Abstract
Background
Endoscopic ultrasound (EUS)-guided transmural or endoscopic retrograde cholangiography (ERC)-based transpapillary drainage may provide alternative treatment strategies for high-risk surgical candidates with symptomatic gallbladder (GB) disease. The primary aim of this study was to perform a systematic review and meta-analysis to investigate the efficacy and safety of endoscopic GB drainage for patients with symptomatic GB disease.
Methods
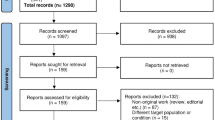
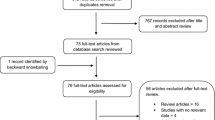
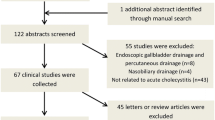
Searches of PubMed, EMBASE, Web of Science, and Cochrane Library databases were performed in accordance with PRISMA and MOOSE guidelines. Pooled proportions were calculated for measured outcomes including technical success, clinical success, adverse event rate, recurrence rate, and rate of reintervention. Subgroup analyses were performed for transmural versus transpapillary, transmural lumen apposing stent (LAMS), and comparison to percutaneous transhepatic drainage. Heterogeneity was assessed with I2 statistics. Publication bias was ascertained by funnel plot and Egger regression testing.
Results
Thirty-six studies (n = 1538) were included. Overall, endoscopic GB drainage achieved a technical and clinical success of 87.33% [(95% CI 84.42–89.77); I2 = 39.55] and 84.16% [(95% CI 80.30–87.38); I2 = 52.61], with an adverse event rate of 11.00% [(95% CI 9.25–13.03); I2 = 7.08]. On subgroup analyses, EUS-guided transmural compared to ERC-assisted transpapillary drainage resulted in higher technical and clinical success rates [OR 3.91 (95% CI 1.52–10.09); P = 0.005 and OR 4.59 (95% CI 1.84–11.46); P = 0.001] and lower recurrence rate [OR 0.17 (95% CI 0.06–0.52); P = 0.002]. Among EUS-guided LAMS studies, technical success was 94.65% [(95% CI 91.54–96.67); I2 = 0.00], clinical success was 92.06% [(95% CI 88.65–94.51); I2 = 0.00], and adverse event rate was 11.71% [(95% CI 8.92–15.23); I2 = 0.00]. Compared to percutaneous drainage, EUS-guided drainage possessed a similar efficacy and safety with significantly lower rate of reintervention [OR 0.05 (95% CI 0.02–0.13); P < 0.001].
Discussion
Endoscopic GB drainage is a safe and effective treatment for high-risk surgical candidates with symptomatic GB disease. EUS-guided transmural drainage is superior to transpapillary drainage and associated with a lower rate of reintervention compared to percutaneous transhepatic drainage.







Similar content being viewed by others
References
Shaffer EA (2005) Epidemiology and risk factors for gallstone disease: has the paradigm changed in the 21st century? Curr Gastroenterol Rep 7:132–140
Everhart JE, Khare M, Hill M, Maurer KR (1999) Prevalence and ethnic differences in gallbladder disease in the United States. Gastroenterology 117:632–639
Schirmer BD, Winters KL, Edlich RF (2005) Cholelithiasis and cholecystitis. J Long Term Eff Med Implants 15:329–338
Stinton LM, Shaffer EA (2012) Epidemiology of gallbladder disease: cholelithiasis and cancer. Gut Liver 6:172–187
Tazuma S (2006) Gallstone disease: Epidemiology, pathogenesis, and classification of biliary stones (common bile duct and intrahepatic). Best Pract Res Clin Gastroenterol 20:1075–1083
Adler DG (2019) Endoscopic Gallbladder Drainage. Am J Gastroenterol 114:700–702
Chaudhary S, Sun S (2016) Endoscopic ultrasound-guided gallbladder drainage: Redefines the boundaries. Endosc Ultrasound 5:281–283
Bakkaloglu H, Yanar H, Guloglu R et al (2006) Ultrasound guided percutaneous cholecystostomy in high-risk patients for surgical intervention. World J Gastroenterol 12:7179–7182
Lee SS, Park DH, Hwang CY et al (2007) EUS-guided transmural cholecystostomy as rescue management for acute cholecystitis in elderly or high-risk patients: a prospective feasibility study. Gastrointest Endosc 66:1008–1012
McKay A, Abulfaraj M, Lipschitz J (2012) Short- and long-term outcomes following percutaneous cholecystostomy for acute cholecystitis in high-risk patients. Surg Endosc 26:1343–1351
Itoi T, Coelho-Prabhu N, Baron TH (2010) Endoscopic gallbladder drainage for management of acute cholecystitis. Gastrointest Endosc 71:1038–1045
Itoi T, Binmoeller KF, Shah J et al (2012) Clinical evaluation of a novel lumen-apposing metal stent for endosonography-guided pancreatic pseudocyst and gallbladder drainage (with videos). Gastrointest Endosc 75:870–876
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA 283:2008–2012
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Controlled Clin Trials 7:177–188
Stuart A, Ord JK (1994) Kendall’s Advanced Theory of Statistics, 6th edn. Edward Arnold, London
Gingrich RA, Awe WC, Boyden AM, Peterson CG (1968) Cholecystostomy in acute cholecystitis Factors influencing morbidity and mortality. Am J Surg 116:310–315
Overton RC (1998) A comparison of fixed-effects and mixed (random-effects) models for meta-analysis tests of moderator variable effects. Psychol Methods 3(3):354–379
Wells G, Shea B, et al. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analysis. 3rd Symposium on Systematic Reviews: Beyond the Basics; July 3–5; Oxford. 2000. https://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 24 August 2019.
