Abstract
Diagnosis of hip osteoarthritis (OA) is based on clinical arguments, and medical imaging is obtained to confirm the diagnosis and rule out other possible sources of pain. Conventional radiographs are recommended as the first line imaging modality to investigate chronic hip pain. They should be obtained in a rigorous technique that includes an antero-posterior (AP) radiograph of the pelvis. The choice of the appropriate lateral view depends on the clinical indication, Lequesne’s false profile being valuable in the assessment of OA. Magnetic resonance imaging (MRI) is more sensitive to detect joint effusion/synovitis, cartilage, labral, and bone marrow lesions. However, structural joint changes are frequent in asymptomatic population and neither radiographs nor MRI have shown a good correlation with pain and functional impairment. MRI seems to be more suitable than radiographs as a biomarker for clinical trials addressing early OA. The absence of a validated MR biomarker of early OA, together with issues related to machine availability and MRI protocol repeatability, prevent the widespread use of MRI in clinical trials.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hip osteoarthritis (OA) is a highly prevalent and disabling disorder that affects elderly but also young patients with a high socio-economic burden [1,2,3,4,5,6,7]. In patients with clinically suspected hip OA, medical imaging contributes to confirm the diagnosis and rule out alternative diagnoses by demonstrating cartilage lesions and associated structural changes [8]. For decades, conventional radiography (CR) has been used to support the clinical diagnosis of hip OA. Over the years, magnetic resonance imaging (MRI) emerged as a powerful imaging modality to detect cartilage lesions and structural changes of the hip joint. The current special issue of Skeletal Radiology granted us the opportunity to address a fundamental question: is radiography still needed to diagnose hip OA? Which imaging modality should be used to diagnose stage and quantify hip OA in clinical practice, in clinical trials and in research? After a brief review on classifications and diagnostic criteria, the current narrative article will summarize strengths and weaknesses of CR and MRI to diagnose hip OA and will propose perspectives on the use of medical imaging. This review article also highlights the importance of rigorous acquisition and reading of hip radiographic and MR images. Imaging of femoro-acetabular impingement (FAI) and advanced quantitative MR techniques for the cartilage are out of the scope of this article and will be addressed separately in this Skeletal Radiology issue.
Classification systems of hip osteoarthritis
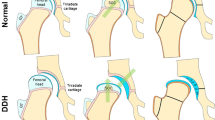
Hip OA can be classified according to its etiology, time of onset, severity, and clinical course. In primary hip OA, cartilage degradation can either be idiopathic or develop in association with dynamic conflict between the articular surfaces, the FAI syndrome [9,10,11] (Fig. 1). In secondary hip OA, joint degradation results from preexisting conditions including developmental hip dysplasia, growth-associated disorders, fracture, femoral head osteonecrosis and inflammatory or metabolic synovial disorders [10, 12,13,14,15,16,17] (Fig. 2). Early-onset and late-onset disease develop either before or after 50 years of age [2]. Early-stage and late-stage OA differ according to the absence or presence of radiological structural changes with a joint space width (JSW) of more or less than 2 mm on AP pelvic radiographs [18,19,20] (Fig. 3). The clinical course of hip OA is usually slow and pain fluctuates over the years with no or minor radiological changes over time [21] (Fig. 4). Rapidly destructive hip OA is uncommon and is defined by the development of complete loss of radiological JSW or severe bone attrition on CR within 12 months after symptoms onset [22,23,24] (Fig. 5). All these classification systems and threshold values are open for discussion, but they rely on good clinical practice standards for which preservative hip surgery should not be performed after 50 years of age or when the radiological JSW is < 2 mm.
A 21-year-old man with moderate left hip pain and osteoarthritis secondary to femoro-acetabular impingement. A AP radiograph demonstrates lateral joint space narrowing (arrows), subchondral sclerosis of the acetabular roof (asterisk) and femoral head osteophytes (arrowheads). B The 45° Dunn lateral view demonstrates Cam deformity at the head-neck junction (arrow)
Secondary hip osteoarthritis. A AP radiograph of the left hip in an 8-year-old boy with Legg-Calvé-Perthes disease showing sclerosis of the femoral head epiphysis (asterisk) and cystic changes of the metaphysis (arrow). B Follow-up AP radiograph of the same patient at the age of 23 years showing secondary osteoarthritis with abnormal femoral head contours, articular incongruity, and joint space narrowing
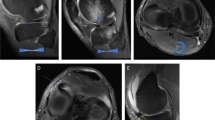
A 38-year-old woman with right hip pain and osteoarthritis. A Anteroposterior radiograph shows cortical buttressing (arrow) with a preserved joint space width (Kellgren 1). B Lequesne false profile shows narrowing of the antero-superior joint space (arrows). C Transverse T1 and D sagittal intermediate-weighted fat suppressed MR arthrography images after intra-articular contrast injection show full-thickness cartilage substance loss in the anterior (arrows in C) and superior (arrows in D) aspect of the joint space, with subchondral cyst-like changes (asterisks in D)
Non-evolutive osteoarthritis of the left hip in a 62-year-old man with limited range of motion but no hip pain. A AP radiograph of the left hip demonstrates lateral joint space narrowing (arrows) and marginal osteophytes (arrowheads). B Follow-up radiograph after 10 years demonstrates no significant change in joint space narrowing. Outcome prediction on radiographs is unreliable. Note that the area underneath the osteophyte (asterisk) does not correspond to the articular joint space
65-year-old man with rapidly destructive osteoarthritis. A AP radiograph of the right hip obtained at onset of symptoms shows early osteophytes (arrowheads) but no joint space narrowing. B AP radiograph obtained 3 months later shows complete joint space narrowing (arrows) with deformity of the femoral head (arrowhead) and subchondral sclerosis (asterisk).
Clinical diagnosis of hip osteoarthritis
Clinical history
Typically, OA-associated hip pain evolves over time with initial intermittent activity-related or weight-bearing pain followed by constant pain, limited range of motion, and altered gait. Several population- or OA-based cohort studies have shown that, on average, there is little to no progression of complaints during a 10-year follow-up period [21, 25] Hip pain can be localized anteriorly, laterally or posteriorly but it may also be referred in the groin, the buttock, the thigh or the knee. A major clinical challenge is to recognize articular hip pain from peri-articular or non-hip-related pain [26,27,28,29,30,31].
