Abstract
Purpose
Lumbar discogenic diffuse pain is still not understood. Authors describe the sinuvertebral nerve (SVN) as one possible cause. Body-donor studies are rare and controversial. Therefore, the aim was to revisit the origin, course and distribution in a body-donor study.
Methods
Six lumbar blocks (3 female, 3 male) aged between 59 and 94 years were dissected. After removal of the back muscles, lamina, dura mater and cauda equina, the anterior vertebral venous plexus, spinal artery and SVN were exposed and evaluated.
Results
43 nerves out of 48 levels could be evaluated. The origin of the SVN was constituted by two roots: a somatic and a sympathetic branch arising from the rami communicantes. In 4/48 intervertebral canals studied (8.3%), we found two SVN at the same level. In 35/48 cases, one SVN was found. In 9/48 cases, no SVN was found. The SVN had a recurrent course below the inferior vertebral notch; in the vertebral canal it showed different patterns: ascending branch (31/43, 72.1%), common branch diverging into two branches (10/43, 23.3%), double ascending branch (1/43, 2.3%) finalizing two levels above and a descending branch (1/43, 2.3%). In 12/43 cases (27.9%) the SVN had ipsilateral connections with another SVN. The distribution ended in the middle of the vertebral body supplying adjacent structures.
Conclusion
A thorough understanding of the anatomy of the SVN might lead to significant benefits in therapy of discogenic low back pain. We suggest blocking the SVN at the level of the inferior vertebral notch of two adjacent segments.
Level of evidence I
Diagnostic: individual cross-sectional studies with consistently applied reference standard and blinding
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The sinuvertebral nerve (SVN) was first described in the nineteenth century by von Luschka as a nerve that enters in a recurrent course inside the vertebral foramen supplying the bone, disc, ligament, dura mater and veins [1].
Many authors described the SVN as one of the main contributing structures for lumbar discogenic pain [2,3,4,5,6,7,8,9,10,11]. Currently, chronic low back pain represents the second leading cause of disability worldwide, being a major welfare and economic problem [12, 13]. Even to date, the pathomechanism of this pain is still not precisely defined and understood neither anatomically [14,15,16] nor psychosocially [17].
Recently, blocking the SVN has proved successful in reducing the intensity and frequency of the lumbar diffuse pain. Various methods have been used such as analgesics, intradiscal electrothermal annuloplasty (IDET), transforaminal epiduroscopic laser ablation (TELA) or radiofrequency ablation of the SVN [10, 11, 18, 19]. Therefore, several diagnostic and treatment procedures have been developed in relation to the pathological effects of the SVN without having clear anatomical references to this nerve.
A review of the literature showed considerable variability regarding the specimens used in previous studies: human body-donors to science [2,3,4, 6,7,8, 20,21,22,23,24,25,26], foetuses and embryos [8, 20, 27,28,29], rats [30,31,32], mixed species [5] or undetermined samples [3]. Different techniques have also been used: dissections [3, 6, 20, 26, 33], histological examination [4, 5, 27], dissection combined with histology [2, 7, 8], immunohistochemistry [21, 23, 24, 29,30,31,32, 34] and dissection combined with immunohistochemistry [22, 25].
The SVN has been studied in the lumbar region [2, 6, 8, 25, 26], cervical [22], and cervicothoracic [3, 33] regions and at unspecified levels [7]. Considering only the lumbar dissection studies on human body-donors, the sample size is limited [6, 8].
The origin, course and distribution of the SVN have been discussed recently but they are still not consistent in the literature. Most authors define the origin as a neural branch emerging from the spinal nerve and a sympathetic postganglionic branch developing from the rami communicantes [2, 3, 7,8,9, 22, 27, 33]. In contrast, several studies define a single origin either as a spinal [3, 8] or a sympathetic branch [22, 25, 29, 34].
Different patterns of its course have been proposed: an ascending course [3, 6,7,8,9, 22, 25], a descending course [3, 7,8,9], a horizontal oblique course [2, 9] and a mixed course including an ascending and descending branch [7, 8, 27, 29,30,31]. A plexiform pattern has also been described [29,30,31, 34].