Jadad AR, Moore RA, Carroll D et al (1996) Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials 17:1–12
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Borenstein M, Higgins JP, Hedges LV, Rothstein HR (2017) Basics of meta-analysis: I(2) is not an absolute measure of heterogeneity. Res Synth Methods 8:5–18
Mohan BP, Adler DG (2019) Heterogeneity in systematic review and meta-analysis: how to read between the numbers. Gastrointest Endosc 89:902–903
Borenstein M, Hedges LV, Higgins JP et al (2011) Introduction to meta- analysis. Wiley, Hoboken
Higgins J, Thompson SG, Spiegelhalter DJ (2009) A re-evaluation of random-effects meta-analysis. J R Statist Soc A 172:137–159
Kamata K, Takenaka M, Kitano M et al (2017) Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis: long-term outcomes after removal of a self-expandable metal stent. World J Gastroenterol 23:661–667
Dollhopf M, Larghi A, Will U et al (2017) EUS-guided gallbladder drainage in patients with acute cholecystitis and high surgical risk using an electrocautery-enhanced lumen-apposing metal stent device. Gastrointest Endosc 86:636–643
Higa JT, Sahar N, Kozarek RA et al (2019) EUS-guided gallbladder drainage with a lumen-apposing metal stent versus endoscopic transpapillary gallbladder drainage for the treatment of acute cholecystitis (with videos). Gastrointest Endosc 90:483–492
Song TJ, Park DH, Eum JB et al (2010) EUS-guided cholecystoenterostomy with single-step placement of a 7F double-pigtail plastic stent in patients who are unsuitable for cholecystectomy: a pilot study (with video). Gastrointest Endosc 71:634–640
Jang JW, Lee SS, Song TJ et al (2012) Endoscopic ultrasound-guided transmural and percutaneous transhepatic gallbladder drainage are comparable for acute cholecystitis. Gastroenterology 142:805–811
de la Serna-Higuera C, Perez-Miranda M, Gil-Simon P et al (2013) EUS-guided transenteric gallbladder drainage with a new fistula-forming, lumen-apposing metal stent. Gastrointest Endosc 77:303–308
Choi JH, Lee SS, Choi JH et al (2014) Long-term outcomes after endoscopic ultrasonography-guided gallbladder drainage for acute cholecystitis. Endoscopy 46:656–661
Moon JH, Choi HJ, Kim DC et al (2014) A newly designed fully covered metal stent for lumen apposition in EUS-guided drainage and access: a feasibility study (with videos). Gastrointest Endosc 79:990–995
Walter D, Teoh AY, Itoi T et al (2016) EUS-guided gall bladder drainage with a lumen-apposing metal stent: a prospective long-term evaluation. Gut 65:6–8
Ge N, Sun S, Sun S, Wang S, Liu X, Wang G (2016) Endoscopic ultrasound-assisted transmural cholecystoduodenostomy or cholecystogastrostomy as a bridge for per-oral cholecystoscopy therapy using double-flanged fully covered metal stent. BMC Gastroenterol 16:9
Kahaleh M, Perez-Miranda M, Artifon EL et al (2016) International collaborative study on EUS-guided gallbladder drainage: Are we ready for prime time? Dig Liver Dis 48:1054–1057
Manta R, Zulli C, Zullo A et al (2017) Endoscopic ultrasound-guided gallbladder drainage for acute cholecystitis with a silicone-covered nitinol short bilaterally flared stent: a case series. Endosc Int Open 5:E1111–E1115
Oh D, Song TJ, Cho DH et al (2019) EUS-guided cholecystostomy versus endoscopic transpapillary cholecystostomy for acute cholecystitis in high-risk surgical patients. Gastrointest Endosc 89:289–298
Siddiqui A, Kunda R, Tyberg A et al (2019) Three-way comparative study of endoscopic ultrasound-guided transmural gallbladder drainage using lumen-apposing metal stents versus endoscopic transpapillary drainage versus percutaneous cholecystostomy for gallbladder drainage in high-risk surgical patients with acute cholecystitis: clinical outcomes and success in an International. Multicenter Study Surg Endosc 33:1260–1270
Teoh AY, Kitano A, Itoi K, et al. EUS-guided Gallbladder drainage reduced adverse events as compared to percutaneous cholecystectomy in patients suffering from acute cholecystitis that were at high risk for cholecystectomy A Randomized Controlled Trial. 2019; 89(6), Supplement: AB130–AB131.
