Abstract
Background
Acute kidney injury (AKI) is a common condition in critically ill children and is associated with increased morbidity and mortality. This study aimed to assess the performance of point-of-care ultrasonography to predict AKI in children undergoing cardiac surgery.
Methods
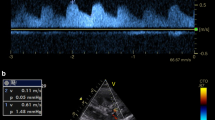
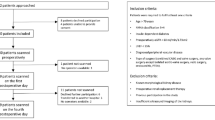
In this prospective study, consecutive children underwent kidney Doppler ultrasound examination within 24 h following cardiac surgery, and an experienced operator obtained both renal resistive index (RRI) and renal pulsatility index (RPI). AKI was defined by the Kidney Disease Improving Global Outcome (KDIGO) criteria. The primary outcome was the diagnosis of severe AKI (KDIGO stage 2 or 3) on day 3.
Results
A total of 58 patients were included. Median age and weight were 12.9 months (IQR 6.0–37.9) and 7.36 kg (IQR 5.19–11.40), respectively. On day 3, 13 patients were classified as having AKI, of which 11 were severe. RRI could effectively predict AKI (area under the ROC curve [AUC] 0.83, 95% CI 0.71–0.92; p < 0.001) as well as RPI (AUC 0.81, 95% CI 0.69–0.90; p < 0.001). The optimal cutoff value for RRI was 0.85 (sensitivity, 73%; specificity, 83%; positive predictive value [PPV], 50%; and negative predictive value [NPV], 93%), while for RPI was 1.95 (sensitivity, 73%; specificity, 78%; PPV, 44%; and NPV, 92%). Similar results were found in the analysis for prediction on day 5. Significant correlations were found between Doppler-based variables and estimated GFR and furosemide dose on day 3.
Conclusions
Kidney Doppler ultrasound may be a promising tool for predicting AKI in children undergoing cardiac surgery.
Graphical Abstract

A higher resolution version of the Graphical abstract is available as Supplementary information


Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
Code availability
Not applicable.
References
Sharma A, Chakraborty R, Sharma K et al (2020) Development of acute kidney injury following pediatric cardiac surgery. Kidney Res Clin Pract 39:259–268. https://doi.org/10.23876/j.krcp.20.053
Li S, Krawczeski CD, Zappitelli M et al (2011) Incidence, risk factors, and outcomes of acute kidney injury after pediatric cardiac surgery: a prospective multicenter study. Crit Care Med 39:1493–1499. https://doi.org/10.1097/CCM.0B013E31821201D3
Kourelis G, Kanakis M, Samanidis G et al (2022) Acute kidney injury predictors and outcomes after cardiac surgery in children with congenital heart disease: an observational cohort study. Diagnostics (Basel) 12:2397. https://doi.org/10.3390/diagnostics12102397
Pande CK, Smith MB, Soranno DE et al (2022) The neglected price of pediatric acute kidney injury: non-renal implications. Front Pediatr 10:893993. https://doi.org/10.3389/fped.2022.893993
Romagnoli S, Ricci Z, Ronco C (2018) Perioperative acute kidney injury: prevention, early recognition, and supportive measures. Nephron 140:105–110. https://doi.org/10.1159/000490500
Webb TN, Goldstein SL (2017) Congenital heart surgery and acute kidney injury. Curr Opin Anesthesiol 30:105–112. https://doi.org/10.1097/ACO.0000000000000406
Kellum JA, Lameire N, Aspelin P et al (2011) (2012) Kidney disease: improving global outcomes (KDIGO) acute kidney injury work group. KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl 2:1–138. https://doi.org/10.1038/kisup.2012.1
Selewski DT, Charlton JR, Jetton JG et al (2015) Neonatal acute kidney injury. Pediatrics 136:e463–e473. https://doi.org/10.1542/PEDS.2014-3819
Toda Y, Sugimoto K (2017) AKI after pediatric cardiac surgery for congenital heart diseases–recent developments in diagnostic criteria and early diagnosis by biomarkers. J Intensive Care 5:49. https://doi.org/10.1186/s40560-017-0242-z
