Abstract
Purpose
Extended resections in hepatopancreatobiliary (HPB) surgery frequently require vascular resection to obtain tumor clearance. The use of alloplastic grafts may increase postoperative morbidity due to septic or thrombotic complications. The use of suitable autologous venous interponates (internal jugular vein, great saphenous vein) is frequently associated with additional incisions. The aim of this study was to report on our experience with venous reconstruction using the introperative easily available parietal peritoneum, focusing on key technical aspects.
Methods
All patients who underwent HPB resections with venous reconstruction using peritoneal patches at our department between January 2017 and November 2021 were included in this retrospective analysis with median follow-up of 2 months (IQR: 1–8 months). We focused on technical aspects of the procedure and evaluated vascular patency and perioperative morbidity.
Results
Parietal peritoneum patches (PPPs) were applied for reconstruction of the inferior vena cava (IVC) (13 patients) and portal vein (PV) (4 patients) during major hepatic (n = 14) or pancreatic (n = 2) resections. There were no cases of postoperative bleeding due to anastomotic leakage. Following PV reconstruction, two patients showed postoperative vascular stenosis after severe pancreatitis with postoperative pancreatic fistula and bile leakage, respectively. In patients with reconstruction of the IVC, no relevant perioperative vascular complications occurred.
Conclusions
The use of a peritoneal patch for reconstruction of the IVC in HPB surgery is a feasible, effective, and low-cost alternative to alloplastic, xenogenous, or venous grafts. The graft can be easily harvested and tailored to the required size. More evidence is still needed to confirm the safety of this procedure for the portal vein regarding long-term results.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multivisceral tumor resections are technically demanding procedures. However, they are the only curative option for patients with locally advanced malignant tumors offering potential long-term survival [1, 2]. The main goal is to achieve tumor clearance by means of a safe surgical procedure. Due to increasing experience in the last decades, vascular resection is now a routine part of extended hepatopancreatobiliary procedures in high-volume centers [3]. A range of surgical techniques (primary anastomosis, graft interposition, or application of patches) using a variety of autologous, xenogenous, or alloplastic grafts and patches are available for reconstruction. Maintaining vascular patency after reconstruction and achieving long-term recurrence-free survival after radical resection are essential for recovery and patient survival. Hence, autologous material is preferred to minimize the risk of infection caused by common septic postoperative complications like biliary leakage, postoperative pancreatic fistula (POPF), and postpancreatectomy acute pancreatitis (PPAP) after HPB procedures [4]. Further advantages of autologous grafts compared to alloplastic grafts include lower costs, no need for anticoagulation after reconstruction, and the option to tailor graft size exactly to the individual geometric need without limitations in size or shape.
In this study, we focus on the peritoneum as autologous tissue graft available for reconstruction of the IVC and PV. Given the first encouraging results in the literature, we adopted this technique and used peritoneal patches for vascular reconstruction in complex multivisceral tumor resections. The largest patient cohort reported to date (52 patients) showed peritoneal patches to be a feasible option for venous reconstruction in HPB surgery [5, 6]. Nevertheless, data in the literature are still very scarce and limited to case reports and small patient collectives mainly with liver resections [5].
We report our experience of using PPPs for venous reconstruction of the IVC and PV in liver and pancreatic surgical procedures and highlight important technical aspects.
Patients and methods
Data were collected retrospectively from all patients who underwent reconstruction of the IVC and PV at our institution from January 2017 to November 2021. We found in total 59 cases with complex surgical multivisceral procedures where a patch or tube interponat for a vascular venous reconstruction was performed. Patients with arterial reconstructions and those with a direct suture vascular anastomosis were excluded since they have not been addressed in the research question. Fifty-eight of the patients included underwent planned elective surgery and in one case, a patch plastic with bovine pericard after thrombectomy of the external iliacal vein in case of graft necrosis after renal transplantation was performed.
We performed in total 48 complex reconstructions of IVC (n = 41) and the PV (n = 8) where a vascular interposition (tube or a patch) was used. Ringed synthetic graft tube (GoreTex®) was applied in 13 cases, when a caval segment has been resected; bovine pericardium (XenoSure® Biologic patch and LeMaitre Vascular®, USA), when a patch reconstruction was needed in 11 cases; an autologous vein in 9 patients for patch reconstruction and tube interposition; and PPPs were used in 17 cases.
