Abstract
Objectives
To calculate the pooled diagnostic performances of whole-body [18F]FDG PET/MR in M staging of [18F]FDG-avid cancer entities.
Methods
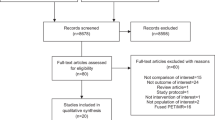
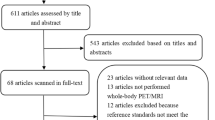
A diagnostic meta-analysis was conducted on the [18F]FDG PET/MR in M staging, including studies: (1) evaluated [18F]FDG PET/MR in detecting distant metastasis; (2) compared[ 18F]FDG PET/MR with histopathology, follow-up, or asynchronous multimodality imaging as the reference standard; (3) provided data for the whole-body evaluation; (4) provided adequate data to calculate the meta-analytic performances. Pooled performances were calculated with their confidence interval. In addition, forest plots, SROC curves, and likelihood ratio scatterplots were drawn. All analyses were performed using STATA 16.
Results
From 52 eligible studies, 2289 patients and 2072 metastases were entered in the meta-analysis. The whole-body pooled sensitivities were 0.95 (95%CI: 0.91–0.97) and 0.97 (95%CI: 0.91–0.99) at the patient and lesion levels, respectively. The pooled specificities were 0.99 (95%CI: 0.97–1.00) and 0.97 (95%CI: 0.90–0.99), respectively. Additionally, subgroup analyses were performed. The calculated pooled sensitivities for lung, gastrointestinal, breast, and gynecological cancers were 0.90, 0.93, 1.00, and 0.97, respectively. The pooled specificities were 1.00, 0.98, 0.97, and 1.00, respectively. Furthermore, the pooled sensitivities for non-small cell lung, colorectal, and cervical cancers were 0.92, 0.96, and 0.86, respectively. The pooled specificities were 1.00, 0.95, and 1.00, respectively.
Conclusion
[18F]FDG PET/MR was a highly accurate modality in M staging in the reported [18F]FDG-avid malignancies. The results showed high sensitivity and specificity in each reviewed malignancy type. Thus, our findings may help clinicians and patients to be confident about the performance of [18F]FDG PET/MR in the clinic.
Clinical relevance statement
Although [18F]FDG PET/MR is not a routine imaging technique in current guidelines, mostly due to its availability and logistic issues, our findings might add to the limited evidence regarding its performance, showing a sensitivity of 0.95 and specificity of 0.97.
Key Points
• The whole-body [18F]FDG PET/MR showed high accuracy in detecting distant metastases at both patient and lesion levels.
• The pooled sensitivities were 95% and 97% and pooled specificities were 99% and 97% at patient and lesion levels, respectively.
• The results suggested that 18F-FDG PET/MR was a strong modality in the exclusion and confirmation of distant metastases.






Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the curve
- CI:
-
Confidence interval
- CT:
-
Computed tomography
- DOR:
-
Diagnostic odds ratio
- FN:
-
False negative
- FP:
-
False positive
- LR:
-
Likelihood ratio
- MR:
-
Magnetic resonance imaging
- NSCLC:
-
Non-small cell lung cancer
- PET:
-
Positron emission tomography
- SROC:
-
Summary receiver-operating characteristic
- TN:
-
True negative
- TP:
-
True positive
References
Buchbender C, Heusner TA, Lauenstein TC, Bockisch A, Antoch G (2012) Oncologic PET/MRI, part 1: Tumors of the brain, head and neck, chest, abdomen, and pelvis. J Nucl Med 53:928–938
Chen LL, Blumm N, Christakis NA, Barabasi AL, Deisboeck TS (2009) Cancer metastasis networks and the prediction of progression patterns. Br J Cancer 101:749–758
Fares J, Fares MY, Khachfe HH, Salhab HA, Fares Y (2020) Molecular principles of metastasis: a hallmark of cancer revisited. Signal Transduct Target Ther 5:1–17
