Abstract
Purpose
Double-level osteotomy (DLO) for knee osteoarthritis is becoming increasingly popular to achieve superior anatomical correction. This study aimed to compare the indication for open-wedge high tibial osteotomy (OWHTO) and DLO and to investigate preoperative bone morphology.
Methods
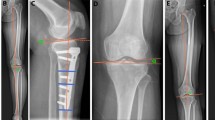
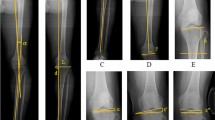
Data of 166 knees treated with osteotomy were evaluated. The weight-bearing line ratio, mechanical lateral distal femoral angle (mLDFA), and mechanical medial proximal tibial angle (mMPTA) were measured. Bone deformity assessment and osteotomy simulation were conducted. Normal values of mLDFA and mMPTA were defined as 85–90°. Bone deformity was classified into four patterns: femoral, tibial, both, and no deformity. Simulation was performed to achieve a postoperative weight-bearing line ratio of 62%. Distal femoral osteotomy (DFO) or OWHTO was performed to achieve an mLDFA of 85° or mMPTA of up to 95°. If the postoperative parameter remained outside the correctable limit, DLO was performed. Cases were classified according to the corrective surgery performed, and those that could not be corrected after DLO were classified into the uncorrectable group.
Results
Femoral, tibial, both, and no deformities were observed in 14.2%, 37.8%, 10.7%, and 33.9% of cases, respectively. No cases were classified into the DFO group; however, 53.6%, 38.1%, and 8.3% were classified into the OWHTO, DLO, and uncorrectable groups, respectively.
Conclusion
Bone deformity differed among cases, and only one-third had tibial deformity. OWHTO and DLO were indicated in approximately 50% and 40% of cases, respectively. Our study results reinforce the importance of evaluating leg morphology before surgical planning to achieve acceptable alignment.





Similar content being viewed by others
Data Availability
Raw data were generated from electronical records of the medical center. Due to confidentiality and concerns, the raw data used in this study is not publicly available. Derived data supporting the findings of this study are available from the corresponding author on request.
Change history
03 June 2024
A Correction to this paper has been published: https://doi.org/10.1007/s00264-024-06232-2
References
Belsey J, Yasen SK, Jobson S, Faulkner J, Wilson AJ (2021) Return to physical activity after high tibial osteotomy or unicompartmental knee arthroplasty: a systematic review and pooling data analysis. Am J Sports Med 49:1372–1380. https://doi.org/10.1177/0363546520948861
Hoorntje A, Witjes S, Kuijer P, Koenraadt KLM, van Geenen RCI, Daams JG, Getgood A, Kerkhoffs G (2017) High rates of return to sports activities and work after osteotomies around the knee: a systematic review and meta-analysis. Sports Med 47:2219–2244. https://doi.org/10.1007/s40279-017-0726-y
Alves P, van Rooij F, Kuratle T, Saffarini M, Miozzari H (2022) Consistent indications, targets and techniques for double-level osteotomy of the knee: a systematic review. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-06915-6
Staubli AE, De Simoni C, Babst R, Lobenhoffer P (2003) TomoFix: a new LCP-concept for open wedge osteotomy of the medial proximal tibia–early results in 92 cases. Injury 34(Suppl 2):B55-62. https://doi.org/10.1016/j.injury.2003.09.025
Khakha RS, Bin Abd Razak HR, Kley K, van Heerwaarden R, Wilson AJ (2021) Role of high tibial osteotomy in medial compartment osteoarthritis of the knee: Indications, surgical technique and outcomes. J Clin Orthop Trauma 23:101618. https://doi.org/10.1016/j.jcot.2021.101618
Akamatsu Y, Kumagai K, Kobayashi H, Tsuji M, Saito T (2018) Effect of Increased Coronal Inclination of the Tibial Plateau After Opening-Wedge High Tibial Osteotomy. Arthroscopy 34(7):2158–2169.e2
