Abstract
Bacterial outer membrane vesicles (OMVs) are nanosized spheroidal particles shed by gram-negative bacteria that contain biomolecules derived from the periplasmic space, the bacterial outer membrane, and possibly other compartments. OMVs can be purified from bacterial culture supernatants, and by genetically manipulating the bacterial cells that produce them, they can be engineered to harbor cargoes and/or display molecules of interest on their surfaces including antigens that are immunogenic in mammals. Since OMV bilayer-embedded components presumably maintain their native structures, OMVs may represent highly useful tools for generating antibodies to bacterial outer membrane targets. OMVs have historically been utilized as vaccines or vaccine constituents. Antibodies that target bacterial surfaces are increasingly being explored as antimicrobial agents either in unmodified form or as targeting moieties for bactericidal compounds. Here, we review the properties of OMVs, their use as immunogens, and their ability to elicit antibody responses against bacterial antigens. We highlight antigens from bacterial pathogens that have been successfully targeted using antibodies derived from OMV-based immunization and describe opportunities and limitations for OMVs as a platform for antimicrobial antibody development.
Key points
• Outer membrane vesicles (OMVs) of gram-negative bacteria bear cell-surface molecules
• OMV immunization allows rapid antibody (Ab) isolation to bacterial membrane targets
• Review and analysis of OMV-based immunogens for antimicrobial Ab development
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The goal of this short review is to synthesize the results of studies that have used outer membrane vesicles (OMVs) from gram-negative bacteria as immunogens for the generation of antibodies (Abs) against bacterial cell-surface targets. We summarize the properties and natural functions of OMVs, common OMV sources, organisms and routes used for immunization, the types of anti-OMV Ab responses elicited (e.g., polyclonal, monoclonal, isotypes), the properties of the target antigens, and the degree of characterization of the resulting Abs. Future perspectives regarding the opportunities and drawbacks of OMV-based Ab generation are presented. For comprehensive introductions to OMV biology, production, purification, characterization, and use in vaccine development, we direct readers to several other review articles (Balhuizen et al. 2021; Klimentova and Stulik 2015; Micoli and MacLennan 2020; Sartorio et al. 2021; Schwechheimer and Kuehn 2015).
Properties of OMVs
OMVs are spheroidal particles 20 to 250 nm in diameter that are shed from the cell surfaces of nearly all gram-negative bacteria (Schwechheimer and Kuehn 2015). Similar particles shed by gram-positive bacteria and other microorganisms are generally referred to as membrane vesicles (MVs) or extracellular vesicles (EVs), hereafter termed EVs in this review (Fig. 1). OMVs are unilamellar vesicles bounded by lipids derived from the bacterial outer membrane (OM) and contain components derived from the periplasmic space as well as a subset of OM constituents, including lipoproteins, lipopolysaccharides (LPS), capsular polysaccharides, integral membrane proteins, and other OM-associated molecules (Lee et al. 2007; Murphy et al. 2014; Roier et al. 2015). The composition of the membrane-embedded and membrane-associated components of OMVs is closely related to that of the bacterial surface; however, the relative abundance of constituents can differ from the OM (Schwechheimer and Kuehn 2015) via mechanisms that are still unclear. Certain components can be enriched or depleted to varying degrees depending on environmental factors such as growth conditions, leading to heterogeneity among the OMVs shed from individual bacterial strains (Nagakubo et al. 2020). OMVs also carry a variety of cargoes in their luminal space including, with both periplasmic and cytoplasmic proteins, peptidoglycan, nucleic acids, and small molecule effectors involved in nutrient acquisition and signaling (Jan 2017). Like OM components, periplasmic components are enriched, depleted, or excluded in OMVs through poorly understood OMV biogenesis mechanisms (Bonnington and Kuehn 2014). The presence of cytoplasmic proteins in OMVs suggests the possibility of specific mechanisms of cellular transport and packaging, although none have yet been fully characterized. Note that evidence for the presence of cytoplasmic and inner membrane proteins in OMVs has been mostly based on proteomic analyses, some of which could not exclude the presence of lysed cells in the samples analyzed, and protein analyses have suggested that OMVs either lack or are highly depleted in these components depending on isolation or purification methodology (van de Waterbeemd et al. 2013). Similarly, although DNA has been detected in OMVs (Bitto et al. 2017), it has been suggested to be either or both surface-associated and luminally packaged, and in the former case, it remains unclear whether DNA originating from lysed cells may be present. The molecular mechanisms responsible for OMV shedding are only partially understood; however, the process of OMV formation is thought to begin with the detachment of peptidoglycan-associated OM proteins (Schwechheimer and Kuehn 2015). The inner leaflet of the OM contains anchored lipoproteins crosslinked to peptidoglycan; OMV formation is thought to occur when local crosslink levels decrease sufficiently (Schwechheimer et al. 2014). Additional factors such as the formation of lipid microdomains, accumulation of vesicle-facilitating molecules such as LPS subtypes, and the actions of quorum sensing molecules have also been suggested to contribute to the induction of membrane curvature, OMV formation, and budding (Schwechheimer and Kuehn 2015).
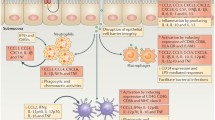
Schematic overview of antibody generation using outer membrane vesicles (OMVs) and extracellular vesicles (EVs). Purified OMVs from gram-negative bacteria or EVs from gram-positive bacteria are used as immunogens for animal immunizations (e.g., mouse, rat, chicken, rabbit, llama). Polyclonal antibodies against OMVs or bacterial antigens can be detected in the serum of responding animals. Hybridoma generation (myeloma cell fusion) or other selection approaches (e.g., phage display libraries) are used to isolate monoclonal antibodies (mAbs). The resulting mAbs are purified and characterized for affinity, specificity, and antimicrobial activity in functional assays. Target identification and validation, using techniques such as mass spectrometry and binding assays, reveal the antigen targeted by the mAb
Gram-positive bacteria have also been shown to shed vesicles, which are referred to as EVs. The EVs of gram-positive bacteria are similar in size to OMVs but display cytoplasmic membrane components on their surfaces, have different phospholipid profiles, incorporate lipoteichoic acid and greater amounts of peptidoglycan, and harbor luminal components derived from the bacterial cytoplasm (Bose et al. 2020). Unlike the OMVs of gram-negative bacteria, gram-positive EVs are not anchored to an internal peptidoglycan layer but are instead anchored and physically blocked by the thick peptidoglycan-containing cell wall. Gram-positive bacterial cells induce localized disruption of the peptidoglycan layer, allowing for the passage of EVs through the resulting temporary channel (Bose et al. 2020). While less studied in comparison to gram-negative OMVs, gram-positive EVs are gaining interest due to their similar properties and applications as OMVs (Bose et al. 2020; Wang et al. 2018).
Functions of OMVs
OMV release contributes to a wide array of biological functions in bacteria, with differences in OMV composition and function based on bacterial species (Jan 2017) and environmental conditions (Kulp and Kuehn 2010). OMVs directly contribute to bacterial survival and are generally used as long-distance effectors. OMV shedding allows for the removal of toxic or degraded cellular components, contributing to bacterial survival during cell stress (McBroom and Kuehn 2007). Bacteria can also use OMVs for nutrient acquisition from the environment, as they can contain hydrolytic enzymes, metal scavenging proteins, and lytic machinery (Schwechheimer and Kuehn 2015). OMVs released from bacterial pathogens can act directly as virulence factors by degrading host cellular and physical barriers (Stentz et al. 2018) and delivering toxins, virulence factors, or immune-modulating factors to host cells (Schwechheimer and Kuehn 2015). The physical presence of OMVs can also passively contribute to the degradation of antimicrobials via enzymatic activity (Ciofu et al. 2000) and/or adsorption of antimicrobials and bacteriophage that target OM components (Manning and Kuehn 2011). OMVs can also contain components that divert the complement system, contributing to the evasion of complement-mediated lysis (Dehinwal et al. 2021). They may also directly contribute to antimicrobial resistance development as vectors for horizontal gene transfer (Dell'Annunziata et al. 2021), although the mechanisms through which DNA is shuttled to OMVs remain unclear and the possibility of non-specific DNA association with OMV surfaces cannot be ruled out. OMVs also play a role in the development and restructuring of bacterial biofilms (Wang et al. 2015). As such, studies of OMVs may deepen our understanding of infections caused by gram-negative bacterial pathogens and offer new avenues for therapeutic targeting. Many of the functions of gram-negative OMVs are likely to extend to gram-positive EVs as well, although investigations of the functions of EVs are still in the early stages.
Production and purification of OMVs
OMVs are an easy-to-produce source of non-replicative, presumably structurally preserved material derived from gram-negative bacterial cells and have been used extensively as antigens for immunization. Production of OMVs for research or therapy can be initiated using several different methodologies. OMVs produced by bacteria during growth without the addition of exogenous stimuli are referred to as spontaneous OMVs (sOMVs). They can be prepared by culturing bacteria and removing cells from the culture medium by centrifugation and filtration, followed by ultracentrifugation, ultrafiltration, or ammonium sulfate precipitation (Balhuizen et al. 2021; Wang et al. 2019a). These techniques can be expected to yield acellular material that contains OMVs as well as potentially other large extracellular materials such as flagella, fimbria, pili, and large protein complexes and/or aggregates. Higher OMV purity can be achieved by additional density gradient centrifugation and/or size exclusion chromatography steps; however, the presence of low levels of extracellular contaminants, some of which may be highly immunogenic, is generally difficult to rule out. Components derived from lysed cells may also contaminate OMV preparations. In some cases, the production of adequate amounts of OMVs may require enhancement of spontaneously occurring vesicle yields. OMV vesiculation can be promoted by the addition of mild non-ionic detergents to bacterial cultures, such as sodium deoxycholate or polyethylene glycol oleyl ether, which largely preserve vesicle integrity and protein folding (Gnopo et al. 2017; van der Pol et al. 2015). However, detergent-based OMVs (dOMVs) may have lower LPS content, less diverse phospholipid profiles, and altered proteomic profiles compared to sOMVs (van de Waterbeemd et al. 2010). Compared to sOMVs, dOMVs can also be less stable and more prone to aggregation (van de Waterbeemd et al. 2010). OMV vesiculation can also be induced through physical processes such as sonication, vortexing, pressure cell disruption, or by the addition of ethylenediaminetetraacetic acid (van der Pol et al. 2015). The resulting native OMVs (nOMVs) show more closely related proteomic profiles to sOMVs than dOMVs; however, differences in membrane protein composition between nOMVs and sOMVs are still observed (van de Waterbeemd et al. 2013; van de Waterbeemd et al. 2010). Interestingly, the composition of nOMVs is thought to more closely mirror that of the bacterial OM and periplasmic space compared with sOMVs (Gnopo et al. 2017; van der Pol et al. 2015). Both dOMVs and nOMVs contain higher levels of cytosolic proteins, including some that are not detected in sOMVs, possibly due to disruption of the inner membrane during mechanical or chemical induction of vesiculation (van de Waterbeemd et al. 2013). The attributes of OMVs produced using different strategies and their impacts on immunogenicity and antigen coverage may be desirable or detrimental depending on the application (van de Waterbeemd et al. 2013). Selection of a particular type of OMV depends on the recipient organism’s sensitivity to LPS, intended antigen coverage, required stability of the OMV formulation, and yield requirements.
Genetic manipulation of OMVs
While the molecular mechanisms involved in OMV production are not fully understood, several pathways have been identified that allow for the modification of OMV vesiculation levels and composition. With respect to vesiculation levels, the deletion of OM proteins that associate with the peptidoglycan layer can result in disruption of peptidoglycan integrity, increased membrane stress, and enhanced vesiculation (Ojima et al. 2020). However, the impacts of mutations related to envelope stress and phospholipid accumulation on OMV composition are unknown. As the specific genes and proteins involved in OMV biogenesis differ between gram-negative bacteria, hypervesiculation mutation strategies are species specific. In Escherichia coli, mutation of genes encoding proteins that are involved in the linkages between the OM and inner membrane with peptidoglycan (e.g., tolA, tolB, ompC, ompF, and pal) induces hypervesiculation (McBroom et al. 2006). Additionally, mutation of nlpI, a gene encoding a protein that restricts the activity of the peptidoglycan endopeptidase Spr, leads to reduced peptidoglycan crosslinking with the OM and hypervesiculation (Schwechheimer et al. 2015). Mutation of the degP gene encoding a periplasmic chaperone/protease increases vesiculation, as does mutation of the related stress signal transmission genes degS and rseA, presumably by increasing the accumulation of misfolded periplasmic proteins and, therefore, the need for export (McBroom et al. 2006). Studies of genetically induced hypervesiculation in various gram-negative pathogens are still in their infancy (Balhuizen et al. 2021). The available molecular toolbox for the control of OMV generation is likely to continue to expand as the molecular mechanisms of OMV biogenesis are further studied.
