Abstract
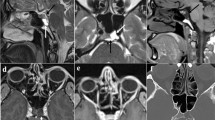
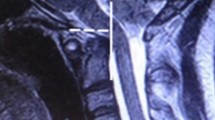
Autosomal dominantly inherited neurofibromatosis type I (NF1) is a systemic disorder caused by a mutation of a gene on chromosome 17q11.2 and characterized by multiple café-au-lait spots, lentiginous macules, Lisch nodules of the iris, and tumors of the nervous system. Bony manifestations such as scoliosis, dysplasia of the greater sphenoidal wing, tibial pseudoarthrosis, short stature, and macrocephaly have been reported in approximately 50% of patients. However, calvarial bone defects are rare. After screening 324 articles, 23 cases (12 adult and 11 pediatric patients) of occipital bone defects in NF1 patients were selected. All patients had a single/multiple bone defect over the lambdoid suture. Adjacent benign plexiform neurofibromas were observed in 14 patients (60.8%, 7 adults and 7 children); one adult patient was diagnosed with neurofibrosarcoma. Meningoencephalocele over the occipital defect was noted in 8 cases (34.78%, all adults). Cranioplasty was performed in only 17.39% of patients. Histologic examination was performed in 7 of the 15 patients with associated neurofibromas/neurofibrosarcomas. Biopsy of the bone margins surrounding the defect was performed in only one case. Pathologic examination of the herniated parieto-occipital or cerebellar tissue was not performed in any of the patients studied. We report the case of a 9-year-old girl with NF1 and a significant occipital bone defect and performed a systematic review of the relevant literature to highlight the challenges in treating this condition and to investigate the underlying mechanisms contributing to bone defects or dysplasia in NF1.






Similar content being viewed by others
Data availability
All data supporting the results of this study are available on the PubMed website.
References
Urimoto MAK, Irashima YUH, Ayashi NAH (1999) Suboccipital meningocele presenting as a huge retropharyngeal mass in a patient with neurofibromatosis Type 1:503–505
Antônio JR, Goloni-Bertollo EM, Trídico LA (2013) Neurofibromatose: Histórico cronológico e aspectos atuais. An Bras Dermatol 88. https://doi.org/10.1590/abd1806-4841.20132125
Rangarajan V, Mahore A, Patil M et al (2015) Brain herniation in neurofibromatosis with dysplasia of occipital bone and posterior skull base. Case Rep Neurol Med 2015. https://doi.org/10.1155/2015/816079
Năstase F, Radaschin D, Niculeț E et al (2021) Orthopaedic manifestations of neurofibromatosis type 1: a case report. Exp Ther Med 23. https://doi.org/10.3892/etm.2021.11058
Hernandez MALU, Pascual JS, Chan KI et al (2022) Rare neuroimaging findings in an adult neurofibromatosis type 1 patient. Can J Neurol Sci 49
Hamano T, Mutoh T, Naiki H et al (2019) Subventricular glial nodules in neurofibromatosis 1 with craniofacial dysmorphism and occipital meningoencephalocele. eNeurologicalSci 17. https://doi.org/10.1016/j.ensci.2019.100213
Kankane V, Jaiswal G, Gupta T (2016) Congenital extra calvarial plexiform neurofibroma in occipito-cervical region with occipital bone defect with neurofibromatosis type 1 and segmental neurofibromatosis: case report and review of literature. J Pediatr Neurosci 11
Solanki C, Ramachandran S, Devi BI, Sharma R (2015) Calvarial defects in the region of the lambdoid suture in neurofibromatosis type-1 patients. J Pediatr Neurosci 10. https://doi.org/10.4103/1817-1745.154322
Yoshida Y, Shindo M, Yamamoto O (2011) Occipital bone dysplasia associated with diffuse plexiform neurofibroma. Eur J Dermatol 21
Mislow JMK, Proctor MR, McNeely PD et al (2007) Calvarial defects associated with neurofibromatosis type 1: report of two cases. J Neurosurg 106
Bodhey NK, Gupta AK (2006) Neurofibromatosis type I with occipital encephalocele [2]. Neurol India 54
Renshaw A, Borsetti M, Nelson RJ, Orlando A (2003) Massive plexiform neurofibroma with associated meningo-encephalocoele and occipital bone defect presenting as a cervical mass. Br J Plast Surg 56. https://doi.org/10.1016/S0007-1226(03)00151-6
Kurimoto M, Hirashima Y, Hayashi N et al (1999) Suboccipital meningocele presenting as a huge retropharyngeal mass in a patient with neurofibromatosis Type 1. J Neurosurg 91. https://doi.org/10.3171/jns.1999.91.3.0503
Mann H, Kozic Z, Medinilla OR (1983) Computed tomography of lambdoid calvarial defect in neurofibromatosis - a case report. Neuroradiology 25. https://doi.org/10.1007/BF00455739
Maroun FB, Jacob JC, Markesteyn PH, Mercer DR (1969) Congenital venous malformation of the scalp associated with plexiform neurofibroma and cranial defect. Case report. J Neurosurg 31. https://doi.org/10.3171/jns.1969.31.4.0465
