Abstract
Objective
To develop and validate a deep learning (DL) signature for predicting lymph node (LN) metastasis in patients with lung adenocarcinoma.
Methods
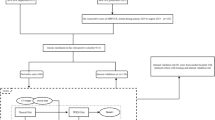
A total of 612 patients with pathologically-confirmed lung adenocarcinoma were retrospectively enrolled and were randomly divided into training cohort (n = 489) and internal validation cohort (n = 123). Besides, 108 patients were enrolled and constituted an independent test cohort (n = 108). Patients’ clinical characteristics and CT semantic features were collected. The radiomics features were derived from contrast-enhanced CT images. The clinical-semantic model and radiomics signature were built to predict LN metastasis. Furthermore, Swin Transformer was adopted to develop a DL signature predictive of LN metastasis. Model performance was evaluated by area under the receiver operating characteristic curve (AUC), sensitivity, specificity, calibration curve, and decision curve analysis. The comparisons of AUC were conducted by the DeLong test.
Results
The proposed DL signature yielded an AUC of 0.948–0.961 across all three cohorts, significantly superior to both clinical-semantic model and radiomics signature (all p < 0.05). The calibration curves show that DL signature predicted probabilities fit well the actual observed probabilities of LN metastasis. DL signature gained a higher net benefit than both clinical-semantic model and radiomics signature. The incorporation of radiomics signature or clinical-semantic risk predictors failed to reveal an incremental value over the DL signature.
Conclusions
The proposed DL signature based on Swin Transformer achieved a promising performance in predicting LN metastasis and could confer important information in noninvasive mediastinal LN staging and individualized therapeutic options.
Key Points
• Accurate prediction for lymph node metastasis is crucial to formulate individualized therapeutic options for patients with lung adenocarcinoma.
• The deep learning signature yielded an AUC of 0.948–0.961 across all three cohorts in predicting lymph node metastasis, superior to both radiomics signature and clinical-semantic model.
• The incorporation of radiomics signature or clinical-semantic risk predictors into deep learning signature failed to reveal an incremental value over deep learning signature.





Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the curve
- CEA:
-
Carcinoembryonic antigen
- CI:
-
Confidence interval
- CS:
-
Clinical-semantic
- CTR:
-
Consolidation-to-tumor ratio
- DL:
-
Deep learning
- ICC:
-
Intraclass correlation coefficient
- LI:
-
Labeling index
- LN:
-
lymph node
- NSCLC:
-
Non-small cell lung cancer
- OR:
-
Odds ratio
- ROC:
-
Receiver operating characteristic curve
References
Siegel RL, Miller KD, Jemal A (2020) Cancer statistics, 2020. CA Cancer J Clin 70(1):7–30
Chiang XH, Hsu HH, Hsieh MS et al (2020) Propensity-matched analysis comparing survival after sublobar resection and lobectomy for cT1N0 lung adenocarcinoma. Ann Surg Oncol 27(3):703–715
Altorki NK, Wang X, Wigle D et al (2018) Perioperative mortality and morbidity after sublobar versus lobar resection for early-stage non-small-cell lung cancer: post-hoc analysis of an international, randomised, phase 3 trial (CALGB/Alliance 140503). Lancet Respir Med 6(12):915–924
Zhang B, Liu R, Ren D et al (2021) Comparison of lobectomy and sublobar resection for stage IA elderly NSCLC patients (≥70 Years): a population-based propensity score matching’s study. Front Oncol 11:610638
Suzuki K, Koike T, Asakawa T et al (2011) A prospective radiological study of thin-section computed tomography to predict pathological noninvasiveness in peripheral clinical IA lung cancer (Japan Clinical Oncology Group 0201). J Thorac Oncol 6(4):751–756
Aokage K, Suzuki K, Wakabayashi M et al (2021) Predicting pathological lymph node status in clinical stage IA peripheral lung adenocarcinoma. Eur J Cardiothorac Surg 60(1):64–71
Choi H, Kim H, Park CM, Kim YT, Goo JM (2021) Central tumor location at chest CT is an adverse prognostic factor for disease-free survival of node-negative early-stage lung adenocarcinomas. Radiology 299(2):438–447
Prabhakar B, Shende P, Augustine S (2018) Current trends and emerging diagnostic techniques for lung cancer. Biomed Pharmacother 106:1586–1599
