Abstract
Background and aims
Transmural EUS-guided gallbladder drainage (EUS-GBD) has been increasingly used in the treatment of gallbladder diseases. Aims of the study were to provide a comprehensive meta-analysis and meta-regression of features and outcomes of this procedure.
Methods
MEDLINE, Scopus, Web of science, and Cochrane databases were searched for literature pertinent to transmural EUS-GBD up to May 2021. Random-effect meta-analysis of proportions and meta-regression of potential modifiers of outcome measures considered were applied. Outcome measures were technical success rate, overall clinical success, and procedure-related adverse events (AEs).
Results
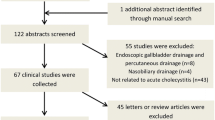
Twenty-seven articles were identified including 1004 patients enrolled between February 2009 and February 2020. Acute cholecystitis was present in 98.7% of cases. Pooled technical success was 98.0% (95% CI 96.3, 99.3; heterogeneity: 23.6%), the overall clinical success was 95.4% (95% CI 92.8, 97.5; heterogeneity: 35.3%), and procedure-related AEs occurred in 14.8% (95% CI 8.8, 21.8; heterogeneity: 82.4%), being stent malfunction/dislodgement the most frequent (3.5%). Procedural-related mortality was 1‰. Meta-regression showed that center experience proxied to > 10 cases/year increased the technical success rate (odds ratio [OR]: 2.84; 95% CI 1.06, 7.59) and the overall clinical success (OR: 3.52; 95% CI 1.33, 9.33). The use of anti-migrating devices also increased the overall clinical success (OR: 2.16; 95% CI 1.07, 4.36) while reducing procedure-related AEs (OR: 0.36; 95% CI 0.14, 0.98).
Conclusion
Physicians’ experience and anti-migrating devices are the main determinants of main clinical outcomes after EUS-GBD, suggesting that treatment in expert centers would optimize results.


Similar content being viewed by others
References
Podboy A, Yuan J, Stave CD, Chan SM, Hwang JH, Teoh AYB (2021) Comparison of EUS-guided endoscopic transpapillary and percutaneous gallbladder drainage for acute cholecystitis: a systematic review with network meta-analysis. Gastrointest Endosc 93(4):797-804.e1. https://doi.org/10.1016/j.gie.2020.09.040
van Houwelingen HC, Arends LR, Stijnen T (2002) Advanced methods in meta-analysis: multivariate approach and meta-regression. Stat Med 21(4):589–624. https://doi.org/10.1002/sim.1040
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA 283(15):2008–2012. https://doi.org/10.1001/jama.283.15.2008
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 29(372):n71. https://doi.org/10.1136/bmj.n71
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng HY, Corbett MS, Eldridge SM, Emberson JR, Hernán MA, Hopewell S, Hróbjartsson A, Junqueira DR, Jüni P, Kirkham JJ, Lasserson T, Li T, McAleenan A, Reeves BC, Shepperd S, Shrier I, Stewart LA, Tilling K, White IR, Whiting PF, Higgins JPT (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 28(366):l4898. https://doi.org/10.1136/bmj.l4898
Joanna Briggs Institute (2017) Checklist for case-series. https://jbi.global/critical-appraisal-tools
Nyaga VN, Arbyn M, Aerts M (2014) Metaprop: a Stata command to perform meta-analysis of binomial data. Arch Public Health 72(1):39. https://doi.org/10.1186/2049-3258-72-39
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 19(14):135. https://doi.org/10.1186/1471-2288-14-135
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558. https://doi.org/10.1002/sim.1186
Lisotti A, Linguerri R, Bacchilega I, Cominardi A, Marocchi G, Fusaroli P (2021) EUS-guided gallbladder drainage in high-risk surgical patients with acute cholecystitis-procedure outcomes and evaluation of mortality predictors. Surg Endosc 28:1–10. https://doi.org/10.1007/s00464-021-08318-z