Fletcher JW, Djulbegovic B, Soares HP et al (2008) Recommendations on the use of 18F-FDG PET in oncology. J Nucl Med 49:480–508
Jadvar H, Alavi A, Gambhir SS (2009) 18F-FDG uptake in lung, breast, and colon cancers: Molecular biology correlates and disease characterization. J Nucl Med 50:1820–1827
Miles K, McQueen L, Ngai S, Law P (2015) Evidence-based medicine and clinical fluorodeoxyglucose PET/MRI in oncology. Cancer Imaging 15:1–8
Morsing A, Hildebrandt MG, Vilstrup MH (2019) Hybrid PET/MRI in major cancers: a scoping review. Eur J Nucl Med Mol Imaging 46:2138–2151
Weber W (2020) Clinical PET/MR. In: Schober O, Kiessling F, Debus J (eds) Molecular Imaging in Oncology. Recent Results in Cancer Research, vol 216. Springer, Cham. https://doi.org/10.1007/978-3-030-42618-7_22
Singnurkar A, Poon R, Metser U (2017) Comparison of 18F-FDG-PET/CT and 18F-FDG-PET/MR imaging in oncology: a systematic review. Ann Nucl Med 31:366–378
Seifert R, Kersting D, Rischpler C et al (2022) Clinical Use of PET/MR in Oncology: An Update. Semin Nucl Med 52:356–364
Salameh J, Bossuyt PM, McGrath TA, et al. (2020) Preferred reporting items for systematic review and metaanalysis of diagnostic test accuracy studies (PRISMA-DTA): explanation, elaboration, and checklist. BMJ 370:m2632. https://doi.org/10.1136/bmj.m2632
Deeks JJ, Higgins JP, Altman DG (2008) Analysing Data and Undertaking Meta-Analyses. In Cochrane Handbook for Systematic Reviews of Interventions (eds J.P. Higgins and S. Green). https://doi.org/10.1002/9780470712184.ch9
Dwamena B (2009) MIDAS: Stata module for meta-analytical integration of diagnostic test accuracy studies. https://EconPapers.repec.org/RePEc:boc:bocode:s456880
Harbord RM, Whiting P (2009) Metandi: meta-analysis of diagnostic accuracy using hierarchical logistic regression. Stata J 9:211–229
Beiderwellen K, Grueneisen J, Ruhlmann V et al (2015) [18F]FDG PET/MRI vs. PET/CT for whole-body staging in patients with recurrent malignancies of the female pelvis: initial results. Eur J Nucl Med Mol Imaging 42:56–65
Berzaczy D, Fueger B, Hoeller C et al (2020) Whole-Body [18F]FDG-PET/MRI vs. [18F]FDG-PET/CT in Malignant Melanoma. Mol Imaging Biol 22:739–744
Bian LH, Wang M, Gong J et al (2019) Comparison of integrated PET/MRI with PET/CT in evaluation of endometrial cancer: a retrospective analysis of 81 cases. PeerJ 7:e7081
Botsikas D, Bagetakos I, Picarra M et al (2019) What is the diagnostic performance of 18-FDG-PET/MR compared to PET/CT for the N- and M- staging of breast cancer? Eur Radiol 29:1787–1798
Brendle C, Schwenzer NF, Rempp H et al (2016) Assessment of metastatic colorectal cancer with hybrid imaging: comparison of reading performance using different combinations of anatomical and functional imaging techniques in PET/MRI and PET/CT in a short case series. Eur J Nucl Med Mol Imaging 43:123–132
Bruckmann NM, Sawicki LM, Kirchner J et al (2020) Prospective evaluation of whole-body MRI and 18F-FDG PET/MRI in N and M staging of primary breast cancer patients. Eur J Nucl Med Mol Imaging 47:2816–2825
Bruckmann NM, Kirchner J, Morawitz J, et al. (2021) Prospective comparison of CT and 18F-FDG PET/MRI in N and M staging of primary breast cancer patients: Initial results. PLoS One 16: e0260804. https://doi.org/10.1371/journal.pone.0260804
Catalano OA, Daye D, Signore A et al (2017) Staging performance of whole-body DWI, PET/CT and PET/MRI in invasive ductal carcinoma of the breast. Int J Oncol 51:281–288
Catalano OA, Coutinho AM, Sahani DV (2017) Colorectal cancer staging: comparison of whole-body PET/CT and PET/MR. Abdom Radiol (NY) 42:1141–1151