Physical examination
Physical examination remains one of the most valuable tools physicians can use to diagnose hip OA. Upright and supine exam tests as well as provocative maneuvers have been developed to increase the likelihood that presenting symptoms originate from the hip joint [32,33,34,35]. Unfortunately, the accuracy of these tests varies with a wide range of sensitivity and specificity [33]. For example, the flexion-abduction and external rotation test had a sensitivity ranging from 41 to 97% and a specificity ranging from 18 to 100% [36]. Therefore, the specific application and interpretation of these clinical tests must be integrated in the context of the patient’s history.
Biological tests
Routine blood tests play little diagnostic role in hip OA, but they contribute to rule out alternative diagnoses. The American College of Rheumatology criteria provide a set of clinical, laboratory, and/or radiographic features to identify patients with OA and to distinguish them from patients with other diseases [37]. Many biological markers may be altered in severe hip OA as in inflammatory or immune-mediated articular disorders, but their use remains limited to research setting and are not used in clinical practice [38, 39].
Radiological diagnosis of hip osteoarthritis
Radiographic hip examination
Radiological workup of the hip includes at least an antero-posterior (AP) radiograph of the pelvis and a lateral radiograph of the hip. The pelvic radiograph provides an overview of the entire pelvic girdle and allows a comparative analysis of both hips, which enhances the detection of subtle bone and joint abnormalities [8, 40,41,42,43]. The pelvic AP radiograph should also be used to assess FAI-associated features since pelvic positioning can be controlled on the AP pelvic radiograph but not on the AP hip radiograph [44]. There is no clear consensus whether the JSW is better evaluated on weight-bearing (WB) or non-weight-bearing (nWB) AP pelvic radiographs [45,46,47,48]. The WB radiograph evaluates the pelvis in its anatomical position with a decrease in acetabular coverage and increase in posterior pelvic tilt in comparison to the nWB pelvic radiograph [49]. The WB radiograph has an overall decrease in image quality with a higher radiation dose, is less reproducible and does not provide additional joint space narrowing (JSN) than nWB radiographs, except in severe acetabular dysplasia and advanced OA [18, 50,51,52].
Lateral radiographs of the hip can be obtained with different degrees of pelvic rotation, hip abduction and flexion [40,41,42]. They provide variable lateral views of the proximal femur [42, 53]. In the setting of early-onset hip OA, the 45° Dunn lateral view offers the better view of the femoral-neck junction to measure Cam-associated features [44, 54, 55] (Fig. 1). The off-lateral view or false profile of Lequesne is the unique radiograph that provides an evaluation of the hip joint in a physiological position in a near sagittal plane [56, 57] enabling to assess anterior acetabular coverage and anterior or posterior JSW [58] (Fig. 6). The off-lateral view enables to detect more hips with JSN than the AP pelvic radiograph alone [58, 59].
Value of Lequesne’s false profile view in a 65-year-old man with mild hip pain after walking. A AP and B Lauenstein lateral radiographs demonstrate almost normal joint space and osteophytes (arrowheads). C Lequesne’s false profile demonstrates almost 50% joint space narrowing in the anterior aspect of the joint (arrows) that cannot be seen on the other radiographs
Normal hip radiograph
Radiographs of a normal hip joint may demonstrate some cortical irregularities and labral ossifications that should not be confused with OA-related structural bone changes [41, 60, 61]. The radiographic JSW corresponds to the distance between the acetabular roof and the femoral head, reflecting the combined thickness of the acetabular and femoral head cartilages [62]. Normal JSW varies from 2 to 7 mm among individuals with limited variability (< 1 mm) between both hips of the same individual [63]. The distance between the fovea capitis and the teardrop does not reflect articular cartilage thickness [62]. On a normal pelvic radiograph, the lateral JSW is larger than or equivalent to the medial JSW in 85% and 15% of cases, respectively [60]. The lateral JSW should not be thinner than the medial JSW except in arched acetabular roof and in ossified labrum [60]. On the Lequesne false profile view, the anterior JSW should always be larger than the posterior JSW [57, 64].
Abnormal radiographic joint space
Joint space narrowing (JSN) of the hip is the radiographic hallmark of late-stage hip OA but is absent in early-stage hip OA. Several patterns of predominant JSN have been recognized, most likely reflecting uneven advanced cartilage loss [62, 65, 66]. Predominant lateral or anterior JSN is the most frequent pattern and is associated with the CAM-type FAI. Predominant medial or posterior JSN is associated with the Pincer-type FAI [62, 66]. Predominant isolated supero-medial JSN can occasionally be seen in late-onset OA and in some secondary forms of hip OA. Good reproducibility and repeatability in the assessment of absent, possible, or definite JSN has been consistently demonstrated but the reproducibility can be influenced by methodological features [48, 67,68,69,70].
JSW can be reliably measured by using manual or computer-assisted methods, providing a continuous variable for cartilage evaluation [67, 69, 71]. JSW shows important inter-individual variations that limit its value to compare patients [63]. Serial JSW measurement can be used to track cartilage changes over time, and disease progression was defined as loss of JSW of ≥ 0.5–0.6 mm/year [48, 69, 72, 73]. JSW change over time seems to better correlate with hip symptoms than absolute JSW [67, 71, 73].
Radiographic structural changes
Structural bone changes on radiographs include subchondral sclerotic or cystic bone changes and osteophyte formation at the periphery of or at distance from the cartilage-covered articular surfaces. Osteophyte formation has received most attention in OA and is an important finding in Kellgren-Lawrence scoring system [74,75,76,77,78,79]. There is currently no accepted or validated definition for early OA [18]. In many clinical trials, hip OA is defined by a Kellgren-Lawrence grade ≥ 2 (definite JSN, definite osteophytes, and possible sclerosis) [74, 75, 80]. The strengths and weaknesses of these grading systems have been extensively addressed [81, 82].
MRI diagnosis of hip osteoarthritis
Hip MRI examination
The standard MRI protocol of the hip usually includes fat-sensitive and fat-saturated fluid-sensitive sequences with the highest spatial resolution achievable which is higher at 3.0 than at 1.5 Tesla. Recommended imaging planes vary and include standard or oblique coronal, sagittal and transverse planes, radial imaging and 3D imaging [83,84,85]. Direct hip traction MR arthrography can also be performed for dedicated cartilage and labrum evaluation but is more invasive than standard MRI due to the need for articular puncture and hip traction.
