Abstract
Purpose
To evaluate potential effects and satisfaction of dignity therapy among patients with hematologic neoplasms in the Chinese cultural context.
Methods
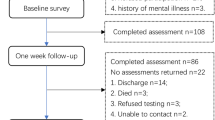
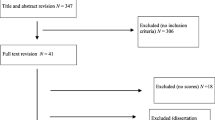
Sixty-six patients with hematologic neoplasms were randomly assigned into either a dignity therapy group (N = 32) or control group (N = 34). The primary outcomes were level of hope and spiritual well-being, as measured according to the Herth Hope Index and the 12-item Functional Assessment of Chronic Illness Therapy-Spiritual Well-Being, at baseline (T0), 1-week follow-up (T1), and 4-week follow-up (T2). Satisfaction with dignity therapy was assessed using a 5-grade marking system at T1.
Results
Among the 66 participants, 61 remained at 1-week follow-up and 57 remained at 4-week follow-up. Group differences were found in the total score and the scores of each dimension of spiritual well-being and level of hope at T1 and T2 (p < 0.05). Interaction effects were statistically significant in terms of spiritual well-being (p < 0.001) and level of hope (p < 0.001). Majority of the patients (93.34%) and family members (96.67%) gave positive evaluations (“very satisfactory” or “relatively satisfactory”) for the dignity therapy intervention.
Conclusion
Implementing dignity therapy among patients with hematologic neoplasms in China was associated with good efficacy in improving spiritual well-being and the level of hope in the short term. Difficulties and solutions involved in the implementation of dignity therapy in multiple cultures deserve attention.

Similar content being viewed by others
Data Availability
The datasets used or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6):394–424. https://doi.org/10.3322/caac.21492
Cao M, Chen W (2019) Epidemiology of cancer in China and the current status of prevention and control. Chin J Clin Oncol 46(3):145–147. https://doi.org/10.3969/j.issn.1000-8179.2019.03.283
Sexauer A, Cheng M, Knight L, Riley A, King L, Smith T (2014) Patterns of hospice use in patients dying from hematologic malignancies. J Palliat Med 17(2):195–199. https://doi.org/10.1089/jpm.2013.0250
Leblanc TW, Abernethy AP, Casarett DJ (2015) What is different about patients with hematologic malignancies? A retrospective cohort study of cancer patients referred to a hospice research network. J Pain Symptom Manag 49(3):505–512. https://doi.org/10.1016/j.jpainsymman.2014.07.003
Fasolino TK, Ashley JL (2016) Palliative and hospice care: educational needs of inpatient registered nurses. Creat Nurs 22(2):114–120. https://doi.org/10.1891/1078-4535.22.2.114
Kuin A, Deliens L, Van Zuylen L, Courtens AM, Vernooij-Dassen MJ, Van dL, B., Van dW, G. (2006) Spiritual issues in palliative care consultations in the Netherlands. Palliat Med 20(6):585–592. https://doi.org/10.1177/0269216306071059
Pearce M, Coan A, Herndon J, Koenig H, Abernethy A (2012) Unmet spiritual care needs impact emotional and spiritual well-being in advanced cancer patients. Support Care Cancer 20(10):2269–2276. https://doi.org/10.1007/s00520-011-1335-1
Vallurupalli M, Lauderdale K, Balboni M, Phelps A, Block S, Ng A, Kachnic L, Vanderweele T, Balboni T (2012) The role of spirituality and religious coping in the quality of life of patients with advanced cancer receiving palliative radiation therapy. J Support Oncol 10(2):81–87. https://doi.org/10.1016/j.suponc.2011.09.003
Chen J, Lin Y, Yan J, Wu Y, Hu R (2018) The effects of spiritual care on quality of life and spiritual well-being among patients with terminal illness: a systematic review. Palliat Med 32(7):1167–1179. https://doi.org/10.1177/0269216318772267
Surbone A, Baider L (2010) The spiritual dimension of cancer care. Crit Rev Oncol Hematol 73(3):228–235. https://doi.org/10.1016/j.critrevonc.2009.03.011
Ferrell B (2005) Dignity therapy: advancing the science of spiritual care in terminal illness. J Clin Oncol 23(24):5427–5428. https://doi.org/10.1200/jco.2005.04.912
