Abstract
Background
Increased left ventricular mass (LVM) is an important risk marker of uremic cardiovascular disease. Calculation of LVM by echocardiography (Echo) relies on geometric assumptions and in adults on hemodialysis overestimates LVM compared to cardiac magnetic resonance (CMR). We compare both techniques in children with chronic kidney disease (CKD).
Methods
Concurrent Echo and CMR was performed in 25 children with CKD (14 after kidney transplantation) aged 8–17 years.
Results
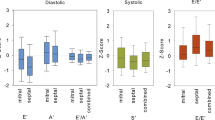
Compared to normal children, CMR-LVM was increased (standard deviation score (SDS) 0.39 ± 0.8 (p = 0.03)), stroke volume and cardiac output decreased (SDS −1.76 ± 1.1, p = 0.002 and −1.11 ± 2.0, p = 0.001). CMR-LVM index but not Echo-LVMI correlated to future glomerular filtration rate (GFR) decline (r = −0.52, p = 0.01). Mean Echo-LVM was higher than CMR-LVM (117 ± 40 vs. 89 ± 29 g, p < 0.0001), with wide limits of agreement (−6.2 to 62.8 g). The Echo-CMR LVM difference increased with higher Echo-LVMI (r = 0.77, p < 0.0001). Agreement of classifying left ventricular hypertrophy was poor with Cohen’s kappa of 0.08. Mean Echo and CMR-ejection fraction differed by 1.42 % with wide limits of agreement (−12.6 to 15.4 %).
Conclusions
Echo overestimates LVM compared to CMR, especially at higher LVM. Despite this, CMR confirms increased LVM in children with CKD. Only CMR-LVMI but not Echo-LVMI correlated to future GFR decline.






Similar content being viewed by others
References
Mitsnefes MM, Kimball TR, Witt SA, Glascock BJ, Khoury PR, Daniels SR (2003) Left ventricular mass and systolic performance in pediatric patients with chronic renal failure. Circulation 107:864–868
Matteucci MC, Wühl E, Picca S, Mastrostefano A, Rinelli G, Romano C, Rizzoni G, Mehls O, de Simone G, Schaefer F, ESCAPE Trial Group (2006) Left ventricular geometry in children with mild to moderate chronic renal insufficiency. J Am Soc Nephrol 17:218–226
Chinali M, de Simone G, Matteucci MC, Picca S, Mastrostefano A, Anarat A, Caliskan S, Jeck N, Neuhaus TJ, Peco-Antic A, Peruzzi L, Testa S, Mehls O, Wühl E, Schaefer F (2007) Reduced systolic myocardial function in children with chronic renal insufficiency. J Am Soc Nephrol 18:593–598
Mitsnefes MM, Kimball TR, Border WL, Witt SA, Glascock BJ, Khoury PR, Daniels SR (2004) Impaired left ventricular diastolic function in children with chronic renal failure. Kidney Int 65:1461–1466
Ten Harkel ADJ, Cransberg K, Van Osch-Gevers M, Nauta J (2009) Diastolic dysfunction in paediatric patients on peritoneal dialysis and after renal transplantation. Nephrol Dial Transplant 24:1987–1991
Litwin M, Wühl E, Jourdan C, Trelewicz J, Niemirska A, Fahr K, Jobs K, Grenda R, Wawer ZT, Rajszys P, Tröger J, Mehls O, Schaefer F (2005) Altered morphologic properties of large arteries in children with chronic renal failure and after renal transplantation. J Am Soc Nephrol 16:1494–1500
Bilginer Y, Ozaltin F, Basaran C, Aki TF, Karabulut E, Duzova A, Besbas N, Topaloglu R, Ozen S, Bakkaloglu M, Bakkaloglu A (2007) Carotid intima-media thickness in children and young adults with renal transplant: internal carotid artery vs. common carotid artery. Pediatr Transplant 11:888–894
Doyon A, Kracht D, Bayazit AK, Deveci M, Duzova A, Krmar RT, Litwin M, Niemirska A, Oguz B, Schmidt BMW, Sözeri B, Querfeld U, Melk A, Schaefer F, Wühl E, 4C Study Consortium (2013) Carotid artery intima-media thickness and distensibility in children and adolescents: reference values and role of body dimensions. Hypertension 62:550–556
