Abstract
Objective
To develop a deep learning algorithm based on automatic detection of landmarks that can be used to automatically calculate forefoot imaging parameters from radiographs and test its performance.
Materials and methods
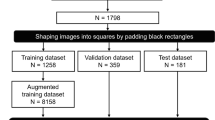
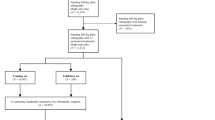
A total of 1023 weight-bearing dorsoplantar (DP) radiographs were included. A total of 776 radiographs were used for training and verification of the model, and 247 radiographs were used for testing the performance of the model. The radiologists manually marked 18 landmarks on each image. By training our model to automatically label these landmarks, 4 imaging parameters commonly used for the diagnosis of hallux valgus could be measured, including the first–second intermetatarsal angle (IMA), hallux valgus angle (HVA), hallux interphalangeal angle (HIA), and distal metatarsal articular angle (DMAA). The reference standard was determined by the radiologists’ measurements. The percentage of correct key points (PCK), intragroup correlation coefficient (ICC), Pearson correlation coefficient (r), root mean square error (RMSE), and mean absolute error (MAE) between the predicted value of the model and the reference standard were calculated. The Bland–Altman plot shows the mean difference and 95% LoA.
Results
The PCK was 84–99% at the 3-mm threshold. The correlation between the observed and predicted values of the four angles was high (ICC: 0.89–0.96, r: 0.81–0.97, RMSE: 3.76–6.77, MAE: 3.22–5.52). However, there was a systematic error between the model predicted value and the reference standard (the mean difference ranged from − 3.00 to − 5.08°, and the standard deviation ranged from 2.25 to 4.47°).
Conclusion
Our model can accurately identify landmarks, but there is a certain amount of error in the angle measurement, which needs further improvement.








Similar content being viewed by others
References
Piqué-Vidal C, Solé MT, Antich J. Hallux valgus inheritance: pedigree research in 350 patients with bunion deformity. J Foot Ankle Surg. 2007;46(3):149–54. https://doi.org/10.1053/j.jfas.2006.10.011.
Hecht PJ, Lin TJ. Hallux valgus. Med Clin North Am. 2014;98(2):227–32. https://doi.org/10.1016/j.mcna.2013.10.007.
Perera AM, Mason L, Stephens MM. The pathogenesis of hallux valgus. J Bone Joint Surg Am. 2011;93(17):1650–61. https://doi.org/10.2106/JBJS.H.01630.
Smyth NA, Aiyer AA. Introduction: why are there so many different surgeries for hallux valgus? Foot Ankle Clin. 2018;23(2):171–82. https://doi.org/10.1016/j.fcl.2018.01.001.
Galois L. History of surgical treatments for hallux valgus. Eur J Orthop Surg Traumatol. 2018;28(8):1633–9. https://doi.org/10.1007/s00590-018-2235-6.
Shi GG, Whalen JL, Turner NS 3rd, Kitaoka HB. Operative approach to adult hallux valgus deformity: principles and techniques. J Am Acad Orthop Surg. 2020;28(10):410–8. https://doi.org/10.5435/JAAOS-D-19-00324.
Fraissler L, Konrads C, Hoberg M, Rudert M, Walcher M. Treatment of hallux valgus deformity. EFORT Open Rev. 2016;1(8):295–302. https://doi.org/10.1302/2058-5241.1.000005.
Coughlin MJ, Freund E. Roger A. Mann Award. The reliability of angular measurements in hallux valgus deformities. Foot Ankle Int. 2001;22(5):369–79. https://doi.org/10.1177/107110070102200503.
Resch S, Ryd L, Stenström A, Johnsson K, Reynisson K. Measuring hallux valgus: a comparison of conventional radiography and clinical parameters with regard to measurement accuracy. Foot Ankle Int. 1995;16(5):267–70. https://doi.org/10.1177/107110079501600504.
Lamm BM, Stasko PA, Gesheff MG, Bhave A. Normal foot and ankle radiographic angles, measurements, and reference points. J Foot Ankle Surg. 2016;55(5):991–8. https://doi.org/10.1053/j.jfas.2016.05.005.