Multiple SVN exiting at the same segment have been reported [6, 7, 26, 27] although the literature is still not consistent [22, 34].
SVN branches tend to produce ipsilateral [7, 8, 29] or contralateral anastomoses [7, 8, 29,30,31], but non-anastomosing SVN branches have also been described [3, 6, 22, 25,26,27, 33].
Because the existing literature is inconsistent regarding the topography of SVN and in view of its increasing relevance to the treatment of chronic low back pain, the aim of our study was to clarify the different morphological aspects of the SVN in comparison to those in the literature.
Materials and methods
Six spine blocks (including vertebral bodies L3–S1), corresponding to six embalmed human body-donors belonging to the Body Donation Center and Dissection Rooms, Complutense University of Madrid, were dissected (three female and three male between 59 and 94 years of age).
The anterolateral and posterior lumbar region was dissected to identify the sympathetic trunk, the rami communicantes and the lumbar spinal nerves (Fig. 1a and b). The psoas major and erector spinae muscles were removed (Fig. 1b) to reveal the external origin of the SVN with its spinal and sympathetic root (Fig. 1).
a. First step in the left lateral approach to the lumbar spine: Identification of the sympathetic trunk (st) and rami communicantes (rc), between the psoas major muscle (pmm) and aorta (a) with lumbar arteries (la) and inferior vena cava (ivc). b. Second step in the lateral approach; after removing the psoas major muscle and the aorta have been removed, the connection of the rami communicantes (rc) with the ventral branches of the lumbar nerves (L3, L4, L5) can be observed. The black arrow shows the level of the sympathetic origin of the sinuvertebral nerve. cr: cranial, me: medial, la: lateral; ca: caudal
Once the anterolateral approach had been performed, the posterior lumbar region was dissected (Fig. 2). After the erector spinae muscles were removed, the laminae, the spinous and the articular processes were exposed (Fig. 2a). The vertebral arches were then removed using a saw and the vertebral canal was exposed to visualize the dura mater and the origin of the lumbar nerves (Fig. 2b). Consecutively, opening the dura mater revealed the pia mater enveloping the cauda equina (Fig. 2b).
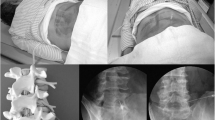
Steps in the posterior approach to the sinuvertebral nerve (arrows): a. Dissection and removal of the back muscles, exposing the lamina (la), spinal process (sp) and articular process (ap). b. After the vertebral arches are removed, severing the vertebral pedicles (pe) and opening the dura mater (d), the pia mater (p) and lumbar nerves (L3, L4, L5) can be seen. c. After the cauda equina and meninges are removed, the anterior vertebral venous plexus (*) can be observed covering the posterior longitudinal ligament, intervertebral discs and vertebral bodies. On the right side, the sinuvertebral nerves can be observed after declining the lumbar nerves (L3, L4, L5, S1) (SVN marked by black arrows). cr: cranial, ca:caudal
Subsequently, the posterior surface of the intervertebral disc and the vertebral body covered by the anterior vertebral venous plexus could be observed. Dissection was continued from the lateral to medial side to visualize the entire origin and course of the SVN in the intervertebral canal (Fig. 2c).
A surgical microscope (Zeiss-OMP1 0.6X–2.5X) was used to help the dissection.
Results
Forty-eight levels were dissected and forty-three SVN in 39 levels were observed (89.6%). Major factors limiting the dissection of all SVN included disruption by surrounding structures such as the venous plexus and microdissection per se.
The origin of the SVN was always formed by two roots: a somatic root arising from the spinal nerve and a sympathetic branch from the rami communicantes (Fig. 3).
