Abstract
The desynchronization of circadian rhythms affected by light may induce physiological and psychological disequilibrium. We aimed to elucidate changes of growth, depression-anxiety like behaviors, melatonin and corticosterone (CORT) secretion, and gut microbiota in rats influenced by long-term light inputs. Thirty male Sprague–Dawley rats were exposed to a 16/8 h light/dark regime for 8 weeks. The light period was set to 13 h of daylight with artificial light (AL group, n = 10), or with natural light (NL group, n = 10), or with mixed artificial-natural light (ANL group, n = 10), and 3 h of artificial night light after sunset. The obtained findings indicated that the highest weight gain and food efficiency were observed in the AL group and the lowest in NL group. In the behavioral tests, the NL and ANL groups showed lower anxiety level than AL group, and ANL groups showed lower depression level than AL group. The NL and ANL groups had delayed acrophases and maintained higher concentrations of melatonin compared to AL group. The circadian rhythm of CORT was only found in ANL group. At the phylum level, the mixed light contributed to a lower abundance of Bacteroidetes. The genus level results recommend a synergistic effect of artificial light and natural light on Lactobacillus abundance and an antagonistic effect on the Lachnospiraceae_NK4A136_group abundance. The study indicated that the mixture of artificial and natural light as well as the alignment of the proportions had beneficial influences on depression-anxiety-like levels, melatonin and corticosterone secretion, and the composition of the gut microbiota.
Key points
• The mixed light can reduce the depression-anxiety level
• The mixed light can maintain the secretion rhythm of melatonin and CORT
• The mixed light can increase Lactobacillus and decrease Lachnospiraceae_NK4A136_group
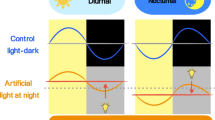
Graphical Abstract








Similar content being viewed by others
Data availability
The data that support the findings of this study are in this published article and available from the corresponding author upon reasonable request.
Code availability
The code applied in the data analysis is available from the corresponding author upon reasonable request.
References
Abell JG, Shipley MJ, Ferrie JE, Kivimäki M, Kumari M (2016) Recurrent short sleep, chronic insomnia symptoms and salivary cortisol: a 10-year follow-up in the Whitehall II study. Psychoneuroendocrinology 68:91–99. https://doi.org/10.1016/j.psyneuen.2016.02.021
Adams JB, Johansen LJ, Powell LD, Quig D, Rubin RA (2011) Gastrointestinal flora and gastrointestinal status in children with autism—comparisons to typical children and correlation with autism severity. BMC Gastroenterol 11:22. https://doi.org/10.1186/1471-230x-11-22
Akpinar Z, Tokgöz S, Gökbel H, Okudan N, Uğuz F, Yilmaz G (2008) The association of nocturnal serum melatonin levels with major depression in patients with acute multiple sclerosis. Psychiatry Res 161(2):253–257. https://doi.org/10.1016/j.psychres.2007.11.022