In addition to modulation of vesiculation levels, the composition of OMVs can be directly controlled through the manipulation of genes involved in OMV protein sorting. This was first shown in E. coli with the protein ClyA, which is concentrated into the membrane of OMVs (Wai et al. 2003) and can be used as a carrier for recombinantly fused antigens to the OMV surface (Kim et al. 2008). Subsequently, a number of other proteins (e.g., Neisseria meningitidis fHbp (Salverda et al. 2016) and E. coli Hbp (Hays et al. 2018; Kuipers et al. 2015)) were shown to localize to OMVs and, via recombinant fusion, to present heterologous antigens on the vesicle surface in different gram-negative bacteria (Wang et al. 2019a). OMVs displaying heterologous fusions to OMV-associated membrane proteins on their surfaces have been found to elicit serum Ab responses in mice (Kuipers et al. 2015; Rappazzo et al. 2016; Salverda et al. 2016). Interestingly, luminal OMV cargo molecules can also elicit weaker Ab titers following immunization, a process that would be expected to require the release of OMV contents; however, few rigorous comparisons of the immunogenicity of surface-displayed versus luminal antigens have been conducted (Fantappie et al. 2014; Muralinath et al. 2011; Salverda et al. 2016). Alternatively, genes encoding proteins enriched in OMVs can be modified to include affinity tags such as SpyTag or avidin, and the presence of these handles on the OMV surface can be used to conjugate heterologous proteins and other molecules (Kim et al. 2008; Weyant et al. 2023). However, other factors such as heterologous protein complexity, fusion orientation, fusion protein expression levels, and potential impacts on bacterial growth and vesiculation rates must be considered in this process. It is expected that there would be size and complexity limitations on the types of heterologous proteins that can be successfully fused with OMV-resident proteins and presented on the OMV surface.
Uses of OMVs as immunogens
OMVs have been developed as vaccines or vaccine components designed to protect against bacterial pathogens for several decades. The most well-studied bacterium in the context of OMV-based vaccines is N. meningitidis group B, with several products receiving regulatory approval in various jurisdictions (one, 4CMenB, by the FDA and EMA) since the 1980s. These include VA-MENGOC-BC® (1989–present, Cuban National Immunization Program and elsewhere in Latin America and the Caribbean for epidemic control) and 4CMenB (Bexsero®; 2013–present, various jurisdictions including Europe and North America), a multicomponent vaccine containing three recombinant proteins produced in E. coli as well as the PorA-containing OMV preparation MeNZB™; the latter was used from 2004 to 2011 in New Zealand to control the spread of an epidemic strain (Micoli and MacLennan 2020). Bactericidal antibodies elicited by 4CMenB provide broad coverage (approximately 57–87%) against meningococcal serogroup B strains worldwide (Castilla et al. 2023). Another OMV-based vaccine developed in Norway in the 1980s, MenBVac®, formed the basis for the development of MeNZB™ and was used to control epidemic outbreaks in Norway and France. Both VA-MENGOC-BC® and MeNZB™ are dOMV-based products extracted using deoxycholate. While these are the only examples of OMV vaccines that have received regulatory approval at the time of writing, several other OMV-based vaccines are under clinical development for pathogens including Klebsiella pneumoniae, Salmonella spp., Shigella spp., Mycobacterium tuberculosis, Haemophilus spp., and Vibrio cholerae (Micoli and MacLennan 2020). Preclinical investigations of OMV vaccines have included a wide range of targets derived from gram-negative and gram-positive bacteria as well as viruses (Lieberman 2022).
As bacterial resistance to the antibiotics currently used for human therapy continues to grow, the development of targeted Ab-based therapies may be necessary as an alternative. In this regard, OMV-based Ab development may provide a facile and rapid method for obtaining antibacterial Abs (Fig. 1). Given the success of OMV-based vaccines against N. meningitidis, researchers have analyzed the Ab responses elicited following OMV vaccination in a variety of animal models and in humans. It is assumed that the mechanisms underlying the generation of Ab responses to OMVs are similar to those for whole bacterial cells, involving uptake and processing by antigen-presenting cells followed by antigenic peptide presentation on MHC class II molecules to drive helper T cell responses, as well as surface capture of unprocessed opsonized OMV antigens for B-cell receptor engagement (Baker et al. 2021; Prior et al. 2021). Given that OMVs presumably present bacterial OM antigens in their native conformations, OMVs provide an attractive route for the development of Abs that recognize intact bacterial cells.
OMVs have been used extensively in generating polyclonal Abs (pAbs) against a variety of bacterial pathogens. Several studies have detected the presence of Abs to defined targets in the sera of immunized animals using enzyme-linked immunosorbent assay (ELISA), immunoprecipitation, western blotting, and mass spectrometry. The pAb responses observed in several of these studies suggest that monoclonal antibodies (mAbs) could potentially be developed against bacterial surface targets through immunization with OMVs. However, because pAb responses were detected in some cases to luminal or secreted proteins or to surface targets that are known to be shed, it remains unclear to what extent pAbs are generated against OMVs themselves (including integral OM proteins) versus copurified antigens and/or OMV degradation products. Note also that while some pAbs derived from OMV immunization have been assessed using in vitro functional assays (e.g., bactericidal assays), it was not possible to ascribe functional activity to Abs directed against any specific antigen(s). A list of antigenic targets determined to be immunogenic following OMV or gram-positive EV-based immunizations is shown in Table 1 and Supplementary Table S1.
The use of OMVs derived from Neisseria species as immunogens has been studied extensively through efforts toward developing efficacious vaccines for meningitis. Ab responses following OMV immunization to the serotype-defining OM proteins (PorA, PorB, RmpM, Opa, and Opc), membrane polysaccharides, as well as many other surface-exposed virulence factors, have been detected and characterized (Awanye et al. 2019). While some serum pAb responses have been validated by ELISA using recombinant or purified antigens, many pAb responses have only been documented by western blot or immunoprecipitation; these techniques may be more susceptible to erroneous target attribution due to factors such as antigen abundance bias and low throughput, limiting the number of experimental controls that can be included. However, reproducible detection of the major OM protein classes, membrane-associated polysaccharides, and other associated antigens across independent experiments and in different organisms suggests that OMVs induce Ab responses to these antigens (Dalseg et al. 1999; Leduc et al. 2020; Viviani et al. 2023; Wedege et al. 2007). Shigella OMVs have also been well studied, and pAb responses to major OM antigens such as LPS, porins, and secretion system components have been observed (Mancini et al. 2021; Necchi et al. 2023). OMVs from several other gram-negative bacteria have been shown to induce pAb responses against membrane antigens (Table 1, Supplementary Table S1). Generation of pAbs to cell membrane targets of gram-positive pathogens such as Bacillus anthracis, Staphylococcus aureus, and Streptococcus species has also been demonstrated (Nakamura et al. 2020; Rivera et al. 2010; Wang et al. 2018). In some cases, pAbs to gram-positive antigens were obtained through direct immunization with EVs derived from the target bacteria; however, most pAbs were generated by heterologous expression of gram-positive bacterial antigens in OMVs derived from gram-negative bacteria, predominantly E. coli strains genetically modified for hypervesiculation.
MAb generation using OMVs
OMV-based immunization has resulted in numerous target-validated mAbs primarily derived from mouse hybridomas (Table 2). Previous studies of Neisseria OMV-based vaccines have identified several OM proteins including PorB and RmpM as immunodominant antigens in mice and humans (Awanye et al. 2019). It is, therefore, unsurprising that OMV immunization enabled the isolation of mAbs directed to these two antigens. In two independent studies, mice were immunized with N. meningitidis strain 44/76 OMVs, and hybridoma-derived mAbs were analyzed by immunoblotting against OMVs as well as by epitope mapping using overlapping peptides from PorB (Delvig et al. 1995) and RmpM (Rosenqvist et al. 1999). This strategy allowed for the isolation of class 3 outer membrane protein (OMP; PorB) mAbs 188,C-1 (IgG3) and 152,D-8 (IgG1) (Delvig et al. 1995) as well as the class 4 OMP (Rmp) mAbs 155,B-4 (IgM), 173,G-1 (IgG1), and 185,H-8 (IgG2a) (Rosenqvist et al. 1999). Note that evidence for PorA binding by mAbs 188,C-1 and 152,D-8 was limited to equivocal ELISA binding to synthetic peptides, as well as potentially western blotting (although these results were not shown). Similarly, evidence for RmpM binding by mAbs 155,B-4, 173,G-1, and 185,H-8 was limited to ELISA binding to synthetic peptides whose locations in the protein’s three-dimensional structure were unclear, as well as potentially western blotting (although these results were not shown); none of the mAbs bound to live or killed bacterial cells by immunogold electron microscopy or flow cytometry. In addition to PorA and Rmp, mAbs to NspA were isolated using two separate methodologies. In one study, mice were sequentially immunized with OMVs derived from three strains of N. meningitidis with diverse serological classifications (M1090, BZ198, and Z1092) (Moe et al. 2002). Hybridoma supernatants were screened for bacterial cell binding and bactericidal activity, resulting in the discovery of mAb 14C7 (IgG3). In the same study, the mAb was validated in whole cell ELISA experiments using E. coli cells expressing N. meningitidis NspA. This effort built on earlier work from the same group in which mice were immunized with E. coli BL21(DE3) OMVs expressing N. meningitidis NspA, and the resulting mAbs (AL4, AL5, AL11, and AL1; all IgG2a) were validated by assessing ELISA binding to isogenic wild-type and NspA-knockout Neisseria cells (Moe et al. 2001). Two mAbs to Neisseria NadA (1079B6 and 4895F9, not isotyped) were also isolated by mouse OMV immunization, hybridoma generation, and immunoblotting. Subsequent antigen identification was conducted using mass spectrometry of tryptic digests (Fukasawa et al. 2003). In addition to protein targets, mAbs to Neisseria α2,8-linked polysialic acid have also been generated (Devi et al. 1996). To do so, OMVs from N. meningitidis M986-NCVl, a non-capsular mutant, were first purified and then chemically conjugated using adipic acid dihydrazide to N-deacetylated capsular polysaccharides (CPS) purified from N. meningitidis as well as E. coli K1 cells (Devi et al. 1996). Immunization and hybridoma generation yielded 11 mAbs of IgM and IgG isotypes, each of which bound to a subset of different Neisseria and E. coli CPS preparations. Interestingly, the binding of individual mAbs to polysialic acid preparations derived from the source bacterium by ELISA was affected by the immobilization method and/or protein conjugation status. Only three mAbs (A2, A3, and B8) showed significant bactericidal activity against N. meningitidis.
In addition to Neisseria, OMVs have been effective antigenic sources in producing mAbs for several other bacterial pathogens. OMVs from Haemophilus influenzae type b were used to produce mAbs in mice via hybridoma generation (Robertson et al. 1982). The resulting mAbs were used to immunoprecipitate three OM protein antigens of different molecular weights. Only one mAb, 6A2 (not isotyped), was able to bind its cognate antigen on the surface of intact bacteria (Robertson et al. 1982). However, further experiments using denaturing western blots revealed that mAb 6A2 bound to H. influenzae LPS and that the erroneous immunoprecipitation result was due to the formation of a complex between LPS and an undefined OM protein, resulting in co-immunoprecipitation (Gulig and Hansen 1985). A similar strategy was used by the same group to identify several mAbs using Moraxella catarrhalis 035E OMVs, including mAb 10F3 (IgG2a) that was shown to bind CopB, an 80 kDa OM protein, by western blotting and colony blotting using whole M. catarrhalis cells and E. coli cells expressing M. catarrhalis CopB by western blotting (Helminen et al. 1993). The same approach was used to discover an anti-M. catarrhalis O35E mAb, 17C7 (IgG2a), that reacted with a single high molecular weight band in western blots and bound to whole bacterial cells. Antigen identification was conducted by plaque screening of a genomic M. catarrhalis O35E library constructed in a recombinant bacteriophage vector. Screening of bacteriophage plaques formed in E. coli cell lawns identified UspA as reactive with 17C7 by radiolabeling. MAb 17C7 was then found to bind UspA by western blot in both phage-infected E. coli cells expressing M. catarrhalis UspA and in M. catarrhalis O35E lysates (Helminen et al. 1994).