Origin of the sinuvertebral nerve (SVN): a. View of the origin of the sympathetic root (arrow) arising from the ramus communicans (rc) of the sympathetic trunk (st) in the encircled area corresponding to the connection of the ramus communicantes with L4 and the origin of the sinuvertebral nerve (arrow) entering into the vertebral canal with the spinal artery (sa) branch of the lumbar artery (la), iliolumbar ligament (ill) and quadratus lumborum muscle (qlm). b. Posterior view of the lumbar spine after sectioning the vertebral pedicles (pe) and removing the vertebral arches. The intervertebral disc of the L4 segment (id) and posterior longitudinal ligament (pll) can be observed. The spinal and sympathetic roots (from L4 and ramus communicans (rc) make up the sinuvertebral nerve (svn). Cr: cranial, me: medial, la: lateral, ca: caudal
In 4 /48 intervertebral canals (8.3%), we found two SVN at the same level (Fig. 4a). In 35/48 intervertebral canals (72.9%), we found just one recognizable SVN (Fig. 4a). In 9/48 (18.75%), we found no SVN.
Posterior view on the posterior wall of the lumbar spine after dissection of the pedicles (pe); the posterior longitudinal ligament (pll), intervertebral disc (id) and posterior vertebral body of L5 are visible: a. On the left side, the sinuvertebral nerves (SVN) and their course (recurrent) can be seen. b. Segments L4 and L5, showing the anterior vertebral venous plexus (vp) covering the posterior wall of the lumbar spine. The spinal origins of the SVN can be seen as well as the proximity of the nerve to the inferior vertebral notch of the vertebral pedicle. The SVN of L4 is divided into two branches, ascending and descending. Cr: cranial, me: medial, la: lateral, ca: caudal
After the two branches united, the nerve entered the intervertebral canal near the inferior vertebral notch in a recurrent course (Figs. 3 and 4).
In 31 cases (72%), the SVN followed an ascending course that ended in the middle of the vertebral body covered by the posterior longitudinal ligament (Figs. 2c, 3, 4) (Table 2). In 10/43 SVN (23.3%), the nerve split into ascending and descending branches of equal length which ended at the midline (Fig. 4b). In 1/43 SVN (2.3%), the ascending branch ended two levels cranially. A descending course of the SVN ending in the inferior disc was observed in 1/43 cases (2.3%) (Figs. 5 and 6).
Sketch of possible courses and connections of the SVN; posterior views on the posterior wall of the lumbar spine: a. Right and left sides showing an ascending course of SVN ending in the middle of the vertebral body (covered by the posterior longitudinal ligament). b. On the right side the nerve splits into two branches: one ascending and one descending ending in the midline. c. The left side shows two SVN at the same vertebral canal. On the right side an ascending branch finalized in two superior vertebrae levels. d. The left side shows the ipsilateral connections between the 2 SVN. On the right side a descending branch
In every case, these nerves supplied the dura mater, the posterior longitudinal ligament, blood vessels of the epidural space, the annuli fibrosi, the vertebral bodies and the superior or inferior intervertebral disc, depending on the course. The SVN was closely related to the spinal artery (Fig. 4a) and surrounded by the anterior vertebral venous plexus (Fig. 4b).
We have found that the SVN connected ipsilaterally in 12/43 cases (27.9%) (Figs. 6 and 7).
Posterior view on the posterior wall of the lumbar spine after resection of the pedicles (pe) showing the posterior longitudinal ligament (pll), intervertebral disc and posterior vertebral body: a. Left side and b. Right segments of L4 and L5, showing the connections ("anastomoses") between the sinuvertebral nerves (svn). cr: cranial, me: medial, la: lateral, ca: caudal
Discussion
Previous methods
To best of our knowledge, 17/23 anatomical studies (73.9%) were based on human body-donors [2, 4, 6,7,8,9, 20,21,22,23,24,25,26,27,28,29, 33]. Four were based on a histological studies of human foetuses and embryos [8, 20, 27, 29]. The remaining articles used rats (4/23 articles [17.3%] [30,31,32, 34], human foetuses and rats (1/23 articles (4, 3%)) [5] or undefined specimen [3].
The above-mentioned studies focused on the cervical, thoracic or cervicothoracic level in 5/23 articles (21.7%) [5, 22, 27, 28, 33]; the segment investigated remained unspecified in 3/23 articles (13%) [3, 7, 29]. Fifteen of the 23 articles (65.2%) investigated the lumbar region [2, 4, 6, 8, 9, 20, 21, 23,24,25,26,27, 31, 32, 34]. Although the lumbar level represents the most frequently used spinal segment for investigating the course of the SVN, only 5/23 cases (21.7%) used human lumbar regions and a dissection technique to identify it [2, 6, 8, 25, 26].