Chochinov HM (2005) Dignity therapy: a novel psychotherapeutic intervention for patients near the end of life. J Clin Oncol 23(24):5520. https://doi.org/10.1200/jco.2005.08.391
Chochinov HM, Hack T, Mcclement S, Kristjanson L, Harlos M (2002) Dignity in the terminally ill: a developing empirical model. Soc Sci Med 54(3):433–443. https://doi.org/10.1016/s0277-9536(01)00084-3
Brożek B, Fopka-Kowalczyk M, Łabuś-Centek M, Damps-Konstańska I, Ratajska A, Jassem E, Larkin P, Krajnik M (2019) Dignity therapy as an aid to coping for COPD patients at their end-of-life stage. Adv Respir Med 87(3):135–145. https://doi.org/10.5603/ARM.a2019.0021
Julião M, Oliveira F, Nunes B, Carneiro A, Barbosa A (2017) Effect of dignity therapy on end-of-life psychological distress in terminally ill Portuguese patients: a randomized controlled trial. Palliat Support Care 15(6):628–637. https://doi.org/10.1017/s1478951516001140
Dose A, Rhudy L (2018) Perspectives of newly diagnosed advanced cancer patients receiving dignity therapy during cancer treatment. Support Care Cancer 26(1):187–195. https://doi.org/10.1007/s00520-017-3833-2
Li Y, Li X, Hou L, Cao L, Liu G, Yang K (2020) Effectiveness of dignity therapy for patients with advanced cancer: a systematic review and meta-analysis of 10 randomized controlled trials. Depress Anxiety 37(3):234–246. https://doi.org/10.1002/da.22980
Bentley B, O’Connor M, Shaw J, Breen L (2017) A narrative review of dignity therapy research. Aust Psychol 52(5):354–362. https://doi.org/10.1111/ap.12282
Li Y, Zhou J (2015) The effects of dignity therapy on hope level and psychological status of patients with advanced lung cancer. J Nurs Sci 30(8):82–83. https://doi.org/10.3870/hlxzz.2015.08.082
Dai H (2011) Effects of dignity therapy on self-esteem related stress and hope levels in liver cancer patients. J Nurs Sci 26(23):66–67. https://doi.org/10.3870/hlxzz.2011.23.066
Sun C, Qin M (2009) The Confucian way of shaping the character of the Chinese nation. J Chongqing Jiaotong Univ (Social Sciences Edition) 9(01):77–79. https://doi.org/10.3969/j.issn.1674-0297.2009.01.021
Xiao J, Chow K, Chan C, Li M, Deng Y (2020) Qualitative study on perceived dignity of cancer patients undergoing chemotherapy in China. Support Care Cancer 28(6):2921–2929. https://doi.org/10.1007/s00520-019-05123-2
Mao J, Ren K, Xu X, Chen Y, Fan Y (2020) The research progress of the influencing factors of the elderly’s attitude towards death in China. Guide Sci Educ 06:187–188. https://doi.org/10.16400/j.cnki.kjdkx.2020.06.086
Hsu C, O’Connor M, Lee S (2009) Understandings of death and dying for people of Chinese origin. Death Stud 33(2):153–174. https://doi.org/10.1080/07481180802440431
Chochinov HM (2012) Dignity therapy: final words for final days. Oxford University Press, New York
Bredle JM, Salsman JM, Debb SM, Arnold BJ, David C (2011) Spiritual well-being as a component of health-related quality of life: the functional assessment of chronic illness therapy—spiritual well-being scale (FACIT-Sp). Relig 2(1):77–94. https://doi.org/10.3390/rel2010077
Liu X, Wei D, Shen Y, Cheng Q, Liang S, Xu X, Zhang M (2016) Evaluation of the reliability and validity of the Chinese version of the Functional Assessment of Chronic Illness Therapy—Spiritual Well-Being Scale (FACIT-Sp) for the treatment of chronic diseases in cancer patients. Chin J Nurs 51(9):1085–1090. https://doi.org/10.3761/j.issn.0254-1769.2016.09.014
Herth K (1992) Abbreviated instrument to measure hope: development and psychometric evaluation. J Adv Nurs 17(10):1251–1259. https://doi.org/10.1111/j.1365-2648.1992.tb01843.x
Zhao H, Wang J (2000) Social support and hope for hemodialysis patients. Chin J Nurs 35(5):306–308
Wang Y (2010) Feasibility study of Chinese version of Herth hope scale for cancer patients. Chin Nurs Res 24(1):20–21. https://doi.org/10.3969/j.issn.1009-6493.2010.01.008