Porphyromonas gingivalis TDC60 OMVs purified via ammonium sulfate precipitation were used to immunize mice, and the resulting mAb TDC4-33H (not isotyped) potentially recognized P. gingivalis LPS based on ladder-like banding pattern in western blots and an ability to prevent IL-8 production by fibroblasts (Hijiya et al. 2010). P. gingivalis OMVs were also used to generate a mAb, Pg-Vc (not isotyped), against hemagglutinin (Shibata et al. 1998). The antigen was identified by western blotting against OMVs, followed by functional testing of inhibition of erythrocyte agglutination induced by OMVs. MAb Pg-Vc showed a similar banding pattern in western blots as an anti-hemagglutinating adhesion (HA-Ag2).
OMVs were prepared from Treponema palladium cells via disruption in a French pressure cell press, followed by purification through a continuous sugar gradient (Blanco et al. 2005). Mice were immunized with the OMV preparation, and sera were assessed for bactericidal activity. Hybridoma generation resulted in mAb M131 (IgM), which exhibited bactericidal activity through binding to a phosphorylcholine epitope specific to T. pallidum. Binding to whole cells was validated by dot-blot analysis and fluorescence microscopy.
Finally, Acinetobacter baumannii nOMVs were used as immunogens with the goal of generating OM protein-targeting single-domain Abs (VHHs) (Lei et al. 2023). Llama immunization with A. baumannii OMVs resulted in strong IgG1 and IgG2b pAb responses. Panning of a phage display library yielded a VHH, OMV81, whose target was identified as the OM pilin protein CsuA/B by western blotting and mass spectrometry. The VHH was demonstrated to bind intact A. baumannii cells by microscopy and whole cell ELISA.
In summary, OMV-based immunogens have been used to raise mAbs against targets that were subsequently identified through various techniques (Table 2). For some of these mAbs, robust binding data to native proteins and/or whole cells was not attempted or reported, and indirect validation techniques (e.g., complement-dependent bactericidal assays, whole cell dot blot) were used to infer target antigen binding, while in other cases, the functional activity of the mAbs beyond antigen binding was not directly tested. In most of the cases highlighted here, passive immunization with mAbs was not attempted but is expected to be critical in demonstrating their utility as alternatives to conventional antimicrobials. Similar to pAbs (Table 1, Supplementary Table S1), several of the targets recognized by the mAbs could have been shed from degraded OMVs or copurified with OMVs, limiting confidence that the OMVs themselves acted as the primary immunogen. In addition, many of the mAb targets are amenable to recombinant overexpression or purification/extraction from bacteria and could thus likely have been generated using conventional immunization strategies.
Perspectives on OMVs as immunogens
There are several opportunities and challenges in the use of gram-negative OMVs for the development of antimicrobial Abs. OMVs allow for the presentation of naturally OM-associated antigens to the immune system in a biologically relevant context without the need for complex purification and formulation processes. In this regard, they share similarities with live bacterial cells. OMVs are more convenient immunogens than bacterial cells due to their non-replicative nature, and because they lack the ability to cause infection in immunized animals, there are no concerns regarding gain of function gene transfer as in live cell immunizations. Interestingly, markers of immunogenicity such as dendritic cell activation and IgG titer have been found to be similar for OMVs and, in some cases, enhanced when compared to attenuated whole bacteria (Baker et al. 2021; Prior et al. 2021). For OMVs produced naturally by bacterial cells, factors such as endogenous protein folding, post-translational modification, oligomeric state, and binding interactions are expected to be largely preserved, whereas they may be compromised in a recombinant or purified antigen, an enriched OM protein preparation, or a killed bacterial cell preparation. It is less certain that chimeric exogenous antigens displayed on OMVs would maintain the same advantages as naturally OMV-associated antigens versus other types of immunogens. While using recombinant antigens for immunization and Ab screening makes target identification unnecessary, it introduces the potential for isolating Abs that fail to recognize native targets on live bacteria. Multiple-pass transmembrane proteins are important target antigens but are difficult to isolate and purify in their native conformations due to instability and aggregation propensity introduced by their transmembrane domains (Schlegel et al. 2014). Additionally, bacterial OMs are densely packed superstructures with a high degree of interaction between components. Isolation of antigens from the membrane architecture risks exposure of, and Ab generation to, inaccessible antigenic epitopes that would fail to be recognized by Abs on live whole cells. While the surfaces of OMVs may be imperfectly representative of the bacterial OM (van de Waterbeemd et al. 2013), they maintain some portion of the bacterial membrane architecture. This is especially important when considering antigens that have immunodominant epitopes that are sterically unavailable in a biological context, which would hinder the selection of Abs to subdominant but functional epitopes of non-native recombinant antigens. Additionally, OMV-based immunization may result in the discovery of unknown antigens or proteins which were not previously considered targets for Ab development. This ability may be important for rare and emerging bacterial pathogens for which extensive OM composition data are lacking.
In addition to reducing immune responses toward undesirable epitopes, OMV-based immunization can stimulate immune responses to weakly immunogenic epitopes through the presence of immunostimulatory molecules such as LPS (Piccioli et al. 2022b). As such, OMVs can be considered to naturally combine the functions of a lipid carrier and adjuvant. Studies comparing the immunogenicity of OMVs versus recombinant proteins combined with adjuvants have found similar or enhanced antibody titers using OMVs (Rosenthal et al. 2014; Rappazzo et al. 2016); however, additional studies are required to determine if the benefits of OMV immunizations are restricted to particular antigens and immunization strategies. For some applications (e.g., human therapy), immunization with sOMVs may induce undesirably strong immune responses; however, immunogenicity can be decreased through formulation modifications or genetic manipulation of LPS content (Rossi et al. 2021). Immunization with OMVs through the intramuscular, intraperitoneal, and subcutaneous routes typically elicits high serum IgG, IgM, and IgA titers in a variety of animal models. Additionally, intranasal immunization may elicit stronger secretory IgA responses (e.g., in saliva and the nasopharynx) with comparable serum titers (Gnopo et al. 2017).
While OMV-based immunization can be advantageous for rapid Ab discovery against OM targets, it also introduces challenges not present when using purified antigens. OMV membrane surfaces can retain soluble components originating from bacteria (e.g., shed components such as flagella, fimbrae, and pilins, as well as potentially components derived from cell lysis) or other sources (Bitar et al. 2019), which could result in the generation of immune responses to components that are not naturally associated with OMVs or the OM (Klimentova and Stulik 2015). Because of this, additional purification steps after initial OMV isolation may be necessary, such as density gradient centrifugation and/or size exclusion chromatography. Even these steps may be insufficient to remove components that do not significantly differ in size or density from OMVs and/or strongly associate with OMVs in a non-specific manner. OMVs may also have stability considerations that complicate their use as immunogens compared to a purified antigen. Due to the presence of enzymatic components in OMVs, as well as the possibility of membrane fusion, aggregation, and/or precipitation, preparation of fresh OMVs may be necessary throughout the immunization and Ab generation process. For example, dOMVs are less stable and more prone to aggregation compared to other OMV classes (van de Waterbeemd et al. 2010). The generation of pAb responses following OMV immunization to luminal cargo proteins suggests that degradation and cargo release can occur; degradation may also be associated with the loss of native structure of OM proteins.
Another challenge for OMV-based immunization is that the immune sera may contain Abs to a variety of OM antigens, as well as potentially to membrane-associated and/or shed antigens, requiring mAbs to a particular antigen of interest to be isolated. Target validation using OMV immunization-derived mAbs is challenging but necessary. While it may be possible to select mAbs to a particular target without a purified antigen using genetic knockout or overexpressing cell lines, in many cases, it is more practical to generate a recombinant antigen for Ab screening. However, for difficult to purify antigens, Ab selection can be performed using the immunized OMV, with obtained mAb sequences analyzed for binding using western blot and mass spectrometry. Alternatively, a heterologous OMV or lipid carrier expressing the antigen of interest can be used to attempt to enrich for a defined antigen. While OMV immunization may be expected to result in the generation of Abs that bind OM targets on live cells, validation of cell binding using knockout and/or antigen-overexpressing strains, immunoprecipitation, or other complementary methods should be performed following antigen identification.
Conclusions
OMVs and other types of bacterial EVs represent useful tools for the generation of Abs that targets the bacterial OM. In particular, they offer important theoretical advantages when attempting to generate Abs against challenging targets such as integral OM proteins; however, very few mAbs raised by OMV-based immunization to date have been conclusively shown to target these complex proteins in their native contexts. Challenges of OMV-based immunogens include potential copurification of immunogenic large extracellular material, non-specific association of soluble molecules with OMV surfaces, OMV degradation leading to loss of native OM architecture, and requirement for post-hoc antigen identification. The development of specific, high-affinity mAbs to bacterial membrane targets will be key to future efforts in antimicrobial drug development, diagnostic testing, and basic microbiology. As the development of antimicrobial resistance and epidemiological pressures increase the need for novel bacterial monitoring and treatment methods, Abs capable of targeting live bacteria are likely to be of increasing importance. OMV-based immunization, while in its relative infancy, fulfills a niche as it allows for rapid Ab generation against immunogenic OM targets, even for emerging or relatively unstudied pathogens.
