Abstract
Objectives
Investigate sex differences in age-related back extensor muscle degeneration using Dixon MRI and analyze the relationship between quantitative muscle parameters and back muscle strength in healthy adults.
Methods
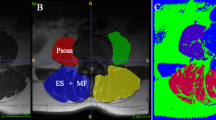
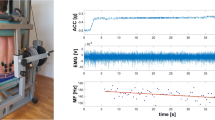
105 healthy subjects underwent lumbar Dixon MRI. Fat fraction (FF), cross-sectional area (CSA), functional CSA (FCSA), and relative FCSA (RFCSA) of multifidus muscle (MF) and erector spinae (ES) were quantified. Back extension muscle strength was measured using an external fixation dynamometer. ANOVA with post hoc Tukey correction was used for age group comparisons. Partial and Spearman’s correlation analyzed relationships between age, muscle parameters, and muscle strength.
Results
MF and ES FF significantly increased with age in both genders (r = 0.55–0.85; p < 0.001). Muscle FF increased prominently for females (40–49 years, MF and 50–59 years, ES) and males (60–73 years, MF and ES). In females, total ES FCSA and RFCSA (r = − 0.42, − 0.37; p < 0.01) correlated with age. While in males, all MF and ES muscle size parameters, except total MF CSA, correlated with age (r = − 0.30 to − 0.58; p < 0.05). Back extension muscle strength correlated with mean FF, total CSA, and total FCAS for MF and ES individually (p < 0.001). The combined MF + ES FCSA correlation coefficient (r = 0.63) was higher than FF (r = − 0.51) and CSA (r = 0.59) (p < 0.001).
Conclusions
Age-related back extensor muscle degeneration varies by muscle type and sex. FCSA has the highest association with back muscle strength compared to FF and CSA.
Clinical relevance statement
The investigation of sex differences in age-related back extensor muscle degeneration utilizing Dixon imaging may hold significant implications for evaluating spine health and enabling earlier intervention. Muscles’ FCSA could contribute to acquiring additional evidence for reflecting muscle function change.
Key Points
• The multifidus muscle (MF) and erector spinae (ES) fat fraction (FF) increased with age at all lumbar disc levels in females and males.
• Age-related changes in muscle morphological quantitative parameters of healthy adults were specific by muscle type and gender.
• The muscle functional cross-sectional area (FCSA) measured by Dixon imaging may better monitor back extensor muscle strength changes than muscle FF and cross-sectional area (CSA).





Similar content being viewed by others
Abbreviations
- BMI:
-
Body mass index
- CSA:
-
Cross-sectional area
- ES:
-
Erector spinae
- FCSA:
-
Functional cross-sectional area
- FF:
-
Fat fraction
- FI:
-
Fat infiltration
- MF:
-
Multifidus muscle
- MVIC:
-
Maximum voluntary isometric contraction
- RCSA:
-
Relative cross-sectional area
- RFCSA:
-
Relative functional cross-sectional area
- TSE:
-
Turbo spin echo
References
Kim DH, Park J, Lee CW, Lee SY (2022) Natural aging course of lumbar extensor muscle mass and strength in community-dwelling older women: a 1-year prospective observational study. Aging Clin Exp Res. https://doi.org/10.1007/s40520-022-02156-2
Dallaway A, Kite C, Griffen C et al (2020) Age-related degeneration of the lumbar paravertebral muscles: systematic review and three-level meta-regression. Exp Gerontol 133:110856
Crawford RJ, Cornwall J, Abbott R, Elliott JM (2017) Manually defining regions of interest when quantifying paravertebral muscles fatty infiltration from axial magnetic resonance imaging: a proposed method for the lumbar spine with anatomical cross-reference. BMC Musculoskelet Disord 18:25
Vives MJ (2016) The paraspinal muscles and their role in the maintenance of global spinal alignment. Another wrinkle in an already complex problem. Spine J 16:459–461
Kim WJ, Shin HM, Lee JS et al (2021) Sarcopenia and back muscle degeneration as risk factors for degenerative adult spinal deformity with sagittal imbalance and degenerative spinal disease: a comparative study. World Neurosurg 148:e547–e555
