Abstract
Purpose
Chronic pelvic pain (CPP) in women is a complex syndrome and symptoms are associated with sexual dysfunction, musculoskeletal and myofascial disorders, and comorbid psychiatric disorders. Its widespread prevalence results in substantial expense due to therapy and lost productivity, and it is perhaps one of the most urgent and neglected medical needs. This systematic review and meta-analysis aimed to estimate the role of mindfulness and pelvic floor physical therapy (PFPT) in the treatment or management of women with CPP.
Methods
This systematic review (CRD42020204987) searched for relevant publications between January 2000 and November 2020 on MEDLINE/PubMed, Web of Science, One File GALE, and Technology Research databases using the following search terms: chronic pelvic pain, pelvic floor physical therapy/physiotherapy, mindfulness, and their variants. Risk of bias and quality of evidence were evaluated.
Results
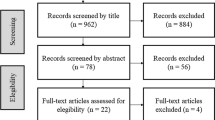
Seven clinical trials (n = 279) were included in the review, and five in the meta-analysis (n = 225). For the pain outcome and its catastrophizing, there was a statistical difference for the Pain Catastrophizing Scale after treatment and during follow-up with mindfulness and PFPT (MD = − 3.82 [− 6.97, − 0.68], p = 0.01, and MD = − 4.49 [− 7.61, − 1.37], p = 0.00, respectively). Sexual function, assessed by the female sexual function index, differed significantly during follow-up between PFPT and mindfulness (MD = − 0.72 [− 1.38, − 0.05], p = 0.03).
Conclusion
The small number of studies applying both PFPT and mindfulness to CPP suggests that a multidisciplinary approach is required to treat women with CPP, and further studies involving these therapeutic techniques throughout the CPP cycle are needed.





Similar content being viewed by others
Availability of data and materials
All relevant data are within the paper.
References
Hilton L, Hempel S, Ewing BA, Apaydin E, Xenakis L, Newberry S, Colaiaco B, Maher AR, Shanman RM, Sorbero ME, Maglione MA (2017) Mindfulness meditation for chronic pain: systematic review and meta-analysis. Ann Behav Med 51:199–213. https://doi.org/10.1007/s12160-016-9844-2
George SE, Clinton SC, Borello-France DF (2013) Physical therapy management of female chronic pelvic pain: anatomic considerations. Clin Anat 26:77–88. https://doi.org/10.1002/ca.22187
Pastore EA, Katzman WB (2012) Recognizing myofascial pelvic pain in the female patient with chronic pelvic pain. J Obstet Gynecol Neonatal Nurs 41:680–691. https://doi.org/10.1111/j.1552-6909.2012.01404.x
Sedighimehr N, Manshadi FD, Shokouhi N, Baghban AA (2018) Pelvic musculoskeletal dysfunctions in women with and without chronic pelvic pain. J Bodyw Mov Ther 22:92–96. https://doi.org/10.1016/j.jbmt.2017.05.001
Miranda R, Schor E, Girao MJ (2009) Postural evaluation in women with chronic pelvic pain. Rev Bras Ginecol Obstet 31:353–360
Hughes C, May S (2020) A directional preference approach for chronic pelvic pain, bladder dysfunction and concurrent musculoskeletal symptoms: a case series. J Man Manip Ther 28:170–180. https://doi.org/10.1080/10669817.2019.1668994
Berghmans B (2018) Physiotherapy for pelvic pain and female sexual dysfunction: an untapped resource. Int Urogynecol J 29:631–638. https://doi.org/10.1007/s00192-017-3536-8
Brotto LA, Basson R, Smith KB, Driscoll M, Sadownik L (2015) Mindfulness-based group therapy for women with provoked vestibulodynia. Mindfulness 6:417–432
Wuest J, Merritt-Gray M, Ford-Gilboe M, Lent B, Varcoe C, Campbell JC (2008) Chronic pain in women survivors of intimate partner violence. J Pain 9:1049–1057. https://doi.org/10.1016/j.jpain.2008.06.009
Adelstein SA, Lee UJ (2016) The role of mindfulness in urinary urgency symptoms. Curr Bladder Dysfunct Rep 11:38–44
Hansen KE, Kesmodel US, Kold M, Forman A (2017) Long-term effects of mindfulness-based psychological intervention for coping with pain in endometriosis: a six-year follow-up on a pilot study. Nord Psychol 69:100–109
Evans S, Fernandez S, Olive L, Payne LA, Mikocka-Walus A (2019) Psychological and mind-body interventions for endometriosis: a systematic review. J Psychosom Res 124:109756. https://doi.org/10.1016/j.jpsychores.2019.109756
Tajerian M, Clark JD (2017) Nonpharmacological interventions in targeting pain-related brain plasticity. Neural Plast 2017:2038573. https://doi.org/10.1155/2017/2038573
Montenegro ML, Mateus-Vasconcelos EC, Candido dos Reis FJ, Rosa e Silva JC, Nogueira AA, Poli Neto OB (2010) Thiele massage as a therapeutic option for women with chronic pelvic pain caused by tenderness of pelvic floor muscles. J Eval Clin Pract 16:981–982. https://doi.org/10.1111/j.1365-2753.2009.01202.x