Devereux RB, Alonso DR, Lutas EM, Gottlieb GJ, Campo E, Sachs I, Reichek N (1986) Echocardiographic assessment of left ventricular hypertrophy: comparison to necropsy findings. Am J Cardiol 57:450–458
De Simone G, Devereux RB, Daniels SR, Koren MJ, Meyer RA, Laragh JH (1995) Effect of growth on variability of left ventricular mass: assessment of allometric signals in adults and children and their capacity to predict cardiovascular risk. J Am Coll Cardiol 25:1056–1062
Khoury PR, Mitsnefes M, Daniels SR, Kimball TR (2009) Age-specific reference intervals for indexed left ventricular mass in children. J Am Soc Echocardiogr 22:709–714
Simpson JM, Savis A, Rawlins D, Qureshi S, Sinha MD (2010) Incidence of left ventricular hypertrophy in children with kidney disease: impact of method of indexation of left ventricular mass. Eur J Echocardiogr 11:271–277
Borzych D, Bakkaloglu SA, Zaritsky J, Suarez A, Wong W, Ranchin B, Qi C, Szabo AJ, Coccia PA, Harambat J, Mitu F, Warady BA, Schaefer F, International Pediatric Peritoneal Dialysis Network (2011) Defining left ventricular hypertrophy in children on peritoneal dialysis. Clin J Am Soc Nephrol 6:1934–1943
Schoenmaker NJ, van der Lee JH, Groothoff JW, van Iperen GG, Frohn-Mulder IME, Tanke RB, Ottenkamp J, Kuipers IM (2013) Low agreement between cardiologists diagnosing left ventricular hypertrophy in children with end-stage renal disease. BMC Nephrol 14:170
Grothues F, Smith GC, Moon JCC, Bellenger NG, Collins P, Klein HU, Pennell DJ (2002) Comparison of interstudy reproducibility of cardiovascular magnetic resonance with two-dimensional echocardiography in normal subjects and in patients with heart failure or left ventricular hypertrophy. Am J Cardiol 90:29–34
Armstrong AC, Gidding S, Gjesdal O, Wu C, Bluemke DA, Lima JAC (2012) LV mass assessed by echocardiography and CMR, cardiovascular outcomes, and medical practice. JACC Cardiovasc Imaging 5:837–848
Schaefer B, Rusai K, Toth A, Pasti K, Ujszaszi A, Kreko M, Horvath E, Sallay P, Reusz GS, Merkely B, Tulassay T, Szabo AJ (2012) Cardiac magnetic resonance imaging in children with chronic kidney disease and renal transplantation. Pediatr Transplant 16:350–356
Malatesta-Muncher R, Wansapura J, Taylor M, Lindquist D, Hor K, Mitsnefes M (2012) Early cardiac dysfunction in pediatric patients on maintenance dialysis and post kidney transplant. Pediatr Nephrol 27:1157–1164
Stewart GA, Foster J, Cowan M, Rooney E, McDonagh T, Dargie HJ, Rodger RS, Jardine AG (1999) Echocardiography overestimates left ventricular mass in hemodialysis patients relative to magnetic resonance imaging. Kidney Int 56:2248–2253
Jakubovic BD, Wald R, Goldstein MB, Leong-Poi H, Yuen DA, Perl J, Lima JA, Liu JJ, Kirpalani A, Dacouris N, Wald R, Connelly KA, Yan AT (2013) Comparative assessment of 2-dimensional echocardiography vs. cardiac magnetic resonance imaging in measuring left ventricular mass in patients with and without end-stage renal disease. Can J Cardiol 29:384–390
Lorenz CH, Walker ES, Morgan VL, Klein SS, Graham TP (1999) Normal human right and left ventricular mass, systolic function, and gender differences by cine magnetic resonance imaging. J Cardiovasc Magn Reson 1:7–21
Vinnakota KC, Bassingthwaighte JB (2004) Myocardial density and composition: a basis for calculating intracellular metabolite concentrations. Am J Physiol Heart Circ Physiol 286:H1742–H1749
