Abstract
Purpose
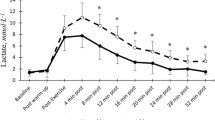
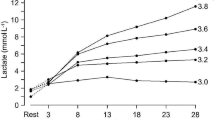
The aim of this study was to investigate lactate recovery kinetics after high-intensity exercises.
Methods
Six competitive middle-distance runners performed 500-, 1000-, and 1500-m trials at 90 % of their current maximal speed over 1500 m. Each event was followed by a passive recovery to obtain blood lactate recovery curves (BLRC). BLRC were fitted by the bi-exponential time function: La(t) = La(0) + A 1(1–e −γ1t) + A 2(1–e −γ2t), where La(0) is the blood lactate concentration at exercise completion, and γ 1 and γ 2 enlighten the lactate exchange ability between the previously active muscles and the blood and the overall lactate removal ability, respectively. Applications of the model provided parameters related to lactate release, removal and accumulation rates at exercise completion, and net amount of lactate released during recovery.
Results
The increase of running distance was accompanied by (1) a continuous decrease in γ 1 (p < 0.05), (2) a primary decrease (p < 0.05) and then a stabilization of γ 2, and (3) a constant increase in blood concentrations (p < 0.05) and whole body accumulation of lactate (p < 0.05). Estimated net lactate release, removal and accumulation rates at exercise completion, as well as the net amount of lactate released during recovery were not significantly altered by distance.
Conclusion
Alterations of lactate exchange and removal abilities have presumably been compensated by an increase in muscle-to-blood lactate gradient and blood lactate concentrations, respectively, so that estimated lactate release, removal and accumulation rates remained almost stable as distance increased.
Similar content being viewed by others
Abbreviations
- A 1 and A 2 :
-
Concentration parameters (amplitudes of the exponential functions)
- BLRC:
-
Blood lactate recovery curves
- La(0):
-
Blood lactate concentration at exercise completion
- La(t):
-
Blood lactate concentration at time t
- Lapeak :
-
Maximal blood lactate concentration during recovery
- Lawarm-up :
-
Blood lactate concentration at the end of the warm-up
- LAR:
-
Lactate accumulation rate
- LRR:
-
Lactate removal rate
- MCR:
-
Metabolic clearance rate of lactate
- MCRR :
-
Metabolic clearance rate of lactate during recovery
- NALR:
-
Net amount of lactate released
- NLRR:
-
Net lactate release rate
- QLaA:
-
Amount of lactate accumulated in the body at exercise completion
- QLaR:
-
Amount of lactate removed from the end of exercise to Lapeak
- Rd R :
-
Lactate disappearance rate
- tLapeak :
-
Time to reach the maximal lactate concentration during recovery
- V M :
-
Lactate distribution volume of muscles previously involved in exercise
- \(\dot{V}\)O2max :
-
Maximal oxygen uptake
- V S :
-
Volume of compartment S (V TLS − V M)
- V TLS :
-
Volume of the total lactate distribution space
- γ 1 :
-
Velocity constant enlighten lactate exchange ability
- γ 2 :
-
Velocity constant enlighten lactate removal ability
References
Allen D, Westerblad H (2004) Physiology. Lactic acid—the latest performance-enhancing drug. Science 305:1112–1113
Bangsbo J, Madsen K, Kiens B, Richter EA (1996) Effect of muscle acidity on muscle metabolism and fatigue during intense exercise in man. J Physiol 495(Pt 2):587–596
Bergman BC, Wolfel EE, Butterfield GE, Lopaschuk GD, Casazza GA, Horning MA, Brooks GA (1999) Active muscle and whole body lactate kinetics after endurance training in men. J Appl Physiol 87:1684–1696
Bishop D, Edge J, Thomas C, Mercier J (2007) High-intensity exercise acutely decreases the membrane content of MCT1 and MCT4 and buffer capacity in human skeletal muscle. J Appl Physiol 102:616–621