de Carvalho AV, de Ferraz IS, de Souza FM et al (2023) Acute kidney injury in critically ill children: predictive value of renal arterial Doppler assessment. Pediatr Res 93:1694–1700. https://doi.org/10.1038/s41390-022-02296-1
Shen H, Na W, Li Y, Qu D (2023) The clinical significance of renal resistance index (RRI) and renal oxygen saturation (RrSO2) in critically ill children with AKI: a prospective cohort study. BMC Pediatr 23:224. https://doi.org/10.1186/s12887-023-03941-2
Qian X, Zhen J, Meng Q et al (2022) Intrarenal Doppler approaches in hemodynamics: a major application in critical care. Front Physiol 13:951307. https://doi.org/10.3389/fphys.2022.951307
Advanced Life Support Group (2016) Advanced paediatric life support: a practical approach to emergencies, 6th edn. Wiley-Blackwell, Manchester UK
Van den Eynde J, Delpire B, Jacquemyn X et al (2022) Risk factors for acute kidney injury after pediatric cardiac surgery: a meta-analysis. Pediatr Nephrol 37:509–519. https://doi.org/10.1007/s00467-021-05297-0
Gottlieb RH, Luhmann K 4th, Oates RP (1989) Duplex ultrasound evaluation of normal native kidneys and native kidneys with urinary tract obstruction. J Ultrasound Med 8:609–611. https://doi.org/10.7863/jum.1989.8.11.609
Warshauer DM, Taylor KJ, Bia MJ et al (1988) Unusual causes of increased vascular impedance in renal transplants: duplex Doppler evaluation. Radiology 169:367–370. https://doi.org/10.1148/radiology.169.2.3051113
O’Neill WC (2000) Sonographic evaluation of renal failure. Am J Kidney Dis 35:1021–1038. https://doi.org/10.1016/S0272-6386(00)70036-9
Boddi M, Natucci F, Ciani E (2015) The internist and the renal resistive index: truths and doubts. Intern Emerg Med 10:893–905. https://doi.org/10.1007/s11739-015-1289-2
Sethi SK, Raina R, Koratala A et al (2023) Point-of-care ultrasound in pediatric nephrology. Pediatr Nephrol 38:1733–1751. https://doi.org/10.1007/s00467-022-05729-5
Darabont R, Mihalcea D, Vinereanu D (2023) Current insights into the significance of the renal resistive index in kidney and cardiovascular disease. Diagnostics (Basel) 13:1687. https://doi.org/10.3390/diagnostics13101687
Le Dorze M, Bouglé A, Deruddre S, Duranteau J (2012) Renal Doppler ultrasound: a new tool to assess renal perfusion in critical illness. Shock 37:360–365. https://doi.org/10.1097/SHK.0b013e3182467156
Neunhoeffer F, Wiest M, Sandner K et al (2016) Non-invasive measurement of renal perfusion and oxygen metabolism to predict postoperative acute kidney injury in neonates and infants after cardiopulmonary bypass surgery. Br J Anaesth 117:623–634. https://doi.org/10.1093/bja/aew307
Hertzberg D, Ceder SL, Sartipy U et al (2017) Preoperative renal resistive index predicts risk of acute kidney injury in patients undergoing cardiac surgery. J Cardiothorac Vasc Anesth 31:847–852. https://doi.org/10.1053/j.jvca.2016.10.006
Wiersema R, Kaufmann T, van der Veen HN et al (2020) Diagnostic accuracy of arterial and venous renal Doppler assessment for acute kidney injury in critically ill patients: a prospective study. J Crit Care 59:57–62. https://doi.org/10.1016/j.jcrc.2020.05.012
Kararmaz A, Arslantas MK, Aksu U et al (2021) Evaluation of acute kidney injury with oxidative stress biomarkers and renal resistive index after cardiac surgery. Acta Chir Belg 121:189–197. https://doi.org/10.1080/00015458.2019.1702371
Bellos I, Pergialiotis V, Kontzoglou K (2019) Renal resistive index as predictor of acute kidney injury after major surgery: a systematic review and meta-analysis. J Crit Care 50:36–43. https://doi.org/10.1016/J.JCRC.2018.11.001
Wu H, Liu K, Darko IN et al (2020) Predictive value of renal resistive index for the onset of acute kidney injury and its non-recovery: a systematic review and meta-analysis. Clin Nephrol 93:172–186. https://doi.org/10.5414/CN109979