Origin
The SVN double-origin hypothesis was supported by nine of the 23 articles identified in the literature review [2, 3, 7,8,9, 22, 26, 27, 33]. A single spinal branch was observed in 2/23 (8.7%) [3, 8] and an exclusively sympathetic branch in 5/23 (21.7%) articles [3, 22, 25, 29, 34] (Table 1).
The works of Kimmel et al. and Groen et al., evaluating lumbar blocks, do not describe the origin in detail using immunohistochemistry [27, 29].
A double origin, spinal and sympathetic, was found in 100% of the nerves in our sample (89.58% of the analysed levels), a higher incidence than in previous reports. The present results are consistent with most of the previously published literature using human body-donors to science and gross dissection for identifying the course of the SVN [2, 7, 8, 22, 26, 33].
None of the nerves examined in the present study had a single spinal origin. This result is not consistent with the study by Pedersen et al. using the same methods for following the course of the SVN (1/8, 12.5%) [8]. Nor could we find an exclusively sympathetic origin for the nerve in any of our specimen. Only two previous studies (2/8, 25%) reported a sympathetic origin of the SVN [22, 25].
Multiple SVN
In 5/23 (21.7%) cases, more than one SVN was described in the same segment [6, 7, 26, 27, 33]. In our sample, two SVN (8/43 SVN, 18.6%) could be described on the same level in only 4/48 intervertebral canals (8.33%). In 35/48 (72.9%), just one recognizable SVN. However, in 9/48 (18.75%) we found no SVN. (Fig. 8).
SVN diversity
Zhao et al. describe two types of a SVN [26]: Type I directly innervates the posterior lateral edge of the intervertebral disc or vertebral body. This SVN has been defined as a recurrent nerve entering the intervertebral canal. In contrast to the authors´ conclusion, we would rather classify type I SVN as small ramifications of the lateral lumbar region or a result of a dissection error. We found no type I SVN in our samples. There is no consistent evidence that the type I is really a nerve; it would be advisable to perform immunohistochemistry for confirmation.
In our sample, the SVN was always closely related to the spinal artery, coinciding with the type II SVN of Zhao et al. [26]. In contrast to the results of Zhao et al., the SVN was also surrounded by the anterior vertebral venous plexus and had different course patterns. These course patterns have been described by others: ascending in 7/23 articles (30.43%) [3, 6,7,8,9, 22, 25]; descending in 4/23 (17.4%) [3, 7,8,9]; a mixed pattern in 6/23 articles (26%) [7, 8, 27, 29,30,31]; an oblique trajectory in 2/23 cases (8.7%) [9, 15]; and a plexiform pattern in 4/23 (17.4%) [29,30,31, 34] (Table 2).
Course
Compared to the previous literature, our sample had more ascending courses (31/43, 72%), if the nerve was present, and the course was ascending in 31 of the 39 (79.49%) levels in which we could identify a SVN. There was a double ascending trajectory in one body-donor in L4 on the left side, representing one of 43 (2.32%) cases and one of 39 (2.56%) levels in which we could identify a SVN. Other authors found an ascending course in 6/8 cases (75%) [6, 8, 9, 22, 25]. A mixed pattern was found in 10/43 cases (23.25%) and in 10/39 (25.64%) levels with SVN´s identified. Two other groups also found a mixed course (2/8 articles, 25%) consistent with our results [7, 8]. Many mixed patterns have probably been considered ascending courses owing to difficulties in microdissections and because the ascending branch is easier to dissect as its limits are clearly marked by the upper pedicle. It should also be borne in mind that dissections of the SVN have proved very difficult owing to its size and its relationship to the anterior vertebral venous plexus.
Only in one case was a descending trajectory found, in L3 on the left side, representing 1/43 (2.32%) cases and 1/48 (2%) levels examined. These values are lower than reported by other authors. Among other human dissection studies, two groups have also found this descending course (2/8 articles, 25%) [7, 8].
No oblique trajectory was found in any of the nerves examined.