Nakayama H, Schroter S, Yamamoto C, Iseki T, Kanto R, Kurosaka K, Kambara S, Yoshiya S, Higa M (2018) Large correction in opening wedge high tibial osteotomy with resultant joint-line obliquity induces excessive shear stress on the articular cartilage. Knee Surg Sports Traumatol Arthrosc 26:1873–1878. https://doi.org/10.1007/s00167-017-4680-x
Kim GW, Kang JK, Song EK, Seon JK (2021) Increased joint obliquity after open-wedge high tibial osteotomy induces pain in the lateral compartment: a comparative analysis of the minimum 4-year follow-up outcomes using propensity score matching. Knee Surg Sports Traumatol Arthrosc 29:3495–3502. https://doi.org/10.1007/s00167-020-06342-5
Song JH, Bin SI, Kim JM, Lee BS (2020) What is an acceptable limit of joint-line obliquity after medial open wedge high tibial osteotomy? analysis based on midterm results. Am J Sports Med 48:3028–3035. https://doi.org/10.1177/0363546520949552
Nakayama H, Iseki T, Kanto R, Kambara S, Kanto M, Yoshiya S, Schroter S (2020) Physiologic knee joint alignment and orientation can be restored by the minimally invasive double level osteotomy for osteoarthritic knees with severe varus deformity. Knee Surg Sports Traumatol Arthrosc 28:742–750. https://doi.org/10.1007/s00167-018-5103-3
Nakamura R, Kuroda K, Takahashi M, Katsuki Y (2022) Open wedge high tibial osteotomy with pes anserinus preservation and insertion of bone substitutes. Arthrosc Tech 11:e69–e78. https://doi.org/10.1016/j.eats.2021.09.002
Kumagai K, Fujimaki H, Yamada S, Nejima S, Matsubara J, Inaba Y (2021) Difference in the early postoperative change of the joint line convergence angle between opening wedge and closed wedge high tibial osteotomies. J Orthop Surg Res 16:66. https://doi.org/10.1186/s13018-021-02214-x
Abs A, Micicoi G, Khakha R, Escudier JC, Jacquet C, Ollivier M (2023) Clinical and radiological outcomes of double-level osteotomy versus open-wedge high tibial osteotomy for bifocal varus deformity. Orthop J Sports Med 11:23259671221148456. https://doi.org/10.1177/23259671221148458
Akamatsu Y, Kobayashi H, Nejima S, Schroter S (2022) Can double-level osteotomy prevent patellofemoral osteoarthritis progression compared with open wedge high tibial osteotomy? Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-022-04523-0
Schroter S, Ihle C, Mueller J, Lobenhoffer P, Stockle U, van Heerwaarden R (2013) Digital planning of high tibial osteotomy. Interrater reliability by using two different software. Knee Surg Sports Traumatol Arthrosc 21:189–196. https://doi.org/10.1007/s00167-012-2114-3
Feucht MJ, Winkler PW, Mehl J, Bode G, Forkel P, Imhoff AB, Lutz PM (2021) Isolated high tibial osteotomy is appropriate in less than two-thirds of varus knees if excessive overcorrection of the medial proximal tibial angle should be avoided. Knee Surg Sports Traumatol Arthrosc 29:3299–3309. https://doi.org/10.1007/s00167-020-06166-3
Paley D, Herzenberg JE, Fautetsworth K, Tetsworth K, McKie J, Bhave A (1994) Deformity planning for frontal and sagittal plane corrective osteotomies. Orthop Clin North Am 25(3):425–465
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16:494–502
Smith JO, Wilson AJ, Thomas NP (2013) Osteotomy around the knee: evolution, principles and results. Knee Surg Sports Traumatol Arthrosc 21:3–22. https://doi.org/10.1007/s00167-012-2206-0
Paley D (2002) Priciples of deformity correction. Springer, New York
Benjamin A (1969) Double osteotomy for the painful knee in rheumatoid arthritis and osteoarthritis. J Bone Joint Surg Br 51:694–699
Babis GC, An KN, Chao EY, Rand JA, Sim FH (2002) Double level osteotomy of the knee: a method to retain joint-line obliquity. clinical results. J Bone Joint Surg Am 84:1380–1388. https://doi.org/10.2106/00004623-200208000-00013
