Abstract
Background
Two-thirds of patients undergoing liver resection for intrahepatic cholangiocarcinoma experience recurrence after surgery. Our aim was to identify factors associated with early recurrence after resection for intrahepatic cholangiocarcinoma.
Methods
Patients with intrahepatic cholangiocarcinoma undergoing curative intent resection (complete resection and lymphadenectomy) were included in two centers between 2005 and 2021 and were divided into three groups: early recurrence (< 12 months after resection), delayed recurrence (> 12 months), and no recurrence. Patients experiencing early (< 90 days) postoperative mortality were excluded.
Results
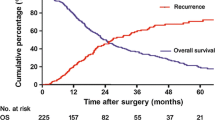
Among 120 included patients, 44 (36.7%) experienced early recurrence, 24 (20.0%) experienced delayed recurrence, and 52 (43.3%) did not experience recurrence after a median follow-up of 59 months (IQR: 26-113). The median recurrence-free survival was 16 months (95% CI: 9.6–22.4). Median overall survival was 55 months (95% CI: 45.7–64.3), while it was 25 months for patients with early recurrence (p < 0.001). Patients with early recurrence had significantly larger tumors (59.1% of tumors > 70 mm in early vs. 58.3% in delayed vs. 26.9% in no recurrence group, p = 0.002), multiple lesions (65.9% vs. 29.2% vs. 11.5%, p < 0.001), and positive lymph nodes (N +) (38.6% vs. 37.5% vs. 11.5%, p = 0.005). In multivariable analysis, presence of multiple lesions (OR: 9.324; 95% CI: 3.051–28.489; p < 0.001) and positive lymph nodes (OR: 3.307. 95% CI: 1.001–11.011. p = 0.05) were associated with early recurrence.
Conclusion
Early recurrence after curative resection of intrahepatic cholangiocarcinoma is frequent and is associated with the presence of multiple lesions and positive lymph nodes, raising the question of surgery’s futility in this context.

Similar content being viewed by others
References
Lepage C, Cottet V, Chauvenet M et al (2011) Trends in the incidence and management of biliary tract cancer: a French population-based study. J Hepatol 54(2):306–310
Wu L, Tsilimigras DI, Paredes AZ et al (2019) Trends in the incidence, treatment and outcomes of patients with intrahepatic cholangiocarcinoma in the USA: facility type is associated with margin status, use of lymphadenectomy and overall survival. World J Surg 43(7):1777–1787. https://doi.org/10.1007/s00268-019-04966-4
Farges O, Fuks D, Boleslawski E et al (2011) Influence of surgical margins on outcome in patients with intrahepatic cholangiocarcinoma: a multicenter study by the AFC-IHCC-2009 study group. Ann Surg 254(5):824–829
Doussot A, Jarnagin WR, Azoulay D et al (2019) Improving actual survival after hepatectomy for intrahepatic cholangiocarcinoma-still a long way to go. Hepatobiliary Surg Nutr 8(2):161–163
Reames BN, Ejaz A, Koerkamp BG et al (2017) Impact of major vascular resection on outcomes and survival in patients with intrahepatic cholangiocarcinoma: a multi-institutional analysis. J Surg Oncol 116(2):133–139
Sutton TL, Billingsley KG, Walker BS et al (2021) Neoadjuvant chemotherapy is associated with improved survival in patients undergoing hepatic resection for intrahepatic cholangiocarcinoma. Am J Surg 221(6):1182–1187
Primrose JN, Fox RP, Palmer DH et al (2019) Capecitabine compared with observation in resected biliary tract cancer (BILCAP): a randomised, controlled, multicentre, phase 3 study. Lancet Oncol 20(5):663–673
Doussot A, Gonen M, Wiggers JK et al (2016) Recurrence patterns and disease-free survival after resection of intrahepatic cholangiocarcinoma: preoperative and postoperative prognostic models. J Am Coll Surg 223(3):493-505.e2
Hu L-S, Zhang X-F, Weiss M et al (2019) Recurrence patterns and timing courses following curative-intent resection for intrahepatic cholangiocarcinoma. Ann Surg Oncol 26(8):2549–2557
Valle J, Wasan H, Palmer DH et al (2010) Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. N Engl J Med 362(14):1273–1281
Pang YY (2000) The Brisbane 2000 terminology of liver anatomy and resections. HPB 2:333–339
Dindo D, Demartines N, Clavien P-A (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240(2):205–213
Rahbari NN, Garden OJ, Padbury R et al (2011) Posthepatectomy liver failure: a definition and grading by the international study group of liver surgery (ISGLS). Surgery 149(5):713–724