We focused on liver and pancreatic resections with PPP vascular reconstruction, as these are procedures associated with significantly higher bacterial contamination and increased risk for septic postoperative complications [6]. Patients who received peritoneal patches for the reconstruction of iliac veins were excluded. In the short-term follow-up, data to assess vascular patency was collected from contrast-enhanced computed tomography (CT) scans with venous phase. If patients were asymptomatic, we did not perform a scheduled imaging. CT scan was performed in cases of postoperative complications or as a staging diagnostic during oncological follow-up. Imaging intervals were variable among the patient collective as a result.
Treatment was discussed in an interdisciplinary tumor conference preoperatively. The indication for resection was a malignant tumor in all cases and an extended oncological (R0) resection was performed.
Postoperative morbidity was evaluated based on the Clavien–Dindo classification of surgical complications [7]. The results were represented as median and interquartile range (IQR). For postoperative patency, we defined a complete occlusion if an imaging vascular contrast was absent and stenosis if half or less of the vascular lumen was contrasted associated with clinical signs (ascites, intestinal venous congestion, lower extremities edema). Thrombosis was diagnosed if a venous thrombus was found intraluminally in CT or ultrasound.
Procedure and important technical aspects
Intraoperatively, the patients were placed in a supine position with the right arm abducted. Laparotomy was performed using a midline or transverse abdominal incision and reversed L-shaped incision for hepatic resection. After excluding metastatic spreading in the abdominal cavity, dissection was started based on tumor location. In most cases, vascular resection was one of the last surgical steps before tumor removal in order to obtain the best possible bleeding control and avoid prolonged interruption of blood flow. The exact degree of vascular involvement of the tumor was assessed intraoperatively. A PPP was needed if the defect of the vessel wall was less than 30% of its circumference; otherwise, a tube graft was preferred. The IVC or PV was first dissected and prepared for clamping at both sides of tumor infiltration. PPPs were harvested from an area of the abdominal wall with intact peritoneum before clamping the vein (Figs. 1 and 2).
Surgical steps of PPP preparation. A Harvesting PPP from the hypochondrium. B and C Preparation is carried out in the layer between the rectus abdominis muscle and its posterior sheath. D The IVC is clamped proximally and distally to the tumor or longitudinally. Single traction sutures are placed at the patch and vessel corners to prevent twisting—arrows marked. E The patch is applied with the peritoneal surface on the luminal side of the vessel. It is important to ensure that the suture is tight but not strained in order to avoid stenosis of the vessel. F The clamp is removed, blood flow is restored and the suture is checked for sufficiency
PPPs were harvested from the right or left hypochondrium, the diaphragm, or from the posterior rectus muscle sheath with a peritoneum layer (Fig. 1). We prefer PPP from the right or left hypochondrium lateral to the rectus abdominis muscule for PV reconstruction (under consideration of the small presented patient number in the study), since the peritoneum is slightly thinner here compared to the ventral abdominal wall. In contrast, we prefer the thicker peritoneum with the posterior rectus layer of the ventral abdominal wall for vascular reconstruction of the VCI.
It is important not to harvest a PPP too small to bridge the vessel defect, in order to avoid a constricted vessel reconstruction that predisposes for thrombosis due to reduced local blood flow. PPP size was documented for eight patients after harvesting and before insertion of the patches. An important technical issue for the reconstruction is the size of the PPP, which is usually harvested larger than the defect of the vascular wall and a size reduction is performed before insertion to avoid PPP enlargement over time. In our institution, reconstruction was performed in a standard manner as a lateral patch plastic of the IVC or PV.