Lai WW, Geva T, Shirali GS, Frommelt PC, Humes RA, Brook MM, Pignatelli RH, Rychik J, Task Force of the Pediatric Council of the American Society of Echocardiography, Pediatric Council of the American Society of Echocardiography (2006) Guidelines and standards for performance of a pediatric echocardiogram: a report from the task force of the pediatric council of the American Society of Echocardiography. J Am Soc Echocardiogr 19:1413–1430
De Simone G, Daniels SR, Kimball TR, Roman MJ, Romano C, Chinali M, Galderisi M, Devereux RB (2005) Evaluation of concentric left ventricular geometry in humans: evidence for age-related systematic underestimation. Hypertension 45:64–68
Buechel EV, Kaiser T, Jackson C, Schmitz A, Kellenberger CJ (2009) Normal right- and left ventricular volumes and myocardial mass in children measured by steady state free precession cardiovascular magnetic resonance. J Cardiovasc Magn Reson 11:19
Robbers-Visser D, Boersma E, Helbing WA (2009) Normal biventricular function, volumes, and mass in children aged 8 to 17 years. J Magn Reson Imaging 29:552–559
Sarikouch S, Peters B, Gutberlet M, Leismann B, Kelter-Kloepping A, Koerperich H, Kuehne T, Beerbaum P (2010) Sex-specific pediatric percentiles for ventricular size and mass as reference values for cardiac MRI: assessment by steady-state free-precession and phase-contrast MRI flow. Circ Cardiovasc Imaging 3:65–76
Kawel-Boehm N, Maceira A, Valsangiacomo-Buechel ER, Vogel-Claussen J, Turkbey EB, Williams R, Plein S, Tee M, Eng J, Bluemke DA (2015) Normal values for cardiovascular magnetic resonance in adults and children. J Cardiovasc Magn Reson 17:29
Wühl E, Witte K, Soergel M, Mehls O, Schaefer F, German Working Group on Pediatric Hypertension (2002) Distribution of 24-h ambulatory blood pressure in children: normalized reference values and role of body dimensions. J Hypertens 20:1995–2007
Neuhauser HK, Thamm M, Ellert U, Hense HW, Rosario AS (2011) Blood pressure percentiles by age and height from nonoverweight children and adolescents in Germany. Pediatrics 127:e978–e988
Neuhauser H, Schienkiewitz A, Schaffrath Rosario A, Dortschy R, Kurth B-M (2013) Referenzperzentile für anthropometrische Maßzahlen und Blutdruck aus der Studie zur Gesundheit von Kindern und Jugendlichen in Deutschland (KiGGS) 2003–2006, 2nd edn. Robert Koch-Institut, Berlin
Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1:307–310
Cohen J (1960) A coefficient of agreement for nominal scales. Educ Psychol Meas 20:37–46
Altman DG (1991) Practical statistics for medical research, 1st edn. Chapman and Hall, Oxford
Schwartz GJ, Brion LP, Spitzer A (1987) The use of plasma creatinine concentration for estimating glomerular filtration rate in infants, children, and adolescents. Pediatr Clin North Am 34:571–590
Filler G, Lepage N (2003) Should the Schwartz formula for estimation of GFR be replaced by cystatin C formula? Pediatr Nephrol 18:981–985
Oh J, Wunsch R, Turzer M, Bahner M, Raggi P, Querfeld U, Mehls O, Schaefer F (2002) Advanced coronary and carotid arteriopathy in young adults with childhood-onset chronic renal failure. Circulation 106:100–105
Missouris CG, Forbat SM, Singer DR, Markandu ND, Underwood R, MacGregor GA (1996) Echocardiography overestimates left ventricular mass: a comparative study with magnetic resonance imaging in patients with hypertension. J Hypertens 14:1005–1010