Tamada K, Seki H, Sato K et al (1991) Efficacy of endoscopic retrograde cholecystoendoprosthesis (ERCCE) for cholecystitis. Endoscopy 23:2–3
Feretis C, Apostolidis N, Mallas E, Manouras A, Papadimitriou J (1993) Endoscopic drainage of acute obstructive cholecystitis in patients with increased operative risk. Endoscopy 25:392–395
Nakatsu T, Okada H, Saito K et al (1997) Endoscopic transpapillary gallbladder drainage (ETGBD) for the treatment of acute cholecystitis. J Hep Bil Pancr Surg 4:31–35
Schlenker C, Trotter JF, Shah RJ et al (2006) Endoscopic gallbladder stent placement for treatment of symptomatic cholelithiasis in patients with end-stage liver disease. Am J Gastroenterol 101:278–283
Kjaer DW, Kruse A, Funch-Jensen P (2007) Endoscopic gallbladder drainage of patients with acute cholecystitis. Endoscopy 39:304–308
Itoi T, Sofuni A, Itokawa F et al (2008) Endoscopic transpapillary gallbladder drainage in patients with acute cholecystitis in whom percutaneous transhepatic approach is contraindicated or anatomically impossible (with video). Gastrointest Endosc 68:455–460
Ogawa O, Yoshikumi H, Maruoka N et al (2008) Predicting the success of endoscopic transpapillary gallbladder drainage for patients with acute cholecystitis during pretreatment evaluation. Can J Gastroenterol 22:681–685
Pannala R, Petersen BT, Gostout CJ, Topazian MD, Levy MJ, Baron TH (2008) Endoscopic transpapillary gallbladder drainage: 10-year single center experience. Minerva Gastroenterol Dietol 54:107–113
Conway JD, Russo MW, Shrestha R (2005) Endoscopic stent insertion into the gallbladder for symptomatic gallbladder disease in patients with end-stage liver disease. Gastrointest Endosc 61:32–36
Mutignani M, Iacopini F, Perri V et al (2009) Endoscopic gallbladder drainage for acute cholecystitis: technical and clinical results. Endoscopy 41:539–546
Lee TH, Park DH, Lee SS et al (2011) Outcomes of endoscopic transpapillary gallbladder stenting for symptomatic gallbladder diseases: a multicenter prospective follow-up study. Endoscopy 43:702–708
Maekawa S, Nomura R, Murase T, Ann Y, Oeholm M, Harada M (2013) Endoscopic gallbladder stenting for acute cholecystitis: a retrospective study of 46 elderly patients aged 65 years or older. BMC Gastroenterol 13:65
Widmer J, Alvarez P, Sharaiha RZ et al (2015) Endoscopic gallbladder drainage for acute cholecystitis. Clin Endosc 48:411–420
McCarthy ST, Tujios S, Fontana RJ et al (2015) Endoscopic transpapillary gallbladder stent placement is safe and effective in high-risk patients without cirrhosis. Dig Dis Sci 60:2516–2522
Yane K, Maguchi H, Katanuma A et al (2015) Feasibility, efficacy, and predictive factors for the technical success of endoscopic nasogallbladder drainage: a prospective study. Gut Liver 9:239–246
Itoi T, Kawakami H, Katanuma A et al (2015) Endoscopic nasogallbladder tube or stent placement in acute cholecystitis: a preliminary prospective randomized trial in Japan (with videos). Gastrointest Endosc 81:111–118
Yang MJ, Yoo BM, Kim JH et al (2016) Endoscopic naso-gallbladder drainage versus gallbladder stenting before cholecystectomy in patients with acute cholecystitis and a high suspicion of choledocholithiasis: a prospective randomised preliminary study. Scand J Gastroenterol 51:472–478
Inoue T, Okumura F, Kachi K et al (2016) Long-term outcomes of endoscopic gallbladder stenting in high-risk surgical patients with calculous cholecystitis (with videos). Gastrointest Endosc 83:905–913
Iino C, Shimoyama T, Igarashi T et al (2018) Comparable efficacy of endoscopic transpapillary gallbladder drainage and percutaneous transhepatic gallbladder drainage in acute cholecystitis. Endosc Int Open 6:E594–E601
