Abstract
Background
The indication of surgery in intrahepatic cholangiocarcinoma (ICC) patients with lymph node metastasis (LNM), macroscopic periductal infiltration (PI), and intrahepatic metastasis (IM) remains unclear.
Methods
Patients who underwent resection for mass-forming (MF) dominant ICC and unresected patients caused by LNM, IM, or locally advanced tumors (UR group) were enrolled. The significance of CA19-9 was investigated in advanced ICC.
Results
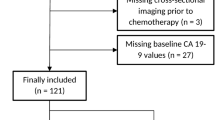
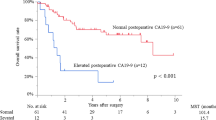
Seventy-three patients who underwent resection and 20 UR patients were analyzed. Using the minimum p value approach based on the overall survival, the optimal CA19-9 cutoff value was 300 U/mL. The OS of the patients with CA19-9 < 37 U/mL (n = 26; MST, 49.6 months) and 37–300 U/mL (n = 28; MST, 45.1 months) was comparable (P = 0.842); however, the OS of the patients with CA19-9 = 37–300 U/mL was significantly better than that with CA19-9 ≥ 300 U/mL (n = 19; MST, 15.3 months; P < 0.001). CA19-9 > 300 U/mL, MF + PI, and IM were independently associated with OS. The OS of the patients with CA19-9 < 300 U/mL who developed LNM (MST, 34.0 months), MF + PI (MST, 32.9 months), or IM (MST, 35.2 months), or who required major vascular resection (MST, 45.1 months) was better than those with CA19-9 ≥ 300 U/mL who developed LNM (MST, 8.7 months; P = 0.005), MF + PI (MST, 7.5 months; P = 0.040), or IM (MST, 8.7 months; P = 0.001), or who required major vascular resection (MST, 14.8 months; P = 0.015); their prognosis was similar with the UR group.
Conclusions
Even if patients had ICC developing LNM, PI, or IM, or require major vascular resection, surgical resection can be indicated for patients with CA19-9 < 300 U/mL. However, the indications for either adjuvant therapy or resection should be carefully determined in patients with CA19-9 ≥ 300 U/mL.



Similar content being viewed by others
Abbreviations
- ICC:
-
Intrahepatic cholangiocarcinoma
- LNM:
-
Lymph node metastasis
- IM:
-
Intrahepatic metastasis
- VI:
-
Vascular invasion
- PI:
-
Periductal infiltrating
- EASL:
-
European Association for the Study of Liver
- CA19-9:
-
Carbohydrate antigen 19-9
- MF:
-
Mass-forming
- IG:
-
Intraductal growth
- TNM:
-
Tumor-node-metastasis
- AJCC:
-
American Joint Committee on Cancer
- UICC:
-
International Union Against Cancer
- CEA:
-
Carcinoembryonic antigen
- PVR:
-
Portal vein resection
- HAR:
-
Hepatic artery resection
- IVCR:
-
Inferior vena cava resection
References
Shirabe K, Mano Y, Taketomi A et al (2010) Clinicopathological prognostic factors after hepatectomy for patients with mass-forming type intrahepatic cholangiocarcinoma: relevance of the lymphatic invasion index. Ann Surg Oncol 17:1816–1822
Yamamoto Y, Sugiura T, Okamura Y et al (2017) The pitfalls of left trisectionectomy or central bisectionectomy for biliary cancer: anatomical classification based on the ventral branches of segment VI portal vein relative to the right hepatic vein. J Gastrointest Surg 30:017–3486
Yamamoto Y, Sugiura T, Okamura Y et al (2016) Is combined pancreatoduodenectomy for advanced gallbladder cancer justified? Surgery 159:810–820
Gurlevik E, Fleischmann-Mundt B, Armbrecht N et al (2013) Adjuvant gemcitabine therapy improves survival in a locally induced, R0-resectable model of metastatic intrahepatic cholangiocarcinoma. Hepatology 58:1031–1041
Shen WF, Zhong W, Liu Q et al (2011) Adjuvant transcatheter arterial chemoembolization for intrahepatic cholangiocarcinoma after curative surgery: retrospective control study. World J Surg 35:2083–2091. https://doi.org/10.1007/s00268-011-1171-y
Cho SY, Park SJ, Kim SH et al (2010) Survival analysis of intrahepatic cholangiocarcinoma after resection. Ann Surg Oncol 17:1823–1830
Ariizumi S, Kotera Y, Takahashi Y et al (2011) Mass-forming intrahepatic cholangiocarcinoma with marked enhancement on arterial-phase computed tomography reflects favorable surgical outcomes. J Surg Oncol 104:130–139
Shirabe K, Shimada M, Harimoto N et al (2002) Intrahepatic cholangiocarcinoma: its mode of spreading and therapeutic modalities. Surgery 131:S159–S164
Turkoglu MA, Yamamoto Y, Sugiura T et al (2016) The favorable prognosis after operative resection of hypervascular intrahepatic cholangiocarcinoma: a clinicopathologic and immunohistochemical study. Surgery 160:683–690
Yamamoto Y, Turkoglu MA, Aramaki T et al (2016) Vascularity of intrahepatic cholangiocarcinoma on computed tomography is predictive of lymph node metastasis. Ann Surg Oncol 23:485–493