The surrounding fat tissue was left on the patch surface and the grafts were placed in saline solution (0.9% NaCl) until needed for the reconstruction (Fig. 1). The vein was side- or cross-clamped proximal and distal to the tumor. No systemic anticoagulation was administrated before or during clamping. After resecting the tumor, the vein defect was reconstructed by inserting the peritoneal patch with a running 4–0 (IVC) or 5–0 (PV) Prolene® suture. The patches were applied with the peritoneal surface on the luminal side of the vessel. As with direct venous anastomosis without patch/ graft interposition, it is important to loosely adapt the suture to avoid tension and create slightly slack knots to prevent stricture of the vein. Before final closure and restoring blood flow, retrograde and antegrade flushing was performed and local application of a heparin/saline solution (5000 IU heparin/500 ml saline) was used. After completing the suture, the clamps were removed to confirm sufficiency of the anastomosis (Fig. 2).
The surgical approach in reconstruction of PV (Fig. 3) and IVC (Figs. 4 and 5) did not differ. If possible, parenchymal hepatic transection was performed before vascular resection for liver procedures in order to avoid damaging the vascular reconstruction (Fig. 3). All patients received pharmacological prophylaxis with heparin (low-molecular-weight LMWH or unfractionated UFH) postoperatively. Treatment followed the German interdisciplinary, evidence- and consensus-based (S3) clinical practice guideline on venous thromboembolism prophylaxis based on patient-related risk factors and type of surgery [8].
Reconstruction of the IVC with PPP. Patient with hepatocellular carcinoma infiltrating the IVC and the diaphragm. Resection was performed after transarterial chemoembolisation (TACE) of segments VII and VIII and portal vein embolization of the right portal vein. Right hemihepatectomy with tangential resection of the IVC and partial diaphragmatic resection achieved R0 removal of the tumor, and vascular reconstruction was performed with a PPP. The patient had a complication-free course apart from a superficial SSI and was discharged 12 days postoperatively. A IVC reconstruction with PPP. The patch is inserted by using a continuous 4–0 Prolene® monofilament suture. B After removing the clamp and restoring the blood flow, the suture is checked for bleeding and stenosis
Results
Patients had a median age of 60 years (IQR: 53–71). Nine underwent hemihepatectomies, four had segmental liver resections, two had pancreatic resections, one underwent resection for paraaortic lymph node metastases, and one hepatic duct resection for bile duct carcinoma (Tables 1 and 2). In eight evaluable cases, PPP size varied between 150 and 3600 mm2. The exact patch size was not measured and reported in the other cases. Size was recorded after harvesting and before insertion of the PPP. No adverse events occurred in any of the patients during the operation. The median operating time was 413.7 min (IQR: 311.5–511) and median blood loss was 1205.8 ml (IQR: 650–1650).
We did not perform any revisions of the patches. One primary abdomen apertum due to intestinal edema with a planned “second look” relaparotomy was performed. Clinically relevant (CDC ≥ 3b) events with prolonged hospital stay and need of intervention occurred in four (24%) of the patients [7]. The main complications in these cases were POPF (n = 1), bilioma (n = 6), biliodigestive anastomosis leakage (n = 3), and postoperative hemorrhage (n = 4) due to impaired coagulation or vascular arrosion in pancreatitis.
The 30-day mortality rate was 6% (n = 1). One patient died from multiorgan failure as a consequence of a biliodigestive anastomosis leakage and sepsis. There were no immediate postoperative complications related to the peritoneal patch reconstruction.
Computed tomography images were available for evaluation of the vascular graft patency in 16 of the 17 patients at a mean follow-up of 17 months (1.5–48 months) after resection. We obtained information for the one patient who was lost for follow-up from his oncologist. He had no clinical signs of recurrence or venous obstruction.
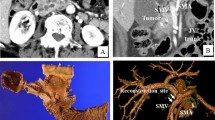
The overall patency rate in the cohort (n = 15: PV n = 2; IVC n = 13) was 88%. We had two cases of obstruction following a septic postoperative course. In one case after distal pancreatic resection with PPP reconstruction of the portal vein, complete vessel obstruction was found during a complicated postoperative course with a POPF C and sepsis due to necrotizing pancreatitis (Fig. 6). The second case of obstruction occurred after left hemihepatectomy with a common ostium biliodigestive anastomosis to the anterior and posterior pedicle and postoperative anastomotic bile leakage where percutaneous transhepatic cholangial drainage (PTCD) was performed. After initial stenosis 2 months postoperatively, portal hypertension with recurrent gastrointestinal bleeding occurred and CT scans showed high-grade stenosis (more than two-thirds of the lumen) of the portal vein. After 15 months, percutaneous transluminal angioplasty (PTA) and a stent were needed to restore portal blood flow (Figs. 7 and 8).
