Abstract
Codeine-containing cough syrup (CCS) is considered as one of the most popular drug of dependence among adolescents because of its inexpensiveness and easy availability. However, its relationship with neurobiological effects remains sparsely explored. Herein, we examined how high-impulse behaviours relate to changes in the brain structural networks. Forty codeine-containing cough syrup dependent (CCSD) users and age-, gender-, and number of cigarettes smoked per day -matched forty healthy control (HC) subjects underwent structural brain imaging via MRI. High-impulse behaviour was assessed using the 30-item self-rated Barratt Impulsiveness Scale (BIS-11), and structural networks were constructed using diffusion tensor imaging and AAL-90 template. Between-group topological metrics were compared using nonparametric permutations. Benjamin–Hochberg false discovery rate correction was used to correct for multiple comparisons (P < 0.05). The relationships between abnormal network metrics and clinical characteristics of CCS dependent (BIS-11 total score, CCS- dependent duration and mean dose) were examined by Spearman’s correlation. Structural networks of the CCSD group demonstrated lower small-world properties than those of the HC group. Abnormal changes in nodal properties among CCSD users were located mainly in the frontal gyrus, inferior parietal lobe and olfactory cortex. NBS analysis further indicated disrupted structural connections between the frontal gyrus and multiple brain regions. There were significant correlations between abnormal nodal properties of the frontal gyrus and clinical characteristics (BIS-11 total score, CCS dependent duration and mean dose) in the CCSD group. These findings suggest that the high-impulse behavioural expression in CCS addiction is associated with widespread brain regions, particularly within those in the frontal cortex. Aberrant brain regions and disrupted connectivity of structural network may be the bases of neuropathology for underlying symptoms of high-impulse behaviours in CCSD users, which may provide a novel sight to better treat and prevent codeine dependency in adolescents.




Similar content being viewed by others
Abbreviations
- CCS:
-
Codeine-containing cough syrup
- CCSD users:
-
Codeine-containing cough syrup dependent
- HC:
-
Healthy control
- HCs:
-
Healthy control subjects
- WM:
-
White matter
- DTI:
-
Diffusion tensor imaging
- FA:
-
Fractional anisotropy
- FN:
-
Streamline number
References
Lo MY, Ong MW, Lin JG, Sun WZ (2015) Codeine consumption from over-the-counter anti-cough syrup in Taiwan: a useful indicator for opioid abuse. Acta Anaesthesiol Taiwan 53(4):135–138. https://doi.org/10.1016/j.aat.2015.10.001
Van Hout MC, Norman I (2016) Misuse of non-prescription codeine containing products: recommendations for detection and reduction of risk in community pharmacies. Int J Drug Policy 27:17–22. https://doi.org/10.1016/j.drugpo.2015.09.007
Tay EMY, Roberts DM. https://doi.org/10.1080/17512433.2018.1537122
Carlson RG, Nahhas RW, Martins SS, Daniulaityte R (2016) Predictors of transition to heroin use among initially non-opioid dependent illicit pharmaceutical opioid users: a natural history study. Drug Alcohol Depend 160(37):127–134. https://doi.org/10.1016/j.drugalcdep.2015.12.026
Li Q, Liu J, Wang W, Wang Y, Li W, Chen J, Zhu J, Yan X, Li Y, Li Z, Ye J, Wang W (2018) Disrupted coupling of large-scale networks is associated with relapse behaviour in heroin-dependent men. J Psychiatry Neurosci 43(1):48–57
Qiu YW, Jiang GH, Ma XF, Su HH, Lv XF, Zhuo FZ (2017) Aberrant interhemispheric functional and structural connectivity in heroin-dependent individuals. Addict Biol 22(4):1057–1067. https://doi.org/10.1111/adb.12387