Ferrone C, Goyal L, Qadan M et al (2020) Management implications of fluorodeoxyglucose positron emission tomography/magnetic resonance in untreated intrahepatic cholangiocarcinoma. Eur J Nucl Med Mol Imaging 47:1871–1884
Fraioli F, Screaton NJ, Janes SM et al (2015) Non-small-cell lung cancer resectability: diagnostic value of PET/MR. Eur J Nucl Med Mol Imaging 42:49–55
Grueneisen J, Beiderwellen K, Heusch P et al (2014) Simultaneous Positron Emission Tomography/Magnetic Resonance Imaging for Whole-Body Staging in Patients With Recurrent Gynecological Malignancies of the Pelvis A Comparison to Whole-Body Magnetic Resonance Imaging Alone. Invest Radiol 49:808–815
Grueneisen J, Schaarschmidt BM, Beiderwellen K et al (2014) Diagnostic value of diffusion-weighted imaging in simultaneous 18F-FDG PET/MR imaging for whole-body staging of women with pelvic malignancies. J Nucl Med 55:1930–1935
Grueneisen J, Schaarschmidt BM, Heubner M et al (2015) Integrated PET/MRI for whole-body staging of patients with primary cervical cancer: preliminary results. Eur J Nucl Med Mol Imaging 42:1814–1824
Heusch P, Nensa F, Schaarschmidt B et al (2015) Diagnostic accuracy of whole-body PET/MRI and whole-body PET/CT for TNM staging in oncology. Eur J Nucl Med Mol Imaging 42:42–48
Huellner MW, de Galiza BF, Husmann L et al (2016) TNM Staging of Non-Small Cell Lung Cancer: Comparison of PET/MR and PET/CT. J Nucl Med 57:21–26
Joo I, Lee JM, Lee DH et al (2017) Preoperative assessment of pancreatic cancer with FDG PET/MR imaging versus FDG PET/CT plus contrast-enhanced multidetector CT: A prospective preliminary study. Radiology 282:149–159
Kirchner J, Sawicki LM, Deuschl C, et al (2017) 18 F-FDG PET/MR imaging in patients with suspected liver lesions: Value of liver-specific contrast agent Gadobenate dimeglumine. PLoS One 12:e0180349. https://doi.org/10.1371/journal.pone.0180349
Kirchner J, Martin O, Umutlu L, et al (2020) Impact of 18F-FDG PET/MR on therapeutic management in high risk primary breast cancer patients – A prospective evaluation of staging algorithms. Eur J Radiol 128:108975. https://doi.org/10.1016/j.ejrad.2020.108975
Klain M, Nappi C, Nicolai E et al (2020) Comparison of simultaneous 18F-2-[18F] FDG PET/MR and PET/CT in the follow-up of patients with differentiated thyroid cancer. Eur J Nucl Med Mol Imaging 47:3066–3073
Lee SJ, Seo HJ, Kang KW et al (2015) Clinical performance of whole-body 18F-FDG PET/Dixon-VIBE, T1-weighted, and T2-weighted MRI protocol in colorectal cancer. Clin Nucl Med 40:e392–e398
Lee DH, Kim SH, Joo I, Hur BY, Han JK (2016) Comparison between 18F-FDG PET/MRI and MDCT for the assessment of preoperative staging and resectability of gastric cancer. Eur J Radiol 85:1085–1091
Lee SM, Goo JM, Park CM et al (2016) Preoperative staging of non-small cell lung cancer: prospective comparison of PET/MR and PET/CT. Eur Radiol 26:3850–3857
Li CC, Chien TM, Huang SP et al (2020) 18 f-fdg pet/mr versus mr alone in whole-body primary staging and restaging of patients with rectal cancer: What is the benefit of pet? J Clin Med 9:1–11
Li H, Chen X, Zhang Y, Wang K, Gao Z (2021) Value of18f-fdg hybrid pet/mr in differentiated thyroid cancer patients with negative131i whole-body scan and elevated thyroglobulin levels. Cancer Manag Res 13:2869–2876
Yi Liu, Dong Zheng, Jia-jin Liu, et al. (2019) Comparing PET/MRI with PET/CT for pretreatment staging of gastric cancer. Gastroenterol Res Pract 9564627. https://doi.org/10.1155/2019/9564627
Melsaether AN, Raad RA, Pujara AC et al (2016) Comparison of Whole-Body F-18 FDG PET/MR Imaging and Whole-Body F-18 FDG PET/CT in Terms of Lesion Detection and Radiation Dose in Patients with Breast Cancer. Radiology 281:193–202