Anastomosis
Previous studies described anastomosis with the contralateral SVN in 5/23 (21.7%) cases [7, 8, 29,30,31] and ipsilateral anastomosis in 4/23 (17.4%) cases [7, 8, 29, 31]. We found ipsilateral anastomosis in 12/43 of our body-donors (27.9%), but no contralateral anastomosis. It should be noted that if we only consider the dissection studies on humans, two groups (2/8 cases, 25%) found anastomosis with contralateral and ipsilateral SVN [7, 8].
Clinical relevance
In healthy individuals, the intervertebral disc is only very weakly supplied at the posterior annulus fibrosus by primary sensory and sympathetic postganglionic fibres via the SVN. Particularly in the case of degenerative disc disease, the increased load leads to an inflammatory reaction and consequently the release of growth factors, resulting in increased sprouting of nerve fibres in the deeper layers of the disc [35,36,37]. Previous experimental studies have established a correlation between hyperinnervation of the annulus fibrosus by additional sprouting of the SVN and increased discogenic pain [38, 39].
Blockade of nerve conduction at this site is associated with an increased risk of complications owing to several relevant surrounding structures, which is why the definition of anatomical landmarks is essential [40]. The initial recurrent course of the SVN entering the intervertebral canal has not been described. However, in all the segments studied in our sample, the nerve was close to the inferior notch of the vertebral pedicle. Therefore, this location could be an elective landmark for infiltrating the nerve. SVN blockade can be effective in both diagnostic and therapeutic settings. Reports of significant improvements in low back pain with low complication rates are well known [41]. Especially when combined with a clear indication and imaging techniques and orientation to anatomical landmarks, this minimally invasive procedure can provide an effective alternative for treating chronic low back pain. Likewise, interim bridging of pain in elderly patients who cannot receive open surgery with lumbar instrumentation owing to their general condition is possible.
Conclusions
One possible cause of lumbar discogenic diffuse pain is the lumbar sinuvertebral nerve. Our results suggest a general pattern of the SVN with two different roots, spinal and sympathetic, and an initial recurrent course entering into the vertebral canal, just close to the inferior vertebral notch of the pedicle. The SVN can then follow different courses: an ascending course, a mixed course dividing into two branches (ascending and descending) or an exclusively descending course. These branches ended deep to the posterior longitudinal ligament after spreading among the adjacent structures. The terminal branches of the SVN had ipsilateral connections but they did not cross the midline; no contralateral connections were found. A thorough understanding of the anatomy of the SVN might lead to significant benefits in therapy of discogenic low back pain. We suggest blocking the SVN at the level of the inferior vertebral notch of two adjacent segments.
Change history
18 June 2021
A Correction to this paper has been published: https://doi.org/10.1007/s00586-021-06894-1
References
von Luschka DH, von Dr Hubert (1850) Die Nerven des menschlichen Wirbelkanales, Luschka, Laupp
Bogduk N, Tynan W, Wilson AS (1981) The nerve supply to the human lumbar intervertebral discs. J Anat 132:39–56
Hovelacque A (1925) Le nerf sinu-vertebral. Masson
Roofe PG (1940) Innervation of annulus fibrosus and posterior longitudinal ligament: fourth and fifth lumbar level. Arch Neurol Psychiatry 44:100–103
Van Buskirk C (1941) Nerves in the vertebral canal: their relation to the sympathetic innervation of the upper extremities. Arch Surg 43:427–432
Lazorthes G, Poulhes J, Espagno J (1947) Etude sur les nerfs sinu-vertebraux lombaires le nerf de roofe existe-t-il. CR Assoc Anat 34:317–320