MRI of the hip cartilage
In fact, MRI of hip cartilage reached maturity later than that of knee cartilage due to several technical challenges that are specific to the hip. Meta-analyses demonstrated a lower accuracy of conventional MRI for the detection of cartilage defects at the hip than at the knee [86, 87]. Technical challenges for hip cartilage MRI include (a) deep and eccentric location of the hip, (b) absence of dedicated hip coils (c) thinness of the hip cartilage, (d) high congruency of the articular surfaces with no fluid between the two hyaline cartilage surfaces [18, 88], and (e) complex anatomy with partial volume artifacts. MRI can demonstrate focal morphological changes of the cartilage, like signal alteration, substance loss, and delamination, before radiographic JSN occurs [89, 90] (Fig. 3). Cartilage defect may represent early biomarker for OA [89]. Compositional and quantitative MRI techniques of the cartilage add some insights into the sequence and rate of articular cartilage changes at the hip that precede overt hip OA [91].
MRI structural changes in hip osteoarthritis
Besides the depiction of hyaline and labral cartilage changes, conventional MRI depicts structural bone changes including bone marrow edema (BME)- and sclerosis-like signal changes along with joint effusion and synovitis [89, 92,93,94,95]. Osteophytes and subcortical cysts are more conspicuous at MRI than at CR because of its multiplanar capacity. MRI, a powerful diagnostic tool in OA imaging, has dramatically changed our understanding of OA that evolved from a cartilage-centered disease to a whole joint organ disease. This new approach of OA offers potentials for early diagnosis and outcome measures for new treatments [90, 94]. However, there is currently no accepted or validated definition of hip OA based on MRI [18]. Several semi-quantitative scoring systems based on location and severity of articular changes have been developed and validated for hip MRI in clinical trials and research including (1) Scoring Hip osteoarthritis with MRI (SHOMRI), (2) Hip OA MRI Scoring System (HOAMS), and (3) Hip Inflammation MRI Scoring System (HIMRISS) [94, 96,97,98,99,100].
Strengths and weaknesses of clinical, radiographic and MRI hip examinations in the setting of suspected hip osteoarthritis
Clinical examination
Clinical examination of the hip of patients with suspected early-stage hip OA is feasible, available, and repeatable with a moderate interobserver reproducibility [101]. Its accuracy is acceptable when findings are integrated with past medical history and present clinical history, in the absence of clinical red flags [33, 102]. Exclusion of all red flags is mandatory to accept a presumptive diagnosis of hip OA [45]. A major weakness of clinical examination is its low sensitivity for detecting early-onset and early-stage hip OA. Clinical examination does not provide any staging system or predictive information but can be used to monitor disease progression (Table 1).
Radiographic examination
Radiological examination of the hip of patients with suspected OA is feasible, available, and repeatable with an acceptable moderate interobserver reproducibility [67, 103]. Despite some variations in radiological practices, the radiographic technique is well documented and reproducible among institutions and over time. Long-term follow-up radiographs can be compared with initial films. Contra-indications for pelvic radiographs are negligible. In the setting of hip OA, pelvic radiographs are easily interpreted by radiologists and clinicians. It yields valuable information to differentiate primary from secondary OA and to detect FAI-associated anatomical features.
Pelvic radiography has poor sensitivity in the detection of many soft tissue, bone, and joint changes [104, 105] and therefore has limited value for ruling out alternative disorders. In the setting of hip OA, radiographs are insensitive to compositional and early structural changes; JSW measurement is insufficient to assess articular cartilage. Deep cartilage defects can be observed at MRI despite normal radiographic JSW of that hip [89] (Fig. 3). Given these limitations, CR does not fulfill the mandatory requirements to become a valuable biomarker of early OA in clinical trials [80, 95, 103, 106].
Radiological-clinical discordances have been frequently observed; hips with radiographic OA may remain asymptomatic and, conversely, painful hips due to early OA may not show radiographic signs of OA [107, 108] (Fig. 7). Intensity of symptoms fairly correlates with radiological staging of OA [109, 110]. In addition to these radio-clinical dissociations at an early stage, radiographic hip OA progression poorly correlates with pain progression [111]. Early radiographic changes also lack predictive values for the development of clinical hip OA at 5–10 years follow-up in large patients cohorts [25, 112]. Change in JSW seems to better correlate with symptoms than the absolute JSW at a given moment (Table 1).
Hypothetical Venn diagram illustrating the lack of coherence between pain, clinical examination, and imaging findings in patients with A presumed hip osteoarthritis and B femoral neck fracture. The shaded area represents the proportion of patients in whom all three parameters are present. In OA, discordance between symptoms, clinical examination, and imaging findings are frequent. In femoral neck fractures, the three parameters are overlapping
MRI examination
Hip MRI is worthwhile feasible with some limitations in availability. In the setting of early OA, a high-resolution hip MRI examination is needed and is the most accurate imaging modality to rule out alternative diagnoses and to diagnose and stage hip OA. Hip MR arthrography with hip traction is more accurate than standard MRI for the depiction of cartilage changes indicating some limitations in the accuracy of non-arthrographic MRI [113]. The interpretation of hip MRI by non-expert radiologists and clinicians remains to be validated in the setting of OA. Variations in local radiological equipment and practices may limit its use in large multi-center studies. Constant improvement in image quality, the availability of new MR sequences and advanced image post-processing might represent a challenge when evaluation long term hip changes at future MRI examinations.
MRI clinical discordances have been seen. Hips with cartilage lesions at MRI may remain asymptomatic, and symptomatic hips may show no signs of OA at MRI [114]. OA-related MRI lesions can also be observed in asymptomatic volunteers [114, 115]. Some hip changes moderately correlate symptoms, including femoral head BME, synovitis/effusion, and muscle atrophy [93, 116]. The severity of BME could correlate that of pain and number of microfractures [93]. to the best of our knowledge, the prevalence and rates of progression of hip changes in OA have not been established yet at MRI [91]. It is therefore not surprising that some clinical trial organisators are reluctant in introducing MRI at inclusion or as a biomarker due to limitations in its interpretation and/or overlapping findings between symptomatic and asymptomatic hips (Table 1).
A plea for CR as first-line imaging modality in clinically suspected hip osteoarthritis
Rising healthcare costs is a major concern in both the political and medical professions with diagnostic imaging representing one of the fastest rising cost segments worldwide. There is a need for value-driven diagnostic algorithms and decreasing unnecessary diagnostic testing that may not alter the course of patients’ management can efficiently reduce healthcare costs [117].