Wu Q, Yu J, Yang C, Chen J, Yang L, Zhang H, Teng S, Li J, Yan D, Cao J, Zhao Y, Wang Z (2016) Nonmedical use of cough syrup among secondary vocational school students: a National Survey in China. Medicine (Baltimore) 95(10):e2969–105. https://doi.org/10.1097/MD.0000000000002969
Qiu YW, Jiang GH, Su HH, Lv XF, Ma XF, Tian JZ, Zhuo FZ (2016) Short-term UROD treatment on cerebral function in codeine-containing cough syrups dependent male individuals. Eur Radiol 26(9):2964–2973. https://doi.org/10.1007/s00330-015-4139-8
Hua K, Wang T, Li C, Li S, Ma X, Li C, Li M, Fu S, Yin Y, Wu Y, Liu M, Yu K, Fang J, Wang P, Jiang G (2018) Abnormal degree centrality in chronic users of codeine-containing cough syrups: a resting-state functional magnetic resonance imaging study. Neuroimage Clin 19:775–781. https://doi.org/10.1016/j.nicl.2018.06.003
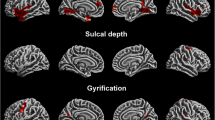
Li M, Hua K, Li S, Li C, Zhan W, Wen H, Ma X, Tian J, Jiang G (2019) Cortical morphology of chronic users of codeine-containing cough syrups: association with sulcal depth, gyrification, and cortical thickness. Eur Radiol. https://doi.org/10.1007/s00330-019-06165-0
Liu F, Zhuo C, Yu C (2016) Altered cerebral blood flow covariance network in schizophrenia. Front Neurosci 10:308. https://doi.org/10.3389/fnins.2016.00308
Qiu YW, Su HH, Lv XF, Jiang GH (2015) Abnormal white matter integrity in chronic users of codeine-containing cough syrups: a tract-based spatial statistics study. AJNR Am J Neuroradiol 36(1):50–56. https://doi.org/10.3174/ajnr.A4070
Grant JE, Chamberlain SR (2014) Impulsive action and impulsive choice across substance and behavioral addictions: cause or consequence? Addict Behav 39(11):1632–1639. https://doi.org/10.1016/j.addbeh.2014.04.022
Broos N, van Mourik Y, Schetters D, De Vries TJ, Pattij T (2017) Dissociable effects of cocaine and yohimbine on impulsive action and relapse to cocaine seeking. Psychopharmacology 234(22):3343–3351. https://doi.org/10.1007/s00213-017-4711-9
Rodriguez-Cintas L, Daigre C, Grau-Lopez L, Barral C, Perez-Pazos J, Voltes N, Braquehais MD, Casas M, Roncero C (2016) Impulsivity and addiction severity in cocaine and opioid dependent patients. Addict Behav 58:104–109. https://doi.org/10.1016/j.addbeh.2016.02.029
Hobkirk AL, Bell RP, Utevsky AV, Huettel S, Meade CS (2019) Reward and executive control network resting-state functional connectivity is associated with impulsivity during reward-based decision making for cocaine users. Drug Alcohol Depend 194:32–39. https://doi.org/10.1016/j.drugalcdep.2018.09.013
Yao S, Yang H, Zhu X, Auerbach RP, Abela JR, Pulleyblank RW, Tong X (2007) An examination of the psychometric properties of the Chinese version of the Barratt Impulsiveness Scale, 11th version in a sample of Chinese adolescents. Percept Mot Skills 104(3 Pt 2):1169–1182. https://doi.org/10.2466/pms.104.4.1169-1182
Cui Z, Zhong S, Xu P, He Y, Gong G (2013) PANDA: a pipeline toolbox for analyzing brain diffusion images. Front Hum Neurosci 7:42. https://doi.org/10.3389/fnhum.2013.00042
Tzourio-Mazoyer N, Landeau B, Papathanassiou D, Crivello F, Etard O, Delcroix N, Mazoyer B, Joliot M (2002) Automated anatomical labeling of activations in SPM using a macroscopic anatomical parcellation of the MNI MRI single-subject brain. Neuroimage 15(1):273–289. https://doi.org/10.1006/nimg.2001.0978
Chen Z, Liu M, Gross DW, Beaulieu C (2013) Graph theoretical analysis of developmental patterns of the white matter network. Front Hum Neurosci 7:716. https://doi.org/10.3389/fnhum.2013.00716
Shu N, Wang X, Bi Q, Zhao T, Han Y (2018) Disrupted topologic efficiency of white matter structural connectome in individuals with subjective cognitive decline. Radiology 286(1):229–238. https://doi.org/10.1148/radiol.2017162696