References
Adriani R, Mousavi Gargari SL, Nazarian S, Sarvary S, Noroozi N (2018) Immunogenicity of Vibrio cholerae outer membrane vesicles secreted at various environmental conditions. Vaccine 36:322–330. https://doi.org/10.1016/j.vaccine.2017.09.004
Alfini R, Brunelli B, Bartolini E, Carducci M, Luzzi E, Ferlicca F, Buccato S, Galli B, Lo Surdo P, Scarselli M, Romagnoli G, Cartocci E, Maione D, Savino S, Necchi F, Delany I, Micoli F (2022) Investigating the role of antigen orientation on the immune response elicited by Neisseria meningitidis factor H binding protein on GMMA. Vaccines (Basel) 10:1182. https://doi.org/10.3390/vaccines10081182
Arato V, Oldrini D, Massai L, Gasperini G, Necchi F, Micoli F (2021) Impact of O-acetylation on S. flexneri 1b and 2a O-antigen immunogenicity in mice. Microorganisms 9:2360. https://doi.org/10.3390/microorganisms9112360
Arigita C, Kersten GF, Hazendonk T, Hennink WE, Crommelin DJ, Jiskoot W (2003) Restored functional immunogenicity of purified meningococcal PorA by incorporation into liposomes. Vaccine 21:950–960. https://doi.org/10.1016/s0264-410x(02)00546-7
Awanye AM, Chang CM, Wheeler JX, Chan H, Marsay L, Dold C, Rollier CS, Bird LE, Nettleship JE, Owens RJ, Pollard AJ, Derrick JP (2019) Immunogenicity profiling of protein antigens from capsular group B Neisseria meningitidis. Sci Rep 9:6843. https://doi.org/10.1038/s41598-019-43139-0
Ayalew S, Confer AW, Shrestha B, Wilson AE, Montelongo M (2013) Proteomic analysis and immunogenicity of Mannheimia haemolytica vesicles. Clin Vaccine Immunol 20:191–196. https://doi.org/10.1128/CVI.00622-12
Bai D, Nakao R, Ito A, Uematsu H, Senpuku H (2015) Immunoreactive antigens recognized in serum samples from mice intranasally immunized with Porphyromonas gingivalis outer membrane vesicles. Pathog Dis 73:ftu006. https://doi.org/10.1093/femspd/ftu006
Baker SM, Settles EW, Davitt C, Gellings P, Kikendall N, Hoffmann J, Wang Y, Bitoun J, Lodrigue KR, Sahl JW, Keim P, Roy C, McLachlan J, Morici LA (2021) Burkholderia pseudomallei OMVs derived from infection mimicking conditions elicit similar protection to a live-attenuated vaccine. NPJ Vaccines 6:18. https://doi.org/10.1038/s41541-021-00281-z
Balhuizen MD, Veldhuizen EJA, Haagsman HP (2021) Outer membrane vesicle induction and isolation for vaccine development. Front Microbiol 12:629090. https://doi.org/10.3389/fmicb.2021.629090
Bartolini E, Ianni E, Frigimelica E, Petracca R, Galli G, Berlanda Scorza F, Norais N, Laera D, Giusti F, Pierleoni A, Donati M, Cevenini R, Finco O, Grandi G, Grifantini R (2013) Recombinant outer membrane vesicles carrying Chlamydia muridarum HtrA induce antibodies that neutralize chlamydial infection in vitro. J Extracell Vesicles 2:20181. https://doi.org/10.3402/jev.v2i0.20181
Bash MC, Lynn F, Concepcion NF, Tappero JW, Carlone GM, Frasch CE (2000) Genetic and immunologic characterization of a novel serotype 4, 15 strain of Neisseria meningitidis. FEMS Immunol Med Microbiol 29:169–176. https://doi.org/10.1111/j.1574-695X.2000.tb01519.x
Beernink PT, Shaughnessy J, Pajon R, Braga EM, Ram S, Granoff DM (2012) The effect of human factor H on immunogenicity of meningococcal native outer membrane vesicle vaccines with over-expressed factor H binding protein. PLoS Pathog 8:e1002688. https://doi.org/10.1371/journal.ppat.1002688
Beernink PT, Ispasanie E, Lewis LA, Ram S, Moe GR, Granoff DM (2019a) A meningococcal native outer membrane vesicle vaccine with attenuated endotoxin and overexpressed factor H binding protein elicits gonococcal bactericidal antibodies. J Infect Dis 219:1130–1137. https://doi.org/10.1093/infdis/jiy609
Beernink PT, Vianzon V, Lewis LA, Moe GR, Granoff DM (2019b) A meningococcal outer membrane vesicle vaccine with overexpressed mutant fHbp elicits higher protective antibody responses in infant rhesus macaques than a licensed serogroup B vaccine. mBio 10:e01231-19. https://doi.org/10.1128/mBio.01231-19
Bishop AL, Schild S, Patimalla B, Klein B, Camilli A (2010) Mucosal immunization with Vibrio cholerae outer membrane vesicles provides maternal protection mediated by antilipopolysaccharide antibodies that inhibit bacterial motility. Infect Immun 78:4402–4420. https://doi.org/10.1128/IAI.00398-10
Bitar A, Aung KM, Wai SN, Hammarstrom ML (2019) Vibrio cholerae derived outer membrane vesicles modulate the inflammatory response of human intestinal epithelial cells by inducing microRNA-146a. Sci Rep 9:7212. https://doi.org/10.1038/s41598-019-43691-9
Bitto NJ, Chapman R, Pidot S, Costin A, Lo C, Choi J, D’Cruze T, Reynolds EC, Dashper SG, Turnbull L, Whitchurch CB, Stinear TP, Stacey KJ, Ferrero RL (2017) Bacterial membrane vesicles transport their DNA cargo into host cells. Sci Rep 7:7072. https://doi.org/10.1038/s41598-017-07288-4
Blanco DR, Champion CI, Dooley A, Cox DL, Whitelegge JP, Faull K, Lovett MA (2005) A monoclonal antibody that conveys in vitro killing and partial protection in experimental syphilis binds a phosphorylcholine surface epitope of Treponema pallidum. Infect Immun 73:3083–3095. https://doi.org/10.1128/IAI.73.5.3083-3095.2005
Bonnington KE, Kuehn MJ (2014) Protein selection and export via outer membrane vesicles. Biochim Biophys Acta 1843:1612–1619. https://doi.org/10.1016/j.bbamcr.2013.12.011
Bose S, Aggarwal S, Singh DV, Acharya N (2020) Extracellular vesicles: an emerging platform in gram-positive bacteria. Microb Cell 7:312–322. https://doi.org/10.15698/mic2020.12.737
Bottero D, Zurita ME, Gaillard ME, Bartel E, Vercellini C, Hozbor D (2018) Membrane vesicles derived from Bordetella bronchiseptica: active constituent of a new vaccine against infections caused by this pathogen. Appl Environ Microbiol 84:e01877-e1917. https://doi.org/10.1128/AEM.01877-17
Carvalho AL, Fonseca S, Miquel-Clopes A, Cross K, Kok KS, Wegmann U, Gil-Cordoso K, Bentley EG, Al Katy SHM, Coombes JL, Kipar A, Stentz R, Stewart JP, Carding SR (2019a) Bioengineering commensal bacteria-derived outer membrane vesicles for delivery of biologics to the gastrointestinal and respiratory tract. J Extracell Vesicles 8:1632100. https://doi.org/10.1080/20013078.2019.1632100
Carvalho AL, Miquel-Clopes A, Wegmann U, Jones E, Stentz R, Telatin A, Walker NJ, Butcher WA, Brown PJ, Holmes S, Dennis MJ, Williamson ED, Funnell SGP, Stock M, Carding SR (2019b) Use of bioengineered human commensal gut bacteria-derived microvesicles for mucosal plague vaccine delivery and immunization. Clin Exp Immunol 196:287–304. https://doi.org/10.1111/cei.13301
Castilla J, Garcia Cenoz M, Abad R, Sanchez-Cambronero L, Lorusso N, Izquierdo C, Canellas Llabres S, Roig J, Malvar A, Gonzalez Carril F, Boone ALD, Perez Martin J, Rodriguez Recio MJ, Galmes A, Caballero A, Garcia Rojas A, Juanas F, Nieto M, Viloria Raymundo LJ, Martinez Ochoa E, Rivas AI, Castrillejo D, Moreno Perez D, Martinez A, Borras E, Sanchez Gomez A, Pastor E, Nartallo V, Arteagoitia JM, Alvarez-Fernandez B, Garcia Pina R, Fernandez Arribas S, Vanrell J, Garcia Hernandez S, Mendoza RM, Mendez M, Lopez-Tercero MM, Fernandez-Rodriguez A, Blanco A, Carrillo de Albornoz FJ, Ruiz Olivares J, Ruiz-Montero R, Limia A, Navarro-Alonso JA, Vazquez JA, Barricarte A (2023) Effectiveness of a meningococcal group B vaccine (4CMenB) in children. N Engl J Med 388:427–438. https://doi.org/10.1056/NEJMoa2206433
Chen L, Valentine JL, Huang CJ, Endicott CE, Moeller TD, Rasmussen JA, Fletcher JR, Boll JM, Rosenthal JA, Dobruchowska J, Wang Z, Heiss C, Azadi P, Putnam D, Trent MS, Jones BD, DeLisa MP (2016) Outer membrane vesicles displaying engineered glycotopes elicit protective antibodies. Proc Natl Acad Sci USA 113:E3609-3618. https://doi.org/10.1073/pnas.1518311113
Ciofu O, Beveridge TJ, Kadurugamuwa J, Walther-Rasmussen J, Hoiby N (2000) Chromosomal beta-lactamase is packaged into membrane vesicles and secreted from Pseudomonas aeruginosa. J Antimicrob Chemother 45:9–13. https://doi.org/10.1093/jac/45.1.9
Dalseg R, Wedege E, Holst J, Haugen IL, Hoiby EA, Haneberg B (1999) Outer membrane vesicles from group B meningococci are strongly immunogenic when given intranasally to mice. Vaccine 17:2336–2345. https://doi.org/10.1016/s0264-410x(99)00046-8
Daniels-Treffandier H, de Nie K, Marsay L, Dold C, Sadarangani M, Reyes-Sandoval A, Langford PR, Wyllie D, Hill F, Pollard AJ, Rollier CS (2016) Impact of reducing complement inhibitor binding on the immunogenicity of native Neisseria meningitidis outer membrane vesicles. PLoS One 11:e0148840. https://doi.org/10.1371/journal.pone.0148840
De Benedetto G, Alfini R, Cescutti P, Caboni M, Lanzilao L, Necchi F, Saul A, MacLennan CA, Rondini S, Micoli F (2017) Characterization of O-antigen delivered by Generalized Modules for Membrane Antigens (GMMA) vaccine candidates against nontyphoidal Salmonella. Vaccine 35:419–426. https://doi.org/10.1016/j.vaccine.2016.11.089
Dehinwal R, Cooley D, Rakov AV, Alugupalli AS, Harmon J, Cunrath O, Vallabhajosyula P, Bumann D, Schifferli DM (2021) Increased production of outer membrane vesicles by Salmonella interferes with complement-mediated innate immune attack. mBio 12:e0086921. https://doi.org/10.1128/mBio.00869-21
Dell’Annunziata F, Folliero V, Giugliano R, De Filippis A, Santarcangelo C, Izzo V, Daglia M, Galdiero M, Arciola CR, Franci G (2021) Gene transfer potential of outer membrane vesicles of gram-negative bacteria. Int J Mol Sci 22:5985. https://doi.org/10.3390/ijms22115985
Delvig AA, Wedege E, Caugant DA, Dalseg R, Kolberg J, Achtman M, Rosenqvist E (1995) A linear B-cell epitope on the class 3 outer-membrane protein of Neisseria meningitidis recognized after vaccination with the Norwegian group B outer-membrane vesicle vaccine. Microbiology (Reading) 141(Pt 7):1593–1600. https://doi.org/10.1099/13500872-141-7-1593
Devi SJ, Karpas AB, Frasch CE (1996) Binding diversity of monoclonal antibodies to α(2→8) polysialic acid conjugated to outer membrane vesicle via adipic acid dihydrazide. FEMS Immunol Med Microbiol 14:211–220. https://doi.org/10.1111/j.1574-695X.1996.tb00289.x
Devi SJ, Zollinger WD, Snoy PJ, Tai JY, Costantini P, Norelli F, Rappuoli R, Frasch CE (1997) Preclinical evaluation of group B Neisseria meningitidis and Escherichia coli K92 capsular polysaccharide-protein conjugate vaccines in juvenile rhesus monkeys. Infect Immun 65:1045–1052. https://doi.org/10.1128/IAI.65.3.1045-1052.1997
Fantappie L, de Santis M, Chiarot E, Carboni F, Bensi G, Jousson O, Margarit I, Grandi G (2014) Antibody-mediated immunity induced by engineered Escherichia coli OMVs carrying heterologous antigens in their lumen. J Extracell Vesicles 3:24015. https://doi.org/10.3402/jev.v3.24015
Fiorino F, Pettini E, Koeberling O, Ciabattini A, Pozzi G, Martin LB, Medaglini D (2021) Long-term anti-bacterial immunity against systemic infection by Salmonella enterica serovar Typhimurium elicited by a GMMA-based vaccine. Vaccines (Basel) 9:495. https://doi.org/10.3390/vaccines9050495