Sun XY, Kong C, Lu SB et al (2019) The parallelogram effect of degenerative structures around the apical vertebra in patients with adult degenerative scoliosis: the influence of asymmetric degeneration and diagonal degeneration on the severity of deformity. Med Sci Monit 25:3435–3445
Yeung KH, Man GCW, Shi L et al (2019) Magnetic resonance imaging-based morphological change of paraspinal muscles in girls with adolescent idiopathic scoliosis. Spine (Phila Pa 1976) 44:1356–1363
Federau C, Kroismayr D, Dyer L, Farshad M, Pfirrmann C (2020) Demonstration of asymmetric muscle perfusion of the back after exercise in patients with adolescent idiopathic scoliosis using intravoxel incoherent motion (IVIM) MRI. NMR Biomed 33:e4194
Dahlqvist JR, Vissing CR, Hedermann G, Thomsen C, Vissing J (2017) Fat replacement of paraspinal muscles with aging in healthy adults. Med Sci Sports Exerc 49:595–601
Wan M, Gray-Gaillard EF, Elisseeff JH (2021) Cellular senescence in musculoskeletal homeostasis, diseases, and regeneration. Bone Res 9:41
Kim JC, Lee SU, Jung SH, Lim JY, Kim DH, Lee SY (2019) Natural aging course of paraspinal muscle and back extensor strength in community-dwelling older adults (sarcopenia of spine, SarcoSpine): a prospective cohort study protocol. BMJ Open 9:e032443
Wilkinson DJ, Piasecki M, Atherton PJ (2018) The age-related loss of skeletal muscle mass and function: measurement and physiology of muscle fibre atrophy and muscle fibre loss in humans. Ageing Res Rev 47:123–132
Chamorro C, Arancibia M, Trigo B, Arias-Poblete L, Jerez-Mayorga D (2021) Absolute reliability and concurrent validity of hand-held dynamometry in shoulder rotator strength assessment: systematic review and meta-analysis. Int J Environ Res Public Health 18:9293
Valentin G, Maribo T (2014) Hand-held dynamometry fixated with a tripod is reliable for assessment of back extensor strength in women with osteoporosis. Osteoporos Int 25:2143–2149
Gassenmaier S, Kahm K, Walter SS, Machann J, Nikolaou K, Bongers MN (2021) Quantification of liver and muscular fat using contrast-enhanced dual source dual energy computed tomography compared to an established multi-echo Dixon MRI sequence. Eur J Radiol 142:109845
Kiefer LS, Fabian J, Lorbeer R et al (2018) Inter- and intra-observer variability of an anatomical landmark-based, manual segmentation method by MRI for the assessment of skeletal muscle fat content and area in subjects from the general population. Br J Radiol. https://doi.org/10.1259/bjr.20180019:20180019
Schlaeger S, Inhuber S, Rohrmeier A et al (2019) Association of paraspinal muscle water-fat MRI-based measurements with isometric strength measurements. Eur Radiol 29:599–608
Biltz NK, Collins KH, Shen KC, Schwartz K, Harris CA, Meyer GA (2020) Infiltration of intramuscular adipose tissue impairs skeletal muscle contraction. J Physiol 598:2669–2683
Klupp E, Cervantes B, Schlaeger S et al (2019) Paraspinal Muscle DTI Metrics Predict Muscle Strength. J Magn Reson Imaging 50:816–823
Kassiano W, Costa B, Nunes JP et al (2022) Muscular strength and skeletal muscle mass in 511 physically independent older women aged 60–88 years. Exp Gerontol 166:111867
Goubert D, De Pauw R, Meeus M et al (2017) Lumbar muscle structure and function in chronic versus recurrent low back pain: a cross-sectional study. Spine J 17:1285–1296
Yang S, Wu W, Zhang C et al (2020) Reliability and validity of three isometric back extensor strength assessments with different test postures. J Int Med Res 48:300060519885268
Gheller BJ, Riddle ES, Lem MR, Thalacker-Mercer AE (2016) Understanding age-related changes in skeletal muscle metabolism: differences between females and males. Annu Rev Nutr 36:129–156
Triolo M, Oliveira AN, Kumari R, Hood DA (2022) The influence of age, sex, and exercise on autophagy, mitophagy, and lysosome biogenesis in skeletal muscle. Skelet Muscle 12:13