Arumugam M, Raes J, Pelletier E, Le Paslier D, Yamada T, Mende DR, Fernandes GR, Tap J, Bruls T, Batto J-M, Bertalan M, Borruel N, Casellas F, Fernandez L, Gautier L, Hansen T, Hattori M, Hayashi T, Kleerebezem M, Kurokawa K, Leclerc M, Levenez F, Manichanh C, Nielsen HB, Nielsen T, Pons N, Poulain J, Qin J, Sicheritz-Ponten T, Tims S, Torrents D, Ugarte E, Zoetendal EG, Wang J, Guarner F, Pedersen O, de Vos WM, Brunak S, Doré J, Antolín M, Artiguenave F, Blottiere HM, Almeida M, Brechot C, Cara C, Chervaux C, Cultrone A, Delorme C, Denariaz G, Dervyn R, Foerstner KU, Friss C, van de Guchte M, Guedon E, Haimet F, Huber W, van Hylckama-Vlieg J, Jamet A, Juste C, Kaci G, Knol J, Kristiansen K, Lakhdari O, Layec S, Le Roux K, Maguin E, Mérieux A, Melo Minardi R, M’Rini C, Muller J, Oozeer R, Parkhill J, Renault P, Rescigno M, Sanchez N, Sunagawa S, Torrejon A, Turner K, Vandemeulebrouck G, Varela E, Winogradsky Y, Zeller G, Weissenbach J, Ehrlich SD, Bork P, Meta HITC (2011) Enterotypes of the human gut microbiome. Nature 473(7346):174–180. https://doi.org/10.1038/nature09944
Bechtold DA, Gibbs JE, Loudon AS (2010) Circadian dysfunction in disease. Trends Pharmacol Sci 31(5):191–198. https://doi.org/10.1016/j.tips.2010.01.002
Begemann SHA, van den Beld GJ, Tenner AD (1997) Daylight, artificial light and people in an office environment, overview of visual and biological responses. Int J Ind Ergonomics 20(3):231–239. https://doi.org/10.1016/S0169-8141(96)00053-4
Berson DM (2003) Strange vision: ganglion cells as circadian photoreceptors. Trends Neurosci 26(6):314–320. https://doi.org/10.1016/s0166-2236(03)00130-9
Biddle A, Stewart L, Blanchard J, Leschine S (2013) Untangling the genetic basis of fibrolytic specialization by Lachnospiraceae and Ruminococcaceae in diverse gut communities. Diversity 5:627–640. https://doi.org/10.3390/d5030627
Bingham C, Arbogast B, Guillaume GC, Lee JK, Halberg F (1982) Inferential statistical methods for estimating and comparing cosinor parameters. Chronobiologia 9(4):397–439
Blask DE, Brainard GC, Dauchy RT, Hanifin JP, Davidson LK, Krause JA, Sauer LA, Rivera-Bermudez MA, Dubocovich ML, Jasser SA, Lynch DT, Rollag MD, Zalatan F (2005) Melatonin-depleted blood from premenopausal women exposed to light at night stimulates growth of human breast cancer xenografts in nude rats. Cancer Res 65(23):11174–11184. https://doi.org/10.1158/0008-5472.Can-05-1945
Blume C, Garbazza C, Spitschan M (2019) Effects of light on human circadian rhythms, sleep and mood. Somnologie (berl) 23(3):147–156. https://doi.org/10.1007/s11818-019-00215-x
Bohák Z, Szabó F, Beckers JF, Melo de Sousa N, Kutasi O, Nagy K, Szenci O (2013) Monitoring the circadian rhythm of serum and salivary cortisol concentrations in the horse. Domest Anim Endocrinol 45(1):38–42. https://doi.org/10.1016/j.domaniend.2013.04.001
Brahe LK, Astrup A, Larsen LH (2013) Is butyrate the link between diet, intestinal microbiota and obesity-related metabolic diseases? Obes Rev 14(12):950–959. https://doi.org/10.1111/obr.12068
Brainard GC, Hanifin JP, Greeson JM, Byrne B, Glickman G, Gerner E, Rollag MD (2001) Action spectrum for melatonin regulation in humans: evidence for a novel circadian photoreceptor. J Neurosci 21(16):6405–6412. https://doi.org/10.1523/jneurosci.21-16-06405.2001
Bravo JA, Forsythe P, Chew MV, Escaravage E, Savignac HM, Dinan TG, Bienenstock J, Cryan JF (2011) Ingestion of Lactobacillus strain regulates emotional behavior and central GABA receptor expression in a mouse via the vagus nerve. Proc Natl Acad Sci U S A 108(38):16050–16055. https://doi.org/10.1073/pnas.1102999108
Brennan R, Jan JE, Lyons CJ (2007) Light, dark, and melatonin: emerging evidence for the importance of melatonin in ocular physiology. Eye 21(7):901–908. https://doi.org/10.1038/sj.eye.6702597
Broussard JL, Van Cauter E (2016) Disturbances of sleep and circadian rhythms: novel risk factors for obesity. Curr Opin Endocrinol Diabetes Obes 23(5):353–359. https://doi.org/10.1097/med.0000000000000276