Frenck RW Jr, Conti V, Ferruzzi P, Ndiaye AGW, Parker S, McNeal MM, Dickey M, Granada JP, Cilio GL, De Ryck I, Necchi F, Suvarnapunya AE, Rossi O, Acquaviva A, Chandrasekaran L, Clarkson KA, Auerbach J, Marchetti E, Kaminski RW, Micoli F, Rappuoli R, Saul A, Martin LB, Podda A (2021) Efficacy, safety, and immunogenicity of the Shigella sonnei 1790GAHB GMMA candidate vaccine: results from a phase 2b randomized, placebo-controlled challenge study in adults. EClinicalMedicine 39:101076. https://doi.org/10.1016/j.eclinm.2021.101076
Fukasawa LO, Gorla MC, Schenkman RP, Garcia LR, Carneiro SM, Raw I, Tanizaki MM (1999) Neisseria meningitidis serogroup C polysaccharide and serogroup B outer membrane vesicle conjugate as a bivalent meningococcus vaccine candidate. Vaccine 17:2951–2958
Fukasawa LO, Gorla MCO, Lemos APS, Schenkman RPF, Brandileone MCC, Fox JW, Raw I, Frasch CE, Tanizaki MM (2003) Immune response to native NadA from Neisseria meningitidis and its expression in clinical isolates in Brazil. J Med Microbiol 52(Pt 2):121–125. https://doi.org/10.1099/jmm.0.05017-0
Gasperini G, Biagini M, Arato V, Gianfaldoni C, Vadi A, Norais N, Bensi G, Delany I, Pizza M, Arico B, Leuzzi R (2018) Outer membrane vesicles (OMV)-based and proteomics-driven antigen selection identifies novel factors contributing to Bordetella pertussis adhesion to epithelial cells. Mol Cell Proteomics 17:205–215. https://doi.org/10.1074/mcp.RA117.000045
Gasperini G, Alfini R, Arato V, Mancini F, Aruta MG, Kanvatirth P, Pickard D, Necchi F, Saul A, Rossi O, Micoli F, Mastroeni P (2021a) Salmonella Paratyphi A outer membrane vesicles displaying Vi polysaccharide as a multivalent vaccine against enteric fever. Infect Immun 89:e00699-e720. https://doi.org/10.1128/IAI.00699-20
Gasperini G, Raso MM, Arato V, Aruta MG, Cescutti P, Necchi F, Micoli F (2021b) Effect of O-antigen chain length regulation on the immunogenicity of Shigella and Salmonella Generalized Modules for Membrane Antigens (GMMA). Int J Mol Sci 22:1309. https://doi.org/10.3390/ijms22031309
Gerke C, Colucci AM, Giannelli C, Sanzone S, Vitali CG, Sollai L, Rossi O, Martin LB, Auerbach J, Di Cioccio V, Saul A (2015) Production of a Shigella sonnei vaccine based on Generalized Modules for Membrane Antigens (GMMA), 1790GAHB. PLoS One 10:e0134478. https://doi.org/10.1371/journal.pone.0134478
Gnopo YMD, Watkins HC, Stevenson TC, DeLisa MP, Putnam D (2017) Designer outer membrane vesicles as immunomodulatory systems - reprogramming bacteria for vaccine delivery. Adv Drug Deliv Rev 114:132–142. https://doi.org/10.1016/j.addr.2017.05.003
Granoff DM, Costa I, Konar M, Giuntini S, Van Rompay KK, Beernink PT (2015) Binding of complement factor H (FH) decreases protective anti-FH binding protein antibody responses of infant rhesus macaques immunized with a meningococcal serogroup B vaccine. J Infect Dis 212:784–792. https://doi.org/10.1093/infdis/jiv081
Gulig PA, Hansen EJ (1985) Coprecipitation of lipopolysaccharide and the 39,000-molecular-weight major outer membrane protein of Haemophilus influenzae type b by lipopolysaccharide-directed monoclonal antibody. Infect Immun 49:819–827. https://doi.org/10.1128/iai.49.3.819-827.1985
Haneberg B, Dalseg R, Wedege E, Hoiby EA, Haugen IL, Oftung F, Andersen SR, Naess LM, Aase A, Michaelsen TE, Holst J (1998) Intranasal administration of a meningococcal outer membrane vesicle vaccine induces persistent local mucosal antibodies and serum antibodies with strong bactericidal activity in humans. Infect Immun 66:1334–1341. https://doi.org/10.1128/IAI.66.4.1334-1341.1998
Hays MP, Houben D, Yang Y, Luirink J, Hardwidge PR (2018) Immunization with Skp delivered on outer membrane vesicles protects mice against enterotoxigenic Escherichia coli challenge. Front Cell Infect Microbiol 8:132. https://doi.org/10.3389/fcimb.2018.00132
Helminen ME, Maciver I, Latimer JL, Cope LD, McCracken GH Jr, Hansen EJ (1993) A major outer membrane protein of Moraxella catarrhalis is a target for antibodies that enhance pulmonary clearance of the pathogen in an animal model. Infect Immun 61:2003–2010. https://doi.org/10.1128/iai.61.5.2003-2010.1993
Helminen ME, Maciver I, Latimer JL, Klesney-Tait J, Cope LD, Paris M, McCracken GH Jr, Hansen EJ (1994) A large, antigenically conserved protein on the surface of Moraxella catarrhalis is a target for protective antibodies. J Infect Dis 170:867–872. https://doi.org/10.1093/infdis/170.4.867
Hijiya T, Shibata Y, Hayakawa M, Abiko Y (2010) A monoclonal antibody against fimA type II Porphyromonas gingivalis inhibits IL-8 production in human gingival fibroblasts. Hybridoma (Larchmt) 29:201–204. https://doi.org/10.1089/hyb.2009.0109
Hou VC, Koeberling O, Welsch JA, Granoff DM (2005) Protective antibody responses elicited by a meningococcal outer membrane vesicle vaccine with overexpressed genome-derived neisserial antigen 1870. J Infect Dis 192:580–590. https://doi.org/10.1086/432102
Howlader DR, Koley H, Sinha R, Maiti S, Bhaumik U, Mukherjee P, Dutta S (2018) Development of a novel S. Typhi and Paratyphi A outer membrane vesicles based bivalent vaccine against enteric fever. PLoS One 13:e0203631. https://doi.org/10.1371/journal.pone.0203631
Hu R, Li J, Zhao Y, Lin H, Liang L, Wang M, Liu H, Min Y, Gao Y, Yang M (2020) Exploiting bacterial outer membrane vesicles as a cross-protective vaccine candidate against avian pathogenic Escherichia coli (APEC). Microb Cell Fact 19:119. https://doi.org/10.1186/s12934-020-01372-7
Huang W, Wang S, Yao Y, Xia Y, Yang X, Li K, Sun P, Liu C, Sun W, Bai H, Chu X, Li Y, Ma Y (2016) Employing Escherichia coli-derived outer membrane vesicles as an antigen delivery platform elicits protective immunity against Acinetobacter baumannii infection. Sci Rep 6:37242. https://doi.org/10.1038/srep37242
Huang W, Zhang Q, Li W, Chen Y, Shu C, Li Q, Zhou J, Ye C, Bai H, Sun W, Yang X, Ma Y (2019) Anti-outer membrane vesicle antibodies increase antibiotic sensitivity of pan-drug-resistant Acinetobacter baumannii. Front Microbiol 10:1379. https://doi.org/10.3389/fmicb.2019.01379
Jan AT (2017) Outer membrane vesicles (OMVs) of gram-negative bacteria: a perspective update. Front Microbiol 8:1053. https://doi.org/10.3389/fmicb.2017.01053
Kanojia G, Raeven RHM, van der Maas L, Bindels THE, van Riet E, Metz B, Soema PC, Ten Have R, Frijlink HW, Amorij JP, Kersten GFA (2018) Development of a thermostable spray dried outer membrane vesicle pertussis vaccine for pulmonary immunization. J Control Release 286:167–178. https://doi.org/10.1016/j.jconrel.2018.07.035
Keenan J, Oliaro J, Domigan N, Potter H, Aitken G, Allardyce R, Roake J (2000) Immune response to an 18-kilodalton outer membrane antigen identifies lipoprotein 20 as a Helicobacter pylori vaccine candidate. Infect Immun 68:3337–3343. https://doi.org/10.1128/IAI.68.6.3337-3343.2000
Keiser PB, Biggs-Cicatelli S, Moran EE, Schmiel DH, Pinto VB, Burden RE, Miller LB, Moon JE, Bowden RA, Cummings JF, Zollinger WD (2011) A phase 1 study of a meningococcal native outer membrane vesicle vaccine made from a group B strain with deleted lpxL1 and synX, over-expressed factor H binding protein, two PorAs and stabilized OpcA expression. Vaccine 29:1413–1420. https://doi.org/10.1016/j.vaccine.2010.12.039
Kim JY, Doody AM, Chen DJ, Cremona GH, Shuler ML, Putnam D, DeLisa MP (2008) Engineered bacterial outer membrane vesicles with enhanced functionality. J Mol Biol 380:51–66. https://doi.org/10.1016/j.jmb.2008.03.076
Klimentova J, Stulik J (2015) Methods of isolation and purification of outer membrane vesicles from gram-negative bacteria. Microbiol Res 170:1–9. https://doi.org/10.1016/j.micres.2014.09.006
Klouwens MJ, Salverda MLM, Trentelman JJ, Ersoz JI, Wagemakers A, Gerritzen MJH, van der Ley PA, Hovius JW (2021) Vaccination with meningococcal outer membrane vesicles carrying Borrelia OspA protects against experimental Lyme borreliosis. Vaccine 39:2561–2567. https://doi.org/10.1016/j.vaccine.2021.03.059
Koeberling O, Welsch JA, Granoff DM (2007) Improved immunogenicity of a H44/76 group B outer membrane vesicle vaccine with over-expressed genome-derived Neisserial antigen 1870. Vaccine 25:1912–1920. https://doi.org/10.1016/j.vaccine.2006.03.092
Koeberling O, Seubert A, Granoff DM (2008) Bactericidal antibody responses elicited by a meningococcal outer membrane vesicle vaccine with overexpressed factor H-binding protein and genetically attenuated endotoxin. J Infect Dis 198:262–270. https://doi.org/10.1086/589308
Koeberling O, Giuntini S, Seubert A, Granoff DM (2009) Meningococcal outer membrane vesicle vaccines derived from mutant strains engineered to express factor H binding proteins from antigenic variant groups 1 and 2. Clin Vaccine Immunol 16:156–162. https://doi.org/10.1128/CVI.00403-08
Koeberling O, Delany I, Granoff DM (2011a) A critical threshold of meningococcal factor H binding protein expression is required for increased breadth of protective antibodies elicited by native outer membrane vesicle vaccines. Clin Vaccine Immunol 18:736–742. https://doi.org/10.1128/CVI.00542-10
Koeberling O, Seubert A, Santos G, Colaprico A, Ugozzoli M, Donnelly J, Granoff DM (2011b) Immunogenicity of a meningococcal native outer membrane vesicle vaccine with attenuated endotoxin and over-expressed factor H binding protein in infant rhesus monkeys. Vaccine 29:4728–4734. https://doi.org/10.1016/j.vaccine.2011.04.095
Koeberling O, Ispasanie E, Hauser J, Rossi O, Pluschke G, Caugant DA, Saul A, MacLennan CA (2014) A broadly-protective vaccine against meningococcal disease in sub-Saharan Africa based on Generalized Modules for Membrane Antigens (GMMA). Vaccine 32:2688–2695. https://doi.org/10.1016/j.vaccine.2014.03.068
Konig E, Gagliardi A, Riedmiller I, Andretta C, Tomasi M, Irene C, Frattini L, Zanella I, Berti F, Grandi A, Caproni E, Fantappie L, Grandi G (2021) Multi-antigen outer membrane vesicle engineering to develop polyvalent vaccines: the Staphylococcus aureus case. Front Immunol 12:752168. https://doi.org/10.3389/fimmu.2021.752168
Kuipers K, Daleke-Schermerhorn MH, Jong WS, ten Hagen-Jongman CM, van Opzeeland F, Simonetti E, Luirink J, de Jonge MI (2015) Salmonella outer membrane vesicles displaying high densities of pneumococcal antigen at the surface offer protection against colonization. Vaccine 33:2022–2029. https://doi.org/10.1016/j.vaccine.2015.03.010
Kulp A, Kuehn MJ (2010) Biological functions and biogenesis of secreted bacterial outer membrane vesicles. Annu Rev Microbiol 64:163–184. https://doi.org/10.1146/annurev.micro.091208.073413
Launay O, Lewis DJM, Anemona A, Loulergue P, Leahy J, Scire AS, Maugard A, Marchetti E, Zancan S, Huo Z, Rondini S, Marhaba R, Finco O, Martin LB, Auerbach J, Cohen D, Saul A, Gerke C, Podda A (2017) Safety profile and immunologic responses of a novel vaccine against Shigella sonnei administered intramuscularly, intradermally and intranasally: results from two parallel randomized phase 1 clinical studies in healthy adult volunteers in Europe. EBioMedicine 22:164–172. https://doi.org/10.1016/j.ebiom.2017.07.013
