Abstract
Vitamin A, which is found in serum, is known to affect keratinocyte proliferation, epidermal differentiation, and keratinization. In mice, stratified epithelia in the oral cavity, esophagus, and forestomach are keratinized; however, these epithelia are not keratinized in humans. Several studies have reported that three-dimensional (3D) cultures of human keratinocytes in serum-containing medium could form keratinized epithelia. Here, we evaluated the effects of serum on the morphology, expression, and localization of differentiation markers and tight junction proteins, and paracellular permeability in 3D cultures of mouse keratinocytes. We found that only 0.1% calcium-depleted serum inhibited keratinization and induced a change in the expression of differentiation marker proteins from loricrin to keratin 4; the inhibition of retinoic acid receptor-mediated signaling reversed these changes. Furthermore, the serum reduced claudin-1 protein expression and prevented its localization at occludin-positive spots on the surface of 3D cultures. On the other hand, the serum increased the protein expression of claudin-4, occludin, zonula occludens-1, and E-cadherin. These changes may contribute to the reduction of the transepithelial electrical resistance by approximately half. In conclusion, mouse keratinocytes derived from the epidermis formed non-keratinized structures in 3D cultures in response to vitamin A in serum. The results suggest that retinoic acid receptor-mediated signaling may be inhibited in the mouse epithelia in the oral cavity, esophagus, and forestomach as well as the epidermis, leading to the keratinization of these epithelia.








Similar content being viewed by others
References
Asselineau D, Bernhard B, Bailly C, Darmon M (1985) Epidermal morphogenesis and induction of the 67 kD keratin polypeptide by culture of human keratinocytes at the liquid-air interface. Exp Cell Res 159:536–539
Asselineau D, Bernard BA, Bailly C, Darmon M, Prunieras M (1986) Human epidermis reconstructed by culture: is it “normal”? J Invest Dermatol 86:181–186
Asselineau D, Bernard BA, Bailly C, Darmon M (1989) Retinoic acid improves epidermal morphogenesis. Dev Biol 133:322–335
Babkair H, Yamazaki M, Uddin MS, Maruyama S, Abe T, Essa A, Sumita Y, Ahsan MS, Swalam W, Cheng J, Saku T (2016) Aberrant expression of the tight junction molecules claudin-1 and zonula occludens-1 mediates cell growth and invasion in oral squamous cell carcinoma. Hum Pathol 57:51–60. https://doi.org/10.1016/j.humpath.2016.07.001
Ban Y, Dota A, Cooper LJ, Fullwood NJ, Nakamura T, Tsuzuki M, Mochida C, Kinoshita S (2003) Tight junction-related protein expression and distribution in human corneal epithelium. Exp Eye Res 76:663–669
Barrett AW, Selvarajah S, Franey S, Wills KA, Berkovitz BK (1998) Interspecies variations in oral epithelial cytokeratin expression. J Anat 193(Pt 2):185–193
Bernard FX, Pedretti N, Rosdy M, Deguercy A (2002) Comparison of gene expression profiles in human keratinocyte mono-layer cultures, reconstituted epidermis and normal human skin; transcriptional effects of retinoid treatments in reconstituted human epidermis. Exp Dermatol 11:59–74
Bertolero F, Kaighn ME, Gonda MA, Saffiotti U (1984) Mouse epidermal keratinocytes. Clonal proliferation and response to hormones and growth factors in serum-free medium. Exp Cell Res 155:64–80
