Abstract
Background
Technical advances in laparoscopy and enhanced recovery after surgery programs have progressively decreased the need for hospitalization. The present study aimed to explore the feasibility and safety of an early discharge protocol after minor laparoscopic liver resection (LLR).
Methods
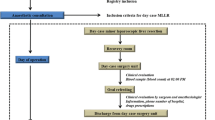
The study sample consisted of patients with both benign and malignant hepatic lesions involving no more than two hepatic segments who underwent minor LLR and were discharged within 24 h. Patients were selected based on their fitness for surgery, proximity to the hospital, and availability of a responsible adult to care for them once discharged. Patients and their accompanying caregiver were instructed about the procedure, its potential complications, and the conditions required for an early discharge. They were also provided with a 24-h dedicated phone number for assistance.
Results
Twenty-four patients [mean age 48.9 year (SD 14.75); 12 women] with no more than one comorbidity were included. The majority (87.5%) was classified as ASA I or II. Thirteen patients (46%) were operated on for malignant lesions. The median operative time was 90 min, the median pneumoperitoneum time was 60 min, and the estimated blood loss was 50 mL. Mortality was zero. No transfusion, conversion, or pedicule clamping was necessary. No anesthesia-related complications occurred. All patients were discharged at 24 h. Only one patient (4.2%) was readmitted at postoperative day 3 for intolerable abdominal pain due to a wound abscess that was treated by antibiotics.
Conclusion
By applying a standardized protocol for admission, preoperative workup, and anesthesia, early discharge after minor LLR can be successfully carried out in highly selected patients with minimal impact on primary healthcare services.
Similar content being viewed by others
References
de’Angelis N, Memeo R, Calderaro J, Felli E, Salloum C, Compagnon P, Luciani A, Laurent A, Cherqui D, Azoulay D (2014) Open and laparoscopic resection of hepatocellular adenoma: trends over 23 years at a specialist hepatobiliary unit. HPB 16:783–788
Payne JH Jr, Tashima W, Lapschies B, Washecka R, Hariharan A, Duh QY (1998) Advanced laparoscopy: “the next generation”. The adrenal, kidney, spleen, pancreas, and liver. Hawaii Med J 57:710–714
de’Angelis N, Brunetti F, Felli E, Mehdaoui D, Memeo R, Carra MC, Zuddas V, Azoulay D (2015) Laparoscopic versus open gastric wedge resection for primary gastrointestinal tumors: clinical outcomes and health care costs analysis. Surg Laparosc Endosc Percutan Tech 25:143–146
Arezzo A, Passera R, Scozzari G, Verra M, Morino M (2013) Laparoscopy for rectal cancer reduces short-term mortality and morbidity: results of a systematic review and meta-analysis. Surg Endosc 27:1485–1502
Ahmad NZ, Byrnes G, Naqvi SA (2008) A meta-analysis of ambulatory versus inpatient laparoscopic cholecystectomy. Surg Endosc 22:1928–1934
Leeder PC, Matthews T, Krzeminska K, Dehn TC (2004) Routine day-case laparoscopic cholecystectomy. Br J Surg 91:312–316
Abdullah HR, Chung F (2014) Postoperative issues: discharge criteria. Anesthesiol Clin 32:487–493
Gagner M, Rheault M, Dubuc J (1992) Laparoscopic partial hepatectomy for liver tumor. Surg Endosc 6:99
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS, Asbun H, O’Rourke N, Tanabe M, Koffron AJ, Tsung A, Soubrane O, Machado MA, Gayet B, Troisi RI, Pessaux P, Van Dam RM, Scatton O, Abu Hilal M, Belli G, Kwon CH, Edwin B, Choi GH, Aldrighetti LA, Cai X, Cleary S, Chen KH, Schon MR, Sugioka A, Tang CN, Herman P, Pekolj J, Chen XP, Dagher I, Jarnagin W, Yamamoto M, Strong R, Jagannath P, Lo CM, Clavien PA, Kokudo N, Barkun J, Strasberg SM (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629
Nguyen KT, Gamblin TC, Geller DA (2009) World review of laparoscopic liver resection-2804 patients. Ann Surg 250:831–841
Goh BK, Chan CY, Wong JS, Lee SY, Lee VT, Cheow PC, Chow PK, Ooi LL, Chung AY (2015) Factors associated with and outcomes of open conversion after laparoscopic minor hepatectomy: initial experience at a single institution. Surg Endosc 29(9):2636–2642
Scott NB, McDonald D, Campbell J, Smith RD, Carey AK, Johnston IG, James KR, Breusch SJ (2013) The use of enhanced recovery after surgery (ERAS) principles in Scottish orthopaedic units—an implementation and follow-up at 1 year, 2010–2011: a report from the Musculoskeletal Audit, Scotland. Arch Orthop Trauma Surg 133:117–124
Lv D, Wang X, Shi G (2010) Perioperative enhanced recovery programmes for gynaecological cancer patients. Cochrane Database Syst Rev 6:CD008239
Hughes MJ, McNally S, Wigmore SJ (2014) Enhanced recovery following liver surgery: a systematic review and meta-analysis. HPB 16:699–706
