Abstract
Purpose
Part of the patients with pelvic organ prolapse but without symptoms of stress urinary incontinence (SUI) may demonstrate SUI after prolapse surgery (occult SUI), and no optimal preoperative screening method is currently available for it. The aim of this study was to estimate the value of the preoperative 1-h pad test with pessary insertion for predicting the need for a mid-urethral sling (MUS) following prolapse surgery.
Methods
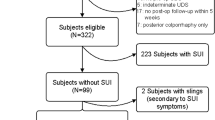
Two hundred and six patients were enrolled for advanced prolapse without complaining of urinary incontinence (UI) in this prospective cohort study. Exclusion criteria included prior or concomitant anti-incontinence surgery. Preoperatively, a stress test, the 1-h pad test and uroflowmetry were performed with prolapse reduction. Primary outcome was postoperative de novo UI. Median follow-up was 31 months (range 12–48 months).
Results
Of the 206 patients, 45 (21.8 %) had evidence of occult SUI preoperatively, 62 (30.1 %) exhibited de novo UI postoperatively, and only 13 (6.3 %) opted MUSs. Patients with occult SUI experienced higher de novo UI rate (53.3 vs. 23.6 %; P = 0.000). The OSUI and concomitant hysterectomy were identified as independent risk factors related to de novo UI (P = 0.000, P = 0.044). We performed receiver operating characteristic (ROC) curve analysis to evaluate the value of preoperative 1-h pad test. The area under ROC curve was 0.816 ± 0.085 (95 % CI 0.649–0.983); the cutoff value was 1.9 g (sensitivity 80.0 %, specificity 83.9 %).
Conclusions
The preoperative 1-h pad test with prolapse reduction is feasible for screening occult SUI, and more than 1.9 g may be a practical indicator of a postoperative subsequent MUS.

Similar content being viewed by others
References
Haylen BT, De Ridder D, Freeman RM et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J 21:5–26
Wein AJ (2012) Re: SUI surgery at the time of vaginal POP repair: is a surgical algorithm possible or desirable? J Urol 188:507–508
Long C-Y, Hsu S-C, Wu T-P et al (2004) Urodynamic comparison of continent and incontinent women with severe uterovaginal prolapse. J Reprod Med 49:33–37
Costantini E, Zucchi A, Giannantoni A et al (2007) Must colposuspension be associated with sacropexy to prevent postoperative urinary incontinence? Eur Urol 51:788–794
Visco AG, Brubaker L, Nygaard I et al (2008) The role of preoperative urodynamic testing in stress-continent women undergoing sacrocolpopexy: the colpopexy and urinary reduction efforts (CARE) randomized surgical trial. Int Urogynecol J 19:607–614
Bump RC, Mattiasson A, Bo K et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Abrams P, Blaivas JG, Stanton SL, Andersen JT (1988) The standardisation of terminology of lower urinary tract function. The International Continence Society Committee on Standardisation of Terminology. Scand J Urol Nephrol Suppl 114:5–19
Barber MD, Walters MD, Bump RC (2005) Short forms of two condition-specific quality-of-life questionnaires for women with pelvic floor disorders (PFDI-20 and PFIQ-7). Am J Obstet Gynecol 193:103–113
Zhu L, Yu S, Xu T et al (2011) Chinese validation of the Pelvic Floor Impact Questionnaire Short Form. Menopause 18:1030–1033
Doaee M, Moradi-Lakeh M, Nourmohammadi A et al (2014) Management of pelvic organ prolapse and quality of life: a systematic review and meta-analysis. Int Urogynecol J 25:153–163
Jundt K, Wagner S, von Bodungen V et al (2010) Occult incontinence in women with pelvic organ prolapse—does it matter? Eur J Med Res 15:112
Ennemoser S, Schönfeld M, von Bodungen V et al (2012) Clinical relevance of occult stress urinary incontinence (OSUI) following vaginal prolapse surgery: long-term follow-up. Int Urogynecol J 23:851–855
Smith TM, DeLancey JO, Fenner DE (2013) Post-reduction stress urinary incontinence rates in posterior versus anterior pelvic organ prolapse: a secondary analysis. Int Urogynecol J 24:1355–1360
Kudish BI, Shveiky D, Gutman RE et al (2014) Hysterectomy and urinary incontinence in postmenopausal women. Int Urogynecol J 25:1523–1531
Altman D, Granath F, Cnattingius S, Falconer C (2007) Hysterectomy and risk of stress-urinary-incontinence surgery: nationwide cohort study. Lancet 370:1494–1499
Sutherst JBM, Shawer M (1981) Assessing the severity of urinary incontinence in women by weighing perineal pads. Lancet 1:1128–1130
Chang TC, Hsiao SM, Chen CH et al (2014) Utilizing preoperative 20-min pad testing with vaginal gauze packing for indicating concomitant midurethral sling during cystocele repair. Eur J Obstet Gynecol Reprod Biol 172:127–130
Abrams P, Cardozo L, Fall M et al (2002) The standardisation of terminology of lower urinary tract function: report from the Standardisation Sub-committee of the International Continence Society. Am J Obstet Gynecol 187:116–126
Brubaker L, Cundiff GW, Fine P et al (2006) Abdominal sacrocolpopexy with Burch colposuspension to reduce urinary stress incontinence. N Engl J Med 354:1557–1566
Brubaker L, Nygaard I, Richter HE et al (2008) Two-year outcomes after sacrocolpopexy with and without Burch to prevent stress urinary incontinence. Obstet Gynecol 112:49
Acknowledgments
We are indebted to Dr. Tao Xu, who was consulted from the Department of Statistics, Peking Union Medical College Hospital, Chinese Academy of Medical Sciences, for help in the statistical analyses.
Conflict of interest
All authors declare that they have no conflicts of interest regarding a financial relationship with the organization that sponsored the research.
Ethical standard
This study has been approved by the Institutional review board ethics committee and has therefore been performed in accordance with the ethical standards outlined in the 1964 Declaration of Helsinki and its later amendments. All persons provided their informed consent prior to their inclusion in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Song, X., Zhu, L. & Ding, J. The value of the preoperative 1-h pad test with pessary insertion for predicting the need for a mid-urethral sling following pelvic prolapse surgery: a cohort study. World J Urol 34, 361–367 (2016). https://doi.org/10.1007/s00345-015-1590-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00345-015-1590-8