A and B CT scan of a patient 2 years after right hemihepatectomy with IVC resection and PPP reconstruction for colorectal metastasis without signs of obstruction, stenosis, or thrombosis; C CT scan showing good patency of VCI 4 years after reconstruction with PPP during right hemihepatectomy for colorectal metastasis
Complications after PPP reconstruction. A CT scan of the PV after PPP reconstruction during left hemihepatectomy for CCC with progressive vascular stenosis at 8 days and 2 and 15 months postoperatively; B percutaneous transluminal angioplasty (PTA) with stent (arro implementation of PV at 15 months postoperatively)
Although the presence of thrombosis could not be proven by the performed image-based diagnostic in those both cases, we suppose the septic situation to be a possible trigger for the impairment of postoperative patency. Nevertheless, these two patients received therapeutic anticoagulation for treatment.
Apart from these cases, there were no other clinical, paraclinical, or radiological signs of stenosis, obstruction, or thrombosis in the cohort.
Discussion
Surgical resection with complete tumor clearance improves patient survival and is superior to palliative therapy with regard to long-term outcome in cases with locally advanced tumors [1, 3, 9]. As a result of improved operative techniques, venous resection is a feasible, standard procedure in high-volume centers [10, 11, 12]. The reconstruction techniques follow the principles of vascular surgery. If primary anastomosis is not possible, a tube graft interposition or patch is applied for reconstruction.
Decision for the type of interponate
The decision for the graft is made depending on the vessel lumen, the type of vascular reconstruction (patch plastic or a tube substitute) and the septic contamination of the surgical procedure, the availability of the graft, and the individual expertise.
In HPB surgery, conventional alloplastic materials such as polyethylene terephthalate (PET) grafts (Dacron®) and (ringed) polytetrafluoroethylene (PTFE) grafts (Gore-Tex®, Gore, USA) are the ones most often used for vascular replacement. In case of high probability for local septic complications such as biliary leakage or pancreatic fistula, autologous material is preferred for the reconstruction. Cryopreserved homografts are mostly used in vascular surgery for reconstruction in the presence of infections for example in abdominal aortic surgery. Data from the literature show comparable rate of graft thrombosis and long-term graft patency for cryopreserved homografts as other biological grafts. However, the need of postoperative immunosuppression and ABO group compatibility is still controversial. We did not use allogenic material since in our collective the reconstruction could be performed, in the majority of cases, with autologous tissue. While autologous venous grafts are suitable and often used, either an additional incision is frequently needed for extraction and/or operation time is longer. In case of a tube graft interposition, we still prefer to harvest an autologous vessel like the saphenous or the jugular vein, which is more suitable for the reconstruction in terms of lumen size as the ovarian or spermatic vein.
For reconstruction with autologous parietal peritoneum, patches can be harvested from the abdominal wall through the same laparotomy without additional incisions. Compared to autologous venous grafts, this technique has several other advantages. The material is easily available, without a considerable increase of the operation time and additional surgical procedure as in case of harvesting another vessel like ovarian/spermatic, saphena, and left renal vein and there is no size limitation. Furthermore, the risk of infection is lower, PPP`s are less expensive and there is no need for postoperative anticoagulation as in the case of synthetic materials [5, 11, 13, 14]. Given all these advantages, vascular reconstruction with peritoneal patches has gained more acceptance in the last decade.
After initial encouraging reports in preclinical studies [15, 16], several case reports followed [16, 17, 18]. The results of a small patient cohort of six patients with PPP reconstruction of the IVC during liver resection were published by the Australian study group of Chin et al. in 1999 [19]. The outcome was encouraging with no mortality or obstruction of the IVC reported postoperatively. The largest series was published in 2015 by the French study group of Dokmak et al. [5]. They reported 52 cases and were the first to use peritoneal patches during pancreatic resection for reconstruction of the portal vein and superior mesenteric vein. Their results showing a patency rate of 97% after application of lateral PPPs are encouraging. The mean follow-up of 14 months for the postoperative CT scan evaluation was nearly comparable to our average time frame of 17 months. However, the majority of the literature still consists of case reports and to the best of our knowledge, there are only four retrospective studies available [6]. In particular, data for pancreatic resections and reconstruction of the portal vein are scarce, which may be one of the reasons for the lack of widespread application yet [20].