Bertolero F, Kaighn ME, Camalier RF, Saffiotti U (1986) Effects of serum and serum-derived factors on growth and differentiation of mouse keratinocytes. In Vitro Cell Dev Biol 22:423–428
Borowiec AS, Delcourt P, Dewailly E, Bidaux G (2013) Optimal differentiation of in vitro keratinocytes requires multifactorial external control. PLoS One 8:e77507. https://doi.org/10.1371/journal.pone.0077507
Boyce ST, Ham RG (1983) Calcium-regulated differentiation of normal human epidermal keratinocytes in chemically defined clonal culture and serum-free serial culture. J Invest Dermatol 81:33s–40s
De Leenheer AP, Lambert WE, Claeys I (1982) All-trans-retinoic acid: measurement of reference values in human serum by high performance liquid chromatography. J Lipid Res 23:1362–1367
Elias PM, Fritsch PO, Lampe M, Williams ML, Brown BE, Nemanic M, Grayson S (1981) Retinoid effects on epidermal structure, differentiation, and permeability. Lab Invest 44:531–540
Frankart A, Malaisse J, De Vuyst E, Minner F, de Rouvroit CL, Poumay Y (2012) Epidermal morphogenesis during progressive in vitro 3D reconstruction at the air-liquid interface. Exp Dermatol 21:871–875. https://doi.org/10.1111/exd.12020
Fuchs E, Green H (1981) Regulation of terminal differentiation of cultured human keratinocytes by vitamin A. Cell 25:617–625
Furuse M, Sasaki H, Fujimoto K, Tsukita S (1998) A single gene product, claudin-1 or -2, reconstitutes tight junction strands and recruits occludin in fibroblasts. J Cell Biol 143:391–401
Furuse M, Hata M, Furuse K, Yoshida Y, Haratake A, Sugitani Y, Noda T, Kubo A, Tsukita S (2002) Claudin-based tight junctions are crucial for the mammalian epidermal barrier: a lesson from claudin-1-deficient mice. J Cell Biol 156:1099–1111. https://doi.org/10.1083/jcb.200110122
Groeger S, Jarzina F, Windhorst A, Meyle J (2016) Influence of retinoic acid on human gingival epithelial barriers. J Periodontal Res 51:748–757. https://doi.org/10.1111/jre.12351
Hatakeyama S, Hayashi S, Yoshida Y, Otsubo A, Yoshimoto K, Oikawa Y, Satoh M (2004) Retinoic acid disintegrated desmosomes and hemidesmosomes in stratified oral keratinocytes. J Oral Pathol Med 33:622–628. https://doi.org/10.1111/j.1600-0714.2004.00245.x
Hatakeyama S, Ishida K, Takeda Y (2010) Changes in cell characteristics due to retinoic acid; specifically, a decrease in the expression of claudin-1 and increase in claudin-4 within tight junctions in stratified oral keratinocytes. J Periodontal Res 45:207–215. https://doi.org/10.1111/j.1600-0765.2009.01219.x
Hennings H, Michael D, Cheng C, Steinert P, Holbrook K, Yuspa SH (1980) Calcium regulation of growth and differentiation of mouse epidermal cells in culture. Cell 19:245–254
Hohl D, Ruf Olano B, de Viragh PA, Huber M, Detrisac CJ, Schnyder UW, Roop DR (1993) Expression patterns of loricrin in various species and tissues. Differentiation 54:25–34
Hosomi J, Hosoi J, Abe E, Suda T, Kuroki T (1983) Regulation of terminal differentiation of cultured mouse epidermal cells by 1α,25-dihydroxyvitamin D3. Endocrinology 113:1950–1957. https://doi.org/10.1210/endo-113-6-1950
Inai T, Sengoku A, Hirose E, Iida H, Shibata Y (2007) Claudin-7 expressed on lateral membrane of rat epididymal epithelium does not form aberrant tight junction strands. Anat Rec (Hoboken) 290:1431–1438. https://doi.org/10.1002/ar.20597
Jones KB, Klein OD (2013) Oral epithelial stem cells in tissue maintenance and disease: the first steps in a long journey. Int J Oral Sci 5:121–129. https://doi.org/10.1038/ijos.2013.46