Mongula JE, Bakers FC, Vöö S et al (2018) Positron emission tomography-magnetic resonance imaging (PET-MRI) for response assessment after radiation therapy of cervical carcinoma: a pilot study. EJNMMI Res 8:1–8
Ohno Y, Koyama H, Yoshikawa T et al (2015) Three-way comparison of whole-body MR, coregistered whole-body FDG PET/MR, and integrated whole-body FDG PET/CT imaging: TNM and stage assessment capability for non-small cell lung cancer patients. Radiology 275:849–861
Ohno Y, Yoshikawa T, Kishida Y et al (2017) Diagnostic performance of different imaging modalities in the assessment of distant metastasis and local recurrence of tumor in patients with non-small cell lung cancer. J Magn Reson Imaging 46:1707–1717
Ohno Y, Yui M, Aoyagi K et al (2019) Whole-Body MRI: Comparison of its capability for TNM staging of malignant pleural mesothelioma with that of coregistered PET/MRI, Integrated FDG PET/CT, and conventional imaging. AJR Am J Roentgenol 212:311–319
Ohno Y, Takeshi Y, Takenaka D, Koyama H, Aoyagi K, Yui M (2020) Comparison of Diagnostic Accuracy for TNM Stage Among Whole-Body MRI and Coregistered PET/MRI Using 1.5-T and 3-T MRI Systems and Integrated PET/CT for Non-Small Cell Lung Cancer. AJR Am J Roentgenol 215:1191–1198
Ohno Y, Yoshikawa T, Takenaka D et al (2022) Small Cell Lung Cancer Staging: Prospective Comparison of Conventional Staging Tests, FDG PET/CT, Whole-Body MRI, and Coregistered FDG PET/MRI. AJR Am J Roentgenol 218:899–908
Piao Y, Cao C, Xu Y et al (2022) Detection and staging of recurrent or metastatic nasopharyngeal carcinoma in the era of FDG PET/MR. Eur Arch Otorhinolaryngol 279:353–359. https://doi.org/10.1007/s00405-021-06779-5
Platzek I, Beuthien-Baumann B, Schramm G et al (2017) FDG PET/MR in initial staging of sarcoma: Initial experience and comparison with conventional imaging. Clin Imaging 42:126–132
Pujara AC, Raad RA, Ponzo F et al (2016) Standardized uptake values from PET/MRI in metastatic breast cancer: An organ-based comparison with PET/CT. Breast J 22:264–273
Queiroz MA, Kubik-Huch RA, Hauser N et al (2015) PET/MRI and PET/CT in advanced gynaecological tumours: initial experience and comparison. Eur Radiol 25:2222–2230
Queiroz MA, Ortega CD, Ferreira FR, Nahas SC, Cerri GG, Buchpiguel CA (2021) Diagnostic accuracy of FDG-PET/MRI versus pelvic MRI and thoracic and abdominal CT for detecting synchronous distant metastases in rectal cancer patients. Eur J Nucl Med Mol Imaging 48:186–195
Ruhlmann V, Ruhlmann M, Bellendorf A et al (2016) Hybrid imaging for detection of carcinoma of unknown primary: A preliminary comparison trial of whole-body PET/MRI versus PET/CT. Eur J Radiol 85:1941–1947
Sarabhai T, Schaarschmidt BM, Wetter A et al (2018) Comparison of 18F-FDG PET/MRI and MRI for pre-therapeutic tumor staging of patients with primary cancer of the uterine cervix. Eur J Nucl Med Mol Imaging 45:67–76
Sawicki LM, Grueneisen J, Schaarschmidt BM et al (2016) Evaluation of 18F-FDG PET/MRI, 18F-FDG PET/CT, MRI, and CT in whole-body staging of recurrent breast cancer. Eur J Radiol 85:459–465
Sawicki LM, Kirchner J, Grueneisen J et al (2018) Comparison of 18F–FDG PET/MRI and MRI alone for whole-body staging and potential impact on therapeutic management of women with suspected recurrent pelvic cancer: a follow-up study. Eur J Nucl Med Mol Imaging 45:622–629
Sekine T, de Galiza BF, Kuhn FP et al (2017) PET plus MR versus PET/CT in the initial staging of head and neck cancer, using a trimodality PET/CT plus MR system. Clin Imaging 42:232–239
Sekine T, de Galiza BF, Sah BR et al (2017) PET/MR Outperforms PET/CT in Suspected Occult Tumors. Clin Nucl Med 42:E88–E95