Wiberg G (1949) Back pain in relation to the nerve supply of the intervertebral disc. Acta Orthop Scand 19:211–221
Pedersen HE, Blunck CF, Gardner E (1956) The anatomy of lumbosacral posterior rami and meningeal branches of spinal nerves (sinu-vertebral nerves): with an experimental study of their functions. JBJS 38:377–391
Bogduk N (1983) The innervation of the lumbar spine. Spine (Phila Pa 1976) 8(3):286–293
Schliessbach J, Siegenthaler A, Heini P, Bogduk N, Curatolo M (2010) Blockade of the sinuvertebral nerve for the diagnosis of lumbar diskogenic pain: an exploratory study. Anesth Analg 111:204–206
Shayota B, Wong TL, Fru D, David G, Iwanaga J, Loukas M, Tubbs RS (2019) A comprehensive review of the sinuvertebral nerve with clinical applications. Anat Cell Biol 52(2):128–133. https://doi.org/10.5115/acb.2019.52.2.128
Nachemson A (2004) Epidemiology and the economics of low back pain. In: Lippincott Williams , Wilkins, Philadelphia (3rd ed) .The lumbar spine
Vos T, Allen C, Arora M, Barber RM, Bhutta ZA, Brown A, Carter A, Casey DC, Charlson FJ, Chen AZ (2016) Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 388:1545–1602
García-Cosamalón J, Fernández-Fernández J, González-Martínez E, Ibáñez-Plágaro J, Robla CJ, Martínez-Madrigal M, López MA, del Valle M, Vega J (2013) Innervation of the intervertebral disc. Neurocirugia (Asturias, Spain) 24:121–129
Bogduk N, Aprill C, Derby R (2013) Lumbar discogenic pain: state-of-the-art review. Pain Med 14(6):813–836. https://doi.org/10.1111/pme.12082
Bogduk N (2016) Functional anatomy of the spine. In: Handbook of clinical neurology, Elsevier. pp 675–688
Joukamaa M (1987) Psychological factors in low back pain. Ann Clin Res
Kim HS, Kashlan ON, Singh R, Adsul NM, Yong Z, Oh SW, Noh JH, Jang IT, Oh SH (2019) Percutaneous transforaminal endoscopic radiofrequency ablation of the sinuvertebral nerve in an olympian with a Left L5 pedicle/pars interarticularis fracture-associated left L5–S1 disk desiccation. World Neurosurg X 3:100032. https://doi.org/10.1016/j.wnsx.2019.100032
Kim HS, Wu PH, Jang I-T (2020) Lumbar degenerative disease part 1: anatomy and pathophysiology of intervertebral discogenic pain and radiofrequency ablation of basivertebral and sinuvertebral nerve treatment for chronic discogenic back pain: a prospective case series and review of literature. Int J Mol Sci 21(4):1483. https://doi.org/10.3390/ijms21041483
Malinský J (1959) The ontogenetic development of nerve terminations in the intervertebral discs of man (histology of intervertebral discs, 11th communication). Cells Tiss Org 38:96–113
Korkala O, Grönblad M, Liesi P, Karaharju E (1985) Immunohistochemical demonstration of nociceptors in the ligamentous structures of the lumbar spine. Spine 10:156–157
Chen X, Bo S, Zhong S (1988) Nerves accompanying the vertebral artery and their clinical relevance. Spine 13:1360–1364
Coppes MH, Marani E, Thomeer RT, Groen GJ (1997) Innervation of" painful" lumbar discs. Spine 22:2342–2349
Palmgren T, Grönblad M, Virri J, Kääpä E, Karaharju E (1999) An immunohistochemical study of nerve structures in the anulus fibrosus of human normal lumbar intervertebral discs. Spine 24(20):2075–2079. https://doi.org/10.1097/00007632-199910150-00002
Raoul S, Faure A, Robert R, Rogez J-M, Hamel O, Cuillère P, Le Borgne J (2002) Role of the sinu-vertebral nerve in low back pain and anatomical basis of therapeutic implications. Surg Radiol Anat 24:366–370
Zhao Q, Cheng L, Yan H, Deng S, Zhao J, Liu Z, Tan X, Zhong E, Zhuo W, Jin D (2020) The anatomical study and clinical significance of the sinuvertebral nerves at the lumbar levels. Spine 45:E61–E66
Kimmel DL (1961) Innervation of spinal dura mater and dura mater of the posterior cranial fossa. Neurology 11:800–800
Groen G, Baljet B, Drukker J (1988) The innervation of the spinal dura mater: anatomy and clinical implications. Acta Neurochir 92:39–46
Groen GJ, Baljet B, Drukker J (1990) Nerves and nerve plexuses of the human vertebral column. Am J Anat 188:282–296