Steel MW 3rd, Johnson KA, DeWitz MA, Ilstrup DM. Radiographic measurements of the normal adult foot. Foot Ankle. 1980;1(3):151–8. https://doi.org/10.1177/107110078000100304.
Vittetoe DA, Saltzman CL, Krieg JC, Brown TD. Validity and reliability of the first distal metatarsal articular angle. Foot Ankle Int. 1994;15(10):541–7. https://doi.org/10.1177/107110079401501004.
Torosdagli N, Liberton DK, Verma P, Sincan M, Lee JS, Bagci U. Deep geodesic learning for segmentation and anatomical landmarking. IEEE Trans Med Imaging. 2019;38(4):919–31. https://doi.org/10.1109/TMI.2018.2875814.
Ibtehaz N, Rahman MS. MultiResUNet : rethinking the U-Net architecture for multimodal biomedical image segmentation. Neural Netw. 2020;121:74–87. https://doi.org/10.1016/j.neunet.2019.08.025.
Ronneberger O, Fischer P, Brox T. U-Net: convolutional networks for biomedical image segmentation[J]. Springer International Publishing; 2015.
Xiao B , Wu H , Wei Y . Simple baselines for human pose estimation and tracking[C]// ECCV. arXiv, 2018.
Hosny A, Parmar C, Quackenbush J, Schwartz LH, Aerts HJWL. Artificial intelligence in radiology. Nat Rev Cancer. 2018;18(8):500–10. https://doi.org/10.1038/s41568-018-0016-5.
Yasaka K, Abe O. Deep learning and artificial intelligence in radiology: current applications and future directions. PLoS Med. 2018;15(11):e1002707. https://doi.org/10.1371/journal.pmed.1002707.
Larson DB, Chen MC, Lungren MP, Halabi SS, Stence NV, Langlotz CP. Performance of a deep-learning neural network model in assessing skeletal maturity on pediatric hand radiographs. Radiology. 2018;287(1):313–22. https://doi.org/10.1148/radiol.2017170236.
Tomita N, Cheung YY, Hassanpour S. Deep neural networks for automatic detection of osteoporotic vertebral fractures on CT scans. Comput Biol Med. 2018;1(98):8–15. https://doi.org/10.1016/j.compbiomed.2018.05.011.
Kim DH, MacKinnon T. Artificial intelligence in fracture detection: transfer learning from deep convolutional neural networks. Clin Radiol. 2018;73(5):439–45. https://doi.org/10.1016/j.crad.2017.11.015.
Lindsey R, Daluiski A, Chopra S, Lachapelle A, Mozer M, Sicular S, Hanel D, Gardner M, Gupta A, Hotchkiss R, Potter H. Deep neural network improves fracture detection by clinicians. Proc Natl Acad Sci U S A. 2018;115(45):11591–6. https://doi.org/10.1073/pnas.1806905115.
Couteaux V, Si-Mohamed S, Nempont O, Lefevre T, Popoff A, Pizaine G, Villain N, Bloch I, Cotten A, Boussel L. Automatic knee meniscus tear detection and orientation classification with Mask-RCNN. Diagn Interv Imaging. 2019;100(4):235–42. https://doi.org/10.1016/j.diii.2019.03.002.
Roblot V, Giret Y, Bou Antoun M, Morillot C, Chassin X, Cotten A, Zerbib J, Fournier L. Artificial intelligence to diagnose meniscus tears on MRI. Diagn Interv Imaging. 2019;100(4):243–9. https://doi.org/10.1016/j.diii.2019.02.007.
Liu F, Zhou Z, Samsonov A, Blankenbaker D, Larison W, Kanarek A, Lian K, Kambhampati S, Kijowski R. Deep learning approach for evaluating knee MR images: achieving high diagnostic performance for cartilage lesion detection. Radiology. 2018;289(1):160–9. https://doi.org/10.1148/radiol.2018172986.
Wang CW, Huang CT, Hsieh MC, Li CH, Chang SW, Li WC, Vandaele R, Marée R, Jodogne S, Geurts P, Chen C, Zheng G, Chu C, Mirzaalian H, Hamarneh G, Vrtovec T, Ibragimov B. Evaluation and comparison of anatomical landmark detection methods for cephalometric X-ray images: a grand challenge. IEEE Trans Med Imaging. 2015;34(9):1890–900. https://doi.org/10.1109/TMI.2015.2412951.