Wang J, Wang X, Xia M, Liao X, Evans A, He Y (2015) GRETNA: a graph theoretical network analysis toolbox for imaging connectomics. Front Hum Neurosci 9:386. https://doi.org/10.3389/fnhum.2015.00386
Wu Y, Liu M, Zeng S, Ma X, Yan J, Lin C, Xu G, Li G, Yin Y, Fu S, Hua K, Li C, Wang T, Li C, Jiang G (2018) Abnormal topology of the structural connectome in the limbic cortico-basal-ganglia circuit and default-mode network among primary insomnia patients. Front Neurosci 12:860. https://doi.org/10.3389/fnins.2018.00860
Rubinov M, Sporns O (2010) Complex network measures of brain connectivity: uses and interpretations. Neuroimage 52(3):1059–1069. https://doi.org/10.1016/j.neuroimage.2009.10.003
Zhang R, Jiang G, Tian J, Qiu Y, Wen X, Zalesky A, Li M, Ma X, Wang J, Li S, Wang T, Li C, Huang R (2016) Abnormal white matter structural networks characterize heroin-dependent individuals: a network analysis. Addict Biol 21(3):667–678. https://doi.org/10.1111/adb.12234
Liu F, Wang Y, Li M, Wang W, Li R, Zhang Z, Lu G, Chen H (2017) Dynamic functional network connectivity in idiopathic generalized epilepsy with generalized tonic-clonic seizure. Hum Brain Mapp 38(2):957–973. https://doi.org/10.1002/hbm.23430
Watts DJ, Strogatz SH (1998) Collective dynamics of 'small-world' networks. Nature 393(6684):440–442. https://doi.org/10.1038/30918
Nichols TE, Holmes AP (2002) Nonparametric permutation tests for functional neuroimaging: a primer with examples. Hum Brain Mapp 15(1):1–25
Benjamini Y, Hochberg Y (1995) Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc (Methodol) 57(1):289–300
Milella MS, Fotros A, Gravel P, Casey KF, Larcher K, Verhaeghe JA, Cox SM, Reader AJ, Dagher A, Benkelfat C, Leyton M (2016) Cocaine cue-induced dopamine release in the human prefrontal cortex. J Psychiatry Neurosci 41(5):322–330. https://doi.org/10.1503/jpn.150207
Koob GF (2006) The neurobiology of addiction: a neuroadaptational view relevant for diagnosis. Addiction 101(Suppl 1):23–30. https://doi.org/10.1111/j.1360-0443.2006.01586.x
Baler RD, Volkow ND (2006) Drug addiction: the neurobiology of disrupted self-control. Trends Mol Med 12(12):559–566. https://doi.org/10.1016/j.molmed.2006.10.005
Otis JM, Namboodiri VM, Matan AM, Voets ES, Mohorn EP, Kosyk O, McHenry JA, Robinson JE, Resendez SL, Rossi MA, Stuber GD (2017) Prefrontal cortex output circuits guide reward seeking through divergent cue encoding. Nature 543(7643):103–107. https://doi.org/10.1038/nature21376
Wang Y, Zhu J, Li Q, Li W, Wu N, Zheng Y, Chang H, Chen J, Wang W (2013) Altered fronto-striatal and fronto-cerebellar circuits in heroin-dependent individuals: a resting-state FMRI study. PLoS ONE ONE 8(3):e58098. https://doi.org/10.1371/journal.pone.0058098
Sinha R (2013) The clinical neurobiology of drug craving. Curr Opin Neurobiol 23(4):649–654. https://doi.org/10.1016/j.conb.2013.05.001
Garavan H (2010) Insula and drug cravings. Brain Struct Funct 214(5–6):593–601. https://doi.org/10.1007/s00429-010-0259-8
Li X, Chen L, Ma R, Wang H, Wan L, Wang Y, Bu J, Hong W, Lv W, Vollstadt-Klein S, Yang Y, Zhang X (2019) The top-down regulation from the prefrontal cortex to insula via hypnotic aversion suggestions reduces smoking craving. Hum Brain Mapp 40(6):1718–1728. https://doi.org/10.1002/hbm.24483
Costumero V, Rosell-Negre P, Bustamante JC, Fuentes-Claramonte P, Llopis JJ, Avila C, Barros-Loscertales A (2018) Left frontoparietal network activity is modulated by drug stimuli in cocaine addiction. Brain Imaging Behav 12(5):1259–1270. https://doi.org/10.1007/s11682-017-9799-3