Kirschner N, Brandner JM (2012) Barriers and more: functions of tight junction proteins in the skin. Ann N Y Acad Sci 1257:158–166. https://doi.org/10.1111/j.1749-6632.2012.06554.x
Kopan R, Traska G, Fuchs E (1987) Retinoids as important regulators of terminal differentiation: examining keratin expression in individual epidermal cells at various stages of keratinization. J Cell Biol 105:427–440
Kubo A, Nagao K, Yokouchi M, Sasaki H, Amagai M (2009) External antigen uptake by Langerhans cells with reorganization of epidermal tight junction barriers. J Exp Med 206:2937–2946. https://doi.org/10.1084/jem.20091527
Lamb R, Ambler CA (2013) Keratinocytes propagated in serum-free, feeder-free culture conditions fail to form stratified epidermis in a reconstituted skin model. PLoS One 8:e52494. https://doi.org/10.1371/journal.pone.0052494
Lichti U, Anders J, Yuspa SH (2008) Isolation and short-term culture of primary keratinocytes, hair follicle populations and dermal cells from newborn mice and keratinocytes from adult mice for in vitro analysis and for grafting to immunodeficient mice. Nat Protoc 3:799–810. https://doi.org/10.1038/nprot.2008.50
Moll R, Divo M, Langbein L (2008) The human keratins: biology and pathology. Histochem Cell Biol 129:705–733. https://doi.org/10.1007/s00418-008-0435-6
Nakatsukasa M, Kawasaki S, Yamasaki K, Fukuoka H, Matsuda A, Tsujikawa M, Tanioka H, Nagata-Takaoka M, Hamuro J, Kinoshita S (2010) Tumor-associated calcium signal transducer 2 is required for the proper subcellular localization of claudin 1 and 7: implications in the pathogenesis of gelatinous drop-like corneal dystrophy. Am J Pathol 177:1344–1355. https://doi.org/10.2353/ajpath.2010.100149
O’Keefe EJ, Woodley DT, Falk RJ, Gammon WR, Briggaman RA (1987) Production of fibronectin by epithelium in a skin equivalent. J Invest Dermatol 88:634–639
Ortiz-Melo MT, Sanchez-Guzman E, Gonzalez-Robles A, Valdes J, Gomez-Flores E, Castro-Munozledo F (2013) Expression of claudins-2 and -4 and cingulin is coordinated with the start of stratification and differentiation in corneal epithelial cells: retinoic acid reversibly disrupts epithelial barrier. Biol Open 2:132–143. https://doi.org/10.1242/bio.20123145
Oshima T, Gedda K, Koseki J, Chen X, Husmark J, Watari J, Miwa H, Pierrou S (2011) Establishment of esophageal-like non-keratinized stratified epithelium using normal human bronchial epithelial cells. Am J Physiol Cell Physiol 300:C1422–C1429. https://doi.org/10.1152/ajpcell.00376.2010
Oshima T, Koseki J, Chen X, Matsumoto T, Miwa H (2012) Acid modulates the squamous epithelial barrier function by modulating the localization of claudins in the superficial layers. Lab Invest 92:22–31. https://doi.org/10.1038/labinvest.2011.139
Pavez Lorie E, Chamcheu JC, Vahlquist A, Torma H (2009) Both all-trans retinoic acid and cytochrome P450 (CYP26) inhibitors affect the expression of vitamin A metabolizing enzymes and retinoid biomarkers in organotypic epidermis. Arch Dermatol Res 301:475–485. https://doi.org/10.1007/s00403-009-0937-7
Ponec M, Weerheim A, Kempenaar J, Mommaas AM, Nugteren DH (1988) Lipid composition of cultured human keratinocytes in relation to their differentiation. J Lipid Res 29:949–961
Poumay Y, Pittelkow MR (1995) Cell density and culture factors regulate keratinocyte commitment to differentiation and expression of suprabasal K1/K10 keratins. J Invest Dermatol 104:271–276
