETAS). J Neurointerv Surg 14(12):1186–1188. https://doi.org/10.1136/neurintsurg-2021-018045
Desai SM, Haussen DC, Aghaebrahim A et al (2018) Thrombectomy 24 hours after stroke: beyond DAWN. J Neurointerv Surg 10(11):1039–1042. https://doi.org/10.1136/neurintsurg-2018-013923
Dhillon PS, Butt W, Podlasek A et al (2023) Endovascular thrombectomy beyond 24 hours from ischemic stroke onset: a propensity score matched cohort study. J Neurointerv Surg 15(3):233–237. https://doi.org/10.1136/neurintsurg-2021-018591
GBD 2019 Stroke Collaborators (2021) Global, regional, and national burden of stroke and its risk factors, 1990–2019: a systematic analysis for the global burden of disease study 2019. Lancet Neurol 20(10):795–820. https://doi.org/10.1016/S1474-4422(21)00252-0
Goyal M, Menon BK, van Zwam WH et al (2016) Endovascular thrombectomy after large-vessel ischaemic stroke: a meta-analysis of individual patient data from five randomized trials. Lancet 387:1723–1731
Ha SH, Ryu JC, Bae JH, Koo S, Kwon B, Lee DH, Chang JY, Kang DW, Kwon SU, Kim JS, Kim BJ (2023) Early response to endovascular thrombectomy after stroke: early, late, and very late time windows. Cerebrovasc Dis 52(1):28–35. https://doi.org/10.1159/000525083
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:13. https://doi.org/10.1186/1471-2288-5-13
Iezzi Z, Patel P, Wolfe J et al (2023) Outcomes following thrombectomy for acute large vessel occlusion beyond 24 hours or with unknown time of onset. J Stroke Cerebrovasc Dis 32(3):106952. https://doi.org/10.1016/j.jstrokecerebrovasdis.2022.106952
Janjua N, El-Gengaihy A, Pile-Spellman J, Qureshi AI (2009) Late endovascular revascularization in acute ischemic stroke based on clinical-diffusion mismatch. AJNR Am J Neuroradiol 30(5):1024–1027. https://doi.org/10.3174/ajnr.A1474
Kobeissi H, Ghozy S, Seymour T et al (2023) Outcomes of patients with atrial fibrillation following thrombectomy for stroke: a systematic review and meta-analysis. JAMA Netw Open 6(1):e2249993. https://doi.org/10.1001/jamanetworkopen.2022.49993
Liu S, Cao W, Wu L et al (2023) Endovascular treatment over 24 hours after ischemic stroke onset: a single-center retrospective study. Neuroradiology 65(4):793–804. https://doi.org/10.1007/s00234-022-03105-6
Manning NW, Wenderoth J, Alsahli K et al (2018) Endovascular thrombectomy >24-hr from stroke symptom onset. Front Neurol 9:501. https://doi.org/10.3389/fneur.2018.00501
Mohamed GA, Nogueira RG, Essibayi MA et al (2023) Tissue Clock Beyond Time Clock: Endovascular Thrombectomy for Patients With Large Vessel Occlusion Stroke Beyond 24 Hours. J Stroke 25(2):282–290. https://doi.org/10.5853/jos.2023.00017
Nogueira RG, Jadhav AP, Haussen DC et al (2018) Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med 378:11–21
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Pandhi A, Chandra R, Abdulrazzak MA et al (2023) Mechanical thrombectomy for acute large vessel occlusion stroke beyond 24 h. J Neurol Sci 447:120594. https://doi.org/10.1016/j.jns.2023.120594
Purrucker JC, Ringleb PA, Seker F et al (2022) Leaving the day behind: endovascular therapy beyond 24 h in acute stroke of the anterior and posterior circulation. Ther Adv Neurol Disord 15:17562864221101084. https://doi.org/10.1177/17562864221101083
Rai A, Cline B, Williams E, Carpenter J, Roberts T (2015) Intravenous thrombolysis outcomes in patients presenting with large vessel acute ischemic strokes–CT angiography-based prognosis. J Neuroimaging 25(2):238–242. https://doi.org/10.1111/jon.12126
Ren JX, Li C, Yan XL, Qu Y, Yang Y, Guo ZN (2021) Crosstalk between oxidative stress and ferroptosis/oxytosis in ischemic stroke: possible targets and molecular mechanisms. Oxid Med Cell Longev 2021:6643382. https://doi.org/10.1155/2021/6643382
Rodriguez-Calienes A, Galecio-Castillo M, Vivanco-Suarez J et al (2023) Endovascular thrombectomy beyond 24 hours from last known well: a systematic review with meta-analysis. J Neurointerv Surg. https://doi.org/10.1136/jnis-2023-020443
Sarraj A, Kleinig TJ, Hassan AE et al (2023) Association of endovascular thrombectomy vs medical management with functional and safety outcomes in patients treated beyond 24 hours of last known well: the select late study. JAMA Neurol 80(2):172–182. https://doi.org/10.1001/jamaneurol.2022.4714
Shaban A, Al Kasab S, Chalhoub RM et al (2023) Mechanical thrombectomy for large vessel occlusion strokes beyond 24 hours. J Neurointerv Surg. 15(e3):e331–e336. https://doi.org/10.1136/jnis-2022-019372
Sierra C, Coca A, Schiffrin EL (2011) Vascular mechanisms in the pathogenesis of stroke. Curr Hypertens Rep 13(3):200–207. https://doi.org/10.1007/s11906-011-0195-x
Yu Jia Z, Sun Song Y, Jon Sheen J, Goo Kim J, Hee LD (2019) Endovascular recanalization of symptomatic non-acute intracranial artery occlusion: Procedural and mid-term clinical outcomes in the anterior circulation. Interv Neuroradiol 25(4):380–389. https://doi.org/10.1177/1591019919826616
Zhang Y, He Y, Chen S et al (2021) Safety and efficacy of intravascular therapy in patients with progressive stroke caused by intracranial large vascular occlusion exceeding the time window of 24 hours. Neurol Res 43(12):1031–1039. https://doi.org/10.1080/01616412.2021.1948768
Acknowledgements
The authors would like to thank Rhanderson Cardoso, MD, for the support in conducting this research. We would also like to thank the Meta-Analysis Academy for immense support in the elaboration of this project.
Funding
This research did not receive any specific grant from any government, private, or non-profit funding source.
Author information
Authors and Affiliations
Contributions
Conception and design of the research: A.L.L.L., M.A.B.; Acquisition of data: A.L.L.L., F.C.G., and C.S.D.; Analysis and interpretation of the data: A.L.L.L., F.C.G., and C.S.D.; Writing of manuscript: all authors; Critical revision of the manuscript for intellectual content: all authors.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent to publication
Not applicable.
Conflict of interest
The authors declare no conflict of interest.
Disclosure of relationships and activities
All the authors contributed equally to this study’s conclusion.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Larcipretti, A.L.L., Gomes, F.C., Dagostin, C.S. et al. Is time really brain in stroke therapy?: A meta-analysis of mechanical thrombectomy up to 155 h post ictus. Acta Neurochir 166, 195 (2024). https://doi.org/10.1007/s00701-024-06070-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00701-024-06070-6