Filbey FM, Gohel S, Prashad S, Biswal BB (2018) Differential associations of combined vs isolated cannabis and nicotine on brain resting state networks. Brain Struct Funct 223(7):3317–3326. https://doi.org/10.1007/s00429-018-1690-5
Li M, Chen H, Wang J, Liu F, Long Z, Wang Y, Iturria-Medina Y, Zhang J, Yu C, Chen H (2014) Handedness- and hemisphere-related differences in small-world brain networks: a diffusion tensor imaging tractography study. Brain Connect 4(2):145–156. https://doi.org/10.1089/brain.2013.0211
Farrer C, Frey SH, Van Horn JD, Tunik E, Turk D, Inati S, Grafton ST (2008) The angular gyrus computes action awareness representations. Cereb Cortex 18(2):254–261. https://doi.org/10.1093/cercor/bhm050
Niu H, Zheng Y, Huma T, Rizak JD, Li L, Wang G, Ren H, Xu L, Yang J, Ma Y, Lei H (2013) Lesion of olfactory epithelium attenuates expression of morphine-induced behavioral sensitization and reinstatement of drug-primed conditioned place preference in mice. Pharmacol Biochem Behav 103(3):526–534. https://doi.org/10.1016/j.pbb.2012.10.009
Kermen F, Sultan S, Sacquet J, Mandairon N, Didier A (2010) Consolidation of an olfactory memory trace in the olfactory bulb is required for learning-induced survival of adult-born neurons and long-term memory. PLoS ONE ONE 5(8):e12118. https://doi.org/10.1371/journal.pone.0012118
Koob GF, Volkow ND (2016) Neurobiology of addiction: a neurocircuitry analysis. Lancet Psychiatry 3(8):760–773. https://doi.org/10.1016/S2215-0366(16)00104-8
Koob GF, Volkow ND (2010) Neurocircuitry of addiction. Neuropsychopharmacology 35(1):217–238. https://doi.org/10.1038/npp.2009.110
Hanlon CA, Dowdle LT, Henderson JS (2018) Modulating neural circuits with transcranial magnetic stimulation: implications for addiction treatment development. Pharmacol Rev 70(3):661–683. https://doi.org/10.1124/pr.116.013649
Madeo G, Bonci A (2019) Rewiring the addicted brain: circuits-based treatment for addiction. Cold Spring Harb Symp Quant Biol 83:173–184. https://doi.org/10.1101/sqb.2018.83.038158
Acknowledgments
We thank the patients for their participation in the study and the medical and nurse staff for their collaboration in the realization of this work.
Funding
This study has received funding by the National Natural Science Foundation of China (Grant Nos. 81901729 and 81771807, 81701111), the Natural Science Foundation of Guangdong (Grant Nos. 2019A1515011314, 2015A030313723).
Author information
Authors and Affiliations
Contributions
YW, GJ—study concepts/study design or data acquisition or data analysis/interpretation, study concepts/study design or data acquisition or data analysis/interpretation, all authors; manuscript drafting or manuscript revision for important intellectual content, all authors; approval of final version of submitted manuscript, all authors; agrees to ensure any questions related to the work are appropriately resolved, all authors; project administration—YW, GJ, Supervision—GJ, writing-original draft—YW, writing-review & editing—YW, ZZ, ML; visualization—ZZ, YW; data curation—SF, YY, ZL, SX; investigation—SF, XM; formal analysis—CG, JL, YY; and software—YW, JF, KY.
Corresponding author
Ethics declarations
Conflict of interest
The authors declaim no financial or any other potential conflict of interest.
Additional information
Communicated by Sebastian Walther.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wu, Y., Zhou, Z., Li, M. et al. Abnormal white matter within brain structural networks is associated with high-impulse behaviour in codeine-containing cough syrup dependent users. Eur Arch Psychiatry Clin Neurosci 271, 823–833 (2021). https://doi.org/10.1007/s00406-020-01111-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00406-020-01111-4