Abstract
Background
Eyebrow tail ptosis is usually associated with dermatochalasis of the upper eyelid, and it is necessary to treat them together. For these associated procedures to be incorporated as a routine in upper eyelid surgeries, they should preferably be less invasive with consequent fewer complications.
Objective
We describe a minimally invasive technique for the correction of mild-to-moderate eyebrow tail ptosis corrected together with superior dermatochalasis through the blepharoplasty incision.
Methods
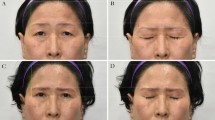
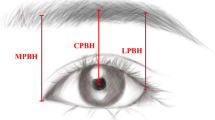
A phase 2 clinical trial was conducted from February 2020 to December 2021. A total of 50 patients underwent conventional upper blepharoplasty surgery associated with the proposed eyebrow lift technique: internal pexia in the periosteum, dissection, and posterior fixation of the orbicularis muscle to the arcus marginalis, removal of the lateral part of the orbicularis muscle, and loosening of the orbital retention ligament. Evaluation of the height of the eyebrow tail was performed with digital photography in the initial consultation and at 30–90 days postoperatively and analyzed with ImageJ software.
Results
Mean difference in brow height at 1-month and 3-month postoperative evaluations compared to the preoperative period was 3.45–3.33 mm, respectively.
Conclusion
Our study demonstrated a minimally invasive surgical technique for the treatment of mild-to-moderate eyebrow ptosis with significant eyebrow tail lift results that remained stable during the study period.
Level of Evidence II
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.




Similar content being viewed by others
References
Glass LRG, Lira J, Enkhbold E et al (2014) The lateral brow: position in relation to age, gender, and ethnicity. Ophthal Plast Reconstr Surg 30(4):295–300
Knize DM (1996) An anatomically based study of the mechanism of eyebrow ptosis. Plast Reconstr Surg 97(7):1321–33
Real DSS, Reis RP, Feitosa RGF, Garcia EB, Ferreira LM (2016) Clinical classification of brow ptosis. Rev Bras Cir Plást 31(3):354–361
Georgescu D, Anderson RL, McCann JD (2010) Brow ptosis correction: a comparison of five techniques. Facial Plast Surg 26(3):186–92
McCord CD, Doxanas MT (1990) Browplasty and brow-pexy: an adjunct to blepharoplasty. Plast Reconstr Surg 86(2):248–54
Harvey A, Zarem MD (2004) Browpexy. Aesthetic Surg J 24(4):368–72
Massry GG (2012) The external browpexy. Ophthal Plast Reconstr Surg 28(2):90–95
Cohen BD, Reiffel AJ, Spinelli HM (2011) Browpexy through the upper lid (BUL): a new technique of lifting the brow with a standard blepharoplasty incision. Aesthet Surg J 31(2):163–169
Lee JM, Lee TE, Lee H et al (2012) Change in brow position after upper blepharoplasty or levator advancement. J Craniofac Surg 23(2):434–436
Prado RB, Silva-Junior DE, Padovani CR et al (2012) Assessment of eyebrow position before and after upper eyelid blepharoplasty. Orbit Amst Neth 31(4):222–226
Nakra T, Modjtahedi S, Vrcek I et al (2016) The effect of upper eyelid blepharoplasty on eyelid and brow position. Orbit 35(6):324–327
Hassanpour SE, Khajouei Kermani H (2016) Brow ptosis after upper blepharoplasty: findings in 70 patients. World J Plast Surg 5(1):58–61
Baker MS, Shams PN, Allen RC (2016) The quantitated internal suture browpexy: comparison of two brow-lifting techniques in patients undergoing upper blepharoplasty. Ophthal Plast Reconstr Surg 32(3):204–206