Launay O, Ndiaye AGW, Conti V, Loulergue P, Scire AS, Landre AM, Ferruzzi P, Nedjaai N, Schutte LD, Auerbach J, Marchetti E, Saul A, Martin LB, Podda A (2019) Booster vaccination with GVGH Shigella sonnei 1790GAHB GMMA vaccine compared to single vaccination in unvaccinated healthy European adults: results from a phase 1 clinical trial. Front Immunol 10:335. https://doi.org/10.3389/fimmu.2019.00335
Leduc I, Connolly KL, Begum A, Underwood K, Darnell S, Shafer WM, Balthazar JT, Macintyre AN, Sempowski GD, Duncan JA, Little MB, Rahman N, Garges EC, Jerse AE (2020) The serogroup B meningococcal outer membrane vesicle-based vaccine 4CMenB induces cross-species protection against Neisseria gonorrhoeae. PLoS Pathog 16:e1008602. https://doi.org/10.1371/journal.ppat.1008602
Lee EY, Bang JY, Park GW, Choi DS, Kang JS, Kim HJ, Park KS, Lee JO, Kim YK, Kwon KH, Kim KP, Gho YS (2007) Global proteomic profiling of native outer membrane vesicles derived from Escherichia coli. Proteomics 7:3143–3153. https://doi.org/10.1002/pmic.200700196
Lei EK, Ryan S, van Faassen H, Foss M, Robotham A, Baltat I, Fulton K, Henry KA, Chen W, Hussack G (2023) Isolation and characterization of a VHH targeting the Acinetobacter baumannii cell surface protein CsuA/B. Appl Microbiol Biotechnol 107:4567–4580. https://doi.org/10.1007/s00253-023-12594-1
Leitner DR, Feichter S, Schild-Prufert K, Rechberger GN, Reidl J, Schild S (2013) Lipopolysaccharide modifications of a cholera vaccine candidate based on outer membrane vesicles reduce endotoxicity and reveal the major protective antigen. Infect Immun 81:2379–2393. https://doi.org/10.1128/IAI.01382-12
Leitner DR, Lichtenegger S, Temel P, Zingl FG, Ratzberger D, Roier S, Schild-Prufert K, Feichter S, Reidl J, Schild S (2015) A combined vaccine approach against Vibrio cholerae and ETEC based on outer membrane vesicles. Front Microbiol 6:823. https://doi.org/10.3389/fmicb.2015.00823
Li Q, Zhou G, Fei X, Tian Y, Wang S, Shi H (2023) Engineered bacterial outer membrane vesicles with lipidated heterologous antigen as an adjuvant-free vaccine platform for Streptococcus suis. Appl Environ Microbiol 89:e0204722. https://doi.org/10.1128/aem.02047-22
Li P, Wang X, Sun X, Guan Z, Sun W (2021) Outer membrane vesicles displaying a heterologous PcrV-HitA fusion antigen promote protection against pulmonary Pseudomonas aeruginosa infection. mSphere 6:e0069921. https://doi.org/10.1128/mSphere.00699-21
Lieberman LA (2022) Outer membrane vesicles: a bacterial-derived vaccination system. Front Microbiol 13:1029146. https://doi.org/10.3389/fmicb.2022.1029146
Liu Q, Liu Q, Yi J, Liang K, Liu T, Roland KL, Jiang Y, Kong Q (2016) Outer membrane vesicles derived from Salmonella Typhimurium mutants with truncated LPS induce cross-protective immune responses against infection of Salmonella enterica serovars in the mouse model. Int J Med Microbiol 306:697–706. https://doi.org/10.1016/j.ijmm.2016.08.004
Liu Q, Yi J, Liang K, Zhang X, Liu Q (2017) Outer membrane vesicles derived from Salmonella enteritidis protect against the virulent wild-type strain infection in a mouse model. J Microbiol Biotechnol 27:1519–1528. https://doi.org/10.4014/jmb.1705.05028
Mancini F, Gasperini G, Rossi O, Aruta MG, Raso MM, Alfini R, Biagini M, Necchi F, Micoli F (2021) Dissecting the contribution of O-antigen and proteins to the immunogenicity of Shigella sonnei generalized modules for membrane antigens (GMMA). Sci Rep 11:906. https://doi.org/10.1038/s41598-020-80421-y
Mancini F, Alfini R, Caradonna V, Monaci V, Carducci M, Gasperini G, Piccioli D, Biagini M, Giannelli C, Rossi O, Pizza M, Micoli F (2023) Exploring the role of GMMA components in the immunogenicity of a 4-valent vaccine against Shigella. Int J Mol Sci 24:2742. https://doi.org/10.3390/ijms24032742
Manning AJ, Kuehn MJ (2011) Contribution of bacterial outer membrane vesicles to innate bacterial defense. BMC Microbiol 11:258. https://doi.org/10.1186/1471-2180-11-258
Marini A, Rossi O, Aruta MG, Micoli F, Rondini S, Guadagnuolo S, Delany I, Henderson IR, Cunningham AF, Saul A, MacLennan CA, Koeberling O (2017) Contribution of factor H-binding protein sequence to the cross-reactivity of meningococcal native outer membrane vesicle vaccines with over-expressed fHbp variant group 1. PLoS One 12:e0181508. https://doi.org/10.1371/journal.pone.0181508
Martin DR, Ruijne N, McCallum L, O’Hallahan J, Oster P (2006) The VR2 epitope on the PorA P1.7-2,4 protein is the major target for the immune response elicited by the strain-specific group B meningococcal vaccine MeNZB. Clin Vaccine Immunol 13:486–491. https://doi.org/10.1128/CVI.13.4.486-491.2006
Matthias KA, Reveille A, Connolly KL, Jerse AE, Gao YS, Bash MC (2020) Deletion of major porins from meningococcal outer membrane vesicle vaccines enhances reactivity against heterologous serogroup B Neisseria meningitidis strains. Vaccine 38:2396–2405. https://doi.org/10.1016/j.vaccine.2020.01.038
Matthias KA, Connolly KL, Begum AA, Jerse AE, Macintyre AN, Sempowski GD, Bash MC (2022) Meningococcal detoxified outer membrane vesicle vaccines enhance gonococcal clearance in a murine infection model. J Infect Dis 225:650–660. https://doi.org/10.1093/infdis/jiab450
McBroom AJ, Kuehn MJ (2007) Release of outer membrane vesicles by gram-negative bacteria is a novel envelope stress response. Mol Microbiol 63:545–558. https://doi.org/10.1111/j.1365-2958.2006.05522.x
McBroom AJ, Johnson AP, Vemulapalli S, Kuehn MJ (2006) Outer membrane vesicle production by Escherichia coli is independent of membrane instability. J Bacteriol 188:5385–5392. https://doi.org/10.1128/JB.00498-06
McConnell MJ, Rumbo C, Bou G, Pachon J (2011) Outer membrane vesicles as an acellular vaccine against Acinetobacter baumannii. Vaccine 29:5705–5710. https://doi.org/10.1016/j.vaccine.2011.06.001
Micoli F, MacLennan CA (2020) Outer membrane vesicle vaccines. Semin Immunol 50:101433. https://doi.org/10.1016/j.smim.2020.101433
Micoli F, Rondini S, Alfini R, Lanzilao L, Necchi F, Negrea A, Rossi O, Brandt C, Clare S, Mastroeni P, Rappuoli R, Saul A, MacLennan CA (2018) Comparative immunogenicity and efficacy of equivalent outer membrane vesicle and glycoconjugate vaccines against nontyphoidal Salmonella. Proc Natl Acad Sci USA 115:10428–10433. https://doi.org/10.1073/pnas.1807655115
Micoli F, Alfini R, Di Benedetto R, Necchi F, Schiavo F, Mancini F, Carducci M, Palmieri E, Balocchi C, Gasperini G, Brunelli B, Costantino P, Adamo R, Piccioli D, Saul A (2020) GMMA is a versatile platform to design effective multivalent combination vaccines. Vaccines (Basel) 8:540. https://doi.org/10.3390/vaccines8030540
Micoli F, Rossi O, Conti V, Launay O, Scire AS, Aruta MG, Nakakana UN, Marchetti E, Rappuoli R, Saul A, Martin LB, Necchi F, Podda A (2021) Antibodies elicited by the Shigella sonnei GMMA vaccine in adults trigger complement-mediated serum bactericidal activity: results from a phase 1 dose escalation trial followed by a booster extension. Front Immunol 12:671325. https://doi.org/10.3389/fimmu.2021.671325
Mitra S, Barman S, Nag D, Sinha R, Saha DR, Koley H (2012) Outer membrane vesicles of Shigella boydii type 4 induce passive immunity in neonatal mice. FEMS Immunol Med Microbiol 66:240–250. https://doi.org/10.1111/j.1574-695X.2012.01004.x
Mitra S, Chakrabarti MK, Koley H (2013) Multi-serotype outer membrane vesicles of Shigellae confer passive protection to the neonatal mice against shigellosis. Vaccine 31:3163–3173. https://doi.org/10.1016/j.vaccine.2013.05.001
Moe GR, Zuno-Mitchell P, Lee SS, Lucas AH, Granoff DM (2001) Functional activity of anti-neisserial surface protein A monoclonal antibodies against strains of Neisseria meningitidis serogroup B. Infect Immun 69:3762–3771. https://doi.org/10.1128/IAI.69.6.3762-3771.2001
Moe GR, Zuno-Mitchell P, Hammond SN, Granoff DM (2002) Sequential immunization with vesicles prepared from heterologous Neisseria meningitidis strains elicits broadly protective serum antibodies to group B strains. Infect Immun 70:6021–6031. https://doi.org/10.1128/IAI.70.11.6021-6031.2002
Muralinath M, Kuehn MJ, Roland KL, Curtiss R 3rd (2011) Immunization with Salmonella enterica serovar Typhimurium-derived outer membrane vesicles delivering the pneumococcal protein PspA confers protection against challenge with Streptococcus pneumoniae. Infect Immun 79:887–894. https://doi.org/10.1128/IAI.00950-10
Murphy K, Park AJ, Hao Y, Brewer D, Lam JS, Khursigara CM (2014) Influence of O polysaccharides on biofilm development and outer membrane vesicle biogenesis in Pseudomonas aeruginosa PAO1. J Bacteriol 196:1306–1317. https://doi.org/10.1128/JB.01463-13
Nagakubo T, Nomura N, Toyofuku M (2020) Cracking open bacterial membrane vesicles. Front Microbiol 10:3026. https://doi.org/10.3389/fmicb.2019.03026
Nagaputra JC, Rollier CS, Sadarangani M, Hoe JC, Mehta OH, Norheim G, Saleem M, Chan H, Derrick JP, Feavers I, Pollard AJ, Moxon ER (2014) Neisseria meningitidis native outer membrane vesicles containing different lipopolysaccharide glycoforms as adjuvants for meningococcal and nonmeningococcal antigens. Clin Vaccine Immunol 21:234–242. https://doi.org/10.1128/CVI.00561-13
Nakamura T, Iwabuchi Y, Hirayama S, Narisawa N, Takenaga F, Nakao R, Senpuku H (2020) Roles of membrane vesicles from Streptococcus mutans for the induction of antibodies to glucosyltransferase in mucosal immunity. Microb Pathog 149:104260. https://doi.org/10.1016/j.micpath.2020.104260
Nakao R, Kobayashi H, Iwabuchi Y, Kawahara K, Hirayama S, Ramstedt M, Sasaki Y, Kataoka M, Akeda Y, Ohnishi M (2022) A highly immunogenic vaccine platform against encapsulated pathogens using chimeric probiotic Escherichia coli membrane vesicles. NPJ Vaccines 7:153. https://doi.org/10.1038/s41541-022-00572-z
Necchi F, Stefanetti G, Alfini R, Palmieri E, Carducci M, Di Benedetto R, Schiavo F, Aruta MG, Giusti F, Ferlenghi I, Goh YS, Rondini S, Micoli F (2021) Neisseria meningitidis factor H binding protein surface exposure on Salmonella Typhimurium GMMA is critical to induce an effective immune response against both diseases. Pathogens 10:726. https://doi.org/10.3390/pathogens10060726
Necchi F, Giannelli C, Acquaviva A, Alfini R, Monaci V, Arato V, Rossi O, Micoli F (2023) From an in vivo to an in vitro relative potency (IVRP) assay to fully characterize a multicomponent O-antigen based vaccine against Shigella. Carbohydr Polym 314:120920. https://doi.org/10.1016/j.carbpol.2023.120920
Nieves W, Petersen H, Judy BM, Blumentritt CA, Russell-Lodrigue K, Roy CJ, Torres AG, Morici LA (2014) A Burkholderia pseudomallei outer membrane vesicle vaccine provides protection against lethal sepsis. Clin Vaccine Immunol 21:747–754. https://doi.org/10.1128/CVI.00119-14
Norheim G, Arne Hoiby E, Caugant DA, Namork E, Tangen T, Fritzsonn E, Rosenqvist E (2004) Immunogenicity and bactericidal activity in mice of an outer membrane protein vesicle vaccine against Neisseria meningitidis serogroup A disease. Vaccine 22:2171–2180. https://doi.org/10.1016/j.vaccine.2003.11.047