Koch M, Garden OJ, Padbury R et al (2011) Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the international study group of liver surgery. Surgery 149(5):680–688
Malka D, Bernardini D, Boudjema K, et al (2019) Cancer des voies biliaires. TNCD
Edeline J, Benabdelghani M, Bertaut A et al (2019) Gemcitabine and oxaliplatin chemotherapy or surveillance in resected biliary tract cancer (PRODIGE 12-ACCORD 18-UNICANCER GI): a randomized phase III study. J Clin Oncol 37(8):658–667
Wang C, Pang S, Si-Ma H et al (2019) Specific risk factors contributing to early and late recurrences of intrahepatic cholangiocarcinoma after curative resection. World J Surg 17(1):2. https://doi.org/10.1186/s12957-018-1540-1
Bridgewater J, Galle PR, Khan SA et al (2014) Guidelines for the diagnosis and management of intrahepatic cholangiocarcinoma. J Hepatol 60(6):1268–1289
Zhang X-F, Beal EW, Bagante F et al (2018) Early versus late recurrence of intrahepatic cholangiocarcinoma after resection with curative intent. Br J Surg 105(7):848–856
Portolani N, Coniglio A, Ghidoni S et al (2006) Early and late recurrence after liver resection for hepatocellular carcinoma: prognostic and therapeutic implications. Ann Surg 243(2):229–235
Valverde A, Bonhomme N, Farges O et al (1999) Resection of intrahepatic cholangiocarcinoma: a Western experience. J Hepatobiliary Pancreat Surg 6(2):122–127
Addeo P, Jedidi I, Locicero A et al (2019) Prognostic impact of tumor multinodularity in intrahepatic cholangiocarcinoma. J Gastrointest Surg 23(9):1801–1809
Xue R, Li R, Guo H et al (2016) Variable intra-tumor genomic heterogeneity of multiple lesions in patients with hepatocellular carcinoma. Gastroenterology 150(4):998–1008
Bagante F, Spolverato G, Merath K et al (2019) Intrahepatic cholangiocarcinoma tumor burden: a classification and regression tree model to define prognostic groups after resection. Surgery 166(6):983–990
Sposito C, Droz Dit Busset M, Virdis M et al (2021) The role of lymphadenectomy in the surgical treatment of intrahepatic cholangiocarcinoma: a review. Eur J Surg Oncol. https://doi.org/10.1016/j.ejso.2021.08.009
Shimada M, Yamashita Y, Aishima S et al (2001) Value of lymph node dissection during resection of intrahepatic cholangiocarcinoma. Br J Surg 88(11):1463–1466
Noji T, Kondo S, Hirano S et al (2008) Computed tomography evaluation of regional lymph node metastases in patients with biliary cancer. Br J Surg 95(1):92–96
Songthamwat M, Chamadol N, Khuntikeo N et al (2017) Evaluating a preoperative protocol that includes magnetic resonance imaging for lymph node metastasis in the cholangiocarcinoma screening and care program (CASCAP) in Thailand. World J Surg Oncol 15(1):176
Hobeika C, Cauchy F, Fuks D et al (2021) Laparoscopic versus open resection of intrahepatic cholangiocarcinoma: nationwide analysis. Br J Surg 108(4):419–426
Bagante F, Spolverato G, Weiss M et al (2017) Defining Long-Term survivors following resection of intrahepatic cholangiocarcinoma. J Gastrointest Surg 21(11):1888–1897
Jutric Z, Johnston WC, Hoen HM et al (2016) Impact of lymph node status in patients with intrahepatic cholangiocarcinoma treated by major hepatectomy: a review of the national cancer database. HPB 18(1):79–87
Akateh C, Ejaz AM, Pawlik TM et al (2020) Neoadjuvant treatment strategies for intrahepatic cholangiocarcinoma. World J Hepatol 12(10):693–708
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Contributions
AN, ST, RS, DF contributed to conception and design. ST, RS, UM, DF provided administrative support. UM, JV, FC, DF contributed to provision of study materials or patients. AN, CH, TC, AB, AD, MS contributed to collection and assembly of data. AN, ST, RS, FC, DF contributed to data analysis and interpretation. All authors contributed to manuscript writing. All authors approved the final version of manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Consent to publish
This study has not been previously published elsewhere. All authors actively contributed to this work and gave their final approval before submission.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nassar, A., Tzedakis, S., Sindayigaya, R. et al. Factors of Early Recurrence After Resection for Intrahepatic Cholangiocarcinoma. World J Surg 46, 2459–2467 (2022). https://doi.org/10.1007/s00268-022-06655-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-022-06655-1