In patients aged above 50 years and hip symptoms suggestive of OA, scientific associations recommend to obtain pelvic and hip CR as the first-line imaging modality [8, 27, 45, 102, 118,119,120,121]. However, cost-effectiveness studies assessing the value of hip radiographs in patients with suspected hip OA indicated a variable impact on patient’s management. As a matter of fact, a presumptive clinical diagnosis of hip OA could be accepted without requiring medical imaging in patients > 50 years without previous relevant medical history as long as symptoms and clinical examination at onset and clinical course at follow-up remain consistent with this diagnosis [45]. A trend in a more comprehensive approach of patients with age-associated articular pain further supports a declining role of medical imaging, in the absence of red flags at onset and of unexpected clinical evolution. A recent study demonstrated that psychological and behavioral characteristics of patients with hip pain better correlated with hip pain than any arthroscopically demonstrated hip lesion [122]. To the best of our knowledge, we are not aware of any validated recommendation proposing hip MRI as the first imaging modality for suspected hip OA in patients aged >50 years. Cost-effectiveness studies in several MSK disorders including OA assessing the value of MRI on patient management demonstrated a significant increase in cost without any therapeutic effect [117, 123].
In patients aged below 50 years of age and presumed hip OA, numerous scientific associations also recommend to obtain conventional radiographs of the hip as the first-line imaging modality without any delay [45, 55, 120, 124, 125]. Studies assessing cost-effectiveness of radiographs are lacking as hip radiographs are used for patient inclusion. Currently, the medical community is still awaiting the multi-center confirmation that preservative hip surgery in young patients with FAI-related disorders is a disease modifying intervention. In case of reliable positive results, MRI could be obtained as second-line imaging modality if MRI yields independent markers to select patients who would benefit from surgery. Cost-effectiveness analysis of hip MRI in the setting of FAI will then become mandatory.
Perspectives that would favor the use of MRI as first-line imaging modality
A currently not foreseen increase in MRI equipment availability and decrease in examination time duration and cost would be mandatory to significantly change patient’s imaging workflow. Currently, in the absence of disease modifying drugs, healthcare system efforts focus on tertiary prevention of hip OA to soften the clinical and functional consequences and to postpone total hip replacement. Currently, there are no proven disease modifying drugs approved by the regulatory agencies and, therefore, the impact of early detection of OA is limited. The availability of disease modifying drugs and of MRI biomarkers that would enable to select patients who are likely to benefit from these drugs would definitely support the use of MRI as a screening tool. Cost-effectiveness studies would then be of value once the cost of these disease modifying drugs would be determined. (Tables 2 and 3).
Currently, hip MRI is considered to be the most sensitive non-invasive imaging modality that enables to assess local pre-OA changes and is the best imaging modality to assess time- and drug-related changes in radiological studies. However, clinical trial organisators are reluctant in including hip MRI in large clinical trials partly because MRI biomarkers are also found in asymptomatic subjects. The lack of a consensus on what represents early hip OA severely limits the feasibility of clinical trials with difficulties in creating homogeneous patients’ subsets for the purpose of clinical studies. Time has come to assess the value of MRI biomarkers, e.g., cartilage volume and composition, effusion-synovitis, and bone marrow edema-like signal intensity, in population-cohorts’ studies.
Conclusion
Hip OA is a heterogeneous group of hip disorders with fluctuating symptoms over time and slow progression of radiographic changes. Pelvic/hip CR is the recommended first-line imaging modality to be obtained in the setting of suspected hip OA with some debate on the moment at which it should be performed during the disease course. MRI is the gold standard imaging technique in early OA. The absence of accepted or validated reference standard for early-stage hip OA, the presence of dissociation between symptoms, clinical evaluation and imaging findings along with absence of disease-modifying drugs in hip OA remain challenging in clinical and research practice. CR should be obtained at inclusion in clinical trials including patients with early-stage OA, but possibly has limited outcome significance. MRI has a lot to offer both at patient inclusion and as primary or secondary outcome biomarker.
Abbreviations
- AP:
-
Antero-posterior
- BME:
-
Bone marrow edema-like
- CR:
-
Conventional radiography
- FAI:
-
Femoro-acetabular impingement
- JSN:
-
Joint space narrowing
- JSW:
-
Joint space width
- MRI:
-
Magnetic resonance imaging
- nWB:
-
Non-weight-bearing
- OA:
-
Osteoarthritis
- WB:
-
Weight-bearing
References
Felson DT, Naimark A, Anderson J, Kazis L, Castelli W, Meenan RF. The prevalence of knee osteoarthritis in the elderly The Framingham Osteoarthritis Study. Arthritis Rheum. 1987;30:914–8.
Kim C, Linsenmeyer KD, Vlad SC, et al. Prevalence of radiographic and symptomatic hip osteoarthritis in an urban United States community: the Framingham osteoarthritis study. Arthritis Rheumatol Hoboken NJ. 2014;66:3013–7.
Dagenais S, Garbedian S, Wai EK. Systematic review of the prevalence of radiographic primary hip osteoarthritis. Clin Orthop. 2009;467:623–37.
Jordan JM, Helmick CG, Renner JB, et al. Prevalence of hip symptoms and radiographic and symptomatic hip osteoarthritis in African-Americans and Caucasians: The Johnston County Osteoarthritis Project. J Rheumatol. 2009;36:809–15.
Murphy LB, Helmick CG, Schwartz TA, et al. One in four people may develop symptomatic hip osteoarthritis in his or her lifetime. Osteoarthritis Cartilage. 2010;18:1372–9.
Culliford DJ, Maskell J, Kiran A, et al. The lifetime risk of total hip and knee arthroplasty: results from the UK general practice research database. Osteoarthr Cartil. 2012;20:519–24.
Fu M, Zhou H, Li Y, Jin H, Liu X. Global, regional, and national burdens of hip osteoarthritis from 1990 to 2019: estimates from the 2019 Global Burden of Disease Study. Arthritis Res Ther. 2022;24:8.
Expert Panel on Musculoskeletal Imaging Mintz DN, Roberts CC, Bencardino JT, Baccei SJ, Caird MS, et al. ACR Appropriateness Criteria® Chronic Hip Pain. J Am Coll Radiol JACR. 2017;14:90–102.
Ganz R, Parvizi J, Beck M, Leunig M, Nötzli H, Siebenrock KA. Femoroacetabular impingement: A cause for osteoarthritis of the hip. Clin Orthop. 2003;112–20.
Ganz R, Leunig M, Leunig-Ganz K, Harris WH. The etiology of osteoarthritis of the hip. Clin Orthop. 2008;466:264–72.
Matsumoto K, Ganz R, Khanduja V. The history of femoroacetabular impingement Bone Jt Res. Br Editorial Soc Bone Joint Surg. 2020;9:572–7.