In our cohort, PPPs were used in both liver and pancreatic surgery for reconstruction of the IVC and PV. We started using PPPs for IVC reconstruction during paraaortic lymphadenectomy in 2017, with one patient undergoing the procedure. In 2020, we applied this technique in eight patients. Although not included in this paper, we have also used PPPs for reconstruction of the external iliac vein in sarcoma resections with good postoperative results.
Data for the use of PPP for tube graft interposition in literature is even more scarce. A systemic review showed in 2021 three studies with seven interposition of PPP tubes after PV resection. Obstruction was reported in four cases (71%) in the follow-up, and one patient presented with stenosis [6]. These results are somehow disappointing, but the number of patients is limited and therefore not representative. Some better data were obtained on the replacement of the vena cava with PPP tube. In 2013, a study group from Australia performed over 15 tubular interpositions with PPP with no signs of obstruction in the follow-up [21].
Very recent results, reported by the study group of Balzan et al., showed in a small cohort of 8 patients promising results after application of falciform ligament tubular graft for the reconstruction of PV/VMS during Whipple procedure with vascular resection [22]. Seven of the 8 patients showed non-altered vascular patency in CT 6 months postoperatively and a partial thrombosis, clinically inapparent, was diagnosed in one patient. These data are encouraging and the falciform ligament can be used as an alternative to the PPP. However, clinical outcome from prospective studies in larger cohorts of patients is still missing.
Decision for the side of PPP’s harvesting
PPPs can be harvested from the hypochondrium lateral to the rectus abdominis muscule where peritoneum is slightly thinner compared to the ventral abdominal wall. For the reconstruction of PV, a thinner peritoneum is needed due to its smaller lumen and thinner vessel wall. Some authors prefer even to use the falciforme ligament as a patch or a tubular graft [5, 6]. Due to the small number of patients reported in literature till now, results and long-term outcome for this graft remain unclear [6].
IVC and the hepatic veins (HV) have a thicker and stronger vascular wall and a PPP with a facial layer from the anterior abdominal wall is suitable for the reconstruction. The patency rate reported reaches, although in small patient collectives, up to 100% [5, 19]
Stenosis and obstruction
Clinical symptoms may indicate the presence of vascular stenosis or obstruction. The symptoms of PV obstruction are initially non-specific as fever, abdominal pain, diarrhea, or ileus and can increase to clinically relevant portal hypertension syndromes presented with ascites and haematemesis. The symptoms of IVC obstruction result from a reduced venous return to the heart. This causes hypotension, tachycardia, edema of the low extremities, elevated liver enzymes, and further organ failure. Diagnostic is accomplished by doppler ultrasound or CT angiography.
According to the French study group, patency rates after PPP reconstruction in liver surgery were better than those observed after pancreatic resection [5]. Our results are in line with these findings. In our small cohort, there were no cases of clinically relevant stenosis postoperatively in patients with reconstruction of the IVC. Two patients developed portal vein obstruction after distal pancreatectomy and hemihepatectomy, respectively (Figs. 5 and 6).
One possible explanation for maintaining postoperative patency after PPP usage could be the inherent fibrinolytic properties of the mesothelium. This aspect was examined in preclinical studies and needs to be studied further [23]. The morbidity rate in our cohort of 24% for patients with CDC ≥ 3b is high but within the reported range for complex multivisceral resections in malignant tumors. Postoperative morbidity was due to sepsis as a result of biliary leakage, pancreatic fistula, or insufficient anastomosis and not related to the patches used.
Anticoagulation after vascular reconstruction
Although there are no guidelines for the postoperative anticoagulation after venous reconstruction, we defined a standard approach for our institution according to the general guidelines for perioperative venous thromboembolism prophylaxis in general and visceral surgery and the available literature based mainly on case reports [8, 11]. After IVC reconstruction with autologous material, patients receive pharmacological prophylaxis with heparin (low-molecular-weight LMWH or unfractionated UFH) for 4 weeks postoperative if no complication occurs.