Bismuth H (1982) Surgical anatomy and anatomical surgery of the liver. World J Surg 6:3–9
Couinaud C (1956) Contribution of anatomical research to liver surgery. Fr Med 19:5–12
Truant S, Oberlin O, Sergent G, Lebuffe G, Gambiez L, Ernst O, Pruvot FR (2007) Remnant liver volume to body weight ratio > or = 0.5%: a new cut-off to estimate postoperative risks after extended resection in noncirrhotic liver. J Am Coll Surg 204:22–33
de’Angelis N, Eshkenazy R, Brunetti F, Valente R, Costa M, Disabato M, Salloum C, Compagnon P, Laurent A, Azoulay D (2015) Laparoscopic versus open resection for colorectal liver metastases: a single-center study with propensity score analysis. J Laparoendosc Adv Surg Tech A 25:12–20
Bryant R, Laurent A, Tayar C, Cherqui D (2009) Laparoscopic liver resection-understanding its role in current practice: the Henri Mondor Hospital experience. Ann Surg 250:103–111
Memeo R, de’Angelis N, Compagnon P, Salloum C, Cherqui D, Laurent A, Azoulay D (2014) Laparoscopic vs. open liver resection for hepatocellular carcinoma of cirrhotic liver: a case-control study. World J Surg 38:2919–2926
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibanes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien–Dindo classification of surgical complications: 5-year experience. Ann Surg 250:187–196
Cherqui D, Husson E, Hammoud R, Malassagne B, Stephan F, Bensaid S, Rotman N, Fagniez PL (2000) Laparoscopic liver resections: a feasibility study in 30 patients. Ann Surg 232:753–762
Robinson TN, Biffl WL, Moore EE, Heimbach JK, Calkins CM, Burch JM (2002) Predicting failure of outpatient laparoscopic cholecystectomy. Am J Surg 184:515–518 (discussion 518–519)
Tuckey JP, Morris GN, Peden CJ, Tate JJ (1996) Feasibility of day case laparoscopic cholecystectomy in unselected patients. Anaesthesia 51:965–968
Voitk AJ (1997) Is outpatient cholecystectomy safe for the higher-risk elective patient? Surg Endosc 11:1147–1149
Wright MC, Phillips-Bute B, Mark JB, Stafford-Smith M, Grichnik KP, Andregg BC, Taekman JM (2006) Time of day effects on the incidence of anesthetic adverse events. Qual Saf Health Care 15:258–263
Vaughan J, Nagendran M, Cooper J, Davidson BR, Gurusamy KS (2014) Anaesthetic regimens for day-procedure laparoscopic cholecystectomy. Cochrane Database Syst Rev 1:CD009784
Arain MR, Buggy DJ (2007) Anaesthesia for cancer patients. Curr Opin Anaesthesiol 20:247–253
Snyder GL, Greenberg S (2010) Effect of anaesthetic technique and other perioperative factors on cancer recurrence. Br J Anaesth 105:106–115
Tenconi SM, Boni L, Colombo EM, Dionigi G, Rovera F, Cassinotti E (2008) Laparoscopic cholecystectomy as day-surgery procedure: current indications and patients’ selection. Int J Surg 6(Suppl 1):S86–S88
Lledo JB, Planells M, Espi A, Serralta A, Garcia R, Sanahuja A (2008) Predictive model of failure of outpatient laparoscopic cholecystectomy. Surg Laparosc Endosc Percutan Tech 18:248–253
Feldman LS, Lee L, Fiore J Jr (2015) What outcomes are important in the assessment of Enhanced Recovery After Surgery (ERAS) pathways? Can J Anaesth 62:120–130
Wetsch WA, Pircher I, Lederer W, Kinzl JF, Traweger C, Heinz-Erian P, Benzer A (2009) Preoperative stress and anxiety in day-care patients and inpatients undergoing fast-track surgery. Br J Anaesth 103:199–205
Gash KJ, Goede AC, Chambers W, Greenslade GL, Dixon AR (2011) Laparoendoscopic single-site surgery is feasible in complex colorectal resections and could enable day case colectomy. Surg Endosc 25:835–840
Lorente-Herce JM, Marin-Morales J, Jimenez-Vega FJ, Ruiz-Julia ML, Claro-Alves BM, Fernandez-Zulueta A, Gallardo-Garcia PA, Marrero-Cantera S, De Quinta-Frutos R (2015) Laparoscopic incisional hernia repair in an ambulatory surgery-extended recovery centre: a review of 259 consecutive cases. Hernia 19:487–492
Rowe AJ, Meneghetti AT, Schumacher PA, Buczkowski AK, Scudamore CH, Panton ON, Chung SW (2009) Perioperative analysis of laparoscopic versus open liver resection. Surg Endosc 23:1198–1203
Polignano FM, Quyn AJ, de Figueiredo RS, Henderson NA, Kulli C, Tait IS (2008) Laparoscopic versus open liver segmentectomy: prospective, case-matched, intention-to-treat analysis of clinical outcomes and cost effectiveness. Surg Endosc 22:2564–2570
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Nicola de’Angelis, Benjamin Menahem, Jean Claude Merle, Francesco Brunetti, Philippe Compagnon, Alain Luciani, Daniel Cherqui, and Alexis Laurent have no conflicts of interest or financial ties to disclose.
Rights and permissions
About this article
Cite this article
de’Angelis, N., Menahem, B., Compagnon, P. et al. Minor laparoscopic liver resection: toward 1-day surgery?. Surg Endosc 31, 4458–4465 (2017). https://doi.org/10.1007/s00464-017-5498-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-017-5498-9