Lespasio MJ, Sultan AA, Piuzzi NS, et al. Hip Osteoarthr: Prim Perm J. 2018;22:17–084.
Sandiford N, Kendoff D, Muirhead-Allwood S. Osteoarthritis of the hip: aetiology, pathophysiology and current aspects of management. Ann Jt [Internet]. AME Publishing Company; 2020 [cited 2022 Aug 20];5. Available from: https://aoj.amegroups.com/article/view/5539.
Harris WH. Etiology of osteoarthritis of the hip. Clin Orthop. 1986;20–33.
Weinstein SL. Natural history of congenital hip dislocation (CDH) and hip dysplasia. Clin Orthop. 1987;62–76.
Lloyd-Roberts GC. Osteoarthritis of the hip; a study of the clinical pathology. J Bone Joint Surg Br. 1955;37-b:8–47.
Klaue K, Durnin CW, Ganz R. The acetabular rim syndrome a clinical presentation of dysplasia of the hip. J Bone Joint Surg Br. 1991;73:423–9.
Gold GE, Cicuttini F, Crema MD, et al. OARSI Clinical Trials recommendations: hip imaging in clinical trials in osteoarthritis. Osteoarthr Cartil. 2015;23:716–31.
Jacobsen S, Sonne-holm S, Søballe K, Gebuhr P, Lund B. Hip dysplasia and osteoarthrosis. Acta Orthop Taylor & Francis. 2005;76:149–58.
Jacobsen S, Rømer L, Søballe K. Degeneration in dysplastic hips. Skeletal Radiol. 2005;34:778–84.
van Berkel AC, Schiphof D, Waarsing JH et al. Course of pain and fluctuations in pain related to suspected early hip osteoarthritis: the CHECK study. Fam Pract. 2022;cmac030.
Della Torre P, Picuti G, Di Filippo P. Rapidly progressive osteoarthritis of the hip. Ital J Orthop Traumatol. 1987;13:187–200.
Depuyt F. Van Holsbeeck M [Rapidly destructive coxarthrosis: case study and literature review]. J Belge Radiol. 1990;73:207–10.
Rosenberg ZS, Shankman S, Steiner GC, Kastenbaum DK, Norman A, Lazansky MG. Rapid destructive osteoarthritis: clinical, radiographic, and pathologic features. Radiol Radiol Soc North Am. 1992;182:213–6.
Runhaar J, Özbulut Ö, Kloppenburg M, Boers M, Bijlsma JWJ, Bierma-Zeinstra SMA. Diagnostic criteria for early hip osteoarthritis: first steps, based on the CHECK study. Rheumatol Oxf Engl. 2021;60:5158–64.
Cibulka MT, White DM, Woehrle J, et al. Hip pain and mobility deficits – hip osteoarthritis. J Orthop Sports Phys Ther. 2009;39:A1-25.
Cibulka MT, Bloom NJ, Enseki KR, Macdonald CW, Woehrle J, McDonough CM. Hip Pain and mobility deficits—hip osteoarthritis: Revision 2017. J Orthop Sports Phys Ther J Orthopaedic Sports Phys Ther. 2017;47:A1-37.
Enseki K, Harris-Hayes M, White DM, et al. Nonarthritic hip joint pain J Orthop Sports Phys Ther. J Orthopaedic Sports Phys Ther. 2014;44:A1-32.
Ariani A, Manara M, Fioravanti A, et al. The Italian Society for Rheumatology clinical practice guidelines for the diagnosis and management of knee, hip and hand osteoarthritis. Reumatismo. 2019;71:5–21.
Lesher JM, Dreyfuss P, Hager N, Kaplan M, Furman M. Hip Joint pain referral patterns: a descriptive study. Pain Med. 2008;9:22–5.
Battaglia PJ, D’Angelo K, Kettner NW. Posterior, lateral, and anterior hip pain due to musculoskeletal origin: a narrative literature review of history, physical examination, and diagnostic imaging. J Chiropr Med. 2016;15:281–93.
Metcalfe D, Perry DC, Claireaux HA, Simel DL, Zogg CK, Costa ML. Does This Patient have hip osteoarthritis?: the rational clinical examination systematic review. JAMA. 2019;322:2323–33.
Reiman MP, Goode AP, Hegedus EJ, Cook CE, Wright AA. Diagnostic accuracy of clinical tests of the hip: a systematic review with meta-analysis. Br J Sports Med BMJ Publ Group Ltd Br Assoc Sport Exerc Med. 2013;47:893–902.
Reiman MP, Mather RC, Cook CE. Physical examination tests for hip dysfunction and injury Br J Sports Med. BMJ Publ Group Ltd Br Assoc Sport and Exerc Med. 2015;49:357–61.
Martin HD, Palmer IJ. History and physical examination of the hip: the basics. Curr Rev Musculoskelet Med. 2013;6:219–25.
Tijssen M, van Cingel R, Willemsen L, de Visser E. Diagnostics of Femoroacetabular impingement and labral pathology of the hip: a systematic review of the accuracy and validity of physical tests. Arthroscopy Elsevier. 2012;28:860–71.
Altman R, Alarcón G, Appelrouth D, Bloch D, et al. The American College of Rheumatology criteria for the classification and reporting of osteoarthritis of the hip. Arthritis Rheum. 1991;34:505–14.
Nepple JJ, Thomason KM, An TW, Harris-Hayes M, Clohisy JC. What Is the Utility of Biomarkers for Assessing the Pathophysiology of Hip Osteoarthritis? A Systematic Review. Clin Orthop Relat Res. 2015;473:1683–701.
da Silva MR, Linhares D, Vasconcelos DM, et al. Neuroimmune expression in hip osteoarthritis: a systematic review. BMC Musculoskelet Disord. 2017;18:394.
Clohisy JC, Carlisle JC, Beaulé PE et al. A systematic approach to the plain radiographic evaluation of the young adult hip. J Bone Joint Surg Am. 2008;90(Suppl 4):47–66.
Mourad C, Omoumi P, Malghem J, Vande Berg BC. Conventional radiography of the hip revisited: correlation with advanced imaging. Magn Reson Imaging Clin N Am. 2019;27:661–83.
Manaster BJ. Adult chronic hip pain: radiographic evaluation. RadioGraphics. 2000;20:S3-25.
Welton KL, Jesse MK, Kraeutler MJ, Garabekyan T, Mei-Dan O. The Anteroposterior pelvic radiograph: acetabular and femoral measurements and relation to hip pathologies. J Bone Joint Surg Am. 2018;100:76–85.