Brown MJ, Jacobs DE (2011) Residential light and risk for depression and falls: results from the LARES study of eight European cities. Public Health Rep 126 Suppl 1(Suppl 1):131–140 https://doi.org/10.1177/00333549111260s117
Brown R, Price RJ, King MG, Husband AJ (1990) Are antibiotic effects on sleep behavior in the rat due to modulation of gut bacteria? Physiol Behav 48(4):561–565. https://doi.org/10.1016/0031-9384(90)90300-s
Buijs FN, León-Mercado L, Guzmán-Ruiz M, Guerrero-Vargas NN, Romo-Nava F, Buijs RM (2016) The circadian system: a regulatory feedback network of periphery and brain. Physiology (Bethesda) 31(3):170–181. https://doi.org/10.1152/physiol.00037.2015
Cajochen C, Münch M, Kobialka S, Kräuchi K, Steiner R, Oelhafen P, Orgül S, Wirz-Justice A (2005) High sensitivity of human melatonin, alertness, thermoregulation, and heart rate to short wavelength light. J Clin Endocrinol Metab 90(3):1311–1316. https://doi.org/10.1210/jc.2004-0957
Carola V, D’Olimpio F, Brunamonti E, Mangia F, Renzi P (2002) Evaluation of the elevated plus-maze and open-field tests for the assessment of anxiety-related behaviour in inbred mice. Behav Brain Res 134(1–2):49–57. https://doi.org/10.1016/s0166-4328(01)00452-1
Cassano P, Cusin C, Mischoulon D, Hamblin MR, De Taboada L, Pisoni A, Chang T, Yeung A, Ionescu DF, Petrie SR, Nierenberg AA, Fava M, Iosifescu DV (2015) Near-infrared transcranial radiation for major depressive disorder: proof of concept study. Psychiatry J 2015:352979 https://doi.org/10.1155/2015/352979
Cassone VM, Warren WS, Brooks DS, Lu J (1993) Melatonin, the pineal gland, and circadian rhythms. J Biol Rhythms 8(Suppl):S73–S81
Challet E (2015) Keeping circadian time with hormones. Diabetes Obes Metab 17(Suppl 1):76–83. https://doi.org/10.1111/dom.12516
Chang AM, Aeschbach D, Duffy JF, Czeisler CA (2015) Evening use of light-emitting eReaders negatively affects sleep, circadian timing, and next-morning alertness. Proc Natl Acad Sci U S A 112(4):1232–1237. https://doi.org/10.1073/pnas.1418490112
Chang AM, Santhi N, St Hilaire M, Gronfier C, Bradstreet DS, Duffy JF, Lockley SW, Kronauer RE, Czeisler CA (2012) Human responses to bright light of different durations. J Physiol 590(13):3103–3112. https://doi.org/10.1113/jphysiol.2011.226555
Chu W, Zhai J, Xu J, Li S, Li W, Chen Z-J, Du Y (2020) Continuous light-induced PCOS-like changes in reproduction, metabolism, and gut microbiota in Sprague-Dawley rats. Front Microbiol 10 https://doi.org/10.3389/fmicb.2019.03145
Cornelissen G (2014) Cosinor-based rhythmometry. Theor Biol Medical Model 11(1):16https://doi.org/10.1186/1742-4682-11-16
de Kloet ER, Joëls M, Holsboer F (2005) Stress and the brain: from adaptation to disease. Nat Rev Neurosci 6(6):463–475. https://doi.org/10.1038/nrn1683
Dibner C, Schibler U, Albrecht U (2010) The mammalian circadian timing system: organization and coordination of central and peripheral clocks. Annu Rev Physiol 72:517–549. https://doi.org/10.1146/annurev-physiol-021909-135821
Dilsaver SC, Coffman JA (1988) Seasonal depression. Am Fam Physician 38(4):173–176
Duffy JF, Czeisler CA (2009) Effect of light on human circadian physiology. Sleep Med Clin 4(2):165–177. https://doi.org/10.1016/j.jsmc.2009.01.004
Fisk AS, Tam SKE, Brown LA, Vyazovskiy VV, Bannerman DM, Peirson SN (2018) Light and cognition: roles for circadian rhythms, sleep, and arousal. Front Neurol 9 https://doi.org/10.3389/fneur.2018.00056
Fonken LK, Nelson RJ (2014) The effects of light at night on circadian clocks and metabolism. Endocr Rev 35(4):648–670. https://doi.org/10.1210/er.2013-1051
