Abstract
Purpose
The difference in prognosis between genders after abdominoperineal resection (APR) for low rectal cancer (LRC) is unclear. This study aimed to compare survival outcomes between genders in patients with LRC who underwent curative APR.
Methods
This retrospective cohort study used a database of consecutive colorectal resections. Patients who received curative APR with LRC were grouped according to their gender. Female patients were frequency-matched 1:1 on American Joint Committee on Cancer (AJCC) stage to male patients. Overall survival (OS), disease-free survival (DFS), and their independent risk factors were examined.
Results
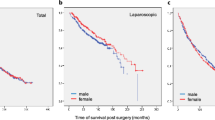
A total of 140 patients with APR for LRC were included after matching: 70 (50.0%) males and 70 (50.0%) females. No significant differences were found between the groups in terms of age, operation methods, AJCC stage, and adjuvant therapy (all P > 0.05). Median follow-up was 39 (range: 3–128) months. Male gender was independently associated with worse OS (adjusted hazard ratio [HR] = 2.755, 95% CI: 1.507–5.038, P = 0.001) and worse DFS (adjusted HR = 2.440, 95% CI: 1.254–4.746, P = 0.009). Subgroup analysis revealed that female patients with stage III disease had better OS (P = 0.001) and DFS (P < 0.001) than male patients.
Conclusion
Gender affects survival after a curative APR for LRC. Compared with females, male patients with LRC after curative APR had worse prognosis, especially for stage III disease.



Similar content being viewed by others
Data availability
The data set supporting the results of this article are included within the article.
References
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68(6):394–424. https://doi.org/10.3322/caac.21492
Chen W, Zheng R, Zeng H, Zhang S, He J (2015) Annual report on status of cancer in China, 2011. Chin J Cancer Res 27(1):2–12. https://doi.org/10.3978/j.issn.1000-9604.2015.01.06
Chen W, Zheng R, Baade PD, Zhang S, Zeng H, Bray F, Jemal A, Yu XQ, He J (2016) Cancer statistics in China, 2015. CA Cancer J Clin 66(2):115–132. https://doi.org/10.3322/caac.21338
Deng Y (2017) Rectal cancer in Asian vs. Western countries: why the variation in incidence? Curr Treat Options in Oncol 18(10):64. https://doi.org/10.1007/s11864-017-0500-2
Zhang S, Cui Y, Weng Z, Gong X, Chen M, Zhong B (2009) Changes on the disease pattern of primary colorectal cancers in Southern China: a retrospective study of 20 years. Int J Color Dis 24(8):943–949. https://doi.org/10.1007/s00384-009-0726-y
Chew MH, Yeh YT, Lim E, Seow-Choen F (2016) Pelvic autonomic nerve preservation in radical rectal cancer surgery: changes in the past 3 decades. Gastroenterol Rep (Oxf) 4(3):173–185. https://doi.org/10.1093/gastro/gow023
Rullier E, Goffre B, Bonnel C, Zerbib F, Caudry M, Saric J (2001) Preoperative radiochemotherapy and sphincter-saving resection for T3 carcinomas of the lower third of the rectum. Ann Surg 234(5):633–640. https://doi.org/10.1097/00000658-200111000-00008
Park SY, Choi GS, Park JS, Kim HJ, Choi WH, Ryuk JP (2013) Robotic-assisted transabdominal intersphincteric resection: a technique involving a completely abdominal approach and coloanal anastomosis. Surg Laparosc Endosc Percutan Tech 23(1):e5–e10. https://doi.org/10.1097/SLE.0b013e318275b27a
Rullier E, Laurent C, Bretagnol F, Rullier A, Vendrely V, Zerbib F (2005) Sphincter-saving resection for all rectal carcinomas: the end of the 2-cm distal rule. Ann Surg 241(3):465–469. https://doi.org/10.1097/01.sla.0000154551.06768.e1
Varpe P, Huhtinen H, Rantala A, Salminen P, Rautava P, Hurme S, Gronroos J (2011) Quality of life after surgery for rectal cancer with special reference to pelvic floor dysfunction. Color Dis 13(4):399–405. https://doi.org/10.1111/j.1463-1318.2009.02165.x