Mascarenhas VV, Castro MO, Rego PA, et al. The Lisbon Agreement on Femoroacetabular Impingement Imaging—part 1: overview. Eur Radiol. 2020;30:5281–97.
Sakellariou G, Conaghan PG, Zhang W, et al. EULAR recommendations for the use of imaging in the clinical management of peripheral joint osteoarthritis. Ann Rheum Dis BMJ Publ Group Ltd. 2017;76:1484–94.
Flintham K, Alzyoud K, England A, Hogg P, Snaith B. Comparing the supine and erect pelvis radiographic examinations: an evaluation of anatomy, image quality and radiation dose. Br J Radiol Br Inst Radiol. 2021;94(1123):20210047.
Snaith B, Field L, Lewis EF, Flintham K. Variation in pelvic radiography practice: why can we not standardise image acquisition techniques? Radiogr Elsevier. 2019;25:374–7.
Auleley G-R, Duche A, Drape J-L, Dougados M, Ravaud P. Measurement of joint space width in hip osteoarthritis: influence of joint positioning and radiographic procedure. Rheumatology. 2001;40:414–9.
Pullen WM, Henebry A, Gaskill T. Variability of Acetabular coverage between supine and weightbearing pelvic radiographs. Am J Sports Med SAGE Publications Inc STM. 2014;42:2643–8.
Bessa FS, Williams BT, Polce EM, et al. No differences in hip joint space measurements between weightbearing or supine anteroposterior pelvic radiographs. Arthrosc J Arthrosc Relat Surg. 2020;36:2843–8.
Fuchs-Winkelmann S, Peterlein C-D, Tibesku CO, Weinstein SL. Comparison of pelvic radiographs in weightbearing and supine positions. Clin Orthop. 2008;466:809–12.
Troelsen A, Jacobsen S, Rømer L, Søballe K. Weightbearing anteroposterior pelvic radiographs are recommended in DDH assessment. Clin Orthop. 2008;466:813–9.
Eijer H, Leunig M, Mahomed MN, Ganz R. Cross-Table Lateral Radiographs for Screening of Anterior Femoral Head-Neck Offset in Patients with Femoro-Acetabular Impingement. HIP International. 2001;11(1):37–41.
Smith KM, Gerrie BJ, McCulloch PC, Lintner DM, Harris JD. Comparison of MRI, CT, Dunn 45° and Dunn 90° alpha angle measurements in femoroacetabular impingement. Hip Int J Clin Exp Res Hip Pathol Ther. 2018;28:450–5.
Schmaranzer F, Kheterpal AB, Bredella MA. Best practices: hip femoroacetabular impingement. Am J Roentgenol. 2021;216:585–98.
Lequesne M. De Seze [False profile of the pelvis. A new radiographic incidence for the study of the hip. Its use in dysplasias and different coxopathies]. Rev Rhum Mal Osteoartic. 1961;28:643–52.
Lequesne MG, Laredo J-D. The faux profil (oblique view) of the hip in the standing position Contribution to the evaluation of osteoarthritis of the adult hip. Ann Rheum Dis BMJ Publishing Group Ltd. 1998;57:676–81.
Damen J, Runhaar J, Kloppenburg M, Meijer R, Bierma-Zeinstra SMA, Oei EHG. Additional Value of different radiographic views on the identification of early radiographic hip and knee osteoarthritis and its progression: a cohort study. Arthritis Care Res. 2017;69:1644–50.
Conrozier T, Bochu M, Gratacos J, Piperno M, Mathieu P, Vignon E. Evaluation of the ‘Lequesne’s false profile’ of the hip in patients with hip osteoarthritis. Osteoarthr Cartil. 1999;7:295–300.
Omoumi P, Vande Berg B. Hip Imaging: normal variants and asymptomatic findings. Semin Musculoskelet Radiol. 2017;21:507–17.
Valente C, Haefliger L, Favre J, Omoumi P. Ossification of the acetabular rim: a highly prevalent finding in asymptomatic non-osteoarthritic hips of all ages. Eur Radiol. 2021;31:6802–9.
Resnick D. Patterns of migration of the femoral head in osteoarthritis of the hip Roentgenographic-pathologic correlation and comparison with rheumatoid arthritis. Am J Roentgenol Radium Ther Nucl Med. 1975;124:62–74.
Lequesne M, Malghem J, Dion E. The normal hip joint space: variations in width, shape, and architecture on 223 pelvic radiographs. Ann Rheum Dis. 2004;63:1145–51.
Laredo J-D, Wyler A, Alvarez C, Aout M, Lequesne M, Vicaut E. Diagnostic performance of bilateral false profile radiographs in early hip osteoarthritis. Joint Bone Spine. 2018;85:93–9.
Ledingham J, Dawson S, Preston B, Milligan G, Doherty M. Radiographic patterns and associations of osteoarthritis of the hip. Ann Rheum Dis BMJ Publishing Group Ltd. 1992;51:1111–6.
Solomon L. Patterns of osteoarthritis of the hip. J Bone Joint Surg Br. 1976;58:176–83.
Conrozier T, Brandt K, Piperno M, Mathieu P, Merle-Vincent F, Vignon E. Reproducibility and sensitivity to change of a new method of computer measurement of joint space width in hip osteoarthritis Performance of three radiographic views obtained at a 3-year interval. Osteoarthr Cartil Elsevier. 2009;17:864–70.
Maheu E, Cadet C, Marty M, et al. Reproducibility and sensitivity to change of various methods to measure joint space width in osteoarthritis of the hip: a double reading of three different radiographic views taken with a three-year interval. Arthritis Res Ther. 2005;7:R1375–85.
Gossec L, Jordan JM, Lam M-A, et al. Comparative evaluation of three semi-quantitative radiographic grading techniques for hip osteoarthritis in terms of validity and reproducibility in 1404 radiographs: report of the OARSI-OMERACT Task Force. Osteoarthr Cartil. 2009;17:182–7.
Goker B, Sancak A, Haznedaroglu S, Arac M, Block JA. The effects of minor hip flexion, abduction or adduction and x-ray beam angle on the radiographic joint space width of the hip. Osteoarthr Cartil. 2005;13:379–86.
Conrozier T, Tron AM, Mathieu P, Vignon E. Quantitative assessment of radiographic normal and osteoarthritic hip joint space. Osteoarthr Cartil. 1995;3(Suppl A):81–7.
Altman RD, Bloch DA, Dougados M et al. Measurement of structural progression in osteoarthritis of the hip: the Barcelona consensus group. Osteoarthritis Cartilage. 2004;12(7):515–24.