After PV reconstruction with autologous graft, prophylactic LMWH doses are applied for a normal diameter ≥ 1.0 cm after reconstruction and half-therapeutic doses of LMWH are applied if the venous diameter was < 1.00 cm.
Our study has some limitations because of its retrospective nature, the heterogeneity of the surgical procedures and the lack of structured follow-up regarding patency rates of vessel reconstructions with PPP. However, it was designed to describe the indications and technical aspects of this still rare procedure. Although data were collected from a small patient cohort, it still represents one of the largest patient cohorts investigated to date. By describing the surgical technique and highlighting important operative steps, we aim to encourage to apply this safe and cost-effective procedure in high-volume centers and further push the borders in surgery of complex multivisceral resections in malignant tumors.
Conclusions
Our data show promising results for safety and patency rates after PPP for venous reconstruction in liver and pancreatic surgery. In patients undergoing reconstruction of the PV, more studies are needed to evaluate the safety and long-term results of this procedure in this setting.
Moreover, prospective randomized studies should examine the advantage of PPP implantation for vascular reconstruction in both liver and pancreatic surgery.
Data availability
Data is available on request from the corresponding author.
References
Nagino M (2019) Fifty-year history of biliary surgery. Ann Gastroenterol Surg 3:598–605
Lee SG, Song GW, Hwang S et al (2010) Surgical treatment of hilar cholangiocarcinoma in the new era: the Asan experience. J Hepatobiliary Pancreat Sci 17:476–489
Igami T, Nishio H, Ebata T, Yokoyama Y, Sugawara G, Nimura Y, Nagino M (2010) Surgical treatment of hilar cholangiocarcinoma in the “new era”: the Nagoya University experience. J Hepatobiliary Pancreat Sci 17:449–454
Berumen J, Hemming A (2016) Vascular reconstruction in hepatic malignancy. Surg Clin North Am. https://doi.org/10.1016/j.suc.2015.11.006
Dokmak S, Aussilhou B, Sauvanet A, Nagarajan G, Farges O, Belghiti J (2015) Parietal peritoneum as an autologous substitute for venous reconstruction in hepatopancreatobiliary surgery. Ann Surg. https://doi.org/10.1097/SLA.0000000000000959
Labori KJ, Kleive D, Khan A, Farnes I, Fosby B, Line PD (2021) Graft type for superior mesenteric and portal vein reconstruction in pancreatic surgery - a systematic review. HPB (Oxford) 23:483–494
Dindo D, Demartines N, Clavien PA, Clavien PA (2004) Classification of surgical complications a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. https://doi.org/10.1097/01.sla.0000133083.54934.ae
Encke A, Haas S, Kopp I (2016) Clinical practice guideline: the prophylaxis of venous thromboembolism. Deutsches Arzteblatt Int. https://doi.org/10.3238/arztebl.2016.0532
Nagino M (2012) Perihilar cholangiocarcinoma: a surgeon’s viewpoint on current topics. J Gastroenterol. https://doi.org/10.1007/s00535-012-0628-6
Nagino M, Nimura Y, Nishio H, Ebata T, Igami T, Matsushita M, Nishikimi N, Kamei Y (2010) Hepatectomy with simultaneous resection of the portal vein and hepatic artery for advanced perihilar cholangiocarcinoma: an audit of 50 consecutive cases. Ann Surg. https://doi.org/10.1097/SLA.0b013e3181e463a7
Balzan SMP, Gava VG, Magalhaes MA, Rieger A, Roman LI, dos Santos C, Marins MP, Rabaioli B, Raupp IT, Kunzler VB (2021) Complete and partial replacement of the inferior vena cava with autologous peritoneum in cancer surgery. J Surg Oncol. https://doi.org/10.1002/jso.26558
Yekebas EF, Bogoevski D, Cataldegirmen G et al (2008) En bloc vascular resection for locally advanced pancreatic malignancies infiltrating major blood vessels: perioperative outcome and long-term survival in 136 patients. Ann Surg. https://doi.org/10.1097/SLA.0b013e31815aab22