Norheim G, Aase A, Caugant DA, Hoiby EA, Fritzsonn E, Tangen T, Kristiansen P, Heggelund U, Rosenqvist E (2005) Development and characterisation of outer membrane vesicle vaccines against serogroup A Neisseria meningitidis. Vaccine 23:3762–3774. https://doi.org/10.1016/j.vaccine.2005.02.021
Norheim G, Tunheim G, Naess LM, Kristiansen PA, Caugant DA, Rosenqvist E (2012) An outer membrane vesicle vaccine for prevention of serogroup A and W-135 meningococcal disease in the African meningitis belt. Scand J Immunol 76:99–107. https://doi.org/10.1111/j.1365-3083.2012.02709.x
Noroozi N, Gargari SLM, Nazarian S, Sarvary S, Adriani RR (2018) Immunogenicity of enterotoxigenic Escherichia coli outer membrane vesicles encapsulated in chitosan nanoparticles. Iran J Basic Med Sci 21:284–291. https://doi.org/10.22038/ijbms.2018.25886.6371
Obiero CW, Ndiaye AGW, Scire AS, Kaunyangi BM, Marchetti E, Gone AM, Schutte LD, Riccucci D, Auerbach J, Saul A, Martin LB, Bejon P, Njuguna P, Podda A (2017) A phase 2a randomized study to evaluate the safety and immunogenicity of the 1790GAHB Generalized Modules for Membrane Antigen vaccine against Shigella sonnei administered intramuscularly to adults from a shigellosis-endemic country. Front Immunol 8:1884. https://doi.org/10.3389/fimmu.2017.01884
O’Dwyer CA, Reddin K, Martin D, Taylor SC, Gorringe AR, Hudson MJ, Brodeur BR, Langford PR, Kroll JS (2004) Expression of heterologous antigens in commensal Neisseria spp.: preservation of conformational epitopes with vaccine potential. Infect Immun 72:6511–6518. https://doi.org/10.1128/IAI.72.11.6511-6518.2004
Ojima Y, Sawabe T, Konami K, Azuma M (2020) Construction of hypervesiculation Escherichia coli strains and application for secretory protein production. Biotechnol Bioeng 117:701–709. https://doi.org/10.1002/bit.27239
Pajon R, Fergus AM, Granoff DM (2013) Mutant native outer membrane vesicles combined with a serogroup A polysaccharide conjugate vaccine for prevention of meningococcal epidemics in Africa. PLoS One 8:e66536. https://doi.org/10.1371/journal.pone.0066536
Palmieri E, Kis Z, Ozanne J, Di Benedetto R, Ricchetti B, Massai L, Carducci M, Oldrini D, Gasperini G, Aruta MG, Rossi O, Kontoravdi C, Shah N, Mawas F, Micoli F (2022) GMMA as an alternative carrier for a glycoconjugate vaccine against group A Streptococcus. Vaccines (Basel) 10:1034. https://doi.org/10.3390/vaccines10071034
Peak IR, Srikhanta YN, Weynants VE, Feron C, Poolman JT, Jennings MP (2013) Evaluation of truncated NhhA protein as a candidate meningococcal vaccine antigen. PLoS One 8:e72003. https://doi.org/10.1371/journal.pone.0072003
Peeters CC, Claassen IJ, Schuller M, Kersten GF, van der Voort EM, Poolman JT (1999) Immunogenicity of various presentation forms of PorA outer membrane protein of Neisseria meningitidis in mice. Vaccine 17:2702–2712. https://doi.org/10.1016/s0264-410x(99)00011-0
Perez JL, Acevedo R, Callico A, Fernandez Y, Cedre B, Ano G, Gonzalez L, Falero G, Talavera A, Perez O, Garcia L (2009) A proteoliposome based formulation administered by the nasal route produces vibriocidal antibodies against El Tor Ogawa Vibrio cholerae O1 in BALB/c mice. Vaccine 27:205–212. https://doi.org/10.1016/j.vaccine.2008.10.052
Perrett KP, McVernon J, Richmond PC, Marshall H, Nissen M, August A, Percell S, Toneatto D, Nolan T (2015) Immune responses to a recombinant, four-component, meningococcal serogroup B vaccine (4CMenB) in adolescents: a phase III, randomized, multicentre, lot-to-lot consistency study. Vaccine 33:5217–5224. https://doi.org/10.1016/j.vaccine.2015.06.103
Petersen H, Nieves W, Russell-Lodrigue K, Roy CJ, Morici LA (2014) Evaluation of a Burkholderia pseudomallei outer membrane vesicle vaccine in nonhuman primates. Procedia Vaccinol 8:38–42. https://doi.org/10.1016/j.provac.2014.07.007
Pettersson A, Kortekaas J, Weynants VE, Voet P, Poolman JT, Bos MP, Tommassen J (2006) Vaccine potential of the Neisseria meningitidis lactoferrin-binding proteins LbpA and LbpB. Vaccine 24:3545–3557. https://doi.org/10.1016/j.vaccine.2006.02.003
Piccioli D, Alfini R, Monaci V, Arato V, Carducci M, Aruta MG, Rossi O, Necchi F, Anemona A, Bartolini E, Micoli F (2022a) Antigen presentation by follicular dendritic cells to cognate B cells is pivotal for Generalised Modules for Membrane Antigens (GMMA) immunogenicity. Vaccine 40:6305–6314. https://doi.org/10.1016/j.vaccine.2022.09.034
Piccioli D, Bartolini E, Micoli F (2022b) GMMA as a ‘plug and play’ technology to tackle infectious disease to improve global health: context and perspectives for the future. Expert Rev Vaccines 21:163–172. https://doi.org/10.1080/14760584.2022.2009803
Piccioli D, Buricchi F, Bacconi M, Bechi N, Galli B, Ferlicca F, Luzzi E, Cartocci E, Marchi S, Romagnoli G, Alfini R, Di Benedetto R, Gallorini S, Savino S, Brunelli B, Bartolini E, Micoli F (2023) Enhanced systemic humoral immune response induced in mice by Generalized Modules for Membrane Antigens (GMMA) is associated with affinity maturation and isotype switching. Vaccines (Basel) 11:1219. https://doi.org/10.3390/vaccines11071219
Prados-Rosales R, Carreno LJ, Batista-Gonzalez A, Baena A, Venkataswamy MM, Xu J, Yu X, Wallstrom G, Magee DM, LaBaer J, Achkar JM, Jacobs WR Jr, Chan J, Porcelli SA, Casadevall A (2014) Mycobacterial membrane vesicles administered systemically in mice induce a protective immune response to surface compartments of Mycobacterium tuberculosis. mBio 5:e01921-14. https://doi.org/10.1128/mBio.01921-14
Price NL, Goyette-Desjardins G, Nothaft H, Valguarnera E, Szymanski CM, Segura M, Feldman MF (2016) Glycoengineered outer membrane vesicles: a novel platform for bacterial vaccines. Sci Rep 6:24931. https://doi.org/10.1038/srep24931
Prior JT, Davitt C, Kurtz J, Gellings P, McLachlan JB, Morici LA (2021) Bacterial-derived outer membrane vesicles are potent adjuvants that drive humoral and cellular immune responses. Pharmaceutics 13:131. https://doi.org/10.3390/pharmaceutics13020131
Quakyi EK, Frasch CE, Buller N, Tsai CM (1999) Immunization with meningococcal outer-membrane protein vesicles containing lipooligosaccharide protects mice against lethal experimental group B Neisseria meningitidis infection and septic shock. J Infect Dis 180:747–754. https://doi.org/10.1086/314927
Raeven RH, van der Maas L, Tilstra W, Uittenbogaard JP, Bindels TH, Kuipers B, van der Ark A, Pennings JL, van Riet E, Jiskoot W, Kersten GF, Metz B (2015) Immunoproteomic profiling of Bordetella pertussis outer membrane vesicle vaccine reveals broad and balanced humoral immunogenicity. J Proteome Res 14:2929–2942. https://doi.org/10.1021/acs.jproteome.5b00258
Raeven RH, Brummelman J, Pennings JL, van der Maas L, Tilstra W, Helm K, van Riet E, Jiskoot W, van Els CA, Han WG, Kersten GF, Metz B (2016) Bordetella pertussis outer membrane vesicle vaccine confers equal efficacy in mice with milder inflammatory responses compared to a whole-cell vaccine. Sci Rep 6:38240. https://doi.org/10.1038/srep38240
Raeven RH, Brummelman J, Pennings JLA, van der Maas L, Helm K, Tilstra W, van der Ark A, Sloots A, van der Ley P, van Eden W, Jiskoot W, van Riet E, van Els CA, Kersten GF, Han WG, Metz B (2018) Molecular and cellular signatures underlying superior immunity against Bordetella pertussis upon pulmonary vaccination. Mucosal Immunol 11:979–993. https://doi.org/10.1038/mi.2017.81
Raeven RHM, Rockx-Brouwer D, Kanojia G, van der Maas L, Bindels THE, Ten Have R, van Riet E, Metz B, Kersten GFA (2020) Intranasal immunization with outer membrane vesicle pertussis vaccine confers broad protection through mucosal IgA and Th17 responses. Sci Rep 10:7396. https://doi.org/10.1038/s41598-020-63998-2
Rappazzo CG, Watkins HC, Guarino CM, Chau A, Lopez JL, DeLisa MP, Leifer CA, Whittaker GR, Putnam D (2016) Recombinant M2e outer membrane vesicle vaccines protect against lethal influenza A challenge in BALB/c mice. Vaccine 34:1252–1258. https://doi.org/10.1016/j.vaccine.2016.01.028
Raso MM, Gasperini G, Alfini R, Schiavo F, Aruta MG, Carducci M, Forgione MC, Martini S, Cescutti P, Necchi F, Micoli F (2020) GMMA and glycoconjugate approaches compared in mice for the development of a vaccine against Shigella flexneri serotype 6. Vaccines (Basel) 8:160. https://doi.org/10.3390/vaccines8020160
Reyes F, Tirado Y, Puig A, Borrero R, Reyes G, Fernandez S, Perez JL, Kadir R, Zayas C, Norazmi MN, Sarmiento ME, Acosta A (2013) Immunogenicity and cross-reactivity against Mycobacterium tuberculosis of proteoliposomes derived from Mycobacterium bovis BCG. BMC Immunol 14(Suppl 1):S7. https://doi.org/10.1186/1471-2172-14-S1-S7
Richardson NI, Ravenscroft N, Arato V, Oldrini D, Micoli F, Kuttel MM (2021) Conformational and immunogenicity studies of the Shigella flexneri serogroup 6 O-antigen: the effect of O-acetylation. Vaccines (Basel) 9:432. https://doi.org/10.3390/vaccines9050432
Rivera J, Cordero RJ, Nakouzi AS, Frases S, Nicola A, Casadevall A (2010) Bacillus anthracis produces membrane-derived vesicles containing biologically active toxins. Proc Natl Acad Sci USA 107:19002–19007. https://doi.org/10.1073/pnas.1008843107
Robertson SM, Frisch CF, Gulig PA, Kettman JR, Johnston KH, Hansen EJ (1982) Monoclonal antibodies directed against a cell surface-exposed outer membrane protein of Haemophilus influenzae type b. Infect Immun 36:80–88. https://doi.org/10.1128/iai.36.1.80-88.1982
Roier S, Leitner DR, Iwashkiw J, Schild-Prufert K, Feldman MF, Krohne G, Reidl J, Schild S (2012) Intranasal immunization with nontypeable Haemophilus influenzae outer membrane vesicles induces cross-protective immunity in mice. PLoS One 7:e42664. https://doi.org/10.1371/journal.pone.0042664
Roier S, Fenninger JC, Leitner DR, Rechberger GN, Reidl J, Schild S (2013) Immunogenicity of Pasteurella multocida and Mannheimia haemolytica outer membrane vesicles. Int J Med Microbiol 303:247–256. https://doi.org/10.1016/j.ijmm.2013.05.001
Roier S, Blume T, Klug L, Wagner GE, Elhenawy W, Zangger K, Prassl R, Reidl J, Daum G, Feldman MF, Schild S (2015) A basis for vaccine development: comparative characterization of Haemophilus influenzae outer membrane vesicles. Int J Med Microbiol 305:298–309. https://doi.org/10.1016/j.ijmm.2014.12.005
Rojas-Lopez M, Martinelli M, Brandi V, Jubelin G, Polticelli F, Soriani M, Pizza M, Desvaux M, Rosini R (2019) Identification of lipid A deacylase as a novel, highly conserved and protective antigen against enterohemorrhagic Escherichia coli. Sci Rep 9:17014. https://doi.org/10.1038/s41598-019-53197-z
Romeu B, Lastre M, Garcia L, Cedre B, Mandariote A, Farinas M, Oliva R, Rosenqvist E, Perez O (2014) Combined meningococcal serogroup A and W135 outer-membrane vesicles activate cell-mediated immunity and long-term memory responses against non-covalent capsular polysaccharide A. Immunol Res 58:75–85. https://doi.org/10.1007/s12026-013-8427-6