Dougados M, Gueguen A, Nguyen M, et al. Radiological progression of hip osteoarthritis: definition, risk factors and correlations with clinical status. Ann Rheum Dis. 1996;55:356–62.
Kellgren JH, Lawrence JS. Radiological assessment of osteo-arthrosis. Ann Rheum Dis. 1957;16:494–502.
Kohn MD, Sassoon AA, Fernando ND. Classifications in brief: Kellgren-Lawrence classification of osteoarthritis. Clin Orthop. 2016;474:1886–93.
Croft P, Cooper C, Wickham C, Coggon D. Defining osteoarthritis of the hip for epidemiologic studies. Am J Epidemiol. 1990;132:514–22.
Reijman M, Hazes JMW, Pols HaP, Bernsen RMD, Koes BW, Bierma-Zeinstra SMA. Validity and reliability of three definitions of hip osteoarthritis: cross sectional and longitudinal approach. Ann Rheum Dis BMJ Publishing Group Ltd. 2004;63:1427–33.
Busse J, Gasteiger W. Tönnis D [A new method for roentgenologic evaluation of the hip joint–the hip factor]. Arch Orthop Unfallchir. 1972;72:1–9.
Kovalenko B, Bremjit P, Fernando N. Classifications in brief: tönnis classification of hip osteoarthritis. Clin Orthop. 2018;476:1680–4.
Macri EM, Runhaar J, Damen J, Oei EHG, Bierma-Zeinstra SMA. Kellgren/Lawrence grading in cohort studies: methodological update and implications illustrated using data from a dutch hip and knee cohort. Arthritis Care Res. 2022;74:1179–87.
Terjesen T, Gunderson RB. Radiographic evaluation of osteoarthritis of the hip. Acta Orthop. 2012;83:185–9.
Theiler R, Stucki G, Schütz R, et al. Parametric and non-parametric measures in the assessment of knee and hip osteoarthritis: interobserver reliability and correlation with radiology. Osteoarthr Cartil. 1996;4:35–42.
Petchprapa CN, Dunham KS, Lattanzi R, Recht MP. Demystifying radial imaging of the hip. Radiogr Rev Publ Radiol Soc N Am Inc. 2013;33:E97–112.
Bellelli A, Silvestri E, Barile A, et al. Position paper on magnetic resonance imaging protocols in the musculoskeletal system (excluding the spine) by the Italian College of Musculoskeletal Radiology. Radiol Med (Torino). 2019;124:522–38.
Chang CY, Huang AJ. MR imaging of normal hip anatomy. Magn Reson Imaging Clin Elsevier. 2013;21:1–19.
Smith TO, Simpson M, Ejindu V, Hing CB. The diagnostic test accuracy of magnetic resonance imaging, magnetic resonance arthrography and computer tomography in the detection of chondral lesions of the hip. Eur J Orthop Surg Traumatol. 2013;23:335–44.
Smith TO, Drew BT, Toms AP, Donell ST, Hing CB. Accuracy of magnetic resonance imaging, magnetic resonance arthrography and computed tomography for the detection of chondral lesions of the knee. Knee Surg Sports Traumatol Arthrosc. 2012;20:2367–79.
Steppacher SD, Meier MK, Albers CE, Tannast M, Siebenrock KA. Acetabular Cartilage thickness differs among cam, pincer, or mixed-type femoroacetabular impingement: a descriptive study using in vivo ultrasonic measurements during surgical hip dislocation. Cartilage. 2021;13:465S-475S.
Teichtahl AJ, Wang Y, Smith S, et al. Structural changes of hip osteoarthritis using magnetic resonance imaging. Arthritis Res Ther. 2014;16:466.
Crema MD, Watts GJ, Guermazi A, Kim Y-J, Kijowski R, Roemer FW. A narrative overview of the current status of MRI of the hip and its relevance for osteoarthritis research - what we know, what has changed and where are we going? Osteoarthritis Cartilage. 2017;25:1–13.
Aguilar HN, Battié MC, Jaremko JL. MRI-based hip cartilage measures in osteoarthritic and non-osteoarthritic individuals: a systematic review. RMD Open. BMJ Specialist Journals; 2017;3:e000358.
Hayashi D, Roemer FW, Katur A, et al. Imaging of synovitis in osteoarthritis: current status and outlook. Semin Arthritis Rheum. 2011;41:116–30.
Taljanovic MS, Graham AR, Benjamin JB, et al. Bone marrow edema pattern in advanced hip osteoarthritis: quantitative assessment with magnetic resonance imaging and correlation with clinical examination, radiographic findings, and histopathology. Skeletal Radiol. 2008;37:423–31.
Roemer FW, Hunter DJ, Winterstein A, et al. Hip Osteoarthritis MRI Scoring System (HOAMS): reliability and associations with radiographic and clinical findings. Osteoarthr Cartil. 2011;19:946–62.
Roemer FW, Eckstein F, Hayashi D, Guermazi A. The role of imaging in osteoarthritis. Best Pract Res Clin Rheumatol. 2014;28:31–60.
Lee S, Nardo L, Kumar D, et al. Scoring hip osteoarthritis with MRI (SHOMRI): a whole joint osteoarthritis evaluation system. J Magn Reson Imaging. 2015;41:1549–57.
Schwaiger BJ, Gersing AS, Lee S, et al. Longitudinal assessment of MRI in hip osteoarthritis using SHOMRI and correlation with clinical progression. Semin Arthritis Rheum. 2016;45:648–55.
Jaremko JL, Lambert RGW, Zubler V, et al. Methodologies for semiquantitative evaluation of hip osteoarthritis by magnetic resonance imaging: approaches based on the whole organ and focused on active lesions. J Rheumatol. 2014;41:359–69.
Guermazi A, Roemer FW, Haugen IK, Crema MD, Hayashi D. MRI-based semiquantitative scoring of joint pathology in osteoarthritis. Nat Rev Rheumatol Nature Publ Group. 2013;9:236–51.
Maksymowych WP, Cibere J, Loeuille D, et al. Preliminary validation of 2 magnetic resonance image scoring systems for osteoarthritis of the hip according to the OMERACT filter. J Rheumatol J Rheumatol. 2014;41:370–8.
Young JJ, Skou ST, Koes BW, Grønne DT, Roos EM. Proportion of patients with hip osteoarthritis in primary care identified by differing clinical criteria: a cross-sectional study of 4699 patients. Osteoarthr Cartil Open. 2020;2: 100111.
