Abstract
Purpose
Acute hypoxia alters the threshold for sensation of cutaneous thermal stimuli. We hypothesised that hypoxia-induced alterations in cutaneous temperature sensation may lead to modulation of the perception of temperature, ultimately influencing behavioural thermoregulation and that the magnitude of this effect could be influenced by daily physical training.
Methods
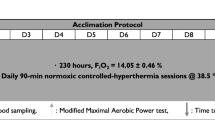
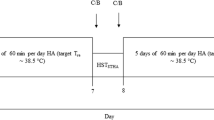
Fourteen men were confined 10 days to a normobaric hypoxic environment (PIO2 = 88.2 ± 0.6 mmHg, corresponding to 4175 m elevation). Subjects were randomly assigned to a non-exercising (Live-high, LH, N = 6), or exercising group (Live-high Train-high, LH-TH, N = 8) comprised of 1-h bouts of cycle ergometry, twice daily, at a work-rate equivalent to 50% hypoxic peak power output. A subset of subjects (N = 5) also completed a control trial under normoxic conditions. The thermal comfort zone (TCZ) was determined in normoxia, and during hypoxic confinement days 2 (HC2) and 10 (HC10) in both groups using a water-perfused suit in which water temperature was regulated by the subjects within a range, they deemed thermally comfortable. Mean skin temperature and proximal–distal temperature gradients (two sites: forearm-fingertip, calf-toe) were recorded each minute throughout the 60-min protocol.
Results
The average width of the TCZ did not differ between the control group (9.0 ± 6.9 °C), and the LH and LH-TH groups on days HC2 (7.2 ± 4.2 °C) and HC10 (10.2 ± 7.5 °C) of the hypoxic exposure (p = 0.256). \(\bar{T}_{\text{SK}}\) was marginally higher on HC2 (35.9 ± 1.0 °C) compared to control (34.9 ± 0.8 °C, p = 0.040), but not on HC10 (35.6 ± 1.0 °C), reflecting the responses of hand perfusion.
Conclusion
There was a little systematic effect of hypoxia or exercise training on TCZ magnitude or boundary temperatures.



Similar content being viewed by others
Abbreviations
- \(\bar{T}_{\text{SK}}\) :
-
Mean skin temperature
- \({\dot{\text{V}}\text{O}}_{{ 2\,{\text{peak}}}}\) :
-
Peak rate of oxygen consumption
- CON:
-
Control group
- FIO2 :
-
Fraction of inspired oxygen
- HC:
-
Hypoxia confinement
- HR:
-
Heart rate
- LH:
-
Live-high group
- LH-TH:
-
Live-high train-high group
- PIO2 :
-
Partial pressure of inspired oxygen
- R:
-
Recovery day
- SpO2 :
-
Capillary oxyhaemoglobin saturation
- TCZ:
-
Thermal comfort zone
- TTY :
-
Tympanic temperature
- WPS:
-
Water-perfused suit
References
Araki T, Matsushita K, Umeno K, Tsujino A, Toda Y (1981) Effect of physical training on exercise-induced sweating in women. J Appl Physiol Respir Environ Exerc Physiol 51(6):1526–1532
Bonne TC, Lundby C, Jørgensen S, Johansen L, Morgan M, Bech SR, Sander M, Papoti M, Nordsborg NB (2014) “Live High–Train High” increases hemoglobin mass in Olympic swimmers. Eur J Appl Physiol 114(7):1439–1449
Burke W, Mekjavic IB (1991) Estimation of regional cutaneous cold sensitivity by analysis of the grasping response. J Appl Physiol 71:1933–1940
Castellani JW, Young AJ (2010) Health and performance challenges during sports training and competition in cold weather. Br J Sports Med 46(11):788–791
Castellani JW, Young AJ, Ducharme MB, Giesbrecht GG, Glickman E, Sallis RE (2006) American College of Sports Medicine position stand: prevention of cold injuries during exercise. Med Sci Sports Exerc 38(11):2012–2029
