Abstract
Objectives
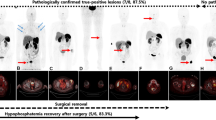
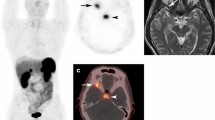
Currently, the main challenge in tumour-induced osteomalacia (TIO) is the difficulty in locating culprit tumours for definitive diagnosis and surgical therapy. Herein, we retrospectively evaluate the efficiency of 68Ga-DOTANOC PET/CT in the localisation and diagnosis of TIO, and compared with 18F-FDG.
Methods
Twenty-four consecutive patients with hypophosphataemic osteomalacia (HO) and suspicion of TIO who were referred to our centre for 68Ga-DOTANOC PET/CT scanning were retrospectively reviewed. The images were evaluated qualitatively as well as semi-quantitatively, and imaging results were compared with the final diagnoses.
Results
Among the total of 21 patients who were included in the final analyses, 17 were diagnosed with TIO, while four were proven to have other causes of HO. 68Ga-DOTANOC PET/CT produced positive results in 16 of the 17 patients with TIO, representing a sensitivity of 94.1%. Moreover, the 68Ga-DOTANOC PET/CT results were negative in 3 of the 4 patients without TIO, representing a specificity of 75.0%. The overall accuracy of 68Ga-DOTANOC PET/CT in locating the tumours responsible for TIO is 90.5%. In particular, 68Ga-DOTANOC PET/CT detected the culprit tumours in 4 out of 10 patients with negative results on previous 18F-FDG PET/CT and showed a significantly higher T/M ratio of tumours than 18F-FDG PET/CT in the same patients (n = 10; 4.76 ± 3.08 vs 1.95 ± 1.33, p < 0.05).
Conclusions
68Ga-DOTANOC PET/CT is an accurate imaging modality in the localisation of tumours for TIO. It is superior to 18F-FDG PET/CT and may be useful in the differential diagnosis of HO.
Key Points
• TIO should be considered a possible cause for patients diagnosed with HO, which usually needs to be differentiated from other aetiologies.
• 68 Ga-DOTANOC PET/CT is an accurate imaging modality in locating culprit tumours for TIO, superior to 18 F-FDG PET/CT.

Similar content being viewed by others
Abbreviations
- 18F-FDG:
-
18F-Fluorodeoxyglucose
- 68Ga-DOTANOC:
-
68Ga-DOTA-1-NaI (3)-octreotide
- 99mTc-HYNIC-TOC:
-
99mTc-Hydrazinonicotinyl-Tyr3-octreotide
- ADV:
-
Adefovir dipivoxil
- ALP:
-
Alkaline phosphatase
- CT:
-
Computed tomography
- DOTA:
-
1,4,7,10-Tetraazacyclododecane-1,4,7,10-tetraacetic acid
- FGF23:
-
Fibroblast growth factor 23
- HCl:
-
Hydrochloric acid
- HO:
-
Hypophosphataemic osteomalacia
- iPTH:
-
Intact parathyroid hormone
- MRI:
-
Magnetic resonance imaging
- PET:
-
Positron emission tomography
- PMT:
-
Phosphaturic mesenchymal tumour
- RAMLA:
-
Row action maximum likelihood algorithm
- SPECT:
-
Single-photon emission computed tomography
- SSTR:
-
Somatostatin receptors
- SUV:
-
Standard uptake value
- T/M:
-
Ratio of tumour SUVmax to mediastinal blood pool SUVmax
- TIO:
-
Tumour-induced osteomalacia
References
Jan de Beur SM (2005) Tumor-induced osteomalacia. JAMA 294:1260–1267
Minisola S, Peacock M, Fukumoto S et al (2017) Tumour-induced osteomalacia. Nat Rev Dis Primers 3:17044
Riminucci M, Collins MT, Fedarko NS et al (2003) FGF-23 in fibrous dysplasia of bone and its relationship to renal phosphate wasting. J Clin Invest 112:683–692