Gaston KJ, Bennie J, Davies TW, Hopkins J (2013) The ecological impacts of nighttime light pollution: a mechanistic appraisal. Biol Rev Camb Philos Soc 88(4):912–927. https://doi.org/10.1111/brv.12036
Gordijn MCM, t Mannetje D, Meesters Y (2012) The effects of blue-enriched light treatment compared to standard light treatment in seasonal affective disorder. J Affect Disord 136(1):72-80https://doi.org/10.1016/j.jad.2011.08.016
Gould TD, Einat H, Bhat R, Manji HK (2004) AR-A014418, a selective GSK-3 inhibitor, produces antidepressant-like effects in the forced swim test. Int J Neuropsychopharmacol 7(4):387–390. https://doi.org/10.1017/s1461145704004535
Graham C, Mullen A, Whelan K (2015) Obesity and the gastrointestinal microbiota: a review of associations and mechanisms. Nutr Rev 73(6):376–385. https://doi.org/10.1093/nutrit/nuv004
Grivas TB, Savvidou OD (2007) Melatonin the “light of night” in human biology and adolescent idiopathic scoliosis. Scoliosis 2:6. https://doi.org/10.1186/1748-7161-2-6
Halberg F, Tong YL, Johnson EA (1967) Circadian system phase — an aspect of temporal morphology; procedures and illustrative examples. In: von Mayersbach H (ed) The Cellular Aspects of Biorhythms: Symposium on Rhythmic Research Sponsored by the VIIIth International Congress of Anatomy Wiesbaden 8–14 August 1965. Springer, Berlin Heidelberg, Berlin, Heidelberg, pp 20–48
Handley SL, Mithani S (1984) Effects of alpha-adrenoceptor agonists and antagonists in a maze-exploration model of ‘fear’-motivated behaviour. Naunyn-Schmiedeb Arch Pharmacol 327(1):1–5. https://doi.org/10.1007/BF00504983
Hanifin JP, Lockley SW, Cecil K, West K, Jablonski M, Warfield B, James M, Ayers M, Byrne B, Gerner E, Pineda C, Rollag M, Brainard GC (2019) Randomized trial of polychromatic blue-enriched light for circadian phase shifting, melatonin suppression, and alerting responses. Physiol Behav 198:57–66. https://doi.org/10.1016/j.physbeh.2018.10.004
Hao Z, Wang W, Guo R, Liu H (2019) Faecalibacterium prausnitzii (ATCC 27766) has preventive and therapeutic effects on chronic unpredictable mild stress-induced depression-like and anxiety-like behavior in rats. Psychoneuroendocrinology 104:132–142. https://doi.org/10.1016/j.psyneuen.2019.02.025
Harb F, Hidalgo MP, Martau B (2015) Lack of exposure to natural light in the workspace is associated with physiological, sleep and depressive symptoms. Chronobiol Int 32(3):368–375. https://doi.org/10.3109/07420528.2014.982757
Helbich M, Browning MHEM, Huss A (2020) Outdoor light at night, air pollution and depressive symptoms: a cross-sectional study in the Netherlands. Sci Total Environ 744:140914 https://doi.org/10.1016/j.scitotenv.2020.140914
Hogg S (1996) A review of the validity and variability of the elevated plus-maze as an animal model of anxiety. Pharmacol Biochem Behav 54(1):21–30. https://doi.org/10.1016/0091-3057(95)02126-4
Hou Y, Wang Y, Song S, Zuo Y, Zhang H, Bai C, Zhao H, Zhang T (2022) Long-term variable photoperiod exposure impairs the mPFC and induces anxiety and depression-like behavior in male Wistar rats. Exp Neurol 347:113908 https://doi.org/10.1016/j.expneurol.2021.113908
Hu H, Kang C, Hou X, Zhang Q, Meng Q, Jiang J, Hao W (2020) Blue light deprivation produces depression-like responses in mongolian gerbils. Front Psychiatry 11:233–233. https://doi.org/10.3389/fpsyt.2020.00233
Husain SF, Yu R, Tang T-B, Tam WW, Tran B, Quek TT, Hwang S-H, Chang CW, Ho CS, Ho RC (2020) Validating a functional near-infrared spectroscopy diagnostic paradigm for major depressive disorder. Sci Rep 10(1):9740. https://doi.org/10.1038/s41598-020-66784-2