Ciuha U, Mekjavic IB (2016) Regional thermal comfort zone in males and females. Physiol Behav 161:123–129
Ciuha U, Eiken O, Mekjavic IB (2015) Effects of normobaric hypoxic bedrest on the thermal comfort zone. J Therm Biol 49–50:39–46
Czuba M, Maszczyk A, Gerasimuk D, Roczniok R, Fidos-Czuba O, Zając A, Gołaś A, Mostowik A, Langfort J (2014) The effects of hypobaric hypoxia on erythropoiesis, maximal oxygen uptake and energy cost of exercise under normoxia in elite biathletes. J Sports Sci Med 13(4):912–920
Debevec T, Pialoux V, Mekjavic IB, Eiken O, Mury P, Millet GP (2014a) Moderate exercise blunts oxidative stress induced by normobaric hypoxic confinement. Med Sci Sport Exerc 41:33–41
Debevec T, Simpson EJ, Macdonald IA, Eiken O, Mekjavić IB (2014b) Exercise training during normobaric hypoxic confinement does not alter hormonal appetite regulation. PLoS One 9:e98874
DiPasquale DM, Kolkhorst FW, Buono MJ (2015) Acute normobaric hypoxia reduces body temperature in humans. High Alt Med 16:61–66
Fritzsche RG, Coyle EF (2000) Cutaneous blood flow during exercise is higher in endurance-trained humans. J Appl Physiol 88(2):738–744
Golja P (2004) The effect of normobaric hypoxia on temperature regulation in humans. Doctoral dissertation, University of Portsmouth, United Kingdom
Golja P, Mekjavic IB (2003) Effect of hypoxia on preferred hand temperature. Aviat Space Environ Med 74(5):522–526
Golja P, Kacin A, Tipton M, Eiken O, Mekjavic IB (2004) Hypoxia increases the cutaneous threshold for sensation of cold. Eur J Appl Physiol 92:62–68
Golja P, Kacin A, Tipton M, Mekjavic IB (2005) Moderate hypoxia does not affect the zone of thermal comfort in humans. Eur J Appl Physiol 93:708–713
Gordon C (2001) The therapeutic potential of regulated hypothermia. Emerg Med 18:81–89
Gordon C, Fogelson L (1991) Comparative effects of hypxia on behavioural thermoregulation in rats, hamsters and mice. Am J Physiol 260:R120–R125
Hicks J, Wood S (1985) Temerature regulation in lizards: effects of hypoxia. Am J Physiol 248:R595–R600
House JR, Tipton MJ (2002) Using skin temperature gradients or skin heat flux measurements to determine thresholds of vasoconstriction and vasodilatation. Eur J Appl Physiol 88(1–2):141–145
Kenshalo D (1976) Sensory functions of the skin in primates: with special reference to man. In: Zotterman Y (ed) Proceedings of the international symposium. Pergamon Press, Stockholm, pp 305–330
Keramidas ME, Kölegård R, Mekjavic IB, Eiken O (2014) Acute effects of normobaric hypoxia on hand-temperature responses during and after local cold stress. High Alt Med Biol 15(2):183–191
Keramidas ME, Kölegård R, Mekjavic IB, Eiken O (2015) Hand temperature responses to local cooling after a 10-day confinement to normobaric hypoxia with and without exercise. Scand J Med Sci Sports 25(5):650–660
Malanda UL, Reulen JP, Saris WH, van Marken Lichten-belt WD (2008) Hypoxia induces no change in cutaneous thresholds for warmth and cold sensation. Eur J Appl Physiol 104:375–381
McDonnell AC, Eiken O, Mekjavic PJ, Mekjavic IB (2014) Circadian rhythm of peripheral perfusion during 10-day hypoxic confinement and bed rest. Eur J Appl Physiol 114(10):2093–2104
Mekjavic IB, Eiken O (2006) Contribution of thermal and nonthermal factors to the regulation of body temperature in humans. J Appl Physiol 100(6):2065–2072
