Abstract
Purpose
We have previously shown that Afghans residing in Denmark for at least 12 years exhibit a lower 24-h ambulatory blood pressure compared to Danes. The purpose of this study was to test the hypothesis that the lower blood pressure reflects attenuated compensatory baroreflex responses in the Afghans.
Methods
On a controlled diet (2,822 cal/day, 55–75 mmol + 2 mmol Na+/kg/day), 12 young males of Afghan (Afghans) and 12 young males of Danish (Danes) origin were exposed to a two-step lower body negative pressure (LBNP) protocol of −20 and −50 mmHg, respectively, each of 10-min duration.
Results
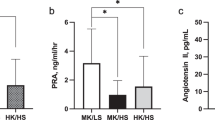
Afghans had lower 24-h systolic blood pressure compared to Danes (115 ± 2 vs. 123 ± 1 mmHg, p < 0.05). Cardiac output and stroke volume were significantly lower in Afghans compared to Danes prior to and during each level of LBNP. However, it decreased to the same extent in both groups during LBNP. During LBNP of −20 mmHg, plasma noradrenaline concentration and plasma renin activity (PRA) increased significantly only in the Afghans. At LBNP of −50 mmHg plasma noradrenaline concentration and PRA both increased significantly and similarly in the two groups.
Conclusion
The lower 24-h ambulatory blood pressure in the Afghans is probably caused by a lower stroke volume, which augmented the circulatory and vasoactive hormonal responses to LBNP in the Afghans. The lower stroke volume in Afghans residing in Denmark compared to that of matched native Danes remains to be explained.

Similar content being viewed by others
Abbreviations
- APP:
-
Arterial pulse pressure
- BSA:
-
Body surface area
- DBP:
-
Diastolic blood pressure
- HR:
-
Heart rate
- HUT:
-
Head up tilt
- LBNP:
-
Lower body negative pressure
- MSNA:
-
Muscle sympathetic nerve activity
- NaCl:
-
Sodium chloride
- PET:
-
Positron emission tomography
- PRA:
-
Plasma renin activity
- SBP:
-
Systolic blood pressure
References
Arbeille PP, Besnard SS, Kerbeci PP, Mohty DM (2005) Portal vein cross-sectional area and flow and orthostatic tolerance: a 90-day bed rest study. J Appl Physiol 99:1853–1857. doi:10.1152/japplphysiol.00331.2005
Asmar A, Bulow J, Simonsen L, Christensen NJ, Frandsen E, Norsk P (2013) Blood pressure in Afghan male immigrants to Denmark. Clin Physiol Funct Imaging 33:470–477. doi:10.1111/cpf.12055
Cai Y et al (2000) Electrical admittance for filling of the heart during lower body negative pressure in humans. J Appl Physiol 89:1569–1576
Cui J, Leuenberger UA, Gao Z, Sinoway LI (2011) Sympathetic and cardiovascular responses to venous distension in an occluded limb. Am J Physiol Regul Integr Comp Physiol 301:R1831–R1837. doi:10.1152/ajpregu.00170.2011
Cui J, McQuillan PM, Blaha C, Kunselman AR, Sinoway LI (2012) Limb venous distension evokes sympathetic activation via stimulation of the limb afferents in humans. Am J Physiol Heart Circ Physiol 303:H457–H463. doi:10.1152/ajpheart.00236.2012
Damgaard M, Norsk P (2005) Effects of ventilation on cardiac output determined by inert gas rebreathing. Clin Physiol Funct Imaging 25:142–147. doi:10.1111/j.1475-097X.2005.00602.x
Damkjaer M, Isaksson GL, Stubbe J, Jensen BL, Assersen K, Bie P (2013) Renal renin secretion as regulator of body fluid homeostasis. Pflugers Arch 465:153–165. doi:10.1007/s00424-012-1171-2
Davy KP, Seals DR, Tanaka H (1998) Augmented cardiopulmonary and integrative sympathetic baroreflexes but attenuated peripheral vasoconstriction with age. Hypertension 32:298–304
Farquhar WB, Taylor JA, Darling SE, Chase KP, Freeman R (2000) Abnormal baroreflex responses in patients with idiopathic orthostatic intolerance. Circulation 102:3086–3091
Franke WD, Lee K, Buchanan DB, Hernandez JP (2004) Blacks and whites differ in responses, but not tolerance, to orthostatic stress. Clin Auton Res 14:19–25. doi:10.1007/s10286-004-0155-5
Fu Q, Witkowski S, Okazaki K, Levine BD (2005) Effects of gender and hypovolemia on sympathetic neural responses to orthostatic stress. Am J Physiol Regul Integr Comp Physiol 289:R109–R116. doi:10.1152/ajpregu.00013.2005