Perdrix L, Mansencal N, Cocheteux B, Chatellier G, Bissery A, Diebold B, Mousseaux E, Abergel E (2011) How to calculate left ventricular mass in routine practice? An echocardiographic versus cardiac magnetic resonance study. Arch Cardiovasc Dis 104:343–351
Barker PCA, Pasquali SK, Darty S, Ing RJ, Li JS, Kim RJ, DeArmey S, Kishnani PS, Campbell MJ (2010) Use of cardiac magnetic resonance imaging to evaluate cardiac structure, function and fibrosis in children with infantile Pompe disease on enzyme replacement therapy. Mol Genet Metab 101:332–337
Malikenas A, Cerniauskiene V, Jakutovic M, Jankauskiene A (2005) Left ventricular geometry in children with chronic renal failure. Med Kaunas Lith 41(Suppl 1):5–11
Raimondi F, Chinali M, Girfoglio D, Benincasa M, Pasquini L, Emma F, de Simone G, Chiara Matteucci M (2009) Inappropriate left ventricular mass in children and young adults with chronic renal insufficiency. Pediatr Nephrol 24:2015–2022
McGill RL, Biederman RWW, Getts RT, Hazlett SM, Sharma SB, Duran J, Brandys DE, Sysak JC, Sureshkumar KK, Sandroni SE, Marcus RJ (2009) Cardiac magnetic resonance imaging in hemodialysis patients. J Nephrol 22:367–372
Chen S-C, Su H-M, Hung C-C, Chang J-M, Liu W-C, Tsai J-C, Lin M-Y, Hwang S-J, Chen H-C (2011) Echocardiographic parameters are independently associated with rate of renal function decline and progression to dialysis in patients with chronic kidney disease. Clin J Am Soc Nephrol 6:2750–2758
Tsioufis C, Kokkinos P, Macmanus C, Thomopoulos C, Faselis C, Doumas M, Stefanadis C, Papademetriou V (2010) Left ventricular hypertrophy as a determinant of renal outcome in patients with high cardiovascular risk. J Hypertens 28:2299–2308
Andrikou E, Tsioufis C, Thomopoulos C, Andrikou I, Kasiakogias A, Leontsinis I, Kordalis A, Katsimichas T, Tousoulis D, Stefanadis C (2012) Left ventricular mass index as a predictor of new-onset microalbuminuria in hypertensive subjects: a prospective study. Am J Hypertens 25:1195–1201
Cuspidi C, Meani S, Negri F, Giudici V, Valerio C, Sala C, Zanchetti A, Mancia G (2009) Indexation of left ventricular mass to body surface area and height to allometric power of 2.7: is the difference limited to obese hypertensives? J Hum Hypertens 23:728–734
Zoccali C, Benedetto FA, Mallamaci F, Tripepi G, Giacone G, Cataliotti A, Seminara G, Stancanelli B, Malatino LS, Investigators CREED (2001) Prognostic impact of the indexation of left ventricular mass in patients undergoing dialysis. J Am Soc Nephrol 12:2768–2774
Cuspidi C, Facchetti R, Bombelli M, Sala C, Tadic M, Grassi G, Mancia G (2015) Prognostic value of left ventricular mass normalized to different body size indexes: findings from the PAMELA population. J Hypertens 33:1082–1089
De Simone G, Kizer JR, Chinali M, Roman MJ, Bella JN, Best LG, Lee ET, Devereux RB, Strong Heart Study Investigators (2005) Normalization for body size and population-attributable risk of left ventricular hypertrophy: the strong heart study. Am J Hypertens 18:191–196
Foppa M, Duncan BB, Rohde LEP (2005) Echocardiography-based left ventricular mass estimation. How should we define hypertrophy? Cardiovasc Ultrasound 3:17
Armstrong AC, Gjesdal O, Almeida A, Nacif M, Wu C, Bluemke DA, Brumback L, Lima JAC (2014) Left ventricular mass and hypertrophy by echocardiography and cardiac magnetic resonance: the multi-ethnic study of atherosclerosis. Echocardiography 31:12–20