Ribbe EB, Alm P, Hallberg E, Norgren LEH (2005) Evaluation of peritoneal tube grafts in the inferior vena cava of the pig. Br J Surg 75:357–360
Theuer CJ, Bergamini TM, Theuer HH, Burns CD, Proctor ML, Carrison RN (1996) Vena cava replacement with a peritoneum-lined vascular graft. Undefined 42:266–270
Yoshioka M, Onda M, Tajiri T, Akimaru K, Mineta S, Hirakata A, Takubo K (2001) Reconstruction of the portal vein using a peritoneal patch-graft. The American Journal of Surgery 181:247–250
Dokmak S, Aussilhou B, Marchese T, Kardoun N, Cauchy F, Schneck AS, Soubrane O (2018) Right trisectionectomy and caval reconstruction with peritoneal patch under short total vascular exclusion for hepatocellular carcinoma with tumoral thrombus in suprahepatic vena cava. Ann Surg Oncol 25:1152
Felli E, Lapergola A, Pessaux P (2018) Autologous peritoneal patch for partial portal vein resection during left hemi hepatectomy (with video). J Visc Surg 155:509–510
Lapergola A, Felli E, Rebiere T, Mutter D, Pessaux P (2020) Autologous peritoneal graft for venous vascular reconstruction after tumor resection in abdominal surgery: a systematic review. Updat Surg. https://doi.org/10.1007/s13304-020-00730-9
Chin PT, Gallagher PJ, Stephen MS (1999) Inferior vena caval resection with autogenous peritoneo-fascial patch graft caval repair: a new technique. Aust N Z J Surg. https://doi.org/10.1046/j.1440-1622.1999.01579.x
Langella S, Menonna F, Casella M, Russolillo N, Tesoriere RL, Alessandro F (2020) Vascular resection during hepatectomy for liver malignancies. Results from a Tertiary Center using Autologous Peritoneal Patch for Venous Reconstruction. World J Surg 44:3100–3107
Pulitanó C, Crawford M, Ho P, Gallagher J, Joseph D, Stephen M, Sandroussi C (2013) The use of biological grafts for reconstruction of the inferior vena cava is a safe and valid alternative: results in 32 patients in a single institution. HPB 15:628–632
Balzan SMP, Gava VG, Rieger A, Magalhães MA, Schwengber A, Ferreira F (2022) Falciform ligament tubular graft for mesenteric-portal vein reconstruction during pancreaticoduodenectomy. J Surg Oncol 125:658–663
Baumann G (1972) Extreme Venen-Bypass-Verfahren bei der Behandlung chronischer femoro-poplitealer Arterien-Verschlüsse im Stadium III und IV. Chir Forum Exp Klin Forsch. https://doi.org/10.1007/978-3-642-48834-4_101
Acknowledgements
The authors would like to thank Loreen Natusch for her contribution to the intraoperative photo documentation.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
Study conception and design: Olga Radulova-Mauersberger, Thilo Welsch. Acquisition of data: Olga Radulova-Mauersberger, Johanna Kirchberg, Marius Distler, Thilo Welsch, Carina Riediger, Jürgen Weitz. Analysis and interpretation of data: Olga Radulova-Mauersberger, Johanna Kirchberg, Thilo Welsch. Writing—original draft preparation: Olga Radulova-Mauersberger. Writing—review and editing: Thilo Welsch, Johanna Kirchberg. Critical revision of the manuscript: Jürgen Weitz. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Consent to participate
Appropriate consent from the patients was available for use of surgical information. Identity of the patient has not been revealed. This article does not contain any studies with animals performed by any of the authors.
Consent for publication
All authors have provided consent for the article to be published in Langenbeck’s Archives of Surgery.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Radulova-Mauersberger, O., Distler, M., Riediger, C. et al. How we do it—the use of peritoneal patches for reconstruction of vena cava inferior and portal vein in hepatopancreatobiliary surgery. Langenbecks Arch Surg 407, 3819–3831 (2022). https://doi.org/10.1007/s00423-022-02662-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00423-022-02662-x