Cardillo J, Sid-Ahmed MA. An image processing system for locating craniofacial landmarks. IEEE Trans Med Imaging. 1994;13(2):275–89. https://doi.org/10.1109/42.293920.
Esteva A, Robicquet A, Ramsundar B, Kuleshov V, DePristo M, Chou K, Cui C, Corrado G, Thrun S, Dean J. A guide to deep learning in healthcare. Nat Med. 2019;25(1):24–9. https://doi.org/10.1038/s41591-018-0316-z.
Miotto R, Wang F, Wang S, Jiang X, Dudley JT. Deep learning for healthcare: review, opportunities and challenges. Brief Bioinform. 2018;19(6):1236–46. https://doi.org/10.1093/bib/bbx044.
Chan HP, Samala RK, Hadjiiski LM, Zhou C. Deep learning in medical image analysis. Adv Exp Med Biol. 2020;1213:3–21. https://doi.org/10.1007/978-3-030-33128-3_1.
Day J, de Cesar NC, Richter M, Mansur NS, Fernando C, Deland JT, Ellis SJ, Lintz F. Evaluation of a weightbearing CT artificial intelligence-based automatic measurement for the M1–M2 intermetatarsal angle in hallux valgus. Foot Ankle Int. 2021. https://doi.org/10.1177/10711007211015177.
Cassar-Pullicino VN. Measurements in musculoskeletal radiology. Springer Verlag Ny; 2017.
Dai J, Qi H, Xiong Y, et al. Deformable convolutional networks[J]. IEEE, 2017.
Rectified linear units improve restricted Boltzmann machines Vinod Nair[C]// International Conference on International Conference on Machine Learning. Omnipress, 2010.
Payer C, Tern D, Bischof H, et al. Integrating spatial configuration into heatmap regression based CNNs for landmark localization[J]. Med Image Anal. 2019.
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016;15(2):155–63. https://doi.org/10.1016/j.jcm.2016.02.012 (Epub 2016 Mar 31. Erratum in: J Chiropr Med. 2017 Dec;16(4):346).
Schober P, Boer C, Schwarte LA. Correlation coefficients: appropriate use and interpretation. Anesth Analg. 2018;126(5):1763–8. https://doi.org/10.1213/ANE.0000000000002864.
Dong Y, Zhang S, Yan Z, Tan C, Metaxas D. . . Automated anatomical landmark detection on distal femur surface using convolutional neural network. 2015 IEEE International Symposium on Biomedical Imaging. IEEE. 2015.
Liu W, Wang Y, Jiang T, et al. Landmarks detection with anatomical constraints for total hip arthroplasty preoperative measurements[C]//International Conference on Medical Image Computing and Computer-Assisted Intervention. Springer, Cham, 2020: 670-679
Yang W, Ye Q, Ming S, Hu X, Jiang Z, Shen Q, He L, Gong X. Feasibility of automatic measurements of hip joints based on pelvic radiography and a deep learning algorithm. Eur J Radiol. 2020;132:109303. https://doi.org/10.1016/j.ejrad.2020.109303.
Ye Q, Shen Q, Yang W, Huang S, Jiang Z, He L, Gong X. Development of automatic measurement for patellar height based on deep learning and knee radiographs. Eur Radiol. 2020;30(9):4974–84. https://doi.org/10.1007/s00330-020-06856-z.
Zhang SC, Sun J, Liu CB, Fang JH, Xie HT, Ning B. Clinical application of artificial intelligence-assisted diagnosis using anteroposterior pelvic radiographs in children with developmental dysplasia of the hip. Bone Joint J. 2020;102-B(11):1574–81. https://doi.org/10.1302/0301-620X.102B11.BJJ-2020-0712.R2.
Funding
This study was funded by MicroRNA-150 Targeting IGF2BP1 to Regulate IAPs to Improve Chemosensitivity of Osteosarcoma and Its Mechanism study (grant number 20190201211JC).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Approval from the Institutional Review Board was obtained and in keeping with the policies for a retrospective review, informed consent was not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, T., Wang, Y., Qu, Y. et al. Feasibility study of hallux valgus measurement with a deep convolutional neural network based on landmark detection. Skeletal Radiol 51, 1235–1247 (2022). https://doi.org/10.1007/s00256-021-03939-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-021-03939-w