Abstract
Introduction
The natural history of motor deficit due to lumbar disc herniation has been thought to be favourable. However, on closer analysis of seminal articles on this topic, this is not the case for patients with severe motor deficits (MRC grade ≤3). The aim of this study is to answer the following questions: (1) Is surgical intervention beneficial in patients with severe motor weakness (defined by MRC grade of 3 or less) due to herniated lumbar nucleus pulposus? (2) Does time to surgery from onset of motor weakness influence the outcome? (3) Are there any other prognostic factors?
Materials and Methods
A comprehensive search was conducted in MEDLINE and EMBASE from 1970 upto July 2013. Inclusion criteria for studies are: (1) minimum of three patients aged 18 and older, who had symptomatic herniated lumbar disc prolapse and underwent surgery, (2) description of pre and post-operative muscle weakness utilising the Medical Research Council (MRC) muscle power grade or equivalent, such that both reviewers could confidently identify a cohort of patients with at least grade three motor weakness or worse, (3) a minimum of 6 months follow-up.
Results
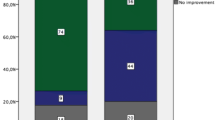
Seven studies were identified with a total of 354 patients. Complete recovery was seen in 38.4 % of patients following surgery and 32 % following non-operative treatment. Age and grade of motor deficit were identified as significant prognostic factors in some of the studies.
Conclusion
The current available evidence is not robust enough to address the questions posed. We have proposed a framework for future studies.

Similar content being viewed by others
References
Mixtar WJ, Barr JS (1934) Rupture of the intervertebral disc with involvement of the spinal canal. N Engl J Med 211:210–215
Peul WC, van Houwelingen HC, van den Hout WB, Brand R, Eekhof JA, Tans JT, Thomeer RT, Koes BW, Leiden-The Hague Spine Intervention Prognostic Study Group (2007) Surgery versus prolonged conservative treatment for sciatica. N Engl J Med 356(22):2245–2256
Hakelius A (1970) Prognosis in sciatica. A clinical follow-up of surgical and non-surgical treatment. Acta Orthop Scand Suppl 129:1–76
Weber H (1983) Lumbar disc herniation. A controlled, prospective study with ten years of observation. Spine (Phila Pa 1976) 8(2):131–140
Weber H (1975) The effect of delayed disc surgery on muscular paresis. Acta Orthop Scand 46(4):631–642
Ryan R, HS Broclain D, Horey D, Oliver S, Prictor M (2007) Cochrane consumers & communication review group: study quality guide p 1–50
Buttermann GR (2004) Treatment of lumbar disc herniation: epidural steroid injection compared with discectomy. A prospective, randomized study. J Bone Joint Surg Am 86A:670–679
Dubourg G, Rozenberg S, Fautrel B, Valls-Bellec I, Bissery A, Lang T, Faillot T, Duplan B, Briançon D, Levy-Weil F, Morlock G, Crouzet J, Gatfosse M, Bonnet C, Houvenagel E, Hary S, Brocq O, Poiraudeau S, Beaudreuil J, de Sauverzac C, Durieux S, Levade MH, Esposito P, Maitrot D, Goupille P, Valat JP, Bourgeois P (2002) A pilot study on the recovery from paresis after lumbar disc herniation. Spine (Phila Pa 1976) 27(13):1426–1431
Ghahreman A, Ferch RD, Rao P, Chandran N, Shadbolt B (2009) Recovery of ankle dorsiflexion weakness following lumbar decompressive surgery. J Clin Neurosci 16(8):1024–1027
Iizuka Y, Iizuka H, Tsutsumi S, Nakagawa Y, Nakajima T, Sorimachi Y, Ara T, Nishinome M, Seki T, Shida K, Takagishi K (2009) Foot drop due to lumbar degenerative conditions: mechanism and prognostic factors in herniated nucleus pulposus and lumbar spinal stenosis. J Neurosurg Spine 10(3):260–264
Jönsson B, Strömqvist B (1995) Motor affliction of the L5 nerve root in lumbar nerve root compression syndromes. Spine (Phila Pa 1976) 20(18):2012–2015
Postacchini F, Giannicola G, Cinotti G (2002) Recovery of motor deficits after microdiscectomy for lumbar disc herniation. J Bone Joint Surg Br 84(7):1040–1045
Eysel P, Rompe JD, Hopf C (1994) Prognostic criteria of discogenic paresis. Eur Spine J 3(4):214–218
Sarikcioglu L, Yaba A, Tanriover G, Demirtop A, Demir N, Ozkan O (2007) Effect of severe crush injury on axonal regeneration: a functional and ultrastructural study. J Reconstr Microsurg 23(3):143–149
Pham K, Gupta R (2009) Understanding the mechanisms of entrapment neuropathies. Review article. Neurosurg Focus 26(2):E7
Jancalek R, Dubovy P (2007) An experimental animal model of spinal root compression syndrome: an analysis of morphological changes of myelinated axons during compression radiculopathy and after decompression. Exp Brain Res 179(1):111–119
Verdú E, Ceballos D, Vilches JJ, Navarro X (2000) Influence of aging on peripheral nerve function and regeneration. J Peripher Nerv Syst 5(4):191–208
Aono H, Iwasaki M, Ohwada T, Okuda S, Hosono N, Fuji T, Yoshikawa H (2007) Surgical outcome of drop foot caused by degenerative lumbar diseases. Spine (Phila Pa 1976) 32(8):E262–E266
Matsui H, Kanamori M, Kawaguchi Y, Kitagawa H, Nakamura H, Tsuji H (1997) Clinical and electrophysiologic characteristics of compressed lumbar nerve roots. Spine (Phila Pa 1976) 22(18):2100–2105
Girardi FP, Cammisa FP Jr, Huang RC, Parvataneni HK, Tsairis P (2002) Improvement of preoperative foot drop after lumbar surgery. J Spinal Disord Tech 15(6):490–494
Gioia G, Mandelli D, Capaccioni B, Randelli F, Tessari L (1999) Surgical treatment of far lateral lumbar disc herniation. Identification of compressed root and discectomy by lateral approach. Spine (Phila Pa 1976) 24(18):1952–1957
Blaauw G, Braakman R, Gelpke GJ, Singh R (1988) Changes in radicular function following low-back surgery. J Neurosurg 69(5):649–652
Guigui P, Benoist M, Delecourt C, Delhoume J, Deburge A (1998) Motor deficit in lumbar spinal stenosis: a retrospective study of a series of 50 patients. J Spinal Disord 11(4):283–288
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Balaji, V.R., Chin, K.F., Tucker, S. et al. Recovery of severe motor deficit secondary to herniated lumbar disc prolapse: is surgical intervention important? A systematic review. Eur Spine J 23, 1968–1977 (2014). https://doi.org/10.1007/s00586-014-3371-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-014-3371-2