Akamatsu Y, Nejima S, Tsuji M, Kobayashi H, Muramatsu S (2022) Joint line obliquity was maintained after double-level osteotomy, but was increased after open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 30:688–697. https://doi.org/10.1007/s00167-020-06430-6
Iseki T, Onishi S, Kanto M, Kanto R, Kambara S, Yoshiya S, Tachibana T, Nakayama H (2021) Double-level osteotomy for severe varus osteoarthritic knees can prevent change in leg length and restore physiological joint geometry. Knee 31:136–143. https://doi.org/10.1016/j.knee.2021.04.011
Kobayashi H, Akamatsu Y, Kumagai K, Kusayama Y, Aratake M, Saito T (2017) Influence of coronal bowing on the lower alignment and the positioning of component in navigation and conventional total knee arthroplasty. Orthop Traumatol Surg Res 103:251–256. https://doi.org/10.1016/j.otsr.2016.11.017
Urabe K, Mahoney OM, Mabuchi K, Itoman M (2008) Morphologic differences of the distal femur between Caucasian and Japanese women. J Orthop Surg (Hong Kong) 16:312–315. https://doi.org/10.1177/230949900801600309
Kuriyama S, Watanabe M, Sekiguchi K, Nakamura S, Nishitani K, Ito H, Matsuda S (2021) Differences in impact on adjacent compartments in medial unicompartmental knee arthroplasty versus high tibial osteotomy with identical valgus alignment. Knee 29:241–250. https://doi.org/10.1016/j.knee.2021.02.017
Micicoi G, Khakha R, Kley K, Wilson A, Cerciello S, Ollivier M (2020) Managing intra-articular deformity in high Tibial osteotomy: a narrative review. J Exp Orthop 7:65. https://doi.org/10.1186/s40634-020-00283-1
Tsuji M, Akamatsu Y, Kobayashi H, Mitsugi N, Inaba Y, Saito T (2020) Joint line convergence angle predicts outliers of coronal alignment in navigated open-wedge high tibial osteotomy. Arch Orthop Trauma Surg 140:707–715. https://doi.org/10.1007/s00402-019-03245-0
Ogawa H, Matsumoto K, Ogawa T, Takeuchi K, Akiyama H (2016) Preoperative varus laxity correlates with overcorrection in medial opening wedge high tibial osteotomy. Arch Orthop Trauma Surg 136:1337–1342. https://doi.org/10.1007/s00402-016-2521-x
Katagiri H, Nakagawa Y, Miyatake K, Ohara T, Shioda M, Sekiya I, Koga H (2023) Short-term outcomes after high tibial osteotomy aimed at neutral alignment combined with arthroscopic centralization of medial meniscus in osteoarthritis patients. J Knee Surg 36:261–268
Kannan A, Hawdon G, McMahon SJ (2012) Effect of flexion and rotation on measures of coronal alignment after TKA. J Knee Surg 25:407–410. https://doi.org/10.1055/s-0032-1313756
Brouwer RW, Jakma TS, Brouwer KH, Verhaar JA (2007) Pitfalls in determining knee alignment: a radiographic cadaver study. J Knee Surg 20:210–215. https://doi.org/10.1055/s-0030-1248045
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Shu Takagawa, Kunihito Hirotomi and Shota Higashihira. The first draft of the manuscript was written by Shu takagawa, Yohei Yukizawa, Yutaka Inaba, Naomi Kobayashi and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Yokohama city university (1/30/2023/ F221200007).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
The authors affirm that human research participants provided informed consent for publication of the images in Figs. 1 and 3.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original version of this article was revised. The correct name should be Shota Higashihira and not Shota Hiagashihra.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Takagawa, S., Yukizawa, Y., Hirotomi, K. et al. Comparison of the indications for high tibial osteotomy and double-level osteotomy for the correction of diverse lower-leg deformities in an Asian population with medial compartment osteoarthritis: a retrospective observational study. International Orthopaedics (SICOT) (2024). https://doi.org/10.1007/s00264-024-06218-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00264-024-06218-0