Lin I, Wiles L, Waller R, et al. What does best practice care for musculoskeletal pain look like? Eleven consistent recommendations from high-quality clinical practice guidelines: systematic review. Br J Sports Med BMJ Publishing Group Ltd and British Assoc Sport Exerc Med. 2020;54:79–86.
Xu L, Hayashi D, Guermazi A, et al. The diagnostic performance of radiography for detection of osteoarthritis-associated features compared with MRI in hip joints with chronic pain. Skeletal Radiol. 2013;42:1421–8.
Armbuster TG, Guerra J, Resnick D, et al. The adult hip: an anatomic study. Part I: the bony landmarks Radiol. 1978;128:1–10.
Guerra J, Armbuster TG, Resnick D, et al. The adult hip: an anatomic study. Part II: the soft-tissue landmarks Radiol. 1978;128:11–20.
Hunter DJ, Losina E, Guermazi A, Burstein D, N. Lassere M, Kraus V,. A Pathway and approach to biomarker validation and qualification for osteoarthritis clinical trials. Curr Drug Targets. 2010;11:536–45.
Pereira D, Peleteiro B, Araújo J, Branco J, Santos RA, Ramos E. The effect of osteoarthritis definition on prevalence and incidence estimates: a systematic review. Osteoarthr Cartil. 2011;19:1270–85.
Kim C, Nevitt MC, Niu J et al. Association of hip pain with radiographic evidence of hip osteoarthritis: diagnostic test study. BMJ. British Medical J Publ Group 2015;351:5983.
Kinds MB, Welsing PMJ, Vignon EP, et al. A systematic review of the association between radiographic and clinical osteoarthritis of hip and knee. Osteoarthr Cartil. 2011;19:768–78.
Chu Miow Lin D, Reichmann WM, Gossec L, Losina E, Conaghan PG, Maillefert JF. Validity and responsiveness of radiographic joint space width metric measurement in hip osteoarthritis: a systematic review. Osteoarthr Cartil. 2011;19:543–9.
Bastick AN, Verkleij SPJ, Damen J, et al. Defining hip pain trajectories in early symptomatic hip osteoarthritis–5 year results from a nationwide prospective cohort study (CHECK). Osteoarthritis Cartil. 2016;24:768–75.
Schiphof D, Runhaar J, Waarsing JH, van Spil WE, van Middelkoop M, Bierma-Zeinstra SMA. The clinical and radiographic course of early knee and hip osteoarthritis over 10 years in CHECK (Cohort Hip and Cohort Knee). Osteoarthr Cartil. 2019;27:1491–500.
Schmaranzer F, Klauser A, Kogler M, et al. Diagnostic performance of direct traction MR arthrography of the hip: detection of chondral and labral lesions with arthroscopic comparison. Eur Radiol. 2015;25:1721–30.
Heerey JJ, Kemp JL, Mosler AB, et al. What is the prevalence of imaging-defined intra-articular hip pathologies in people with and without pain? A systematic review and meta-analysis. Br J Sports Med. 2018;52:581–93.
Tresch F, Dietrich TJ, Pfirrmann CWA, Sutter R. Hip MRI: Prevalence of articular cartilage defects and labral tears in asymptomatic volunteers A comparison with a matched population of patients with femoroacetabular impingement. J Magn Reson Imaging. 2017;46:440–51.
Kijima H, Yamada S, Konishi N, et al. The differences in imaging findings between painless and painful osteoarthritis of the hip Clin Med Insights Arthritis Musculoskelet Disord. SAGE Publications Ltd STM. 2020;13:1179544120946747.
Issa K, Jauregui JJ, McElroy M, Banerjee S, Kapadia BH, Mont MA. Unnecessary magnetic resonance imaging of hips: an economic burden to patients and the healthcare system. J Arthroplasty. 2014;29:1911–4.
Zhang Z, Huang C, Jiang Q et al. Guidelines for the diagnosis and treatment of osteoarthritis in China (2019 edition). Ann Transl Med. 2020;8:1213.
Reiman MP, Agricola R, Kemp JL, et al. Consensus recommendations on the classification, definition and diagnostic criteria of hip-related pain in young and middle-aged active adults from the International Hip-related Pain Research Network, Zurich 2018 Br J Sports Med. BMJ Publ Group Ltd British Assoc Sport Exerc Med. 2020;54:631–41.
Griffin DR, Dickenson EJ, O’Donnell J, et al. The Warwick Agreement on femoroacetabular impingement syndrome (FAI syndrome): an international consensus statement. Br J Sports Med BMJ Publ Group Ltd and Br Assoc Sport Exerc Med. 2016;50:1169–76.
Osteoarthritis | NICE impact arthritis | Reviewing the impact of our guidance | Measuring the use of NICE guidance | Into practice | What we do | About [Internet]. NICE. NICE; [cited 2022 Sep 20]. Available from: https://www.nice.org.uk/about/what-we-do/into-practice/measuring-the-use-of-nice-guidance/impact-of-our-guidance/nice-impact-arthritis/osteoarthritis.
Westermann RW, Lynch TS, Jones MH, et al. Predictors of hip pain and function in femoroacetabular impingement: a prospective cohort analysis. Orthop J Sports Med. 2017;5:2325967117726521.
Keeney JA, Nunley RM, Adelani M, Mall N. Magnetic resonance imaging of the hip: poor cost utility for treatment of adult patients with hip pain. Clin Orthop Relat Res. 2014;472:787–92.
Kolasinski SL, Neogi T, Hochberg MC, et al. 2019 American College of Rheumatology/Arthritis Foundation Guideline for the Management of Osteoarthritis of the Hand, Hip, and Knee. Arthritis Care Res. 2020;72:149–62.
Osteoarthritis: care and management [Internet]. London: National Institute for Health and Care Excellence (NICE); 2020 [cited 2022 Sep 23]. Available from: http://www.ncbi.nlm.nih.gov/books/NBK568417/.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key points
• In clinical practice, radiographs are still recommended as first line imaging modality for clinically suspected hip osteoarthritis.
• MRI shows structural lesions of the cartilage, bone and soft tissues and is possibly more suitable than radiographs to be used as a biomarker.
• Development and validation of disease modifying drugs and interventions could alter current imaging strategies.
• Absence of validated diagnostic criteria for early-stage hip OA, and dissociation between pain, physical examination and imaging findings in hip OA remain challenging.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mourad, C., Vande Berg, B. Osteoarthritis of the hip: is radiography still needed?. Skeletal Radiol 52, 2259–2270 (2023). https://doi.org/10.1007/s00256-022-04270-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-022-04270-8