Mc CR (1947) Osteomalacia with Looser’s nodes (Milkman’s syndrome) due to a raised resistance to vitamin D acquired about the age of 15 years. Q J Med 16:33–46
Folpe AL (2019) Phosphaturic mesenchymal tumors: a review and update. Semin Diagn Pathol 36:260–268
Sun ZJ, Jin J, Qiu GX, Gao P, Liu Y (2015) Surgical treatment of tumor-induced osteomalacia: a retrospective review of 40 cases with extremity tumors. BMC Musculoskelet Disord 16:43
Zuo QY, Wang H, Li W et al (2017) Treatment and outcomes of tumor-induced osteomalacia associated with phosphaturic mesenchymal tumors: retrospective review of 12 patients. BMC Musculoskelet Disord 18:403
Jadhav S, Kasaliwal R, Shetty NS et al (2014) Radiofrequency ablation, an effective modality of treatment in tumor-induced osteomalacia: a case series of three patients. J Clin Endocrinol Metab 99:3049–3054
Chong WH, Molinolo AA, Chen CC, Collins MT (2011) Tumor-induced osteomalacia. Endocr Relat Cancer 18:R53–R77
Ria R, Dammacco F, Vacca A (2018) Heavy-chain diseases and myeloma-associated Fanconi syndrome: an update. Mediterr J Hematol Infect Dis 10:e2018011
Girgis CM, Wong T, Ngu MC et al (2011) Hypophosphataemic osteomalacia in patients on adefovir dipivoxil. J Clin Gastroenterol 45:468–473
Dupond JL, Mahammedi H, Magy N, Blagosklonov O, Meaux-Ruault N, Kantelip B (2005) Detection of a mesenchymal tumor responsible for hypophosphatemic osteomalacia using FDG-PET. Eur J Intern Med 16:445–446
Jagtap VS, Sarathi V, Lila AR et al (2011) Tumor-induced osteomalacia: a single center experience. Endocr Pract 17:177–184
Seo HJ, Choi YJ, Kim HJ et al (2011) Using (18)F-FDG PET/CT to detect an occult mesenchymal tumor causing oncogenic osteomalacia. Nucl Med Mol Imaging 45:233–237
Duet M, Kerkeni S, Sfar R, Bazille C, Liote F, Orcel P (2008) Clinical impact of somatostatin receptor scintigraphy in the management of tumor-induced osteomalacia. Clin Nucl Med 33:752–756
Houang M, Clarkson A, Sioson L et al (2013) Phosphaturic mesenchymal tumors show positive staining for somatostatin receptor 2A (SSTR2A). Hum Pathol 44:2711–2718
Jing H, Li F, Zhuang H et al (2013) Effective detection of the tumors causing osteomalacia using [Tc-99m]-HYNIC-octreotide (99mTc-HYNIC-TOC) whole body scan. Eur J Radiol 82:2028–2034
Breer S, Brunkhorst T, Beil FT et al (2014) Ga-68 DOTA-TATE PET/CT allows tumor localization in patients with tumor-induced osteomalacia but negative In-111-octreotide SPECT/CT. Bone 64:222–227
El-Maouche D, Sadowski SM, Papadakis GZ et al (2016) (68)Ga-DOTATATE for tumor localization in tumor-induced osteomalacia. J Clin Endocrinol Metab 101:3575–3581
Paquet M, Gauthe M, Zhang Yin J et al (2018) Diagnostic performance and impact on patient management of (68)Ga-DOTA-TOC PET/CT for detecting osteomalacia-associated tumours. Eur J Nucl Med Mol Imaging 45:1710–1720
von Falck C, Rodt T, Rosenthal H et al (2008) (68)Ga-DOTANOC PET/CT for the detection of a mesenchymal tumor causing oncogenic osteomalacia. Eur J Nucl Med Mol Imaging 35:1034
Ho CL (2015) Ga68-DOTA Peptide PET/CT to detect occult mesenchymal tumor-inducing osteomalacia: a case series of three patients. Nucl Med Mol Imaging 49:231–236
Kabasakal L, Demirci E, Ocak M et al (2012) Comparison of (6)(8)Ga-DOTATATE and (6)(8)Ga-DOTANOC PET/CT imaging in the same patient group with neuroendocrine tumours. Eur J Nucl Med Mol Imaging 39:1271–1277