Mercer J (2001) Glossary of terms for thermal physiology. Jpn J Physiol 51:245–280
Miyagawa K, Kamijo Y, Ikegawa S, Goto M, Nose H (2011) Reduced hyperthermia-induced cutaneous vasodilation and enhanced exercise-induced plasma water loss at simulated high altitude (3200 m) in humans. J Appl Physiol 110:157–165
Nadel ER, Pandolf KB, Roberts MF, Stolwijk JA (1974) Mechanisms of thermal acclimation to exercise and heat. J Appl Physiol 37(4):515–520
Ramanathan NL (1964) A new weighting system for mean surface temperature of the human body. J Appl Physiol 19:531–533
Richardson A, Watt P, Maxwell N (2009) Hydration and the physiological responses to acute normobaric hypoxia. Wilderness Environ Med 20:212–220
Roberts MF, Wenger CB, Stolwijk JA, Nadel ER (1977) Skin blood flow and sweating changes following exercise training and heat acclimation. J Appl Physiol Respir Environ Exerc Physiol 43(1):133–137
Robinson KA, Haymes EM (1990) Metabolic effects of exposure to hypoxia plus cold at rest and during exercise in humans. J Appl Physiol 68:720–725
Rubenstein EH, Sessler DI (1990) Skin-surface temperature gradients correlate with fingertip blood flow in humans. Anesthesiology 73:541–545
Schlader ZJ, Sarker S, Mündel T, Coleman GL, Chapman CL, Sackett JR, Johnson BD (2016) Hemodynamic responses upon the initiation of thermoregulatory behavior in young healthy adults. Temperature 3(2):271–285
Simmons GH, Minson CT, Cracowski JL, Halliwill JR (2007) Systemic hypoxia causes cutaneous vasodilation in healthy humans. J Appl Physiol 103(2):608–615
Simmons GH, Barrett-O’Keefe Z, Minson CT, Halliwill JR (2011) Cutaneous vascular and core temperature responses to sustained cold exposure in hypoxia. Exp Physiol 96:1062–1071
Yogev D, Mekjavic IB (2007) A new method for evaluation of behavioural thermoregulation in humans. In: Mekjavic IB, Kounalakis S, Taylor N (eds) Proceedings of the 12th international conference on environmental ergonomics (ICEE XII). Biomed, Ljubljana, pp 359–360
Yogev D, Eiken O, Pisot R, Biolo G, di Prampero P, Narici M, Mekjavic IB (2010) Effect of 21 days of horizontal bed rest on behavioural thermoregulation. Eur J Appl Physiol 108:281–288
Acknowledgements
The researchers would like to thank the subjects for their participation and enthusiasm in the study. We are grateful to Mr. Adi Kosenina for and Mr. Bogomir Vrhovec for their technical assistance. This work was supported by the Slovene Research Agency (Grants L3-4328 and L3-3654) and a European Space Agency (ESA) Programme for European Cooperating States (ESTEC/Contract No. 40001043721/11/NL/KML) to Igor B. Mekjavic. Urša Ciuha was a recipient of a SPIRIT Slovenia Scholarship (Public Agency of the Republic of Slovenia for the Promotion of the Entrepreneurship, Innovation, Development, Investment and Tourism), with operation partly financed by the European Union, European Social Fund.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest, financial or otherwise, associated with this work.
Additional information
Communicated by Narihiko Kondo.
Rights and permissions
About this article
Cite this article
Morrison, S.A., Ciuha, U., Zavec-Pavlinić, D. et al. The effect of a Live-high Train-high exercise regimen on behavioural temperature regulation. Eur J Appl Physiol 117, 255–265 (2017). https://doi.org/10.1007/s00421-016-3515-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-016-3515-7