Kedia P, Sharaiha RZ, Kumta NA et al (2015) Endoscopic gallbladder drainage compared with percutaneous drainage. Gastrointest Endosc 82:1031–1036
Irani S, Ngamruengphong S, Teoh A et al (2017) Similar efficacies of endoscopic ultrasound gallbladder drainage with a lumen-apposing metal stent versus percutaneous transhepatic gallbladder drainage for acute cholecystitis. Clin Gastroenterol Hepatol 15:738–745
Saumoy M, Tyberg A, Brown E et al (2019) Successful cholecystectomy after endoscopic ultrasound gallbladder drainage compared with percutaneous cholecystostomy, Can it be done? J Clin Gastroenterol 53:231–235
Teoh AYB, Serna C, Penas I et al (2017) Endoscopic ultrasound-guided gallbladder drainage reduces adverse events compared with percutaneous cholecystostomy in patients who are unfit for cholecystectomy. Endoscopy 49:130–138
Kozarek RA (1984) Selective cannulation of the cystic duct at time of ERCP. J Clin Gastroenterol 6:37–40
Feretis CB, Manouras AJ, Apostolidis NS, Golematis BC (1990) Endoscopic transpapillary drainage of gallbladder empyema. Gastrointest Endosc 36:523–525
Chan JHY, Teoh AYB (2018) Current status of endoscopic gallbladder drainage. Clin Endosc 51:150–155
Boregowda U, Umapathy C, Nanjappa A et al (2018) Endoscopic ultrasound guided gallbladder drainage—Is it ready for prime time? World J Gastrointest Pharmacol Ther 9:47–54
Werbel GB, Nahrwold DL, Joehl RJ, Vogelzang RL, Rege RV (1989) Percutaneous cholecystostomy in the diagnosis and treatment of acute cholecystitis in the high-risk patient. Arch Surg 124:782–785 discussion 5-6
Jang JW, Lee SS, Park DH, Seo DW, Lee SK, Kim MH (2011) Feasibility and safety of EUS-guided transgastric/transduodenal gallbladder drainage with single-step placement of a modified covered self-expandable metal stent in patients unsuitable for cholecystectomy. Gastrointest Endosc 74:176–181
McGahan JP, Lindfors KK (1989) Percutaneous cholecystostomy: an alternative to surgical cholecystostomy for acute cholecystitis? Radiology 173:481–485
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Marvin Ryou has the following disclosures: Medtronic/Covidien—Consultant, Pentax—Consultant. Christopher C Thompson has the following disclosures: Apollo Endosurgery—Consultant/Research Support (Consulting fees/Institutional Research Grants), Aspire Bariatrics—Research Support (Institutional Research Grant), BlueFlame Healthcare Venture Fund—General Partner, Boston Scientific—Consultant (Consulting fees), Covidien/Medtronic—Consultant (Consulting Fees), EnVision Endoscopy (Board Member), Fractyl—Consultant/Advisory Board Member (Consulting Fees), GI Dynamics—Consultant (Consulting Fees)/ Research Support (Institutional Research Grant), GI Windows—Ownership interest, Olympus/Spiration—Consultant (Consulting Fees)/Research Support (Equipment Loans). Spatz—Research Support (Institutional Research Grant), USGI Medical—Consultant (Consulting Fees)/Advisory Board Member (Consulting fees)/Research Support (Research Grant). All authors approve of final submission. Thomas R. McCarty, Kelly E. Hathorn, Ahmad Najdat Bazarbashi, and Kunal Jajoo have no conflicts of interest of financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.



Rights and permissions
About this article
Cite this article
McCarty, T.R., Hathorn, K.E., Bazarbashi, A.N. et al. Endoscopic gallbladder drainage for symptomatic gallbladder disease: a cumulative systematic review meta-analysis. Surg Endosc 35, 4964–4985 (2021). https://doi.org/10.1007/s00464-020-07758-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07758-3