Rosenqvist E, Musacchio A, Aase A, Hoiby EA, Namork E, Kolberg J, Wedege E, Delvig A, Dalseg R, Michaelsen TE, Tommassen J (1999) Functional activities and epitope specificity of human and murine antibodies against the class 4 outer membrane protein (Rmp) of Neisseria meningitidis. Infect Immun 67:1267–1276. https://doi.org/10.1128/IAI.67.3.1267-1276.1999
Rosenthal JA, Huang CJ, Doody AM, Leung T, Mineta K, Feng DD, Wayne EC, Nishimura N, Leifer C, DeLisa MP, Mendez S, Putnam D (2014) Mechanistic insight into the TH1-biased immune response to recombinant subunit vaccines delivered by probiotic bacteria-derived outer membrane vesicles. PLoS One 9(11):e112802. https://doi.org/10.1371/journal.pone.0112802
Rossi O, Citiulo F, Mancini F (2021) Outer membrane vesicles: moving within the intricate labyrinth of assays that can predict risks of reactogenicity in humans. Hum Vaccin Immunother 17:601–613. https://doi.org/10.1080/21645515.2020.1780092
Roy K, Hamilton DJ, Munson GP, Fleckenstein JM (2011) Outer membrane vesicles induce immune responses to virulence proteins and protect against colonization by enterotoxigenic Escherichia coli. Clin Vaccine Immunol 18:1803–1808. https://doi.org/10.1128/CVI.05217-11
Salverda ML, Meinderts SM, Hamstra HJ, Wagemakers A, Hovius JW, van der Ark A, Stork M, van der Ley P (2016) Surface display of a borrelial lipoprotein on meningococcal outer membrane vesicles. Vaccine 34:1025–1033. https://doi.org/10.1016/j.vaccine.2016.01.019
Sanders H, Norheim G, Chan H, Dold C, Vipond C, Derrick JP, Pollard AJ, Maiden MCJ, Feavers IM (2015) FetA antibodies induced by an outer membrane vesicle vaccine derived from a serogroup B meningococcal isolate with constitutive FetA expression. PLoS One 10:e0140345. https://doi.org/10.1371/journal.pone.0140345
Sartorio MG, Pardue EJ, Feldman MF, Haurat MF (2021) Bacterial outer membrane vesicles: from discovery to applications. Annu Rev Microbiol 75:609–630. https://doi.org/10.1146/annurev-micro-052821-031444
Schager AE, Dominguez-Medina CC, Necchi F, Micoli F, Goh YS, Goodall M, Flores-Langarica A, Bobat S, Cook CNL, Arcuri M, Marini A, King LWD, Morris FC, Anderson G, Toellner KM, Henderson IR, Lopez-Macias C, MacLennan CA, Cunningham AF (2018) IgG responses to porins and lipopolysaccharide within an outer membrane-based vaccine against nontyphoidal Salmonella develop at discordant rates. mBio 9:e02379-17. https://doi.org/10.1128/mBio.02379-17
Schild S, Nelson EJ, Bishop AL, Camilli A (2009) Characterization of Vibrio cholerae outer membrane vesicles as a candidate vaccine for cholera. Infect Immun 77:472–484. https://doi.org/10.1128/IAI.01139-08
Schlegel S, Hjelm A, Baumgarten T, Vikstrom D, de Gier JW (2014) Bacterial-based membrane protein production. Biochim Biophys Acta 1843:1739–1749. https://doi.org/10.1016/j.bbamcr.2013.10.023
Schwechheimer C, Kuehn MJ (2015) Outer-membrane vesicles from gram-negative bacteria: biogenesis and functions. Nat Rev Microbiol 13:605–619. https://doi.org/10.1038/nrmicro3525
Schwechheimer C, Kulp A, Kuehn MJ (2014) Modulation of bacterial outer membrane vesicle production by envelope structure and content. BMC Microbiol 14:324. https://doi.org/10.1186/s12866-014-0324-1
Schwechheimer C, Rodriguez DL, Kuehn MJ (2015) NlpI-mediated modulation of outer membrane vesicle production through peptidoglycan dynamics in Escherichia coli. Microbiologyopen 4:375–389. https://doi.org/10.1002/mbo3.244
Shibata Y, Kurihara K, Takiguchi H, Abiko Y (1998) Construction of a functional single-chain variable fragment antibody against hemagglutinin from Porphyromonas gingivalis. Infect Immun 66:2207–2212. https://doi.org/10.1128/IAI.66.5.2207-2212.1998
Shoemaker DR, Saunders NB, Brandt BL, Moran EE, Laclair AD, Zollinger WD (2005) Intranasal delivery of group B meningococcal native outer membrane vesicle vaccine induces local mucosal and serum bactericidal antibody responses in rabbits. Infect Immun 73:5031–5038. https://doi.org/10.1128/IAI.73.8.5031-5038.2005
Sokaribo AS, Perera SR, Sereggela Z, Krochak R, Balezantis LR, Xing X, Lam S, Deck W, Attah-Poku S, Abbott DW, Tamuly S, White AP (2021) A GMMA-CPS-based vaccine for non-typhoidal Salmonella. Vaccines (Basel) 9:165. https://doi.org/10.3390/vaccines9020165
Stentz R, Carvalho AL, Jones EJ, Carding SR (2018) Fantastic voyage: the journey of intestinal microbiota-derived microvesicles through the body. Biochem Soc Trans 46:1021–1027. https://doi.org/10.1042/BST20180114
Stevenson TC, Cywes-Bentley C, Moeller TD, Weyant KB, Putnam D, Chang YF, Jones BD, Pier GB, DeLisa MP (2018) Immunization with outer membrane vesicles displaying conserved surface polysaccharide antigen elicits broadly antimicrobial antibodies. Proc Natl Acad Sci USA 115:E3106-3115. https://doi.org/10.1073/pnas.1718341115
Sun J, Lin X, He Y, Zhang B, Zhou N, Huang JD (2023) A bacterial outer membrane vesicle-based click vaccine elicits potent immune response against Staphylococcus aureus in mice. Front Immunol 14:1088501. https://doi.org/10.3389/fimmu.2023.1088501
Troncoso G, Sanchez S, Kolberg J, Rosenqvist E, Veiga M, Ferreiros CM, Criado M (2001) Analysis of the expression of the putatively virulence-associated neisserial protein RmpM (class 4) in commensal Neisseria and Moraxella catarrhalis strains. FEMS Microbiol Lett 199:171–176. https://doi.org/10.1111/j.1574-6968.2001.tb10669.x
Trzewikoswki de Lima G, Rodrigues TS, Portilho AI, Correa VA, Gaspar EB, De Gaspari E (2020) Immune responses of meningococcal B outer membrane vesicles in middle-aged mice. Pathog Dis 78:ftaa028. https://doi.org/10.1093/femspd/ftaa028
van de Waterbeemd B, Streefland M, van der Ley P, Zomer B, van Dijken H, Martens D, Wijffels R, van der Pol L (2010) Improved OMV vaccine against Neisseria meningitidis using genetically engineered strains and a detergent-free purification process. Vaccine 28:4810–4816. https://doi.org/10.1016/j.vaccine.2010.04.082
van de Waterbeemd B, Mommen GP, Pennings JL, Eppink MH, Wijffels RH, van der Pol LA, de Jong AP (2013) Quantitative proteomics reveals distinct differences in the protein content of outer membrane vesicle vaccines. J Proteome Res 12:1898–1908. https://doi.org/10.1021/pr301208g
van der Pol L, Stork M, van der Ley P (2015) Outer membrane vesicles as platform vaccine technology. Biotechnol J 10:1689–1706. https://doi.org/10.1002/biot.201400395
Viviani V, Fantoni A, Tomei S, Marchi S, Luzzi E, Bodini M, Muzzi A, Giuliani MM, Maione D, Derrick JP, Delany I, Pizza M, Biolchi A, Bartolini E (2023) OpcA and PorB are novel bactericidal antigens of the 4CMenB vaccine in mice and humans. NPJ Vaccines 8:54. https://doi.org/10.1038/s41541-023-00651-9
Wai SN, Lindmark B, Soderblom T, Takade A, Westermark M, Oscarsson J, Jass J, Richter-Dahlfors A, Mizunoe Y, Uhlin BE (2003) Vesicle-mediated export and assembly of pore-forming oligomers of the enterobacterial ClyA cytotoxin. Cell 115:25–35. https://doi.org/10.1016/s0092-8674(03)00754-2
Wang X, Thompson CD, Weidenmaier C, Lee JC (2018) Release of Staphylococcus aureus extracellular vesicles and their application as a vaccine platform. Nat Commun 9:1379. https://doi.org/10.1038/s41467-018-03847-z
Wang H, Liang K, Kong Q, Liu Q (2019a) Immunization with outer membrane vesicles of avian pathogenic Escherichia coli O78 induces protective immunity in chickens. Vet Microbiol 236:108367. https://doi.org/10.1016/j.vetmic.2019.07.019
Wang S, Gao J, Wang Z (2019b) Outer membrane vesicles for vaccination and targeted drug delivery. Wiley Interdiscip Rev Nanomed Nanobiotechnol 11:e1523. https://doi.org/10.1002/wnan.1523
Wang W, Chanda W, Zhong M (2015) The relationship between biofilm and outer membrane vesicles: a novel therapy overview. FEMS Microbiol Lett 362:fnv117. https://doi.org/10.1093/femsle/fnv117
Wedege E, Froholm LO (1986) Human antibody response to a group B serotype 2a meningococcal vaccine determined by immunoblotting. Infect Immun 51:571–578. https://doi.org/10.1128/iai.51.2.571-578.1986
Wedege E, Kuipers B, Bolstad K, van Dijken H, Froholm LO, Vermont C, Caugant DA, van den Dobbelsteen G (2003) Antibody specificities and effect of meningococcal carriage in Icelandic teenagers receiving the Norwegian serogroup B outer membrane vesicle vaccine. Infect Immun 71:3775–3781. https://doi.org/10.1128/IAI.71.7.3775-3781.2003
Wedege E, Bolstad K, Aase A, Herstad TK, McCallum L, Rosenqvist E, Oster P, Martin D (2007) Functional and specific antibody responses in adult volunteers in New Zealand who were given one of two different meningococcal serogroup B outer membrane vesicle vaccines. Clin Vaccine Immunol 14:830–838. https://doi.org/10.1128/CVI.00039-07
Weyant KB, Oloyede A, Pal S, Liao J, Jesus MR, Jaroentomeechai T, Moeller TD, Hoang-Phou S, Gilmore SF, Singh R, Pan DC, Putnam D, Locher C, de la Maza LM, Coleman MA, DeLisa MP (2023) A modular vaccine platform enabled by decoration of bacterial outer membrane vesicles with biotinylated antigens. Nat Commun 14:464. https://doi.org/10.1038/s41467-023-36101-2
Weynants V, Denoel P, Devos N, Janssens D, Feron C, Goraj K, Momin P, Monnom D, Tans C, Vandercammen A, Wauters F, Poolman JT (2009) Genetically modified L3,7 and L2 lipooligosaccharides from Neisseria meningitidis serogroup B confer a broad cross-bactericidal response. Infect Immun 77:2084–2093. https://doi.org/10.1128/IAI.01108-08
Williams JN, Weynants V, Poolman JT, Heckels JE, Christodoulides M (2014) Immuno-proteomic analysis of human immune responses to experimental Neisseria meningitidis outer membrane vesicle vaccines identifies potential cross-reactive antigens. Vaccine 32:1280–1286. https://doi.org/10.1016/j.vaccine.2013.12.070
Zhang L, Wen Z, Lin J, Xu H, Herbert P, Wang XM, Mehl JT, Ahl PL, Dieter L, Russell R, Kosinski MJ, Przysiecki CT (2016) Improving the immunogenicity of a trivalent Neisseria meningitidis native outer membrane vesicle vaccine by genetic modification. Vaccine 34:4250–4256. https://doi.org/10.1016/j.vaccine.2016.05.049
Zhang X, Yang F, Zou J, Wu W, Jing H, Gou Q, Li H, Gu J, Zou Q, Zhang J (2018) Immunization with Pseudomonas aeruginosa outer membrane vesicles stimulates protective immunity in mice. Vaccine 36:1047–1054. https://doi.org/10.1016/j.vaccine.2018.01.034
Funding
Open Access funding provided by National Research Council Canada. This work was supported by the Ideation Fund Small Teams Initiative (National Research Council Canada).
Author information
Authors and Affiliations
Contributions
EKL, AA, KAH, and GH conceived the review article and wrote the manuscript. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Ethics approval
Studies involving research on animals and human participants are reviewed in this manuscript.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lei, E.K., Azmat, A., Henry, K.A. et al. Outer membrane vesicles as a platform for the discovery of antibodies to bacterial pathogens. Appl Microbiol Biotechnol 108, 232 (2024). https://doi.org/10.1007/s00253-024-13033-5
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00253-024-13033-5