Abstract
Objectives
Aimed to develop a nomogram model based on deep learning features and radiomics features for the prediction of early hematoma expansion.
Methods
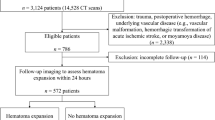
A total of 561 cases of spontaneous intracerebral hemorrhage (sICH) with baseline Noncontrast Computed Tomography (NCCT) were included. The metrics of hematoma detection were evaluated by Intersection over Union (IoU), Dice coefficient (Dice), and accuracy (ACC). The semantic features of sICH were judged by EfficientNet-B0 classification model. Radiomics analysis was performed based on the region of interest which was automatically segmented by deep learning. A combined model was constructed in order to predict the early expansion of hematoma using multivariate binary logistic regression, and a nomogram and calibration curve were drawn to verify its predictive efficacy by ROC analysis.
Results
The accuracy of hematoma detection by segmentation model was 98.2% for IoU greater than 0.6 and 76.5% for IoU greater than 0.8 in the training cohort. In the validation cohort, the accuracy was 86.6% for IoU greater than 0.6 and 70.0% for IoU greater than 0.8. The AUCs of the deep learning model to judge semantic features were 0.95 to 0.99 in the training cohort, while in the validation cohort, the values were 0.71 to 0.83. The deep learning radiomics model showed a better performance with higher AUC in training cohort (0.87), internal validation cohort (0.83), and external validation cohort (0.82) than either semantic features or Radscore.
Conclusion
The combined model based on deep learning features and radiomics features has certain efficiency for judging the risk grade of hematoma.
Clinical relevance statement
Our study revealed that the deep learning model can significantly improve the work efficiency of segmentation and semantic feature classification of spontaneous intracerebral hemorrhage. The combined model has a good prediction efficiency for early hematoma expansion.
Key Points
• We employ a deep learning algorithm to perform segmentation and semantic feature classification of spontaneous intracerebral hemorrhage and construct a prediction model for early hematoma expansion.
• The deep learning radiomics model shows a favorable performance for the prediction of early hematoma expansion.
• The combined model holds the potential to be used as a tool in judging the risk grade of hematoma.






Similar content being viewed by others
Abbreviations
- ACC:
-
Accuracy
- AHA/ASA:
-
American Heart Association/American Stroke Association
- AUC:
-
Area under the ROC curve
- CT:
-
Computed tomography
- CTA :
-
CT angiography
- FOV :
-
Field of view
- FPN :
-
Feature Pyramid Networks
- GCS:
-
Glasgow coma scale
- GLCM:
-
Gray level cooccurrence matrix
- GLRLM:
-
Gray level run length matrix
- GLSZM :
-
Gray level size zone matrix
- HE:
-
Hematoma expansion
- ICC:
-
Intraclass correlation coefficient
- IoU:
-
Intersection over Union
- LASSO:
-
Least Absolute Shrinkage and Selection Operator
- NCCT:
-
Noncontrast computed tomography
- PACS:
-
Picture Archiving and Communication System
- ROC:
-
Receiver operating characteristic curve
- ROI:
-
Region of interest
- sICH:
-
Spontaneous intracerebral hemorrhage
References
Keep RF, Hua Y, Xi G (2012) Intracerebral haemorrhage: mechanisms of injury and therapeutic targets. Lancet Neurol 11(8):720–731
Graeb DA, Robertson WD, Lapointe JS, Nugent RA, Harrison PB (1982) Computed tomographic diagnosis of intraventricular hemorrhage. Etiology and prognosis. Radiology 143(1):91-96
Joseph P, Broderick M, Thomas G, Brott M, John E, Duldner M (1993) Volume of intracerebral hemorrhage. A powerful and easy-to-use predictor of 30-day mortality. Stroke 24(6):1603-1622
