Abstract
Background
Some patients with uncomplicated diverticulitis have extraluminal air. Our objective was to determine if patients with Hinchey 1a diverticulitis and isolated extraluminal air present more severe episode than patients without extraluminal air.
Methods
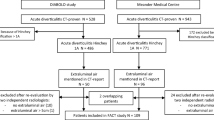
The present study is a monocentric observational retrospective cohort study. Computed tomographies of patients with diagnosed uncomplicated diverticulitis were retrospectively reviewed from the 01 January 2005 to the 31 December 2009. The presence of extraluminal air was determined. Leukocyte count, CRP value, and length of hospitalization were extracted from the patients’ files. The follow-up period was from the time of diagnosis to the 15th of March 2019, the latest. Follow-up was censored for death and sigmoidectomy. Recurrence and emergency sigmoidectomy were documented during the follow-up period. The study was performed according to the STROBE guideline.
Results
Three hundred and one patients with an episode of Hinchey 1a diverticulitis were included. Extraluminal air was present in 56 patients (18.60%). Leukocyte count (12.4 ± 4.1(G/l) versus 10.7 ± 3.5(G/l), p = 0.05), CRP value (156.9 ± 95.1(mg/l) versus 89.9 ± 74.8(mg/l), p < 0.001), and length of hospital stay (10.9 ± 5.5(days) versus 8.4 ± 3.6(days), p < 0.001) were significantly higher in patients with extraluminal air than in patients without extraluminal air. Seventy-two patients (23.92%) presented a recurrence during the follow-up period. Survival estimates did not differ between patients with or without extraluminal air (p = 0.717). Eleven patients (3.65%) required emergency surgery during the follow-up period. Patients with extraluminal air had shorter emergency surgery-free survival than patients without extraluminal air (p < 0.05).
Conclusion
The presence of extraluminal air in Hinchey 1a diverticulitis indicates a more severe episode, with higher inflammation parameters at admission, longer length of stay, and an increased risk for emergency sigmoidectomy.



Similar content being viewed by others
References
Parks T (1975) Natural history of diverticular disease of the colon. Clin Gastroenterol 4:53–69
Hughes LE (1969) Postmortem survey of diverticular disease of the colon. I. Diverticulosis and diverticulitis. Gut 10:336–344
Reddy VB, Longo WE (2013) The burden of diverticular disease on patients and healthcare systems. Gastroenterol Hepatol (N Y) 9:21–27
Schoetz DJ Jr (1999) Diverticular disease of the colon: a century-old problem. Dis Colon Rectum 42:703–709
Parks T (1969) Natural history of diverticular disease of the colon. A review of 521 cases. Br Med J 4:639–642
Klarenbeek BR, de Korte N, van der Peet DL, Cuesta MA (2012) Review of current classifications for diverticular disease and a translation into clinical practice. Int J Color Dis 27:207–214
Feingold D, Steele SR, Lee S, Kaiser A, Boushey R, Buie WD, Rafferty JF (2014) Practice parameters for the treatment of sigmoid diverticulitis. Dis Colon Rectum 57:284–294
Wasvary H, Turfah F, Kadro O et al (1999) Same hospitalization resection for acute diverticulitis. Am Surg 65:632–635 discussion 636
Neff CC, vanSonnenberg E (1989) CT of diverticulitis. Diagnosis and treatment. Radiol Clin N Am 27:743–752
Kaiser AM, Jiang JK, Lake JP, Ault G, Artinyan A, Gonzalez-Ruiz C, Essani R, Beart RW Jr (2005) The management of complicated diverticulitis and the role of computed tomography. Am J Gastroenterol 100:910–917
Nally DM, Kavanagh DO (2019) Current controversies in the management of diverticulitis: a review. Dig Surg 36:195–205
STATA (2013) Version 13. StataCorp LP, College Station, USA
Dharmarajan S, Hunt SR, Birnbaum EH, Fleshman JW, Mutch MG (2011) The efficacy of nonoperative management of acute complicated diverticulitis. Dis Colon Rectum 54:663–671
Bolkenstein HE, van de Wall BJM, Consten ECJ, Broeders IAMJ, Draaisma WA (2017) Risk factors for complicated diverticulitis: systematic review and meta-analysis. Int J Color Dis 32:1375–1383
Garcia-Gomez MA, Belmonte-Montes C, Cosme-Reyes C et al (2017) Prognostic value of the presence of pericolic air bubbles detected by computed tomography in acute diverticulitis. Cir Cir 85:471–477
Bolkenstein HE, van Dijk ST, Consten ECJ, Heggelman BGF, Hoeks CMA, Broeders IAMJ, Boermeester MA, Draaisma WA (2019) Conservative treatment in diverticulitis patients with pericolic extraluminal air and the role of antibiotic treatment. J Gastrointest Surg [Epub ahead of print]
Mora Lopez L, Serra Pla S, Serra-Aracil X, Ballesteros E, Navarro S (2013) Application of a modified Neff classification to patients with uncomplicated diverticulitis. Color Dis 15:1442–1447
Sallinen V, Mali J, Leppaniemi A et al (2015) Assessment of risk for recurrent diverticulitis: a proposal of risk score for complicated recurrence. Medicine (Baltimore) 94:e557
El-Sayed C, Radley S, Mytton J et al (2018) Risk of recurrent disease and surgery following an admission for acute diverticulitis. Dis Colon Rectum 61:382–389
Hupfeld L, Burcharth J, Pommergaard HC, Rosenberg J (2017) Risk factors for recurrence after acute colonic diverticulitis: a systematic review. Int J Color Dis 32:611–622
Buchs NC, Mortensen NJ, Ris F, Morel P, Gervaz P (2015) Natural history of uncomplicated sigmoid diverticulitis. World J Gastrointest Surg 7:313–318
Author information
Authors and Affiliations
Contributions
JM, NCB, and PAP conceived and designed the study. JM and AC acquired the data. JM and ER analyzed the data. JM, AC, ER, AB, CT, PAP, FR, and NCB interpreted the data. JM, AC, ER, AB, CT, PAP, FR, and NCB contributed to the writing of the manuscript and to its critical revision. JM, AC, ER, AB, CT, PAP, FR, and NCB approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors disclose no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOC 79 kb)
Rights and permissions
About this article
Cite this article
Meyer, J., Caruso, A., Roos, E. et al. The clinical significance of extraluminal air in Hinchey 1a diverticulitis: results from a retrospective cohort study with 10-year follow-up. Int J Colorectal Dis 34, 2053–2058 (2019). https://doi.org/10.1007/s00384-019-03424-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-019-03424-w