Bret C, Messonnier L, Nouck Nouck JM, Freund H, Dufour AB, Lacour JR (2003) Differences in lactate exchange and removal abilities in athletes specialised in different track running events (100 to 1500 m). Int J Sports Med 24:108–113
Brooks GA (1986) The lactate shuttle during exercise and recovery. Med Sci Sports Exerc 18:360–368
Brooks GA (2000) Intra- and extra-cellular lactate shuttles. Med Sci Sports Exerc 32:790–799
Brooks GA (2002) Lactate shuttle—between but not within cells? J Physiol 541:333–334
Brooks GA (2009) Cell–cell and intracellular lactate shuttles. J Physiol 587:5591–5600
Brooks GA, Butterfield GE, Wolfe RR, Groves BM, Mazzeo RS, Sutton JR, Wolfel EE, Reeves JT (1991) Decreased reliance on lactate during exercise after acclimatization to 4300 m. J Appl Physiol 71:333–341
Coggins M, Lindner J, Rattigan S, Jahn L, Fasy E, Kaul S, Barrett E (2001) Physiologic hyperinsulinemia enhances human skeletal muscle perfusion by capillary recruitment. Diabetes 50:2682–2690
Costa Leite T, Da Silva D, Guimaraes Coelho R, Zancan P, Sola-Penna M (2007) Lactate favours the dissociation of skeletal muscle 6-phosphofructo-1-kinase tetramers down-regulating the enzyme and muscle glycolysis. Biochem J 408:123–130
Donovan CM, Brooks GA (1983) Endurance training affects lactate clearance, not lactate production. Am J Physiol 244:E83–E92
Dubouchaud H, Eydoux N, Granier P, Prefaut C, Mercier J (1999) Lactate transport activity in rat skeletal muscle sarcolemmal vesicles after acute exhaustive exercise. J Appl Physiol 87:955–961
Dubouchaud H, Butterfield GE, Wolfel EE, Bergman BC, Brooks GA (2000) Endurance training, expression, and physiology of LDH, MCT1, and MCT4 in human skeletal muscle. Am J Physiol Endocrinol Metab 278:E571–E579
Emhoff CA, Messonnier LA, Horning MA, Fattor JA, Carlson TJ, Brooks GA (2013) Direct and indirect lactate oxidation in trained and untrained men. J Appl Physiol 1985 115:829–838
Eydoux N, Py G, Lambert K, Dubouchaud H, Prefaut C, Mercier J (2000) Training does not protect against exhaustive exercise-induced lactate transport capacity alterations. Am J Physiol Endocrinol Metab 278:E1045–E1052
Favero TG, Zable AC, Colter D, Abramson JJ (1997) Lactate inhibits Ca(2+)-activated Ca(2+)-channel activity from skeletal muscle sarcoplasmic reticulum. J Appl Physiol 82:447–452
Freund H, Zouloumian P (1981a) Lactate after exercise in man: I. Evolution kinetics in arterial blood. Eur J Appl Physiol Occup Physiol 46:121–133
Freund H, Zouloumian P (1981b) Lactate after exercise in man: IV. Physiological observations and model predictions. Eur J Appl Physiol Occup Physiol 46:161–176
Freund H, Oyono-Enguéllé S, Heitz A, Marbach J, Ott C, Zouloumian P, Lampert E (1986) Work rate-dependent lactate kinetics after exercise in humans. J Appl Physiol 61:932–939
Freund H, Oyono-Enguéllé S, Heitz A, Marbach J, Ott C, Gartner M (1989) Effect of exercise duration on lactate kinetics after short muscular exercise. Eur J Appl Physiol Occup Physiol 58:534–542
Hollidge-Horvat MG, Parolin ML, Wong D, Jones NL, Heigenhauser GJ (1999) Effect of induced metabolic acidosis on human skeletal muscle metabolism during exercise. Am J Physiol 277:E647–E658
Jubrias SA, Crowther GJ, Shankland EG, Gronka RK, Conley KE (2003) Acidosis inhibits oxidative phosphorylation in contracting human skeletal muscle in vivo. J Physiol 553:589–599
Juel C (1997) Lactate-proton cotransport in skeletal muscle. Physiol Rev 77:321–358
Juel C, Bangsbo J, Graham T, Saltin B (1990) Lactate and potassium fluxes from human skeletal muscle during and after intense, dynamic, knee extensor exercise. Acta Physiol Scand 140:147–159
Korzeniewski B, Zoladz JA (2015) Possible mechanisms underlying slow component of VO2 on-kinetics in skeletal muscle. J Appl Physiol 1985 118:1240–1249