Agostini D, Zeppa Donati S, Lucertini F et al (2018) Muscle and bone health in postmenopausal women: role of protein and vitamin D supplementation combined with exercise training. Nutrients 10:1103
Collins BC, Laakkonen EK, Lowe DA (2019) Aging of the musculoskeletal system: How the loss of estrogen impacts muscle strength. Bone 123:137–144
Chen Z, Li WY, Ho M, Chau PH (2021) The prevalence of sarcopenia in Chinese older adults: meta-analysis and meta-regression. Nutrients 13:1441
Martin BI, Mirza SK, Spina N, Spiker WR, Lawrence B, Brodke DS (2019) Trends in lumbar fusion procedure rates and associated hospital costs for degenerative spinal diseases in the United States, 2004 to 2015. Spine (Phila Pa 1976) 44:369–376
Crawford RJ, Filli L, Elliott JM et al (2016) Age- and level-dependence of fatty infiltration in lumbar paravertebral muscles of healthy volunteers. AJNR Am J Neuroradiol 37:742–748
Berry DB, Rodriguez-Soto AE, Englund EK et al (2020) Multiparametric MRI characterization of level dependent differences in lumbar muscle size, quality, and microstructure. JOR Spine 3:e1079
Lee SH, Park SW, Kim YB, Nam TK, Lee YS (2017) The fatty degeneration of lumbar paraspinal muscles on computed tomography scan according to age and disc level. Spine J 17:81–87
Li Y, Sun J, Wang G (2021) Lumbar lordosis morphology correlates to pelvic incidence and erector spinae muscularity. Sci Rep 11:802
Burian E, Syvari J, Holzapfel C et al (2018) Gender- and age-related changes in trunk muscle composition using chemical shift encoding-based water(-)fat MRI. Nutrients 10:1972
Cagnie B, Dhooge F, Schumacher C et al (2015) Fiber typing of the erector spinae and multifidus muscles in healthy controls and back pain patients: a systematic literature review. J Manipulative Physiol Ther 38:653–663
Vikne H, Strom V, Pripp AH, Gjovaag T (2020) Human skeletal muscle fiber type percentage and area after reduced muscle use: a systematic review and meta-analysis. Scand J Med Sci Sports 30:1298–1317
Wang Y, Pessin JE (2013) Mechanisms for fiber-type specificity of skeletal muscle atrophy. Curr Opin Clin Nutr Metab Care 16:243–250
Agten A, Stevens S, Verbrugghe J, Eijnde BO, Timmermans A, Vandenabeele F (2020) The lumbar multifidus is characterised by larger type I muscle fibres compared to the erector spinae. Anat Cell Biol 53:143–150
Takahashi S, Hoshino M, Ohyama S et al (2021) Relationship of back muscle and knee extensors with the compensatory mechanism of sagittal alignment in a community-dwelling elderly population. Sci Rep 11:2179
Acknowledgements
The authors thank Hui Lin, for their helpful advice on the statistical analysis.
Funding
This study has received funding from Chongqing Science and Technology Commission, China (No. cstc2019jscx-msxmX0221).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Dr. Wei Chen (Department of Radiology, The first affiliated hospital, Army Medical University).
Conflict of interest
Xiaoyue Zhou is an employee of Siemens Healthcare. The remaining authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
Hui Lin (Department of Epidemiology, College of Preventive Medicine, Third Military Medical University) kindly provided statistical advice for this manuscript.
Informed consent
Written informed consent was obtained from all subjects in this study.
Ethical approval
Institutional Review Board approval was obtained (No: (A) KY2021059).
Study subjects or cohorts overlap
Study subjects or cohorts have not been previously reported.
Methodology
• Prospective
• Cross-sectional study
• Performed at one institution
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, P., Zhou, Z., Sun, L. et al. Quantitative multi-parameter assessment of age- and gender-related variation of back extensor muscles in healthy adults using Dixon MR imaging. Eur Radiol 34, 69–79 (2024). https://doi.org/10.1007/s00330-023-09954-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-09954-w