Teoh AYB, Kitano M, Itoi T, Pérez-Miranda M, Ogura T, Chan SM, Serna-Higuera C, Omoto S, Torres-Yuste R, Tsuichiya T, Wong KT, Leung CH, Chiu PWY, Ng EKW, Lau JYW (2020) Endosonography-guided gallbladder drainage versus percutaneous cholecystostomy in very high-risk surgical patients with acute cholecystitis: an international randomised multicentre controlled superiority trial (DRAC 1). Gut 69(6):1085–1091. https://doi.org/10.1136/gutjnl-2019-319996
Cho SH, Oh D, Song TJ, Park DH, Seo DW, Lee SK, Kim MH, Lee YN, Moon JH, Lee SS (2020) Comparison of the effectiveness and safety of lumen-apposing metal stents and anti-migrating tubular self-expandable metal stents for EUS-guided gallbladder drainage in high surgical risk patients with acute cholecystitis. Gastrointest Endosc 91(3):543–550. https://doi.org/10.1016/j.gie.2019.09.042
Ogura T, Nishioka N, Yamada M, Yamada T, Higuchi K (2021) EUS-guided gallbladder drainage using an improved self-expandable covered metal stent with anti-stent migration system (with video). Dig Dis 39(2):150–155. https://doi.org/10.1159/000509215
Sagami R, Hayasaka K, Ujihara T, Nakahara R, Murakami D, Iwaki T, Katsuyama Y, Harada H, Tsuji H, Sato T, Nishikiori H, Murakami K, Amano Y (2020) Feasibility of endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis patients receiving antithrombotic therapy. Ann Gastroenterol 33(4):391–397. https://doi.org/10.20524/aog.2020.0496
Yakira ND, Kadded G, Dixon RE, Confer B, Shah RN, Khara HS et al (2020) Endoscopic ultrasound guided gallbladder drainage (EUS-GBD) with lumen apposing metal stents (LAMS) in patients with acute cholecystitis has excellent long-term outcomes: a large, multicenter us study. Gastrointestinal Endosc 91:AB298–AB299. https://doi.org/10.1016/j.gie.2020.03.2106
Teoh AY, Perez-Miranda M, Kunda R, Lee SS, Irani S, Yeaton P, Sun S, Baron TH, Moon JH, Holt B, Khor CJL, Rerknimitr R, Bapaye A, Chan SM, Choi HJ, James TW, Kongkam P, Lee YN, Parekh P, Ridtitid W, Serna-Higuera C, Tan DMY, Torres-Yuste R (2019) Outcomes of an international multicenter registry on EUS-guided gallbladder drainage in patients at high risk for cholecystectomy. Endosc Int Open 7(8):E964–E973. https://doi.org/10.1055/a-0915-2098
Oh D, Song TJ, Cho DH, Park DH, Seo DW, Lee SK, Kim MH, Lee SS (2019) EUS-guided cholecystostomy versus endoscopic transpapillary cholecystostomy for acute cholecystitis in high-risk surgical patients. Gastrointest Endosc 89(2):289–298. https://doi.org/10.1016/j.gie.2018.08.052
Kanno Y, Kozakai F, Koshita S, Ogawa T, Kusunose H, Masu K, Sakai T, Murabayashİ T, Ito K (2019) Technical issues stemming from endoscopic-ultrasound-guided gallbladder drainage: a single center experience. Turk J Gastroenterol 30(12):1055–1061. https://doi.org/10.5152/tjg.2019.181032
James TW, Krafft M, Croglio M, Nasr J, Baron T (2019) EUS-guided gallbladder drainage in patients with cirrhosis: results of a multicenter retrospective study. Endosc Int Open 7(9):E1099–E1104. https://doi.org/10.1055/a-0965-6662
Kozakai F, Kanno Y, Ito K, Koshita S, Ogawa T, Kusunose H, Masu K, Sakai T, Murabayashi T, Yonamine K, Kawakami Y, Fujii Y, Miyamoto K, Noda Y (2019) Endoscopic ultrasonography-guided gallbladder drainage as a treatment option for acute cholecystitis after metal stent placement in malignant biliary strictures. Clin Endosc 52(3):262–268. https://doi.org/10.5946/ce.2018.183
Teeratorn N, WiriyapornRidtitid W, Piyachaturawat P, Kongkam P, Rerknimitr R (2019) 1029 Outcomes of endoscopic gallbladder drainage in acute cholecystitis: transpapillary approach versus endoscopic ultrasoud-guided transmural approach. Gastrointest Endosc 89:AB132–AB133
Ahmed O, Ogura T, Eldahrouty A, Khalaf H, Mohammed E, Okasha H, Sameer A, Abdelaal U, Higuchi K (2018) Endoscopic ultrasound-guided gallbladder drainage: Results of long-term follow-up. Saudi J Gastroenterol 24(3):183–188. https://doi.org/10.4103/sjg.SJG_506_17