Wild D, Bomanji JB, Benkert P et al (2013) Comparison of 68Ga-DOTANOC and 68Ga-DOTATATE PET/CT within patients with gastroenteropancreatic neuroendocrine tumors. J Nucl Med 54:364–372
Zhang J, Zhu Z, Zhong D et al (2015) 68Ga DOTATATE PET/CT is an accurate imaging modality in the detection of culprit tumors causing osteomalacia. Clin Nucl Med 40:642–646
John JR, Hephzibah J, Oommen R, Shanthly N, Mathew D (2019) Ga-68 DOTATATE positron emission tomography-computed tomography imaging in oncogenic osteomalacia: experience from a tertiary level hospital in South India. Indian J Nucl Med 34:188–193
Clifton-Bligh RJ, Hofman MS, Duncan E et al (2013) Improving diagnosis of tumor-induced osteomalacia with Gallium-68 DOTATATE PET/CT. J Clin Endocrinol Metab 98:687–694
Bhavani N, Reena Asirvatham A, Kallur K et al (2016) Utility of gallium-68 DOTANOC PET/CT in the localization of tumour-induced osteomalacia. Clin Endocrinol (Oxf) 84:134–140
Singh D, Chopra A, Ravina M et al (2017) Oncogenic osteomalacia: role of Ga-68 DOTANOC PET/CT scan in identifying the culprit lesion and its management. Br J Radiol 90:20160811
Jiang Y, Hou G, Cheng W (2020) Performance of 68Ga-DOTA-SST PET/CT, octreoscan SPECT/CT and 18F-FDG PET/CT in the detection of culprit tumors causing osteomalacia: a meta-analysis. Nucl Med Commun 41:370–376
Agrawal K, Bhadada S, Mittal BR et al (2015) Comparison of 18F-FDG and 68Ga DOTATATE PET/CT in localization of tumor causing oncogenic osteomalacia. Clin Nucl Med 40:e6–e10
Ding J, Hu G, Wang L, Li F, Huo L (2018) Increased activity due to fractures does not significantly affect the accuracy of 68Ga-DOTATATE PET/CT in the detection of culprit tumor in the evaluation of tumor-induced osteomalacia. Clin Nucl Med 43:880–886
Weidner N (1991) Review and update: oncogenic osteomalacia-rickets. Ultrastruct Pathol 15:317–333
Folpe AL, Fanburg-Smith JC, Billings SD et al (2004) Most osteomalacia-associated mesenchymal tumors are a single histopathologic entity: an analysis of 32 cases and a comprehensive review of the literature. Am J Surg Pathol 28:1–30
Acknowledgements
We would like to thank Fuhua Wen and Dake Zhang for the preparation of PET tracers and all the technicians for PET/CT image acquisition and processing in PET/CT Center at the First Affiliated Hospital of Sun Yat-Sen University.
Funding
The authors state that this study has received funding from the Medical Scientific Research Foundation of Guangdong Province of China (No. A2019528) and Natural Science Foundation of Guangdong Province of China (No. 2019A1515010845).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Xiangsong Zhang.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Study subjects or cohorts overlap
One study subject has been previously reported in Clin Nucl Med. 2018 Jun;43(6):e198–e199.
Methodology
• retrospective
• diagnostic or prognostic study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
He, Q., Zhang, B., Zhang, L. et al. Diagnostic efficiency of 68Ga-DOTANOC PET/CT in patients with suspected tumour-induced osteomalacia. Eur Radiol 31, 2414–2421 (2021). https://doi.org/10.1007/s00330-020-07342-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-020-07342-2