Zhang HY, Zhang YQ, Rui W, Wei L, Zhang YQ, Xiang Z, Liu BL, Cheng JX, Li X, Huo JL (2011) The validation of the standard Chinese version of the European Organization for Research and Treatment of Cancer Quality of Life Core Questionnaire 30 (EORTC QLQ-C30) in pre-operative patients with brain tumor in China. BMC Med Res Methodol 11(1):56. https://doi.org/10.1186/1471-2288-11-56
Wan C, Chen M, Zhang C, Tang X (2005) Evaluation of the Chinese version of EORTC QLQ-C30. J Pract Oncol 20(4):353–355. https://doi.org/10.3969/j.issn.1001-1692.2005.04.028
World Medical Association (2013) World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA 310(20):2191–2194
Chochinov HM, Kristjanson L, Breitbart W, Mcclement S, Hack T, Hassard T, Harlos M (2011) Effect of dignity therapy on distress and end-of-life experience in terminally ill patients: a randomised controlled trial. Lancet Oncol 12(8):753–762. https://doi.org/10.1016/s1470-2045(11)70153-X
Hall S, Goddard C, Opio D, Speck P, Martin P, Higginson I (2011) A novel approach to enhancing hope in patients with advanced cancer: a randomised phase II trial of dignity therapy. BMJ Support Palliat Care 1(3):315–321. https://doi.org/10.1136/bmjspcare-2011-000054
Martínez M, Arantzamendi M, Belar A, Carrasco JM, Centeno C (2017) ‘Dignity therapy’, a promising intervention in palliative care: a comprehensive systematic literature review. Palliat Med 31(6):492–509. https://doi.org/10.1177/0269216316665562
Gong Y, Cui L, Sun X (2014) Effects of dignity therapy on self-esteem and level of hope among patients with pancreatic cancer. J NursRehabil 13(9):826–828. https://doi.org/10.3969/j.issn.1671-9875.2014.09.003
Mcclement S, Chochinov HM, Hack T, Hassard T, Kristjanson LJ, Harlos M (2007) Dignity therapy: family member perspectives. J Palliat Med 10(5):1076–1082. https://doi.org/10.1089/jpm.2007.0002
Li R (2018) Applicability analysis of dignity therapy in China. Med Phil 39(2):1–15. https://doi.org/10.12014/j.issn.1002-0772.2018.01b.01
Zeng T, Chen F, Yang X, Fang P (2008) A survey of attitudes toward end-stage treatment and death among cancer patients. J Nurs Sci 23(7):74–76. https://doi.org/10.3969/j.issn.1001-4152.2008.07.035
Acknowledgements
The authors thank all participants and their family members for their time and participation. Additionally, we would like to thank the doctors and nurses in the Hematology Department for their support and advice regarding this research.
Funding
This study was supported by the Scientific Research Talents Training Project from Fujian Province Health Commission (Grant No. 2018-ZQN-63) and the Science and Technology Innovation Joint Fund Project of Fujian Province, China (Grant No. 2019Y9029).
Author information
Authors and Affiliations
Contributions
Jingyi Chen: conceptualization, data curation, investigation, writing—original draft.
Jie Yan: data curation, software.
Chunfeng Wang: software, writing—review and editing.
Ying Wang: data curation, writing—review and editing.
Yong Wu: resources, project administration.
Rong Hu: methodology, validation, supervision.
Corresponding authors
Ethics declarations
Informed consent
The trial was approved by the Ethics Committee of the Fujian Medical University (number 2017/00049). Written informed consent was obtained from each participant prior to the study. The study was carried out in accordance with the Declaration of Helsinki.
Consent to participate
Written informed consent for publication was obtained from all participants included in this study.
Consent for publications
Patients signed informed consent regarding publishing their data.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, J., Yan, J., Wang, C. et al. Effects and satisfaction of dignity therapy among patients with hematologic neoplasms in the Chinese cultural context: a randomized controlled trial. Support Care Cancer 29, 6819–6829 (2021). https://doi.org/10.1007/s00520-021-06227-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-021-06227-4