Hussain MM, Pan X (2015) Circadian regulators of intestinal lipid absorption. J Lipid Res 56(4):761–770. https://doi.org/10.1194/jlr.R051573
Jiang H, Ling Z, Zhang Y, Mao H, Ma Z, Yin Y, Wang W, Tang W, Tan Z, Shi J, Li L, Ruan B (2015) Altered fecal microbiota composition in patients with major depressive disorder. Brain Behav Immun 48:186–194. https://doi.org/10.1016/j.bbi.2015.03.016
Kaczmarek JL, Musaad SM, Holscher HD (2017) Time of day and eating behaviors are associated with the composition and function of the human gastrointestinal microbiota. Am J Clin Nutr 106(5):1220–1231. https://doi.org/10.3945/ajcn.117.156380
Kalsbeek A, van der Spek R, Lei J, Endert E, Buijs RM, Fliers E (2012) Circadian rhythms in the hypothalamo-pituitary-adrenal (HPA) axis. Mol Cell Endocrinol 349(1):20–29. https://doi.org/10.1016/j.mce.2011.06.042
Karatsoreos IN, Bhagat S, Bloss EB, Morrison JH, McEwen BS (2011) Disruption of circadian clocks has ramifications for metabolism, brain, and behavior. Proc Natl Acad Sci U S A 108(4):1657–1662. https://doi.org/10.1073/pnas.1018375108
Lee CC, Liang F, Lee IC, Lu TH, Shan YY, Jeng CF, Zou YF, Yu HT, Chen Alen SK (2022) External light-dark cycle shapes gut microbiota through intrinsically photosensitive retinal ganglion cells. EMBO Rep 23(6):e52316 https://doi.org/10.15252/embr.202052316
Leone V, Gibbons SM, Martinez K, Hutchison AL, Huang EY, Cham CM, Pierre JF, Heneghan AF, Nadimpalli A, Hubert N, Zale E, Wang Y, Huang Y, Theriault B, Dinner AR, Musch MW, Kudsk KA, Prendergast BJ, Gilbert JA, Chang EB (2015) Effects of diurnal variation of gut microbes and high-fat feeding on host circadian clock function and metabolism. Cell Host Microbe 17(5):681–689. https://doi.org/10.1016/j.chom.2015.03.006
Levitan RD (2007) The chronobiology and neurobiology of winter seasonal affective disorder. Dialogues Clin Neurosci 9(3):315–324 https://doi.org/10.31887/DCNS.2007.9.3/rlevitan
Magnusson A, Boivin D (2003) Seasonal affective disorder: an overview. Chronobiol Int 20(2):189–207. https://doi.org/10.1081/CBI-120019310
Marqueze EC, Vasconcelos S, Garefelt J, Skene DJ, Moreno CR, Lowden A (2015) Natural light exposure, sleep and depression among day workers and shiftworkers at arctic and equatorial latitudes. PLoS One 10(4):e0122078 https://doi.org/10.1371/journal.pone.0122078
Mason BL, Li Q, Minhajuddin A, Czysz AH, Coughlin LA, Hussain SK, Koh AY, Trivedi MH (2020) Reduced anti-inflammatory gut microbiota are associated with depression and anhedonia. J Affect Disord 266:394–401. https://doi.org/10.1016/j.jad.2020.01.137
Matenchuk BA, Mandhane PJ, Kozyrskyj AL (2020) Sleep, circadian rhythm, and gut microbiota. Sleep Med Rev 53:101340 https://doi.org/10.1016/j.smrv.2020.101340
McIntyre IM, Norman TR, Burrows GD, Armstrong SM (1989) Human melatonin suppression by light is intensity dependent. J Pineal Res 6(2):149–156. https://doi.org/10.1111/j.1600-079x.1989.tb00412.x
Meng C, Wang W, Hao Z, Liu H (2020) Investigation on the influence of isolated environment on human psychological and physiological health. Sci Total Environ 716:136972 https://doi.org/10.1016/j.scitotenv.2020.136972
Meng Q, Lian Y, Jiang J, Wang W, Hou X, Pan Y, Chu H, Shang L, Wei X, Hao W (2018) Blue light filtered white light induces depression-like responses and temporary spatial learning deficits in rats. Photochem Photobiol Sci 17(4):386–394. https://doi.org/10.1039/c7pp00271h