Dowlatshahi D, Demchuk AM, Flaherty ML, Ali M, Lyden PL, Smith EE (2011) Defining hematoma expansion in intracerebral hemorrhage: relationship with patient outcomes. Neurology 76(14):1238–1244
Zhang D, Chen J, Guo J et al (2018) Hematoma heterogeneity on noncontrast computed tomography predicts intracerebral hematoma expansion: a meta-analysis. World Neurosurg 114:e663–e676
Li Q, Liu Q, Yang W et al (2017) Island sign an imaging predictor for early hematoma expansion and poor outcome in patients with intracerebral hemorrhage. Stroke 48(11):3019–3025
Yu Z, Zheng J, He M et al (2019) Accuracy of swirl sign for predicting hematoma enlargement in intracerebral hemorrhage: a meta-analysis. J Neurol Sci 399:155–160
Yu Z, Zheng J, Ma L et al (2017) The predictive accuracy of the black hole sign and the spot sign for hematoma expansion in patients with spontaneous intracerebral hemorrhage. Neurol Sci 38(9):1591–1597
Peng W, Reis C, Reis H, Zhang J, Yang J (2017) Predictive value of CTA spot sign on hematoma expansion in intracerebral hemorrhage patients. Biomed Res Int 2017:1–9
Li H, Xie Y, Liu H, Wang X (2022) Non-contrast CT-based radiomics score for predicting hematoma enlargement in spontaneous intracerebral hemorrhage. Clin Neuroradiol 32(2):517–528
Zhong J, Jin Y, Song Z et al (2021) Deep learning for automatically predicting early haematoma expansion in Chinese patients. Stroke and Vascular Neurology 6(4):610–614
Zhou Q, Zhu W, Li F, Yuan M, Zheng L, Liu X (2022) Transfer learning of the ResNet-18 and DenseNet-121 model used to diagnose intracranial hemorrhage in CT scanning. Curr Pharm Des 28(4):287
Lao J, Chen Y, Li Z et al (2017) A deep learning-based radiomics model for prediction of survival in glioblastoma multiforme. Sci Rep 7(1):10353
Liu Y, Fang Q, Jiang A, Meng Q, Pang G, Deng X (2021) Texture analysis based on U-Net neural network for intracranial hemorrhage identification predicts early enlargement. Comput Methods Programs Biomed 206:106140
Zheng X, Yao Z, Huang Y et al (2020) Deep learning radiomics can predict axillary lymph node status in early-stage breast cancer. Nat Commun 11(1):1236
Morotti A, Boulouis G, Dowlatshahi D et al (2019) Standards for detecting, interpreting, and reporting noncontrast computed tomographic markers of intracerebral hemorrhage expansion. Ann Neurol 86(4):480–492
Xu W, Tang W, Wu L et al (2022) Early prediction of cerebral computed tomography under intelligent segmentation algorithm combined with serological indexes for hematoma enlargement after intracerebral hemorrhage. Comput Math Methods Med 2022:1–8
Morgan T, Zuccarello M, Narayan R, Keyl P, Lane K, Hanley D (2008) Preliminary findings of the minimally-invasive surgery plus rtPA for intracerebral hemorrhage evacuation (MISTIE) clinical trial. Acta Neurochir Suppl 105:147–151
Newell DW, Shah MM, Wilcox R et al (2011) Minimally invasive evacuation of spontaneous intracerebral hemorrhage using sonothrombolysis. J Neurosurg 115(3):592–601
Butcher KS, Jeerakathil T, Hill M et al (2013) The intracerebral hemorrhage acutely decreasing arterial pressure trial. Stroke 44(3):620–626
Sporns PB, Schwake M, Schmidt R et al (2017) Computed tomographic blend sign is associated with computed tomographic angiography spot sign and predicts secondary neurological deterioration after intracerebral hemorrhage. Stroke 48(1):131–135
Strub WM, Leach JL, Tomsick T, Vagal A (2007) Overnight preliminary head CT interpretations provided by residents: locations of misidentified intracranial hemorrhage. Am J Neuroradiol 28(9):1679–1682
Xu W, Ding Z, Shan Y et al (2020) A nomogram model of radiomics and satellite sign number as imaging predictor for intracranial hematoma expansion. Front Neurosci 14:491
Chen Q, Xia T, Zhang M, Xia N, Liu J, Yang Y (2021) Radiomics in stroke neuroimaging: techniques, applications, and challenges. Aging Dis 12(1):143