Moher D, Liberati A, Tetzlaff J, Altman DG, Prisma Group (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Cochrane Training (2019) Cochrane handbook for systematic reviews of interventions: Cochrane. www.training.cochrane.org/handbook. Accessed May 2021
McGrath S, Zhao X, Steele R, Thombs BD, Benedetti A, Collaboration DESD (2020) Estimating the sample mean and standard deviation from commonly reported quantiles in meta-analysis. Stat Methods Med Res 19:2520–2537. https://doi.org/10.1177/0962280219889080
Borenstein M, Hedges LV, Higgins JP, Rothstein HR (2009) Introduction to meta-analysis. Wiley, New York
Hedges LV (1981) Distribution theory for Glass’s estimator of effect size and related estimators. J duc Behav Stat 6:107–128. https://doi.org/10.3102/10769986006002107
Goldfinger C, Pukall CF, Thibault-Gagnon S, McLean L, Chamberlain S (2016) Effectiveness of cognitive-behavioral therapy and physical therapy for provoked vestibulodynia: a randomized pilot study. J Sex Med 13:88–94. https://doi.org/10.1016/j.jsxm.2015.12.003
Ladi-Seyedian SS, Sharifi-Rad L, Nabavizadeh B, Kajbafzadeh AM (2019) Traditional biofeedback vs. pelvic floor physical therapy-is one clearly superior? Curr Urol Rep 20:38. https://doi.org/10.1007/s11934-019-0901-9
Li X, Hu L (2016) The role of stress regulation on neural plasticity in pain chronification. Neural Plast 2016:6402942. https://doi.org/10.1155/2016/640294
Lampe A, Solder E, Ennemoser A, Schubert C, Rumpold G, Sollner W (2000) Chronic pelvic pain and previous sexual abuse. Obstet Gynecol 96:929–933. https://doi.org/10.1016/s0029-7844(00)01072-3
Wein AJ (2015) Re: Prevalence of myofascial chronic pelvic pain and the effectiveness of pelvic floor physical therapy. J Urol 194:730. https://doi.org/10.1016/j.juro.2015.06.065
Bonder JH, Chi M, Rispoli L (2017) Myofascial pelvic pain and related disorders. Phys Med Rehabil Clin N Am 28:501–515. https://doi.org/10.1016/j.pmr.2017.03.005
Rosenbaum TY (2010) Musculoskeletal pain and sexual function in women. J Sex Med 7:645–653. https://doi.org/10.1111/j.1743-6109.2009.01490.x
Bonnema R, McNamara M, Harsh J, Hopkins E (2018) Primary care management of chronic pelvic pain in women. Cleve Clin J Med 85:215–223
Moseley GL, Flor H (2012) Targeting cortical representations in the treatment of chronic pain: a review. Neurorehabil Neural Repair 26(6):646–652. https://doi.org/10.1177/1545968311433209
Dewitte M, Borg C, Lowenstein L (2018) A psychosocial approach to female genital pain. Nat Rev Urol 15(1):25–41. https://doi.org/10.1038/nrurol.2017.187
Gentilcore-Saulnier E, McLean L, Goldfinger C, Pukall CF, Chamberlain S (2010) Pelvic floor muscle assessment outcomes in women with and without provoked vestibulodynia and the impact of a physical therapy program. J Sex Med 7:1003–1022. https://doi.org/10.1111/j.1743-6109.2009.01642.x
Henzell H, Berzins K, Langford JP (2017) Provoked vestibulodynia: current perspectives. Int J Womens Health 9:631–642. https://doi.org/10.2147/IJWH.S113416
Edwards RR, Dworkin RH, Sullivan MD, Turk DC, Wasan AD (2016) The role of psychosocial processes in the development and maintenance of chronic pain. J Pain 17:T70-92. https://doi.org/10.1016/j.jpain.2016.01.001
Van Oudenhove L, Crowell MD, Drossman DA, Halpert AD, Keefer L, Lackner JM, Murphy TB, Naliboff BD, Levy RL (2016) Biopsychosocial aspects of functional gastrointestinal disorders. Gastroenterology. https://doi.org/10.1053/j.gastro.2016.02.027
Allaire C, Williams C, Bodmer-Roy S, Zhu S, Arion K, Ambacher K, Wu J, Yosef A, Wong F, Noga H, Britnell S, Yager H, Bedaiwy MA, Albert AY, Lisonkova S, Yong PJ (2018) Chronic pelvic pain in an interdisciplinary setting: 1-year prospective cohort. Am J Obstet Gynecol 218:114e111-114e112. https://doi.org/10.1016/j.ajog.2017.10.002
Berghmans B, Seleme MR, Bernards ATM (2020) Physiotherapy assessment for female urinary incontinence. Int Urogynecol J 31:917–931. https://doi.org/10.1007/s00192-020-04251-2
Funding
None.
Author information
Authors and Affiliations
Contributions
CCB: protocol/project development; data collection or management; data analysis; manuscript writing/editing. RF: protocol/project development. CM: protocol/project development. R: data collection or management; data analysis; manuscript writing/editing. TM: data analysis. GVPM: data collection or management; data analysis; manuscript writing/editing. MC: data collection.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Code availability
Not applicable.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bittelbrunn, C.C., de Fraga, R., Martins, C. et al. Pelvic floor physical therapy and mindfulness: approaches for chronic pelvic pain in women—a systematic review and meta-analysis. Arch Gynecol Obstet 307, 663–672 (2023). https://doi.org/10.1007/s00404-022-06514-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-022-06514-3