Abstract
Background
Atlanto-occipital dislocation (AOD) is a rare but severe sequela of high energy trauma. Children are at increased risk, due to their immature spine and biomechanical characteristics.
Literature review
The prevailing mechanism of injury is motor vehicle collision as passenger. AOD commonly presents with cardiorespiratory arrest, spinal cord injury or cranial nerve deficits. Concomitant injuries, such as traumatic brain injury, are frequently encountered. Diagnosis is made on CT and MRI imaging. Posterior internal fixation is the recommended treatment. Thirty-four percent of patients die, 41 % survive with deficits and 25 % have a complete neurological recovery. Initial symptoms, GCS score and degree of spinal cord injury appear to be predictors of outcome.
Illustrative case
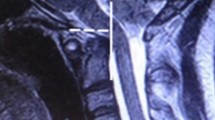
We report the case of a 9-year-old boy, who presented in extremis with cardiac arrest after a motor vehicle collision. Upon successful resuscitation, diagnostic imaging showed AOD and a Chiari I malformation. An occiput-C2 posterior instrumented fusion was performed. The patient subsequently received intensive rehabilitation and recovered to independent ambulation, with a persistent, asymptomatic Chiari I malformation.
Conclusion
This case highlights the potential for positive outcome in paediatric AOD, despite the presence of strong predictors of poor or fatal outcome at presentation.




Similar content being viewed by others
References
Davis D, Bohlman H, Walker a E et al (1971) The pathological findings in fatal craniospinal injuries. J Neurosurg 34:603–613. doi:10.3171/jns.1971.34.5.0603
Adams VI (1992) Neck injuries: I. Occipitoatlantal dislocation—a pathologic study of twelve traffic fatalities. J Forensic Sci 37:556–564
Menezes AH, Traynelis VC (2008) Anatomy and biomechanics of normal craniovertebral junction (a) and biomechanics of stabilization (b). Childs Nerv Syst 24:1091–1100. doi:10.1007/s00381-008-0606-8
MacKenzie EJ, Rivara FP, Jurkovich GJ et al (2006) A national evaluation of the effect of trauma-center care on mortality. N Engl J Med 354:366–378. doi:10.1056/NEJMsa052049
Rudehill A, Bellander B-M, Weitzberg E et al (2002) Outcome of traumatic brain injuries in 1,508 patients: impact of prehospital care. J Neurotrauma 19:855–868. doi:10.1089/08977150260190447
Pang D, Nemzek WR, Zovickian J (2007) Atlanto-occipital dislocation: Part 1—normal occipital condyle-C 1 interval in 89 children. Neurosurgery 61:514–521. doi:10.1227/01.NEU.0000290897.77448.1F
Pang D, Nemzek WR, Zovickian J (2007) Atlanto-occipital dislocation—part 2: the clinical use of (occipital) condyle-C1 interval, comparison with other diagnostic methods, and the manifestation, management, and outcome of atlanto-occipital dislocation in children. Neurosurgery 61:995–1015. doi:10.1227/01.neu.0000303196.87672.78
Haque A, Price AV, Sklar FH et al (2009) Screw fixation of the upper cervical spine in the pediatric population. Clinical article J Neurosurg Pediatr 3:529–533. doi:10.3171/2009.2.PEDS08l149
Anderson RCE, Ragel BT, Mocco J et al (2007) Selection of a rigid internal fixation construct for stabilization at the craniovertebral junction in pediatric patients. J Neurosurg 107:36–42. doi:10.3171/PED-07/07/036
Tubbs RS, Hallock JD, Radcliff V et al (2011) Ligaments of the craniocervical junction. J Neurosurg Spine 14:697–709. doi:10.3171/2011.1.SPINE10612
Menezes AH (2008) Craniocervical developmental anatomy and its implications. Childs Nerv Syst 24:1109–1122. doi:10.1007/s00381-008-0600-1
Mortazavi M, Gore PA, Chang S et al (2011) Pediatric cervical spine injuries: a comprehensive review. Childs Nerv Syst 27:705–717. doi:10.1007/s00381-010-1342-4
Reid DC, Henderson R, Saboe L, Miller JD (1987) Etiology and clinical course of missed spine fractures. J Trauma 27:980–986
Deliganis AV, Baxter AB, Hanson JA et al (2000) Radiologic spectrum of craniocervical distraction injuries. Radiographics 20:S237–S250. doi:10.1148/radiographics.20.suppl_1.g00oc23s237
Theodore N, Aarabi B, Dhall SS et al (2013) The diagnosis and management of traumatic atlanto-occipital dislocation injuries. Neurosurgery 72:114–126. doi:10.1227/NEU.0b013e31827765e0
Traynelis VC, Marano GD, Dunker RO (1986) Traumatic atlanto-occipital dislocation. J Neurosurg 65:624–629. doi:10.1016/S0002-9610(02)01408-3
Pang D, Pollack IF (1989) Spinal cord injury without radiographic abnormality in children—the SCIWORA syndrome. J Trauma 29:654–664
Dolan EJ, Transfeldt EE, Tator CH et al (1980) The effect of spinal distraction on regional spinal cord blood flow in cats. J Neurosurg 53:756–764. doi:10.3171/jns.1980.53.6.0756
Davis JW, Phreaner DL, Hoyt DB, Mackersie RC (1993) The etiology of missed cervical spine injuries. J Trauma 34:342–346
Schultz KD, Petronio J, Haid RW et al (2000) Pediatric occipitocervical arthrodesis. A review of current options and early evaluation of rigid internal fixation techniques. Pediatr Neurosurg 33:169–181
Crostelli M, Mariani M, Mazza O, Ascani E (2009) Cervical fixation in the pediatric patient: our experience. Eur Spine J 18(Suppl 1):20–28. doi:10.1007/s00586-009-0980-2
Ahmed R, Traynelis VC, Menezes AH (2008) Fusions at the craniovertebral junction. Childs Nerv Syst 24:1209–1224. doi:10.1007/s00381-008-0607-7
Hwang SW, Gressot LV, Rangel-Castilla L et al (2012) Outcomes of instrumented fusion in the pediatric cervical spine. J Neurosurg Spine 17:397–409. doi:10.3171/2012.8.SPINE12770
Singhal A, Bowen-Roberts T, Steinbok P et al (2011) Natural history of untreated syringomyelia in pediatric patients. Neurosurg Focus 31:E13. doi:10.3171/2011.9.FOCUS11208
Schijman E, Steinbok P (2004) International survey on the management of Chiari I malformation and syringomyelia. Childs Nerv Syst 20:341–348. doi:10.1007/s00381-003-0882-2
Olivero WC, Dinh DH (1992) Chiari I malformation with traumatic syringomyelia and spontaneous resolution: case report and literature review. Neurosurgery 30:758–760
Sun JC, Steinbok P, Cochrane DD (2000) Spontaneous resolution and recurrence of a Chiari I malformation and associated syringomyelia. Case report J Neurosurg 92:207–210
Tachibana S, Iida H, Yada K (1992) Significance of positive Queckenstedt test in patients with syringomyelia associated with Arnold-Chiari malformations. J Neurosurg 76:67–71. doi:10.3171/jns.1992.76.1.0067
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Electronic supplementary material
ESM 1
(PDF 273 kb)
Rights and permissions
About this article
Cite this article
Beez, T., Brown, J. Traumatic atlanto-occipital dislocation in children—a case-based update on clinical characteristics, management and outcome. Childs Nerv Syst 33, 27–33 (2017). https://doi.org/10.1007/s00381-016-3265-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-016-3265-1