Poumay Y, Dupont F, Marcoux S, Leclercq-Smekens M, Herin M, Coquette A (2004) A simple reconstructed human epidermis: preparation of the culture model and utilization in in vitro studies. Arch Dermatol Res 296:203–211. https://doi.org/10.1007/s00403-004-0507-y
Prunieras M, Regnier M, Woodley D (1983) Methods for cultivation of keratinocytes with an air-liquid interface. J Invest Dermatol 81:28s–33s
Regnier M, Desbas C, Bailly C, Darmon M (1988) Differentiation of normal and tumoral human keratinocytes cultured on dermis: reconstruction of either normal or tumoral architecture. In Vitro Cell Dev Biol 24:625–632
Rosdy M, Clauss LC (1990) Terminal epidermal differentiation of human keratinocytes grown in chemically defined medium on inert filter substrates at the air-liquid interface. J Invest Dermatol 95:409–414
Segrelles C, Holguin A, Hernandez P, Ariza JM, Paramio JM, Lorz C (2011) Establishment of a murine epidermal cell line suitable for in vitro and in vivo skin modelling. BMC Dermatol 11:9. https://doi.org/10.1186/1471-5945-11-9
Seo A, Kitagawa N, Matsuura T, Sato H, Inai T (2016) Formation of keratinocyte multilayers on filters under airlifted or submerged culture conditions in medium containing calcium, ascorbic acid, and keratinocyte growth factor. Histochem Cell Biol 146:585–597. https://doi.org/10.1007/s00418-016-1472-1
Smith EL, Walworth NC, Holick MF (1986) Effect of 1α,25-dihydroxyvitamin D3 on the morphologic and biochemical differentiation of cultured human epidermal keratinocytes grown in serum-free conditions. J Invest Dermatol 86:709–714
Takaoka M, Nakamura T, Ban Y, Kinoshita S (2007) Phenotypic investigation of cell junction-related proteins in gelatinous drop-like corneal dystrophy. Invest Ophthalmol Vis Sci 48:1095–1101. https://doi.org/10.1167/iovs.06-0740
Torma H (2011) Regulation of keratin expression by retinoids. Dermatoendocrinol 3:136–140. https://doi.org/10.4161/derm.3.3.15026
Tsuruta D, Green KJ, Getsios S, Jones JC (2002) The barrier function of skin: how to keep a tight lid on water loss. Trends Cell Biol 12:355–357
Virtanen M, Sirsjo A, Vahlquist A, Torma H (2010) Keratins 2 and 4/13 in reconstituted human skin are reciprocally regulated by retinoids binding to nuclear receptor RARα. Exp Dermatol 19:674–681. https://doi.org/10.1111/j.1600-0625.2010.01079.x
Wanner R, Wolff B, Glowacki F, Kolde G, Wittig B (1999) The loss of desmosomes after retinoic acid treatment results in an apparent inhibition of HaCaT keratinocyte differentiation. Arch Dermatol Res 291:346–353
Yoshida Y, Ban Y, Kinoshita S (2009) Tight junction transmembrane protein claudin subtype expression and distribution in human corneal and conjunctival epithelium. Invest Ophthalmol Vis Sci 50:2103–2108. https://doi.org/10.1167/iovs.08-3046
Acknowledgements
This study was supported in part by a Grant-in-Aid for Scientific Research (C) (no. 26460285) from the Ministry of Education, Culture, Sports, Science, and Technology in Japan.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
418_2018_1741_MOESM1_ESM.tif