Benson AB, Venook AP, Al-Hawary MM, Cederquist L, Chen YJ, Ciombor KK, Cohen S, Cooper HS, Deming D, Engstrom PF, Grem JL, Grothey A, Hochster HS, Hoffe S, Hunt S, Kamel A, Kirilcuk N, Krishnamurthi S, Messersmith WA, Meyerhardt J, Mulcahy MF, Murphy JD, Nurkin S, Saltz L, Sharma S, Shibata D, Skibber JM, Sofocleous CT, Stoffel EM, Stotsky-Himelfarb E, Willett CG, Wuthrick E, Gregory KM, Gurski L, Freedman-Cass DA (2018) Rectal cancer, version 2.2018, NCCN clinical practice guidelines in oncology. J Natl Compr Cancer Netw 16(7):874–901. https://doi.org/10.6004/jnccn.2018.0061
den Dulk M, Putter H, Collette L, Marijnen CAM, Folkesson J, Bosset JF, Rodel C, Bujko K, Pahlman L, van de Velde CJH (2009) The abdominoperineal resection itself is associated with an adverse outcome: the European experience based on a pooled analysis of five European randomised clinical trials on rectal cancer. Eur J Cancer 45(7):1175–1183. https://doi.org/10.1016/j.ejca.2008.11.039
Perry WB, Connaughton JC (2007) Abdominoperineal resection: how is it done and what are the results? Clin Colon Rectal Surg 20(3):213–220. https://doi.org/10.1055/s-2007-984865
Herrinton LJ, Altschuler A, McMullen CK, Bulkley JE, Hornbrook MC, Sun V, Wendel CS, Grant M, Baldwin CM, Demark-Wahnefried W, Temple LK, Krouse RS (2016) Conversations for providers caring for patients with rectal cancer: comparison of long-term patient-centered outcomes for patients with low rectal cancer facing ostomy or sphincter-sparing surgery. CA Cancer J Clin 66(5):387–397. https://doi.org/10.3322/caac.21345
Seike K, Koda K, Oda K, Kosugi C, Shimizu K, Miyazaki M (2009) Gender differences in pelvic anatomy and effects on rectal cancer surgery. Hepatogastroenterology 56(89):111–115
Salerno G, Daniels IR, Brown G, Heald RJ, Moran BJ (2006) Magnetic resonance imaging pelvimetry in 186 patients with rectal cancer confirms an overlap in pelvic size between males and females. Color Dis 8(9):772–776. https://doi.org/10.1111/j.1463-1318.2006.01090.x
Tilney HS, Heriot AG, Purkayastha S, Antoniou A, Aylin P, Darzi AW, Tekkis PP (2008) A national perspective on the decline of abdominoperineal resection for rectal cancer. Ann Surg 247(1):77–84. https://doi.org/10.1097/SLA.0b013e31816076c3
Lydrup ML, Hoglund P (2015) Gender aspects of survival after surgical treatment for rectal cancer. Color Dis 17(5):390–396. https://doi.org/10.1111/codi.12871
Anderin C, Martling A, Hellborg H, Holm T (2010) A population-based study on outcome in relation to the type of resection in low rectal cancer. Dis Colon rectum 53(5):753–760. https://doi.org/10.1007/DCR.0b013e3181cf7e27
Nomura M, Takahashi H, Fujii M, Miyoshi N, Haraguchi N, Hata T, Matsuda C, Yamamoto H, Mizushima T, Mori M, Doki Y (2019) Clinical significance of invasion distance relative to prognosis in pathological T3 colorectal cancer. Oncol Lett 18(5):5614–5620. https://doi.org/10.3892/ol.2019.10913
Kleemann M, Benecke C, Helfrich D, Bruch HP, Keck T, Laubert T (2014) Prospective analysis of more than 1,000 patients with rectal carcinoma: are there gender-related differences? Viszeralmedizin 30(2):118–124. https://doi.org/10.1159/000362680
Wolff HA, Conradi LC, Beissbarth T, Leha A, Hohenberger W, Merkel S, Fietkau R, Raab HR, Tschmelitsch J, Hess CF, Becker H, Wittekind C, Sauer R, Rodel C, Liersch T, German Rectal Cancer Study G (2013) Gender affects acute organ toxicity during radiochemotherapy for rectal cancer: long-term results of the German CAO/ARO/AIO-94 phase III trial. Radiother Oncol 108(1):48–54. https://doi.org/10.1016/j.radonc.2013.05.009