Maciejewski H, Bourdin M, Lacour JR, Denis C, Moyen B, Messonnier L (2013) Lactate accumulation in response to supramaximal exercise in rowers. Scand J Med Sci Sports 23:585–592
Marcinek DJ, Kushmerick MJ, Conley KE (2010) Lactic acidosis in vivo: testing the link between lactate generation and H+ accumulation in ischemic mouse muscle. J Appl Physiol 108:1479–1486
Messonnier L, Freund H, Bourdin M, Belli A, Lacour JR (1997) Lactate exchange and removal abilities in rowing performance. Med Sci Sports Exerc 29:396–401
Messonnier L, Freund H, Feasson L, Prieur F, Castells J, Denis C, Linossier MT, Geyssant A, Lacour JR (2001) Blood lactate exchange and removal abilities after relative high-intensity exercise: effects of training in normoxia and hypoxia. Eur J Appl Physiol 84:403–412
Messonnier L, Freund H, Denis C, Dormois D, Dufour AB, Lacour JR (2002) Time to exhaustion at VO(2)max is related to the lactate exchange and removal abilities. Int J Sports Med 23:433–438
Messonnier L, Kristensen M, Juel C, Denis C (2007) Importance of pH regulation and lactate/H+ transport capacity for work production during supramaximal exercise in humans. J Appl Physiol 102:1936–1944
Messonnier LA, Emhoff CA, Fattor JA, Horning MA, Carlson TJ, Brooks GA (2013) Lactate kinetics at the lactate threshold in trained and untrained men. J Appl Physiol 114:1593–1602
Miller BF, Fattor JA, Jacobs KA, Horning MA, Navazio F, Lindinger MI, Brooks GA (2002) Lactate and glucose interactions during rest and exercise in men: effect of exogenous lactate infusion. J Physiol 544:963–975
Mortensen SP, Damsgaard R, Dawson EA, Secher NH, Gonzalez-Alonso J (2008) Restrictions in systemic and locomotor skeletal muscle perfusion, oxygen supply and VO2 during high-intensity whole-body exercise in humans. J Physiol 586:2621–2635
Nelson CR, Fitts RH (2014) Effects of low cell pH and elevated inorganic phosphate on the pCa-force relationship in single muscle fibers at near-physiological temperatures. Am J Physiol Cell Physiol 306:C670–C678
Nielsen OB, de Paoli F, Overgaard K (2001) Protective effects of lactic acid on force production in rat skeletal muscle. J Physiol 536:161–166
Osnes JB, Hermansen L (1972) Acid–base balance after maximal exercise of short duration. J Appl Physiol 32:59–63
Pedersen TH, Nielsen OB, Lamb GD, Stephenson DG (2004) Intracellular acidosis enhances the excitability of working muscle. Science 305:1144–1147
Pilegaard H, Bangsbo J, Henningsen P, Juel C, Richter EA (1995) Effect of blood flow on muscle lactate release studied in perfused rat hindlimb. Am J Physiol 269:E1044–E1051
Roth DA, Brooks GA (1990) Lactate transport is mediated by a membrane-bound carrier in rat skeletal muscle sarcolemmal vesicles. Arch Biochem Biophys 279:377–385
Stanley WC, Gertz EW, Wisneski JA, Neese RA, Morris DL, Brooks GA (1986) Lactate extraction during net lactate release in legs of humans during exercise. J Appl Physiol 1985 60:1116–1120
Thomas C, Sirvent P, Perrey S, Raynaud E, Mercier J (2004) Relationships between maximal muscle oxidative capacity and blood lactate removal after supramaximal exercise and fatigue indexes in humans. J Appl Physiol 97:2132–2138
Thomas C, Perrey S, Lambert K, Hugon G, Mornet D, Mercier J (2005) Monocarboxylate transporters, blood lactate removal after supramaximal exercise, and fatigue indexes in humans. J Appl Physiol 98:804–809
Acknowledgments
The authors would like to thank Josiane Castells for her technical assistance, all the athletes for their voluntary participation in this study, and the coaches, the clubs, and Pierre Bavazzano for their support. This project was supported by the Université Savoie Mont Blanc.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflicts of interest, financial or otherwise, are declared by the authors.