Greenleaf JE et al (2000) Low LBNP tolerance in men is associated with attenuated activation of the renin–angiotensin system. Am J Physiol Regul Integr Comp Physiol 279:R822–R829
Hinds K, Stachenfeld NS (2010) Greater orthostatic tolerance in young black compared with white women. Hypertension 56:75–81. doi:10.1161/hypertensionaha.110.150011
Hjemdahl P (1993) Plasma catecholamines—analytical challenges and physiological limitations. Bailliere’s Clin Endocrinol Metab 7:307–353
Jarvis SS, Florian JP, Curren MJ, Pawelczyk JA (2012) A somatostatin analog improves tilt table tolerance by decreasing splanchnic vascular conductance. J Appl Physiol 112:1504–1511. doi:10.1152/japplphysiol.01475.2010
Johnson JM (2002) How do veins talk to arteries? J Physiol 538:341
Joyner MJ, Charkoudian N, Wallin BG (2010) Sympathetic nervous system and blood pressure in humans: individualized patterns of regulation and their implications. Hypertension 56:10–16. doi:10.1161/hypertensionaha.109.140186
Kurian AK, Cardarelli KM (2007) Racial and ethnic differences in cardiovascular disease risk factors: a systematic review. Ethn Dis 17:143–152
Levine BD et al (2002) Human muscle sympathetic neural and haemodynamic responses to tilt following spaceflight. J Physiol 538:331–340
Lundvall J, Lanne T (1989) Large capacity in man for effective plasma volume control in hypovolaemia via fluid transfer from tissue to blood. Acta Physiol Scand 137:513–520. doi:10.1111/j.1748-1716.1989.tb08788.x
Meneton P, Jeunemaitre X, de Wardener HE, MacGregor GA (2005) Links between dietary salt intake, renal salt handling, blood pressure, and cardiovascular diseases. Physiol Rev 85:679–715. doi:10.1152/physrev.00056.2003
Norsk P et al (1993) Arterial pulse pressure and vasopressin release in humans during lower body negative pressure. Am J Physiol 264:R1024–R1030
Olsen H, Vernersson E, Lanne T (2000) Cardiovascular response to acute hypovolemia in relation to age. Implications for orthostasis and hemorrhage. Am J Physiol Heart Circ Physiol 278:H222–H232
Pechere-Bertschi A et al (1998) Circadian variations of renal sodium handling in patients with orthostatic hypotension. Kidney Int 54:1276–1282. doi:10.1046/j.1523-1755.1998.00089.x
Persson F et al (2009) Renal effects of aliskiren compared with and in combination with irbesartan in patients with type 2 diabetes, hypertension, and albuminuria. Diabetes Care 32:1873–1879. doi:10.2337/dc09-0168
Poulter NR, Khaw KT, Hopwood BE, Mugambi M, Peart WS, Rose G, Sever PS (1990) The Kenyan Luo migration study: observations on the initiation of a rise in blood pressure. BMJ 300:967–972
Taneja I, Moran C, Medow MS, Glover JL, Montgomery LD, Stewart JM (2007) Differential effects of lower body negative pressure and upright tilt on splanchnic blood volume. Am J Physiol Heart Circ Physiol 292:H1420–H1426. doi:10.1152/ajpheart.01096.2006
Wallin BG, Morlin C, Hjemdahl P (1987) Muscle sympathetic activity and venous plasma noradrenaline concentrations during static exercise in normotensive and hypertensive subjects. Acta Physiol Scand 129:489–497. doi:10.1111/j.1748-1716.1987.tb08088.x
Wenner MM, Rose WC, Delaney EP, Stillabower ME, Farquhar WB (2007) Influence of plasma osmolality on baroreflex control of sympathetic activity. Am J Physiol Heart Circ Physiol 293:H2313–H2319. doi:10.1152/ajpheart.01383.2006
Xin W, Lin Z, Mi S (2014) Orthostatic hypotension and mortality risk: a meta-analysis of cohort studies. Heart 100:406–413. doi:10.1136/heartjnl-2013-304121
Acknowledgments
The efficient support of our laboratory technician, Jakob Utzon-Frank is gratefully acknowledged. This study was supported by Grant No. 272-07-0614 from the Danish Research Councils (Danish Agency for Science, Technology and Innovation).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Communicated by Michael Lindinger.
Rights and permissions
About this article
Cite this article
Asmar, A., Bülow, J., Simonsen, L. et al. Circulatory responses to lower body negative pressure in young Afghans and Danes: implications for understanding ethnic effects on blood pressure regulation. Eur J Appl Physiol 114, 2321–2329 (2014). https://doi.org/10.1007/s00421-014-2946-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00421-014-2946-2