Shimada K, Sano T, Sakamoto Y et al (2007) Surgical outcomes of the mass-forming plus periductal infiltrating types of intrahepatic cholangiocarcinoma: a comparative study with the typical mass-forming type of intrahepatic cholangiocarcinoma. World J Surg 31:2016–2022. https://doi.org/10.1007/s00268-007-9194-0
Ribero D, Pinna AD, Guglielmi A et al (2012) Surgical approach for long-term survival of patients with intrahepatic cholangiocarcinoma: a multi-institutional analysis of 434 patients. Arch Surg 147:1107–1113
Farges O, Fuks D, Boleslawski E et al (2011) Influence of surgical margins on outcome in patients with intrahepatic cholangiocarcinoma: a multicenter study by the AFC-IHCC-2009 study group. Ann Surg 254:824–829
de Jong MC, Nathan H, Sotiropoulos GC et al (2011) Intrahepatic cholangiocarcinoma: an international multi-institutional analysis of prognostic factors and lymph node assessment. J Clin Oncol 29:3140–3145
Jiang W, Zeng ZC, Tang ZY et al (2011) A prognostic scoring system based on clinical features of intrahepatic cholangiocarcinoma: the Fudan score. Ann Oncol 22:1644–1652
Bridgewater J, Galle PR, Khan SA et al (2014) Guidelines for the diagnosis and management of intrahepatic cholangiocarcinoma. J Hepatol 60:1268–1289
CC C (2009) American Joint Committee on Cancer: AJCC cancer staging atlas: a companion to the seventh editions of the AJCC cancer staging manual and handbook, 2nd edn
Shimada M, Yamashita Y, Aishima S et al (2001) Value of lymph node dissection during resection of intrahepatic cholangiocarcinoma. Br J Surg 88:1463–1466
Shimada K, Sano T, Nara S et al (2009) Therapeutic value of lymph node dissection during hepatectomy in patients with intrahepatic cholangiocellular carcinoma with negative lymph node involvement. Surgery 145:411–416
Kobayashi S, Tomokuni A, Gotoh K et al (2015) Evaluation of the safety and pathological effects of neoadjuvant full-dose gemcitabine combination radiation therapy in patients with biliary tract cancer. Cancer Chemother Pharmacol 76:1191–1198
Koprowski H, Steplewski Z, Mitchell K et al (1979) Colorectal carcinoma antigens detected by hybridoma antibodies. Somatic Cell Genet 5:957–971
Kondo N, Murakami Y, Uemura K et al (2014) Elevated perioperative serum CA 19-9 levels are independent predictors of poor survival in patients with resectable cholangiocarcinoma. J Surg Oncol 110:422–429
Hatzaras I, Schmidt C, Muscarella P et al (2010) Elevated CA 19-9 portends poor prognosis in patients undergoing resection of biliary malignancies. HPB 12:134–138
Chung MJ, Lee KJ, Bang S et al (2011) Preoperative serum CA 19-9 level as a predictive factor for recurrence after curative resection in biliary tract cancer. Ann Surg Oncol 18:1651–1656
Bergquist JR, Ivanics T, Storlie CB et al (2016) Implications of CA19-9 elevation for survival, staging, and treatment sequencing in intrahepatic cholangiocarcinoma: a national cohort analysis. J Surg Oncol 114:475–482
Available at: www.esmo.org/content/download/117241/2057634/file/ESMO-2017-Abstract-Book.pdf
Japan LCSGo (2010) General rules for the clinical and pathological study of primary liver cancer 3th English ed. Tokyo, Japan
Yamamoto Y, Shimada K, Sakamoto Y et al (2009) Clinicopathological characteristics of intrahepatic cholangiocellular carcinoma presenting intrahepatic bile duct growth. J Surg Oncol 99:161–165
Uno M, Shimada K, Yamamoto Y et al (2012) Periductal infiltrating type of intrahepatic cholangiocarcinoma: a rare macroscopic type without any apparent mass. Surg Today 42:1189–1194
Ebata T, Kosuge T, Hirano S et al (2014) Proposal to modify the International Union Against Cancer staging system for perihilar cholangiocarcinomas. Br J Surg 101:79–88
Kawai S, Suzuki K, Nishio K et al (2008) Smoking and serum CA19-9 levels according to Lewis and secretor genotypes. Int J Cancer 123:2880–2884
Sugiura T, Uesaka K, Kanemoto H et al (2012) Serum CA19-9 is a significant predictor among preoperative parameters for early recurrence after resection of pancreatic adenocarcinoma. J Gastrointest Surg 16:977–985
Pollom EL, Alagappan M, Park LS et al (2017) Does radiotherapy still have a role in unresected biliary tract cancer? Cancer Med 6:129–141
Uenishi T, Yamazaki O, Horii K et al (2006) A long-term survivor of intrahepatic cholangiocarcinoma with paraaortic lymph node metastasis. J Gastroenterol 41:391–392
Acknowledgements
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Yamamoto, Y., Sugiura, T., Todaka, A. et al. Surgical Indication for Advanced Intrahepatic Cholangiocarcinoma According to the Optimal Preoperative Carbohydrate Antigen 19-9 Cutoff Value. World J Surg 42, 3331–3340 (2018). https://doi.org/10.1007/s00268-018-4605-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4605-y