Molcan L, Sutovska H, Okuliarova M, Senko T, Krskova L, Zeman M (2019) Dim light at night attenuates circadian rhythms in the cardiovascular system and suppresses melatonin in rats. Life Sci 231:116568 https://doi.org/10.1016/j.lfs.2019.116568
Moore RY, Lenn NJ (1972) A retinohypothalamic projection in the rat. J Comp Neurol 146(1):1–14. https://doi.org/10.1002/cne.901460102
Morrissey B, Malakellis M, Whelan J, Millar L, Swinburn B, Allender S, Strugnell C (2016) Sleep duration and risk of obesity among a sample of Victorian school children. BMC Public Health 16:245. https://doi.org/10.1186/s12889-016-2913-4
Naseribafrouei A, Hestad K, Avershina E, Sekelja M, Linløkken A, Wilson R, Rudi K (2014) Correlation between the human fecal microbiota and depression. Neurogastroenterol Motil 26(8):1155–1162. https://doi.org/10.1111/nmo.12378
Navara KJ, Nelson RJ (2007) The dark side of light at night: physiological, epidemiological, and ecological consequences. J Pineal Res 43(3):215–224. https://doi.org/10.1111/j.1600-079X.2007.00473.x
Oron U, Ilic S, De Taboada L, Streeter J (2007) Ga-As (808 nm) laser irradiation enhances ATP production in human neuronal cells in culture. Photomed Laser Surg 25(3):180–182. https://doi.org/10.1089/pho.2007.2064
Otsuka T, Goto M, Kawai M, Togo Y, Sato K, Katoh K, Furuse M, Yasuo S (2012) Photoperiod regulates corticosterone rhythms by altered adrenal sensitivity via melatonin-independent mechanisms in Fischer 344 rats and C57BL/6J mice. PLoS One 7(6):e39090 https://doi.org/10.1371/journal.pone.0039090
Panda S, Sato TK, Castrucci AM, Rollag MD, DeGrip WJ, Hogenesch JB, Provencio I, Kay SA (2002) Melanopsin (Opn4) requirement for normal light-induced circadian phase shifting. Science 298(5601):2213–2216. https://doi.org/10.1126/science.1076848
Persengiev S, Kanchev L, Vezenkova G (1991) Circadian patterns of melatonin, corticosterone, and progesterone in male rats subjected to chronic stress: effect of constant illumination. J Pineal Res 11(2):57–62. https://doi.org/10.1111/j.1600-079x.1991.tb00456.x
Pittendrigh CS (1993) Temporal organization: reflections of a Darwinian clock-watcher. Annu Rev Physiol 55:16–54. https://doi.org/10.1146/annurev.ph.55.030193.000313
Porsolt RD, Le Pichon M, Jalfre M (1977) Depression: a new animal model sensitive to antidepressant treatments. Nature 266(5604):730–732. https://doi.org/10.1038/266730a0
Portune KJ, Benítez-Páez A, Del Pulgar EM, Cerrudo V, Sanz Y (2017) Gut microbiota, diet, and obesity-related disorders-the good, the bad, and the future challenges. Mol Nutr Food Res 61(1) https://doi.org/10.1002/mnfr.201600252
Provencio I, Rodriguez IR, Jiang G, Hayes WP, Moreira EF, Rollag MD (2000) A novel human opsin in the inner retina. J Neurosci 20(2):600–605. https://doi.org/10.1523/jneurosci.20-02-00600.2000
Reiter RJ, Tan DX, Korkmaz A, Erren TC, Piekarski C, Tamura H, Manchester LC (2007) Light at night, chronodisruption, melatonin suppression, and cancer risk: a review. Crit Rev Oncog 13(4):303–328. https://doi.org/10.1615/critrevoncog.v13.i4.30
Rimmer DW, Boivin DB, Shanahan TL, Kronauer RE, Duffy JF, Czeisler CA (2000) Dynamic resetting of the human circadian pacemaker by intermittent bright light. Am J Physiol Regul Integr Comp Physiol 279(5):R1574–R1579. https://doi.org/10.1152/ajpregu.2000.279.5.R1574
Riva A, Borgo F, Lassandro C, Verduci E, Morace G, Borghi E, Berry D (2017) Pediatric obesity is associated with an altered gut microbiota and discordant shifts in Firmicutes populations. Environ Microbiol 19(1):95–105. https://doi.org/10.1111/1462-2920.13463
Rivest RW, Wurtman RJ (1983) Relationship between light intensity and the melatonin and drinking rhythms of rats. Neuroendocrinology 37(2):155–160. https://doi.org/10.1159/000123534