Simpson JM, Rawlins D, Mathur S, Chubb H, Sinha MD (2013) Systolic and diastolic ventricular function assessed by tissue Doppler imaging in children with chronic kidney disease. Echocardiography 30:331–337
Ley S, Eichhorn J, Ley-Zaporozhan J, Ulmer H, Schenk J-P, Kauczor H-U, Arnold R (2007) Evaluation of aortic regurgitation in congenital heart disease: value of MR imaging in comparison to echocardiography. Pediatr Radiol 37:426–436
Weaver DJ, Kimball TR, Koury PR, Mitsnefes MM (2009) Cardiac output and associated left ventricular hypertrophy in pediatric chronic kidney disease. Pediatr Nephrol 24:565–570
Lindblad YT, Axelsson J, Balzano R, Vavilis G, Chromek M, Celsi G, Bárány P (2013) Left ventricular diastolic dysfunction by tissue Doppler echocardiography in pediatric chronic kidney disease. Pediatr Nephrol 28:2003–2013
Dogan CS, Akman S, Simsek A, Ozdem S, Comak E, Gokceoglu AU, Kardelen F, Koyun M (2015) Assessment of left ventricular function by tissue Doppler echocardiography in pediatric chronic kidney disease. Ren Fail. doi:10.3109/0886022X.2015.1061301
Lu X, Xie M, Tomberlin D, Klas B, Nadvoretskiy V, Ayres N, Towbin J, Ge S (2008) How accurately, reproducibly, and efficiently can we measure left ventricular indices using M-mode, 2-dimensional, and 3-dimensional echocardiography in children? Am Heart J 155:946–953
Pacileo G, Castaldi B, Di Salvo G, Limongelli G, Rea A, D’Andrea A, Russo MG, Calabrò R (2013) Assessment of left-ventricular mass and remodeling in obese adolescents: M-mode, 2D or 3D echocardiography? J Cardiovasc Med 14:144–149
Friedberg MK, Su X, Tworetzky W, Soriano BD, Powell AJ, Marx GR (2010) Validation of 3D echocardiographic assessment of left ventricular volumes, mass, and ejection fraction in neonates and infants with congenital heart disease: a comparison study with cardiac MRI. Circ Cardiovasc Imaging 3:735–742
Foster BJ, Mackie AS, Mitsnefes M, Ali H, Mamber S, Colan SD (2008) A novel method of expressing left ventricular mass relative to body size in children. Circulation 117:2769–2775
Acknowledgments
The authors would like to thank Adriana Komancsek (radiographer) for the competent acquisition of CMR images.
Ethical approval
The study confirmed to the declaration of Helsinki, was approved by the ethics committee of the University of Freiburg and registered in the German registry of clinical trials (Deutsches Register Klinische Studien, trial no. DRKS00003295).
Informed consent
Prior written informed consent was obtained from all parents (and adolescents where appropriate).
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary table
Available pediatric normal values for left ventricular dimensions (DOCX 39 kb)
Glossary
- BSA
-
Body surface area
- CMR(−)
-
Cardiac magnetic resonance/measured by CMR
- Echo(−)
-
Echocardiography/ echocardiographicaly measured
- EF
-
Ejection fraction
- LVM
-
Left ventricular mass
- LVH
-
Left ventricular hypertrophy
- LVMI
-
LVM indexed to height in m2.7
- LVMBSA
-
LVM normalized to body surface area
- ABPM
-
24-hour ambulatory blood pressure measurement
- CKD
-
Chronic kidney disease
- CI
-
Confidence interval
Rights and permissions
About this article
Cite this article
Arnold, R., Schwendinger, D., Jung, S. et al. Left ventricular mass and systolic function in children with chronic kidney disease—comparing echocardiography with cardiac magnetic resonance imaging. Pediatr Nephrol 31, 255–265 (2016). https://doi.org/10.1007/s00467-015-3198-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-015-3198-z