Sharkey AR, Sah BR, Withey SJ et al (2021) Initial experience in staging primary oesophageal/gastro-oesophageal cancer with 18F-FDG PET/MRI. Eur J Hybrid Imaging 5:1–3
Steiner A, Narva S, Rinta-Kiikka I, Hietanen S, Hynninen J, Virtanen J (2021) Diagnostic efficiency of whole-body 18F-FDG PET/MRI, MRI alone, and SUV and ADC values in staging of primary uterine cervical cancer. Cancer Imaging 21:1–1
Taneja S, Jena A, Goel R, Sarin R, Kaul S (2014) Simultaneous whole-body 18F-FDG PET-MRI in primary staging of breast cancer: A pilot study. Eur J Radiol 83:2231–2239
Tsuyoshi H, Tsujikawa T, Yamada S, Okazawa H, Yoshida Y (2020) Diagnostic value of F-18 FDG PET/MRI for staging in patients with ovarian cancer. EJNMMI Res 10:1–4
Tsuyoshi H, Tsujikawa T, Yamada S, Okazawa H, Yoshida Y (2020) Diagnostic value of 18F-FDG PET/MRI for staging in patients with endometrial cancer. Cancer Imaging 20:1–9
Tsuyoshi H, Tsujikawa T, Yamada S, Okazawa H, Yoshida Y (2021) Diagnostic value of18f-fdg pet/mri for revised 2018 figo staging in patients with cervical cancer. Diagnostics 11:202
Vermersch M, Mulé S, Chalaye J et al (2021) Impact of the18f-fdg-pet/mri on metastatic staging in patients with hepatocellular carcinoma: Initial results from 104 patients. J Clin Med 10:4017
Yoon JH, Lee JM, Chang W et al (2020) Initial M staging of rectal cancer: FDG PET/MRI with a hepatocyte-specific contrast agent versus contrast-enhanced CT. Radiology 294:310–319
Matthew JP, Joanne EM, Patric MB et al (2021) The PRISMA 2020 statement: An updated guideline for reporting systematic reviews. Int J Surg 88:105906. https://doi.org/10.1016/j.ijsu.2021.105906
Sawicki LM, Kirchner J, Grueneisen J et al (2017) Whole-body staging of female patients with recurrent pelvic malignancies: Ultra-fast 18F-FDG PET/MRI compared to 18F-FDG PET/CT and CT. PLoS One 45:622–629
Shen G, Hu S, Liu B, Kuang A et al (2016) Diagnostic performance of whole-body PET/MRI for detecting malignancies in cancer patients: a meta-analysis. PLoS One 11:e0154497
Li J, Zhou H, Zhang X, Song F, Pang X, Wei Z (2020) A two-way comparison of whole-body 18FDG PET-CT and whole-body contrast-enhanced MRI for distant metastasis staging in patients with malignant tumors: a meta-analysis of 13 prospective studies. Ann Palliat Med 9:247–255
Sacks A, Peller PJ, Surasi DS, Chatburn L, Mercier G, Subramaniam RM (2011) Value of PET/CT in the Management of Liver Metastases, Part 1. AJR Am J Roentgenol 197:W256–W259
Qu X, Huang X, Yan W, Wu L, Dai K (2012) A meta-analysis of 18FDG-PET–CT, 18FDG-PET, MRI and bone scintigraphy for diagnosis of bone metastases in patients with lung cancer. Eur J Radiol 81:1007–1015
Ming Y, Wu N, Qian T et al (2020) Progress and Future Trends in PET/CT and PET/MRI Molecular Imaging Approaches for Breast Cancer. Front Oncol 10:1301
Evangelista L, Cuppari L, Burei M, Zorz A, Caumo F (2019) Head-to-head comparison between 18F-FDG PET/CT and PET/MRI in breast cancer. Clin Transl Imaging 7:99–104
Machado Medeiros T, Altmayer S, Watte G et al (2020) 18F-FDG PET/CT and whole-body MRI diagnostic performance in M staging for non–small cell lung cancer: a systematic review and meta-analysis. Eur Radiol 30:3641–3649
Czernin J, Benz MR, Allen-Auerbach MS (2010) PET/CT imaging: The incremental value of assessing the glucose metabolic phenotype and the structure of cancers in a single examination. Eur J Radiol 73:470–480
Detterbeck FC, Falen S, Rivera MP, Halle JS, Socinski MA (2004) Seeking a home for a PET, part 2: Defining the appropriate place for positron emission tomography imaging in the staging of patients with suspected lung cancer. Chest 125:2300–2308