Armstrong BK, Sobti D, Mancini R (2016) Partial orbicularis resection for the augmentation of traditional internal brow pexy: the “tuck and rise.” Ophthal Plast Reconstr Surg 32(6):473–6
Broadbent T, Mohktarzadeh A, Harrison A (2017) Minimally invasive brow lifting techniques. Curr Opin Ophthalmol 28(5):539–43
Briceño CA, Zhang-Nunes SX, Massry GG (2015) Minimally invasive surgical adjuncts to upper blepharoplasty. Facial Plast Surg Clin North Am 23(2):137–51
Burroughs JR, Bearden WH, Anderson RL, McCann JD (2006) Internal brow elevation at blepharoplasty. Arch Facial Plast Surg 8(1):36–41
Knize DM (1995) Transpalpebral approach to the corrugator supercilii and procerus muscles. Plast Reconstr Surg 95(1):52–60
Photogrid app. Grade, (2021) Photo app. Available in: www.photogrid.app. Access at: 20 dez. 2021
Rasband WS, Image J. US National Institutes of Health [Internet] (1997) [cited 2019 May 1]. Available from: http://imagej.nih.gov/ij/
Ramella V, Stocco C, Facchin F, Troisi L, Papa G, Arnez ZM (2018) How to make your life easier: blepharoplasty markings with microsurgical clamps. Plastic Reconstr Surg Global Open 6(8):e1873. https://doi.org/10.1097/GOX.0000000000001873
Bonnecaze G, Chaput B, Filleron T, Al Hawat A, Vergez S, Chaynes P (2015) The frontal branch of the facial nerve: can we define a safety zone? Surg Radiol Anat 37(5):499–506
Cook BE, Lucarelli MJ, Lemke BN (2001) Depressor supercilii muscles: anatomy, histology, and cosmetic implications. Am J Surg 17(6):404–411
Starck WJ, Griffin JE Jr, Epker BN (1996) Objective evalua-tion of the eyelids and eyebrows after blepharoplasty. J Oral Maxillofac Surg 54(3):297–302
Frankel AS, Kamer FM (1997) The effect of blepharoplasty on eyebrow position. Arch Otolaryngol Head Neck Surg 123(4):393–396
Fagien S (1992) Eyebrow analysis after blepharoplasty in patients with brow ptosis. Ophthal Plast Reconstr Surg 8(3):210–214
Mokhtarzadeh A, Massry GG, Bitrian E et al (2017) Quantitative efficacy of external and internal browpexy performed in conjunction with blepharoplasty. Orbit 36(2):102–109
Tyers AG (2006) Brow lift via the direct and trans-blepharoplasty approaches. Orbit 25(4):261–5
Mealey L, Bridgstock R, Townsend GC (1999) Symmetry and perceived facial attractiveness: a monozygotic co-twin comparison. J Pers Soc Psychol 76(1):151–158
Mühlbauer W, Holm C (1998) Eyebrow asymmetry: ways of correction. Aesthetic Plast Surg 22(5):366–371
Yalc¸inkaya E, Cingi C, So¨ken H, et al (2016) Aesthetic analysis of the ideal eyebrow shape and position. Eur Arch Oto-Rhino-Laryngology 273(2):305–310
Funding
The authors received no financial support for the research and authorship of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no conflicts of interest with respect to the authorship and publication of this article.
Informed Consent
Consent for publication of the work was received by all authors and co-authors.
Informed Consent
Informed consent regarding the use of patient images.
Human Rights
The study was approved by the Research Ethics Committee, CAAE no. 26796819.5.0000.5532, and registered in the Brazilian Clinical Trials Registry (REBEC) under no. RBR-75n8453 https://ensaiosclinicos.gov.br/rg/RBR-75n8453.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Silva, J.J.X., Vaz, R.T., Ohmuro, M.l. et al. Brow Lift Through The Upper Blepharoplasty Incision: Prospective Clinical Study. Aesth Plast Surg 47, 1851–1858 (2023). https://doi.org/10.1007/s00266-023-03548-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-023-03548-z