Kandathil A, Kay FU, Butt YM, Wachsmann JW, Subramaniam RM (2018) Role of FDG PET/CT in the eighth edition of TNM staging of non-small cell lung cancer. Radiographics 38(7):2134–2149
Pak K, Park S, Cheon GJ et al (2015) Update on nodal staging in non-small cell lung cancer with integrated positron emission tomography/computed tomography: a meta-analysis. Ann Nucl Med 29(5):409–419
Liu Y, Kim J, Balagurunathan Y et al (2018) Prediction of pathological nodal involvement by CT-based Radiomic features of the primary tumor in patients with clinically node-negative peripheral lung adenocarcinomas. Med Phys 45(6):2518–2526
Wang X, Zhao X, Li Q et al (2019) Can peritumoral radiomics increase the efficiency of the prediction for lymph node metastasis in clinical stage T1 lung adenocarcinoma on CT? Eur Radiol 29(11):6049–6058
Cong M, Feng H, Ren J-L et al (2020) Development of a predictive radiomics model for lymph node metastases in pre-surgical CT-based stage IA non-small cell lung cancer. Lung Cancer 139:73–79
He L, Huang Y, Yan L et al (2019) Radiomics-based predictive risk score: a scoring system for preoperatively predicting risk of lymph node metastasis in patients with resectable non-small cell lung cancer. Chin J Cancer Res 31(4):641–652
Peng X, Yang S, Zhou L et al (2021) Repeatability and reproducibility of computed tomography radiomics for pulmonary nodules: a multicenter phantom study. Invest Radiol 57(4):242–253
Han Y, Ma Y, Wu Z et al (2021) Histologic subtype classification of non-small cell lung cancer using PET/CT images. Eur J Nucl Med Mol Imaging 48(2):350–360
Chaunzwa TL, Hosny A, Xu Y et al (2021) Deep learning classification of lung cancer histology using CT images. Sci Rep 11(1):5471
Avanzo M, Gagliardi V, Stancanello J et al (2021) Combining computed tomography and biologically effective dose in radiomics and deep learning improves prediction of tumor response to robotic lung stereotactic body radiation therapy. Med Phys 48(10):6257–6269
Tian P, He B, Mu W et al (2021) Assessing PD-L1 expression in non-small cell lung cancer and predicting responses to immune checkpoint inhibitors using deep learning on computed tomography images. Theranostics 11(5):2098–2107
Hou R, Li X, Xiong J et al (2021) Predicting tyrosine kinase inhibitor treatment response in stage IV lung adenocarcinoma patients with EGFR mutation using model-based deep transfer learning. Front Oncol 11:679764
Zhong Y, She Y, Deng J et al (2022) Deep learning for prediction of N2 Metastasis and survival for clinical stage I non-small cell lung cancer. Radiology 302(1):200–211
Kim H, Goo JM, Lee KH, Kim YT, Park CM (2020) Preoperative CT-based deep learning model for predicting disease-free survival in patients with lung adenocarcinomas. Radiology 296(1):216–224
Zhao X, Wang X, Xia W et al (2020) A cross-modal 3D deep learning for accurate lymph node metastasis prediction in clinical stage T1 lung adenocarcinoma. Lung Cancer 145:10–17
Ran J, Cao R, Cai J et al (2021) Development and validation of a nomogram for preoperative prediction of lymph node metastasis in lung adenocarcinoma based on radiomics signature and deep learning signature. Front Oncol 11:585942
Wang Y-W, Chen C-J, Huang H-C et al (2021) Dual energy CT image prediction on primary tumor of lung cancer for nodal metastasis using deep learning. Comput Med Imaging Graph 91:101935
Yan R, Fan X, Xiao Z et al (2022) Inhibition of DCLK1 sensitizes resistant lung adenocarcinomas to EGFR-TKI through suppression of Wnt/β-Catenin activity and cancer stemness. Cancer Lett 531:83–97
Yasukawa M, Ohbayashi C, Kawaguchi T et al (2019) Analysis of histological grade in resected lung-invasive adenocarcinoma. Anticancer Res 39(3):1491–1500
Yoshizawa A, Sumiyoshi S, Sonobe M et al (2013) Validation of the IASLC/ATS/ERS lung adenocarcinoma classification for prognosis and association with EGFR and KRAS gene mutations: analysis of 440 Japanese patients. J Thorac Oncol 8(1):52–61
Agarwal D, Marques G, de la Torre-Díez I et al (2021) Transfer learning for alzheimer’s disease through neuroimaging biomarkers: a systematic review. Sensors (Basel) 21(21):7259
LIU Z, LIN Y, CAO Y, et al (2021) Swin transformer: hierarchical vision transformer using shifted windows. arXiv Prepr. 2021, arXiv:2103.14030.