Dahlsgaard-Wallenius SE, Hildebrandt MG, Johansen A et al (2021) Hybrid PET/MRI in non-small cell lung cancer (NSCLC) and lung nodules—a literature review. Eur J Nucl Med Mol Imaging 48:584–591
Whiteford MH, Whiteford HM, Yee LF et al (2000) Usefulness of FDG-PET scan in the assessment of suspected metastatic or recurrent adenocarcinoma of the colon and rectum. Dis Colon Rectum 43:759–767
Zhang Z, Zhou N, Guo X, Li N, Zhu H, Yang Z (2022) Pretherapeutic Assessment of Pancreatic Cancer: Comparison of FDG PET/CT Plus Delayed PET/MR and Contrast-Enhanced CT/MR. Front Oncol 11:5719
Crimi F, Valeggia S, Baffoni L et al (2021) [18F]FDG PET/MRI in rectal cancer. Ann Nucl Med 35:281–290
Kijima S, Sasaki T, Nagata K, Utano K, Lefor AT, Sugimoto H (2014) Preoperative evaluation of colorectal cancer using CT colonography, MRI, and PET/CT. World J Gastroenterol 20:16964
Tsili AC, Alexiou G, Naka C, Argyropoulou MI (2021) Imaging of colorectal cancer liver metastases using contrast-enhanced US, multidetector CT, MRI, and FDG PET/CT: a meta-analysis. Acta Radiol 62:302–312
Choi SH, Kim SY, Park SH (2018) Diagnostic performance of CT, gadoxetate disodium-enhanced MRI, and PET/CT for the diagnosis of colorectal liver metastasis: systematic review and meta-analysis. J Mag Reson Imaging 47:1237–1250
Mirshahvalad SA, Hinzpeter R, Kohan A et al (2022) Diagnostic performance of [18F]-FDG PET/MR in evaluating colorectal cancer: a systematic review and meta-analysis. Eur J Nucl Med Mol Imaging 49:4205–4217
Gassert FG, Rübenthaler J, Cyran CC et al (2021) 18F FDG PET/MRI with hepatocyte-specific contrast agent for M staging of rectal cancer: a primary economic evaluation. Eur J Nucl Med Mol Imaging 48:3268–3276
Pesapane F, Downey K, Rotili A, Cassano E, Koh DM (2020) Imaging diagnosis of metastatic breast cancer. Insights Imaging 11:1–4
Petralia G, Padhani AR, Pricolo P et al (2019) Whole-body magnetic resonance imaging (WB-MRI) in oncology: recommendations and key uses. Radiol Med 124:218–233
Virarkar M, Viswanathan C, Iyer R et al (2019) The Role of Positron Emission Tomography/Magnetic Resonance Imaging in Gynecological Malignancies. J Comput Assist Tomogr 43:825–834
Kang S, Kim SK, Chung DC et al (2010) Diagnostic value of 18F-FDG PET for evaluation of paraaortic nodal metastasis in patients with cervical carcinoma: a metaanalysis. J Nucl Med 51:360–367
Buchbender C, Heusner TA, Lauenstein TC, Bockisch A, Antoch G (2020) Performance of different imaging techniques for detection of para-aortic lymph node metastasis from gynecological malignancies: a systematic review and meta-analysis. Gynecol Obstet Invest 85:53–71
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Patrick Veit-Haibach.
Conflict of interest
The authors of this manuscript declare relationships with the following companies: Siemens Healthineers and POINT.
PVH received travel support and IIS grants from Siemens Healthineers in the last 3 years outside of this work. Ur Metser is an advisor for POINT.
Statistics and biometry
One of the authors (SAM) has significant statistical expertise.
Informed consent
Not applicable (meta-analytic study).
Ethical approval
Not applicable (meta-analytic study).
Study subjects or cohorts overlap
None.
Methodology
• Meta-analysis
• systematic review
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mirshahvalad, S.A., Kohan, A., Metser, U. et al. Diagnostic performance of whole-body [18F]FDG PET/MR in cancer M staging: A systematic review and meta-analysis. Eur Radiol 34, 673–685 (2024). https://doi.org/10.1007/s00330-023-10009-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-10009-3