Cvitković Kuzmić A, Brkljačić B, Ivanković D, Galešić K (2000) Doppler sonographic renal resistance index in healthy children. Eur Radiol 10:1644–1648. https://doi.org/10.1007/s003300000466
Murat A, Akarsu S, Ozdemir H et al (2005) Renal resistive index in healthy children. Eur J Radiol 53:67–71. https://doi.org/10.1016/j.ejrad.2004.05.005
Kelly LK, Seri I (2008) Renal developmental physiology relevance to clinical care. NeoReviews 9:e150–e161. https://doi.org/10.1542/NEO.9-4-E150
Fiselier T, Derkx F, Monnens L et al (1984) The basal levels of active and inactive plasma renin concentration in infancy and childhood. Clin Sci 67:383–387. https://doi.org/10.1042/CS0670383
Zubarev AV (2001) Ultrasound of renal vessels. Eur Radiol 11:1902–1915. https://doi.org/10.1007/S003300101012
Eibenberger K, Schima H, Trubel W et al (1995) Intrarenal Doppler ultrasonography: which vessel should be investigated? J Ultrasound Med 14:451–455. https://doi.org/10.7863/jum.1995.14.6.451
Saif A, Soliman N, Abdelhamid A (2014) Doppler assessment of renal hemodynamic alterations in homozygous sickle cell disease and sickle beta-thalassemia. Ultrason Imaging 37:258–264. https://doi.org/10.1177/0161734614553831
Gaies MG, Gurney JG, Yen AH et al (2010) Vasoactive–inotropic score as a predictor of morbidity and mortality in infants after cardiopulmonary bypass*. Pediatr Crit Care Med 11:234–238. https://doi.org/10.1097/PCC.0b013e3181b806fc
Ninmer EK, Charlton JR, Spaeder MC (2022) Risk factors for sepsis-associated acute kidney injury in the PICU: a retrospective cohort study. Pediatr Crit Care Med 23:e366–e370. https://doi.org/10.1097/PCC.0000000000002957
Deruddre S, Cheisson G, Mazoit J-X et al (2007) Renal arterial resistance in septic shock: effects of increasing mean arterial pressure with norepinephrine on the renal resistive index assessed with Doppler ultrasonography. Intensive Care Med 33:1557–1562. https://doi.org/10.1007/s00134-007-0665-4
Lex DJ, Tóth R, Cserép Z et al (2014) A comparison of the systems for the identification of postoperative acute kidney injury in pediatric cardiac patients. Ann Thorac Surg 97:202–210. https://doi.org/10.1016/j.athoracsur.2013.09.014
Gao P, He W, Jin Y et al (2023) Acute kidney injury after infant cardiac surgery: a comparison of pRIFLE, KDIGO, and pROCK definitions. BMC Nephrol 24:1–9. https://doi.org/10.1186/s12882-023-03306-y
Xu X, Nie S, Zhang A et al (2018) A new criterion for pediatric AKI based on the reference change value of serum creatinine. J Am Soc Nephrol 29:2432–2442. https://doi.org/10.1681/ASN.2018010090
Lee YJ, Park YS, Park SJ, Jhang WK (2022) Estimating baseline creatinine values to define acute kidney injury in critically ill pediatric patients. Kidney Res Clin Pract 41:322–331. https://doi.org/10.23876/j.krcp.21.120
Acknowledgements
Thank you to Carolina Grotta Ramos Telio for her review of the manuscript. We also thank the legal guardians of the participants, attending physicians, pediatric critical care residents, and the nursing staff.
Author information
Authors and Affiliations
Contributions
Conception and design: THdS; acquisition of data: FMdS; AVdC, IdSF, THdS; analysis and interpretation of data: FMdS, IdSF, THdS; drafting the article: FMdS, IdSF, THdS; revising the article critically for important intellectual content: RJNN, MBB, and APD; all of the authors read and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
De Souza, F.M., De Carvalho, A.V., Ferraz, I.S. et al. Acute kidney injury in children undergoing cardiac surgery: predictive value of kidney arterial Doppler-based variables. Pediatr Nephrol (2024). https://doi.org/10.1007/s00467-024-06319-3
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00467-024-06319-3