Kojima Y, Maeda T, Arai R, Shichikawa K (1990) Nerve supply to the posterior longitudinal ligament and the intervertebral disc of the rat vertebral column as studied by acetylcholinesterase histochemistry. I. Distribution in the lumbar region. J Anat 169:237–246
Nakamura S-i, Takahashi K, Takahashi Y, Morinaga T, Shimada Y, Moriya H (1996) Origin of nerves supplying the posterior portion of lumbar intervertebral discs in rats. Spine 21:917–924
Sekiguchi Y, Konnai Y, Kikuchi S, Sugiura Y (1996) An anatomic study of neuropeptide immunoreactivities in the lumbar dura mater after lumbar sympathectomy. Spine 21:925–930
Hovelacque A (1927) Des nerfs craniens et rachidiens et du système grand sympathique chez l’homme. Doin et Cie, Paris, pp 323–341
Suseki K, Takahashi Y, Takahashi K, Chiba T, Yamagata M, Moriya H (1998) Sensory nerve fibres from lumbar intervertebral discs pass through rami communicantes: a possible pathway for discogenic low back pain. J Bone Jt Surg Br 80:737–742
Huang EJ, Reichardt LF (2001) Neurotrophins: roles in neuronal development and function. Annu Rev Neurosci 24:677–736
Hadjipavlou A, Tzermiadianos M, Bogduk N, Zindrick M (2008) The pathophysiology of disc degeneration: a critical review. J Bone Jt Surg Br 90:1261–1270
Purmessur D, Freemont AJ, Hoyland JA (2008) Expression and regulation of neurotrophins in the nondegenerate and degenerate human intervertebral disc. Arthritis Res Ther 10:R99
Connally GH, Sanders SH (1991) Predicting low back pain patients’ response to lumbar sympathetic nerve blocks and interdisciplinary rehabilitation: the role of pretreatment overt pain behavior and cognitive coping strategies. Pain 44:139–146
Nakamura S, Takahashi K, Takahashi Y, Yamagata M, Moriya H (1996) The afferent pathways of discogenic low-back pain: evaluation of L2 spinal nerve infiltration. J Bone Jt Surg Br 78:606–612
Chandler G, Dalley G, Hemmer J Jr, Seely T (2001) Gray ramus communicans nerve block: novel treatment approach for painful osteoporotic vertebral compression fracture. South Med J 94:387–393
Jang JS, Kwon HK, Lee JJ, Hwang SM, Lim SY (2010) Rami communicans nerve block for the treatment of symptomatic schmorl’s nodes-A case report. The Korean journal of pain 23:262–265
Iwanaga J, Singh V, Ohtsuka A, Hwang Y, Kim HJ, Moryś J, Ravi KS, Ribatti D, Trainor PA, Sañudo JR (2021) Acknowledging the use of human cadaveric tissues in research papers: recommendations from anatomical journal editors. Clin Anat 34:2–4
Acknowledgements
This work was supported by two grants: Spanish Spine Society (GEER) and of the Spanish Ministry of Education (Collaboration Scholarships in University Departments) (Number 20CO1/011852).
The authors sincerely thank those who donated their bodies to science so that anatomical research could be performed. Results from such research can potentially increase mankind’s overall knowledge that can then improve patient care. Therefore, these donors and their families deserve our highest gratitude [42].
Funding
Open access funding provided by University of Innsbruck and Medical University of Innsbruck. The authors have no financial or personal relationship with any third party whose interests could be positively or negatively influenced by the article’s content. This research did receive a grant from the Spanish Ministry of Education (Collaboration Scholarships in University Departments) (Number 20CO1/011852).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Ethical approval and consent to participate
The body-donors to science belonged to the Bodies Donation Center and Dissection Rooms, Universidad Complutense de Madrid, Spain.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Quinones, S., Konschake, M., Aguilar, L.L. et al. Clinical anatomy of the lumbar sinuvertebral nerve with regard to discogenic low back pain and review of literature. Eur Spine J 30, 2999–3008 (2021). https://doi.org/10.1007/s00586-021-06886-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-06886-1