Le Berre A, Kamagata K, Otsuka Y et al (2019) Convolutional neural network-based segmentation can help in assessing the substantia nigra in neuromelanin MRI. Neuroradiology 61(12):1387–1395
Hagiwara A, Fujita S, Ohno Y, Aoki S (2020) Variability and standardization of quantitative imaging: monoparametric to multiparametric quantification, radiomics, and artificial intelligence. Invest Radiol 55(9):601–616
Hosny A, Parmar C, Quackenbush J, Schwartz LH, Aerts H (2018) Artificial intelligence in radiology. Nat Rev Cancer 18(8):500–510
Dal Bello MG, Filiberti RA, Alama A et al (2019) The role of CEA, CYFRA21-1 and NSE in monitoring tumor response to Nivolumab in advanced non-small cell lung cancer (NSCLC) patients. J Transl Med 17(1):74
Jiao Z, Cao S, Li J et al (2021) Clinical associations of preoperative and postoperative serum CEA and lung cancer outcome. Front Mol Biosci 8:686313
Gu Y, She Y, Xie D et al (2018) A texture analysis-based prediction model for lymph node metastasis in stage IA lung adenocarcinoma. Ann Thorac Surg 106(1):214–220
Kim H, Goo JM, Kim YT, Park CM (2019) Consolidation-to-tumor ratio and tumor disappearance ratio are not independent prognostic factors for the patients with resected lung adenocarcinomas. Lung Cancer 137:123–128
Chen Y-C, Lin Y-H, Chien H-C et al (2021) Preoperative consolidation-to-tumor ratio is effective in the prediction of lymph node metastasis in patients with pulmonary ground-glass component nodules. Thoracic Cancer 12(8):1203–1209
Zhang Y, Zhao F, Wu M et al (2021) Association of postoperative recurrence with radiological and clinicopathological features in patients with stage IA-IIA lung adenocarcinoma. Eur J Radiol 141:109802
Kim HJ, Cho JY, Lee YJ et al (2019) Clinical significance of pleural attachment and indentation of subsolid nodule lung cancer. Cancer Res Treat 51(4):1540–1548
Silvestri GA, Gonzalez AV, Jantz MA et al (2013) Methods for staging non-small cell lung cancer: diagnosis and management of lung cancer, 3rd ed: American College of Chest Physicians evidence-based clinical practice guidelines. Chest 143(5 Suppl):e211S–e250S
Leiro-Fernández V, Fernández-Villar A (2021) Mediastinal staging for non-small cell lung cancer. Transl Lung Cancer Res 10(1):496–505
Walker CM, Chung JH, Abbott GF et al (2012) Mediastinal lymph node staging: from noninvasive to surgical. AJR Am J Roentgenol 199(1):W54–W64
Funding
This study has received funding from the National Natural Science Foundation of China (NO.81873889).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Liming Xia.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Study subjects or cohorts overlap
Some study subjects or cohorts have been previously reported in a prior study, where 182 patients with early-stage lung adenocarcinoma were previously reported on the relationship between CT morphological features and Ki-67 (PMID: 34164176). The present study has a much larger sample size and focuses on predicting lymph node metastasis in lung adenocarcinoma.
Methodology
• retrospective
• diagnostic study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
(PDF 161 kb)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ma, X., Xia, L., Chen, J. et al. Development and validation of a deep learning signature for predicting lymph node metastasis in lung adenocarcinoma: comparison with radiomics signature and clinical-semantic model. Eur Radiol 33, 1949–1962 (2023). https://doi.org/10.1007/s00330-022-09153-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-09153-z