Shen Q, Shan Y, Hu Z et al (2018) Quantitative parameters of CT texture analysis as potential markers for early prediction of spontaneous intracranial hemorrhage enlargement. Eur Radiol 28(10):4389–4396
Song Z, Guo D, Tang Z et al (2021) Noncontrast computed tomography-based radiomics analysis in discriminating early hematoma expansion after spontaneous intracerebral hemorrhage. Korean J Radiol 22(3):415
Heang-Ping Chan PD (2020) Deep learning in medical image analysis. Adv Exp Med Biol 1213:3–21
Rao BN, Mohanty S, Sen K, Acharya UR, Cheong KH, Sabut S (2022) Deep transfer learning for automatic prediction of hemorrhagic stroke on CT images. Comput Math Methods Med 2022:3560507
Tan M, Le Q (2019) EfficientNet: rethinking model scaling for convolutional neural networks. Proceedings of the 36th International Conference on Machine Learning, Long Beach, California, PMLR 6105–6114
Greenberg SM, Ziai WC, Cordonnier C et al (2022) 2022 Guideline for the management of patients with spontaneous intracerebral hemorrhage: a guideline from the American Heart Association/American Stroke Association. Stroke 53(7):e282–e361
Morotti A, Arba F, Boulouis G, Charidimou A (2020) Noncontrast CT markers of intracerebral hemorrhage expansion and poor outcome. Neurology 95(14):632–643
Fisher CM (1971) Pathological observations in hypertensive cerebral hemorrhage. J Neuropathol Exp Neurol 30(3):536–550
Wilkinson DA, Pandey AS, Thompson BG, Keep RF, Hua Y, Xi G (2018) Injury mechanisms in acute intracerebral hemorrhage. Neuropharmacology 134(Pt B):240–248
Le VH, Kha QH, Minh TNT, Nguyen VH, Le VL, Le NQK (2023) Development and Validation of CT-Based Radiomics Signature for Overall Survival Prediction in Multi-organ Cancer. J Digit Imaging 36(3):911–922
Lam LHT, Do DT, Diep DTN et al (2022) Molecular subtype classification of low-grade gliomas using magnetic resonance imaging-based radiomics and machine learning. NMR Biomed 35(11):e4792
Acknowledgements
This study was supported in part by Hangzhou Jianpei Technology Company Ltd. We would like to thank Yuzhen Xi from 903rd Hospital of PLA and Luoyu Wang from Hangzhou First People’s Hospital for the data collection and interpretation.
Qijun Shen contributed to the final manuscript and supervising all the data.
Funding
This study has received funding from the medical and health research project of Zhejiang province, China (No. 2023KY953).
This study has received funding from the medical and health research project of Zhejiang province, China (No. 2021KY240).
This study has received funding from the Science and Technology Project for the development of Hangzhou Biomedicine and Health, China (No. 2021WJCY028).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Qijun Shen.
Conflict of interest
One of the authors of this manuscript (Linyang He) is an employee of Hangzhou Jianpei Technology Company Ltd. The remaining authors declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Informed consent was waived by IRB. Written informed consent was not required for this study because of the retrospective nature of the study.
Ethical approval
Institutional Review Board approval was obtained. This study was approved by the Institutional Review Board (Medical Ethics Committee) of Hangzhou First People's Hospital and was conducted in accordance with relevant guidelines.
Study subjects or cohorts overlap
Study subjects or cohorts have not been previously reported.
Methodology
• retrospective
• diagnostic or prognostic study
• multicenter study
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Feng, C., Ding, Z., Lao, Q. et al. Prediction of early hematoma expansion of spontaneous intracerebral hemorrhage based on deep learning radiomics features of noncontrast computed tomography. Eur Radiol 34, 2908–2920 (2024). https://doi.org/10.1007/s00330-023-10410-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-10410-y