Saha MM, Agarwal KN, Bhardwaj OP (1969) Calvarial bone defects in neurofibromatosis. Am J Roentgenol Radium Ther Nucl Med 105. https://doi.org/10.2214/ajr.105.2.319
Davidson KC (1966) Cranial and intracranial lesions in neurofibromatosis. Am J Roentgenol Radium Ther Nucl Med 98. https://doi.org/10.2214/ajr.98.3.550
JOFFE N (1965) Calcarial bone defects involving the lambdoid suture in neurofibromatosis. Br J Radiol 38. https://doi.org/10.1259/0007-1285-38-445-23
Arrington DK, Danehy AR, Peleggi A et al (2013) Calvarial defects and skeletal dysplasia in patients with neurofibromatosis type 1: clinical article. J Neurosurg Pediatr 11. https://doi.org/10.3171/2013.1.PEDS12409
Friedrich RE, Emami P, Hagel C et al (2018) Repair of occipital bone defects in neurofibromatosis type 1 by means of CAD/CAM prefabricated titanium plates. Craniomaxillofac Trauma Reconstr 11. https://doi.org/10.1055/s-0037-1608699
Kurimoto M, Mizumaki Y, Fukuda O et al (2008) Giant plexiform neurofibroma and suboccipital meningocele manifesting as segmental neurofibromatosis - case report. Neurol Med Chir (Tokyo) 48. https://doi.org/10.2176/nmc.48.271
Hunt JC, Pugh DG (1961) Skeletal lesions in neurofibromatosis. Radiology 76. https://doi.org/10.1148/76.1.1
Kaufman B, Yonas H, White RJ, Miller CF (1979) Acquired middle cranial fossa fistulas: normal pressure and nontraumatic in origin. Neurosurgery 5. https://doi.org/10.1227/00006123-197910000-00011
Ogle RC, Tholpady SS, McGlynn KA, Ogle RA (2004) Regulation of cranial suture morphogenesis. In: Cells Tissues Organs
Kaspiris A, Savvidou OD, Vasiliadis ES et al (2022) Current aspects on the pathophysiology of bone metabolic defects during progression of scoliosis in neurofibromatosis type 1. J Clin Med 11
Stevenson DA, Yan J, He Y et al (2011) Multiple increased osteoclast functions in individuals with neurofibromatosis type 1. Am J Med Genet A 155. https://doi.org/10.1002/ajmg.a.33965
Sharma R, Wu X, Rhodes SD et al (2013) Hyperactive Ras/MAPK signaling is critical for tibial nonunion fracture in neurobromin-decient mice. Hum Mol Genet 22. https://doi.org/10.1093/hmg/ddt333
Ono K, Karolak MR, de la Croix Ndong J et al (2013) The Ras-GTPase activity of neurofibromin restrains ERK-dependent FGFR signaling during endochondral bone formation. Hum Mol Genet 22. https://doi.org/10.1093/hmg/ddt162
Legius E, Messiaen L, Wolkenstein P et al (2021) Revised diagnostic criteria for neurofibromatosis type 1 and Legius syndrome: an international consensus recommendation. Genet Med 23. https://doi.org/10.1038/s41436-021-01170-5
Ly KI, Blakeley JO (2019) The diagnosis and management of neurofibromatosis type 1. Med Clin North Am 103
Gutmann DH, Ferner RE, Listernick RH et al (2017) Neurofibromatosis type 1. Nat Rev Dis Primers 3:17004. https://doi.org/10.1038/nrdp.2017.4
Hirbe AC, Gutmann DH (2014) Neurofibromatosis type 1: a multidisciplinary approach to care. Lancet Neurol 13
Lam S, Kuether J, Fong A, Reid R (2015) Cranioplasty for large-sized calvarial defects in the pediatric population: a review. Craniomaxillofac Trauma Reconstr 8. https://doi.org/10.1055/s-0034-1395880
Frassanito P, Massimi L, Tamburrini G et al (2018) Custom-made hydroxyapatite for cranial repair in a specific pediatric age group (7–13 years old): a multicenter post-marketing surveillance study. Child’s Nervous System 34. https://doi.org/10.1007/s00381-018-3905-8
Kahen EJ, Brohl A, Yu D et al (2018) Neurofibromin level directs RAS pathway signaling and mediates sensitivity to targeted agents in malignant peripheral nerve sheath tumors. Oncotarget 9. https://doi.org/10.18632/oncotarget.25181
Ferrara UP, Tortora C, Rosano C et al (2022) Bone metabolism in patients with type 1 neurofibromatosis: key role of sun exposure and physical activity. Sci Rep 12. https://doi.org/10.1038/s41598-022-07855-4
Acknowledgements
The authors have nothing to declare.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by AA, FV and AR. Surgery was performed by GP and AC. Histopathological examination was conducted by GG. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No potential conflict of interest was reported by the author(s).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Alice Antico and Francesca Vitulli share joint first authorship.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Antico, A., Vitulli, F., Rossi, A. et al. Pathogenesis and treatment of a giant occipital bone defect with meningoencephalocele in an NF1 child: case report and review of the literature. Childs Nerv Syst 40, 27–39 (2024). https://doi.org/10.1007/s00381-023-06232-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-023-06232-4