Additional information
Communicated by Jean-René Lacour.
Appendix
Appendix
An application of the bi-compartmental model of lactate distribution space allows the prediction of the net lactate release rate (NLRR, mmol min−1) during recovery using the following equation:
where V S is the volume of compartment S [i.e., 250 mL kg−1 body mass; V S = V TLS (volume of the total lactate distribution space) − V M (lactate distribution volume of muscles previously involved in exercise)], µ is the net muscular release rate of lactate at t → ∞ and was set at 0.12 mmol min−1 (Bret et al. 2003; Freund and Zouloumian 1981b; Maciejewski et al. 2013), and d 2 is the efficiency of lactate utilization in compartment S. The application of the model gives realistic prediction when d 2 is close to γ 2. Therefore, to approximate NLRR, we set, as previously (Bret et al. 2003; Freund and Zouloumian 1981b; Maciejewski et al. 2013), d 2 = γ 2 − 0.005. The integral of Eq. (2) gives an estimation of the net amount of lactate released during recovery (NALR, mmol) from the previously active muscles to the blood (Bret et al. 2003). The maximal value (NALRmax) will be considered (Maciejewski et al. 2013).
Recently, Maciejewski et al. (2013) have developed a method to estimate the amount of lactate accumulated in the body at exercise completion (QLaA, mmol):
where QLaA at Lapeak is the quantity of lactate accumulated at Lapeak which is calculated as the following:
where Lapeak represents the maximal blood lactate concentration during recovery, and V TLS represents the volume of the total lactate distribution space (i.e., 500 mL kg−1).
QLaR represents the amount of lactate removed from the end of exercise to Lapeak, which is calculated as
where tLapeak is the time to reach the maximal lactate concentration during recovery. For more information about this method, we refer the reader to Maciejewski et al. (2013).
Lactate removal rate at the end of each exercise [LRR(0), mmol min−1] was estimated from the following equation:
A calculation of the lactate accumulation rate (LAR, mmol min−1) during each fraction of 500 m was derived from QLaA values according to the following equation:
where ΔQLaA is the difference in QLaA between two distances and t is the time to complete 500 m. For the first 500 m, ΔQLaA = QLaA − (Lawarm-up × V TLS), where Lawarm-up is the blood lactate concentration at the end of the warm-up.
As done in the past (Freund et al. 1986; Messonnier et al. 2001), a metabolic clearance rate of lactate during recovery (MCRR, mL kg−1 min−1) can be derived from γ 2 values according to the following equation:
A calculation of the lactate disappearance rate at exercise completion (Rd R(0), mg kg−1 min−1) can also be derived from Eq. (8) according to the following equation:
Rights and permissions
About this article
Cite this article
Chatel, B., Bret, C., Edouard, P. et al. Lactate recovery kinetics in response to high-intensity exercises. Eur J Appl Physiol 116, 1455–1465 (2016). https://doi.org/10.1007/s00421-016-3420-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-016-3420-0