Anderloni A, Attili F, Sferrazza A, Rimbaș M, Costamagna G, Repici A, Larghi A (2017) EUS-guided gallbladder drainage using a lumen-apposing self-expandable metal stent in patients with coagulopathy or anticoagulation therapy: a case series. Endosc Int Open 5(11):E1100–E1103. https://doi.org/10.1055/s-0043-118828
Sowier S, Sowier A, Wiechowska-Kozłowska A, Białecki J, Pyda P (2019) Initial experience with endoscopic ultrasound-guided gallbladder drainage. Wideochir Inne Tech Maloinwazyjne 14(2):195–202. https://doi.org/10.5114/wiitm.2018.79528
Vozzo CF, Simons-Linares CR, Abou Saleh M, Stevens T, Chahal P (2020) Safety of EUS-guided gallbladder drainage using a lumen-apposing metal stent in patients requiring anticoagulation. VideoGIE 5(10):500-503.e1. https://doi.org/10.1016/j.vgie.2020.07.009
Dollhopf M, Larghi A, Will U, Rimbaş M, Anderloni A, Sanchez-Yague A, Teoh AYB, Kunda R (2017) EUS-guided gallbladder drainage in patients with acute cholecystitis and high surgical risk using an electrocautery-enhanced lumen-apposing metal stent device. Gastrointest Endosc 86(4):636–643. https://doi.org/10.1016/j.gie.2017.02.027
Teoh AYB, Serna C, Penas I, Chong CCN, Perez-Miranda M, Ng EKW, Lau JYW (2017) Endoscopic ultrasound-guided gallbladder drainage reduces adverse events compared with percutaneous cholecystostomy in patients who are unfit for cholecystectomy. Endoscopy 49(2):130–138. https://doi.org/10.1055/s-0042-119036
Irani S, Ngamruengphong S, Teoh A, Will U, Nieto J, Abu Dayyeh BK, Gan SI, Larsen M, Yip HC, Topazian MD, Levy MJ, Thompson CC, Storm AC, Hajiyeva G, Ismail A, Chen YI, Bukhari M, Chavez YH, Kumbhari V, Khashab MA (2017) Similar efficacies of endoscopic ultrasound gallbladder drainage with a lumen-apposing metal stent versus percutaneous transhepatic gallbladder drainage for acute cholecystitis. Clin Gastroenterol Hepatol 15(5):738–745. https://doi.org/10.1016/j.cgh.2016.12.021
Manta R, Zulli C, Zullo A, Forti E, Tringali A, Dioscoridi L, Zito F, Bertani H, Conigliaro R, Mutignani M (2017) Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series. Endosc Int Open 5(11):E1111–E1115. https://doi.org/10.1055/s-0043-118659.Erratum.In:EndoscIntOpen.2017Nov;5(11):C3
Choi JH, Kim HW, Lee JC, Paik KH, Seong NJ, Yoon CJ, Hwang JH, Kim J (2017) Percutaneous transhepatic versus EUS-guided gallbladder drainage for malignant cystic duct obstruction. Gastrointest Endosc 85(2):357–364. https://doi.org/10.1016/j.gie.2016.07.067
Kamata K, Takenaka M, Kitano M, Omoto S, Miyata T, Minaga K, Yamao K, Imai H, Sakurai T, Watanabe T, Nishida N, Kudo M (2017) Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis: long-term outcomes after removal of a self-expandable metal stent. World J Gastroenterol 23(4):661–667. https://doi.org/10.3748/wjg.v23.i4.661
Kahaleh M, Perez-Miranda M, Artifon EL, Sharaiha RZ, Kedia P, Peñas I, De la Serna C, Kumta NA, Marson F, Gaidhane M, Boumitri C, Parra V, RondonClavo CM, Giovannini M (2016) International collaborative study on EUS-guided gallbladder drainage: Are we ready for prime time? Dig Liver Dis 48(9):1054–1057. https://doi.org/10.1016/j.dld.2016.05.021
Takagi W, Ogura T, Sano T, Onda S, Okuda A, Masuda D, Imoto A, Takeuchi T, Fukunishi S, Higuchi K (2016) EUS-guided cholecystoduodenostomy for acute cholecystitis with an anti-stent migration and anti-food impaction system; a pilot study. Therap Adv Gastroenterol 9(1):19–25. https://doi.org/10.1177/1756283X15609285
Choi JH, Lee SS, Choi JH, Park DH, Seo DW, Lee SK, Kim MH (2014) Long-term outcomes after endoscopic ultrasonography-guided gallbladder drainage for acute cholecystitis. Endoscopy 46(8):656–661. https://doi.org/10.1055/s-0034-1365720