Rosen LN, Targum SD, Terman M, Bryant MJ, Hoffman H, Kasper SF, Hamovit JR, Docherty JP, Welch B, Rosenthal NE (1990) Prevalence of seasonal affective disorder at four latitudes. Psychiatry Res 31(2):131–144. https://doi.org/10.1016/0165-1781(90)90116-m
Rosenthal NE, Sack DA, Gillin JC, Lewy AJ, Goodwin FK, Davenport Y, Mueller PS, Newsome DA, Wehr TA (1984) Seasonal affective disorder. A description of the syndrome and preliminary findings with light therapy. Arch Gen Psychiatry 41(1):72–80 https://doi.org/10.1001/archpsyc.1984.01790120076010
Ruby NF, Brennan TJ, Xie X, Cao V, Franken P, Heller HC, O’Hara BF (2002) Role of melanopsin in circadian responses to light. Science 298(5601):2211–2213. https://doi.org/10.1126/science.1076701
Schiffer F, Johnston AL, Ravichandran C, Polcari A, Teicher MH, Webb RH, Hamblin MR (2009) Psychological benefits 2 and 4 weeks after a single treatment with near infrared light to the forehead: a pilot study of 10 patients with major depression and anxiety. Behav Brain Funct 5:46. https://doi.org/10.1186/1744-9081-5-46
Simpson CA, Diaz-Arteche C, Eliby D, Schwartz OS, Simmons JG, Cowan CSM (2021) The gut microbiota in anxiety and depression - a systematic review. Clin Psychol Rev 83:101943 https://doi.org/10.1016/j.cpr.2020.101943
Stadlbauer V, Engertsberger L, Komarova I, Feldbacher N, Leber B, Pichler G, Fink N, Scarpatetti M, Schippinger W, Schmidt R, Horvath A (2020) Dysbiosis, gut barrier dysfunction and inflammation in dementia: a pilot study. BMC Geriatr 20(1):248. https://doi.org/10.1186/s12877-020-01644-2
Stevens RG (2006) Artificial lighting in the industrialized world: circadian disruption and breast cancer. Cancer Causes Control 17(4):501–507. https://doi.org/10.1007/s10552-005-9001-x
Stojanov S, Berlec A, Štrukelj B (2020) The influence of probiotics on the Firmicutes/Bacteroidetes ratio in the treatment of obesity and inflammatory bowel disease. Microorganisms 8(11):1715. https://doi.org/10.3390/microorganisms8111715
Stothard ER, McHill AW, Depner CM, Birks BR, Moehlman TM, Ritchie HK, Guzzetti JR, Chinoy ED, LeBourgeois MK, Axelsson J, Wright KP Jr (2017) Circadian entrainment to the natural light-dark cycle across seasons and the weekend. Curr Biol 27(4):508–513. https://doi.org/10.1016/j.cub.2016.12.041
Sublette ME, Cheung S, Lieberman E, Hu S, Mann JJ, Uhlemann A-C, Miller JM (2021) Bipolar disorder and the gut microbiome: a systematic review. Bipolar Disord 23(6):544–564. https://doi.org/10.1111/bdi.13049
Sugden D (1989) Melatonin biosynthesis in the mammalian pineal gland. Experientia 45(10):922–932. https://doi.org/10.1007/bf01953049
Sujino M, Masumoto KH, Yamaguchi S, van der Horst GT, Okamura H, Inouye ST (2003) Suprachiasmatic nucleus grafts restore circadian behavioral rhythms of genetically arrhythmic mice. Curr Biol 13(8):664–668. https://doi.org/10.1016/s0960-9822(03)00222-7
Tanaka Y, Akiyoshi J, Kawahara Y, Ishitobi Y, Hatano K, Hoaki N, Mori A, Goto S, Tsuru J, Matsushita H, Hanada H, Kodama K, Isogawa K, Kitamura H, Fujikura Y (2011) Infrared radiation has potential antidepressant and anxiolytic effects in animal model of depression and anxiety. Brain Stimul 4(2):71–76. https://doi.org/10.1016/j.brs.2010.04.001
Thaiss A Christoph, Zeevi D, Levy M, Zilberman-Schapira G, Suez J, Tengeler Anouk C, Abramson L, Katz Meirav N, Korem T, Zmora N, Kuperman Y, Biton I, Gilad S, Harmelin A, Shapiro H, Halpern Z, Segal E, Elinav E (2014) Transkingdom control of microbiota diurnal oscillations promotes metabolic homeostasis. Cell 159(3):514–529. https://doi.org/10.1016/j.cell.2014.09.048