Katzenstein J, Steinert R, Ptok H, Otto R, Gastinger I, Lippert H, Meyer F (2018) Gender-specific differences of the early postoperative and oncosurgical long-term outcome in rectal cancer-data obtained in a prospective multicenter observational study. Chirurg 89(6):458–465. https://doi.org/10.1007/s00104-018-0634-1
Martling A, Granath F, Cedermark B, Johansson R, Holm T (2009) Gender differences in the treatment of rectal cancer: a population based study. Eur J Surg Oncol 35(4):427–433. https://doi.org/10.1016/j.ejso.2008.03.001
Glynne-Jones R, Wyrwicz L, Tiret E, Brown G, Rodel C, Cervantes A, Arnold D, Committee EG (2017) Rectal cancer: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 28(suppl_4):iv22–iv40. https://doi.org/10.1093/annonc/mdx224
Doyle DJ, Garmon EH (2019) American Society of Anesthesiologists Classification (ASA Class). In: StatPearls. Treasure Island (FL),
Ueno H, Mochizuki H, Akagi Y, Kusumi T, Yamada K, Ikegami M, Kawachi H, Kameoka S, Ohkura Y, Masaki T, Kushima R, Takahashi K, Ajioka Y, Hase K, Ochiai A, Wada R, Iwaya K, Shimazaki H, Nakamura T, Sugihara K (2012) Optimal colorectal cancer staging criteria in TNM classification. J Clin Oncol 30(13):1519–1526. https://doi.org/10.1200/JCO.2011.39.4692
Watanabe T, Itabashi M, Shimada Y, Tanaka S, Ito Y, Ajioka Y, Hamaguchi T, Hyodo I, Igarashi M, Ishida H, Ishihara S, Ishiguro M, Kanemitsu Y, Kokudo N, Muro K, Ochiai A, Oguchi M, Ohkura Y, Saito Y, Sakai Y, Ueno H, Yoshino T, Boku N, Fujimori T, Koinuma N, Morita T, Nishimura G, Sakata Y, Takahashi K, Tsuruta O, Yamaguchi T, Yoshida M, Yamaguchi N, Kotake K, Sugihara K, Japanese Society for Cancer of the C, Rectum (2015) Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2014 for treatment of colorectal cancer. Int J Clin Oncol 20(2):207–239. https://doi.org/10.1007/s10147-015-0801-z
Benson AB 3rd, Choti MA, Cohen AM, Doroshow JH, Fuchs C, Kiel K, Martin EW Jr, McGinn C, Petrelli NJ, Posey JA, Skibber JM, Venook A, Yeatman TJ, National Comprehensive Cancer N (2000) NCCN practice guidelines for colorectal cancer. Oncology 14(11A):203–212
Engstrom PF, Arnoletti JP, Benson AB 3rd, Chen YJ, Choti MA, Cooper HS, Covey A, Dilawari RA, Early DS, Enzinger PC, Fakih MG, Fleshman J Jr, Fuchs C, Grem JL, Kiel K, Knol JA, Leong LA, Lin E, Mulcahy MF, Rao S, Ryan DP, Saltz L, Shibata D, Skibber JM, Sofocleous C, Thomas J, Venook AP, Willett C, National Comprehensive Cancer N (2009) NCCN clinical practice guidelines in oncology: rectal cancer. J Natl Compr Cancer Netw 7(8):838–881
Huh JW, Kim YJ, Kim HR (2012) Distribution of lymph node metastases is an independent predictor of survival for sigmoid colon and rectal cancer. Ann Surg 255(1):70–78. https://doi.org/10.1097/SLA.0b013e31823785f6
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibanes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250(2):187–196. https://doi.org/10.1097/SLA.0b013e3181b13ca2
Zutshi M, Hull T, Shedda S, Lavery I, Hammel J (2013) Gender differences in mortality, quality of life and function after restorative procedures for rectal cancer. Color Dis 15(1):66–73. https://doi.org/10.1111/j.1463-1318.2012.03075.x
Yang Y, Wang G, He J, Ren S, Wu F, Zhang J, Wang F (2017) Gender differences in colorectal cancer survival: a meta-analysis. Int J Cancer 141(10):1942–1949. https://doi.org/10.1002/ijc.30827
White A, Ironmonger L, Steele RJC, Ormiston-Smith N, Crawford C, Seims A (2018) A review of sex-related differences in colorectal cancer incidence, screening uptake, routes to diagnosis, cancer stage and survival in the UK. BMC Cancer 18(1):906. https://doi.org/10.1186/s12885-018-4786-7