Antibody specificities examined by immunofluorescence localization in oral mucosal epithelium obtained from the lower jaws of pigs. Cryosections were double stained with anti-K4 and anti-LOR antibodies. Arrows indicate the boundary between non-keratinized lingual alveolar epithelium (the left-hand side) and keratinized lingual gingiva (the right-hand side). K4 signals (green) were observed in almost all layers in the non-keratinized stratified epithelium (b). A higher magnification of the lower layers of non-keratinized stratified epithelium revealed that K4 signals are faint in the basal layer (d). K4 signals gradually decreased from the upper layers to the basal layer on the right-side of the arrow (b). Contrary to the K4 signals, LOR signals (red) appeared in the upper layer that corresponds to the granular layer on the right-side of the arrow (b’, c’). Merged images are shown in a′′–d”. Nuclei were stained with DAPI (blue). The scale bar in b” is applied to a–a′′ and b–b”: 50 μm. The scale bar in d” is applied to c–c” and d–d”: 20 μm (TIF 29411 KB)
418_2018_1741_MOESM2_ESM.tif
The raw data obtained from the immunoblotting shown in Fig. 7. COCA cultures were airlifted for 2 weeks in the presence of 0%, 0.1%, 1%, or 10% ch-FBS and analyzed by immunoblotting. Cells were lysed, fractionated by SDS-PAGE, and transferred onto PVDF membranes. Immunoblotting was performed using antibodies against CLDN1, CLDN4, occludin, ZO-1, E-cadherin, and K4. Membranes were reprobed after stripping the primary and secondary antibodies. Lysates obtained from COCA 3D cultures in 0% (lane 1), 0.1% (lane 2), 1% (lane 3), and 10% (lane 4) ch-FBS were used. The observed band sizes (indicated by arrowheads) are as follows: CLDNs 1 and 4, ~20 kDa; occludin, 59 kDa; ZO-1, ~225 kDa; E-cadherin, ~135 kDa; K4, 57 kDa (TIF 8974 KB)
418_2018_1741_MOESM3_ESM.tif
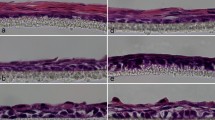
Controls for immunofluorescence in COCA 3D cultures. COCA cells seeded on insert filters were airlifted for 2 weeks in the presence of 0% (a, a’, a”), 0.1% (b, b’, b”), 1% (c, c’, c”), and 10% (d, d’, d”) ch-FBS. COCA cells seeded on insert filters were airlifted for 1 week in the presence of 1% (e, e’, e”) ch-FBS and for another week with 0.2 μM BMS 493 (f, f’, f”). Cryosections were incubated with BSA-PBS in place of primary antibodies and then secondary antibodies were added (a mixture of anti-mouse and anti-rabbit Ig conjugated with either Alexa 488 or Alexa 568). Images derived from Alexa 488 (green) are shown in a–f. Images derived from Alexa 568 (red) are shown in a’–f’. Nuclei were stained with DAPI (blue). Merged images are shown in a”–f”. No specific signals were observed in these controls. Scale bar: 20 μm (TIF 29214 KB)
418_2018_1741_MOESM4_ESM.tif
Antibody specificities examined by immunofluorescence localization in MDCK II cells. Cells were double stained with mouse anti-occludin (b, c, d, e) and either rabbit anti-CLDN1 (b’), anti-CLDN4 (c’), anti-ZO-1 (d’), or anti-E-cadherin (e’) antibodies. In the control (a–a”), BSA-PBS was used in place of primary antibodies. Merged images are shown in a”–e”. Nuclei were stained with DAPI (blue). Occludin was localized at the apical junctions with CLDN1, CLDN4, and ZO-1, but E-cadherin was localized in the lateral cell membrane below the apical junctions. Some nuclei were heavily or weakly stained with anti-CLDN4 (c’) or anti-ZO-1 antibody (d’), respectively. Scale bar: 20 μm (TIF 23817 KB)
Rights and permissions
About this article
Cite this article
Ozaki, A., Otani, T., Kitagawa, N. et al. Serum affects keratinization and tight junctions in three-dimensional cultures of the mouse keratinocyte cell line COCA through retinoic acid receptor-mediated signaling. Histochem Cell Biol 151, 315–326 (2019). https://doi.org/10.1007/s00418-018-1741-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00418-018-1741-2