de la Serna-Higuera C, Pérez-Miranda M, Gil-Simón P, Ruiz-Zorrilla R, Diez-Redondo P, Alcaide N, Sancho-del Val L, Nuñez-Rodriguez H (2013) EUS-guided transenteric gallbladder drainage with a new fistula-forming, lumen-apposing metal stent. Gastrointest Endosc 77(2):303–308. https://doi.org/10.1016/j.gie.2012.09.021
Jang JW, Lee SS, Park DH, Seo DW, Lee SK, Kim MH (2011) Feasibility and safety of EUS-guided transgastric/transduodenal gallbladder drainage with single-step placement of a modified covered self-expandable metal stent in patients unsuitable for cholecystectomy. Gastrointest Endosc 74(1):176–181. https://doi.org/10.1016/j.gie.2011.03.1120
Okamoto K, Suzuki K, Takada T et al (2018) Tokyo guidelines 2018: flowchart for the management of acute cholecystitis. J Hepatobiliary Pancreat Sci 25(1):55–72. https://doi.org/10.1002/jhbp.516
Anderloni A, Buda A, Vieceli F et al (2016) Endoscopic ultrasound-guided transmural stenting for gallbladder drainage in high-risk patients with acute cholecystitis: a systematic review and pooled analysis. Surg Endosc 30:5200–5208
Kalva NR, Vanar V, Forcione D, Bechtold ML, Puli SR (2018) Efficacy and safety of lumen apposing self-expandable metal stents for EUS guided cholecystostomy: a meta-analysis and systematic review. Can J Gastroenterol Hepatol 12(2018):7070961. https://doi.org/10.1155/2018/7070961
Manta R, Mutignani M, Galloro G, Conigliaro R, Zullo A (2018) Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a lumen-apposing metal stent: a systematic review of case series. Eur J Gastroenterol Hepatol 30(7):695–698. https://doi.org/10.1097/MEG.0000000000001112
Jain D, Bhandari BS, Agrawal N, Singhal S (2018) Endoscopic ultrasound-guided gallbladder drainage using a lumen-apposing metal stent for acute cholecystitis: a systematic review. Clin Endosc 51(5):450–462. https://doi.org/10.5946/ce.2018.024
Cotton PB, Eisen GM, Aabakken L, Baron TH, Hutter MM, Jacobson BC, Mergener K, Nemcek A Jr, Petersen BT, Petrini JL, Pike IM, Rabeneck L, Romagnuolo J, Vargo JJ (2010) A lexicon for endoscopic adverse events: report of an ASGE workshop. Gastrointest Endosc 71(3):446–454. https://doi.org/10.1016/j.gie.2009.10.027
Tyberg A, Jha K, Shah S, Kedia P, Gaidhane M, Kahaleh M (2020) EUS-guided gallbladder drainage: a learning curve modified by technical progress. Endosc Int Open 8(1):E92–E96
Rücker G, Schumacher M (2008) Simpson’s paradox visualized: the example of the rosiglitazone meta-analysis. BMC Med Res Methodol 30(8):34. https://doi.org/10.1186/1471-2288-8-34
Author information
Authors and Affiliations
Contributions
CF conceived the hypothesis, planned the study and wrote the manuscript; CB, MS and ED collected data, helped in interpreting results and in manuscript preparation; CC provided quality assessment and final data check for inclusion in the analysis. GE and AA helped in manuscript writing providing important intellectual contents. AC coordinated the study and performed statistical analyses.
Corresponding author
Ethics declarations
Disclosures
Carlo Fabbri is a consultant for Boston Scientific; Andrea Anderloni is a consultant for Medtronic, Boston Scientific, and Olympus. Cecilia Binda, Monica Sbrancia, Elton Dajti, Chiara Coluccio, Giorgio Ercolani, and Alessandro Cucchetti have no financial ties to disclose. The author(s) received no financial support for the research, authorship, and/or publication of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Fabbri, C., Binda, C., Sbrancia, M. et al. Determinants of outcomes of transmural EUS-guided gallbladder drainage: systematic review with proportion meta-analysis and meta-regression. Surg Endosc 36, 7974–7985 (2022). https://doi.org/10.1007/s00464-022-09339-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-022-09339-y