Berger MD, Yang D, Sunakawa Y, Zhang W, Ning Y, Matsusaka S, Okazaki S, Miyamoto Y, Suenaga M, Schirripa M, Lenz AM, Bohanes P, Barzi A, Figueiredo JC, Hanna DL, Lenz HJ (2016) Impact of sex, age, and ethnicity/race on the survival of patients with rectal cancer in the United States from 1988 to 2012. Oncotarget 7(33):53668–53678. https://doi.org/10.18632/oncotarget.10696
Hussain A, Mahmood F, Torrance ADW, Clarke H, Howitt C, Dawson R (2018) Oncological outcomes of abdominoperineal resection for the treatment of low rectal cancer: a retrospective review of a single UK tertiary centre experience. Ann Med Surg (Lond) 34:28–33. https://doi.org/10.1016/j.amsu.2018.06.007
Habr-Gama A, Sao Juliao GP, Mattacheo A, de Campos-Lobato LF, Aleman E, Vailati BB, Gama-Rodrigues J, Perez RO (2017) Extralevator abdominal perineal excision versus standard abdominal perineal excision: impact on quality of the resected specimen and postoperative morbidity. World J Surg 41(8):2160–2167. https://doi.org/10.1007/s00268-017-3963-1
Seshadri RA, West NP, Sundersingh S (2017) A pilot randomized study comparing extralevator with conventional abdominoperineal excision for low rectal cancer after neoadjuvant chemoradiation. Color Dis 19(7):O253–O262. https://doi.org/10.1111/codi.13726
Peacock O, Waters PS, Bressel M, Lynch AC, Wakeman C, Eglinton T, Koh CE, Lee PJ, Austin KK, Warrier SK, Solomon MJ, Frizelle FA, Heriot AG (2019) Prognostic factors and patterns of failure after surgery for T4 rectal cancer in the beyond total mesorectal excision era. Br J Surg 106(12):1685–1696. https://doi.org/10.1002/bjs.11242
Ozawa H, Kotake K, Hosaka M, Hirata A, Sugihara K (2016) Impact of lateral pelvic lymph node dissection on the survival of patients with T3 and T4 low rectal cancer. World J Surg 40(6):1492–1499. https://doi.org/10.1007/s00268-016-3444-y
Martijnse IS, Dudink RL, Kusters M, Vermeer TA, West NP, Nieuwenhuijzen GA, van Lijnschoten I, Martijn H, Creemers GJ, Lemmens VE, van de Velde CJ, Sebag-Montefiore D, Glynne-Jones R, Quirke P, Rutten HJ (2012) T3+ and T4 rectal cancer patients seem to benefit from the addition of oxaliplatin to the neoadjuvant chemoradiation regimen. Ann Surg Oncol 19(2):392–401. https://doi.org/10.1245/s10434-011-1955-1
Freischlag K, Sun Z, Adam MA, Kim J, Palta M, Czito BG, Migaly J, Mantyh CR (2017) Association between incomplete neoadjuvant radiotherapy and survival for patients with locally advanced rectal cancer. JAMA Surg 152(6):558–564. https://doi.org/10.1001/jamasurg.2017.0010
Funding
This work was supported by the research project of the Sichuan Medical Association and the Health Commission of Sichuan Province of China (No. 20PJYY1734).
Author information
Authors and Affiliations
Contributions
BF and DZG conceived and supervised the study; DZG designed experiments; XCH and LGQ performed experiments; ZX and LW analyzed data; BF and SJY wrote the manuscript; WD and XYJB made manuscript revisions. All authors reviewed the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that they have no conflict of interest.
Ethics approval
This retrospective study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The Human Investigation Committee (IRB) of Mianyang Central Hospital approved this study.
Consent to participate
The need for individual consent was waived by the committee.
Consent for publication
Not applicable.
Code availability
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bao, F., Shang, J., Xiang, C. et al. Gender aspects of survival after abdominoperineal resection for low rectal cancer: a retrospective study. Int J Colorectal Dis 35, 2001–2010 (2020). https://doi.org/10.1007/s00384-020-03671-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-020-03671-2