Thapan K, Arendt J, Skene DJ (2001) An action spectrum for melatonin suppression: evidence for a novel non-rod, non-cone photoreceptor system in humans. J Physiol 535(Pt 1):261–267. https://doi.org/10.1111/j.1469-7793.2001.t01-1-00261.x
Touitou Y, Reinberg A, Touitou D (2017) Association between light at night, melatonin secretion, sleep deprivation, and the internal clock: health impacts and mechanisms of circadian disruption. Life Sci 173:94–106. https://doi.org/10.1016/j.lfs.2017.02.008
Tsai JF, Hsiao S, Wang SY (2007) Infrared irradiation has potential antidepressant effect. Prog Neuropsychopharmacol Biol Psychiatry 31(7):1397–1400. https://doi.org/10.1016/j.pnpbp.2007.06.006
Vacca M, Celano G, Calabrese FM, Portincasa P, Gobbetti M, De Angelis M (2020) The controversial role of human gut Lachnospiraceae. Microorganisms 8(4) https://doi.org/10.3390/microorganisms8040573
Wang C, Li W, Wang H, Ma Y, Zhao X, Zhang X, Yang H, Qian J, Li J (2019) Saccharomyces boulardii alleviates ulcerative colitis carcinogenesis in mice by reducing TNF-α and IL-6 levels and functions and by rebalancing intestinal microbiota. BMC Microbiol 19(1):246. https://doi.org/10.1186/s12866-019-1610-8
Wehr TA (1991) The durations of human melatonin secretion and sleep respond to changes in daylength (photoperiod). J Clin Endocrinol Metab 73(6):1276–1280. https://doi.org/10.1210/jcem-73-6-1276
Wei L, Yue F, Xing L, Wu S, Shi Y, Li J, Xiang X, Lam SM, Shui G, Russell R, Zhang D (2020) Constant light exposure alters gut microbiota and promotes the progression of steatohepatitis in high fat diet rats. Front Microbiol 11:1975. https://doi.org/10.3389/fmicb.2020.01975
Wong-Riley MTT, Liang HL, Eells JT, Chance B, Henry MM, Buchmann E, Kane M, Whelan HT (2005) Photobiomodulation directly benefits primary neurons functionally inactivated by toxins: role of cytochrome c oxidase. J Biol Chem 280(6):4761–4771. https://doi.org/10.1074/jbc.M409650200
Wright KP Jr, McHill AW, Birks BR, Griffin BR, Rusterholz T, Chinoy ED (2013b) Entrainment of the human circadian clock to the natural light-dark cycle. Curr Biol 23(16):1554–1558. https://doi.org/10.1016/j.cub.2013.06.039
Wright Kenneth P, McHill Andrew W, Birks Brian R, Griffin Brandon R, Rusterholz T, Chinoy Evan D (2013a) Entrainment of the human circadian clock to the natural light-dark cycle. Curr Biol 23(16):1554–1558 https://doi.org/10.1016/j.cub.2013.06.039
Wu G, Tang W, He Y, Hu J, Gong S, He Z, Wei G, Lv L, Jiang Y, Zhou H, Chen P (2018) Light exposure influences the diurnal oscillation of gut microbiota in mice. Biochem Biophys Res Commun 501(1):16–23. https://doi.org/10.1016/j.bbrc.2018.04.095
Zarrinpar A, Chaix A, Yooseph S, Panda S (2014) Diet and feeding pattern affect the diurnal dynamics of the gut microbiome. Cell Metab 20(6):1006–1017. https://doi.org/10.1016/j.cmet.2014.11.008
Zeitzer JM, Dijk DJ, Kronauer R, Brown E, Czeisler C (2000) Sensitivity of the human circadian pacemaker to nocturnal light: melatonin phase resetting and suppression. J Physiol 526 Pt 3(Pt 3):695–702 https://doi.org/10.1111/j.1469-7793.2000.00695.x
Zeitzer JM, Khalsa SB, Boivin DB, Duffy JF, Shanahan TL, Kronauer RE, Czeisler CA (2005) Temporal dynamics of late-night photic stimulation of the human circadian timing system. Am J Physiol Regul Integr Comp Physiol 289(3):R839–R844. https://doi.org/10.1152/ajpregu.00232.2005
Zhang Y, Fan Q, Hou Y, Zhang X, Yin Z, Cai X, Wei W, Wang J, He D, Wang G, Yuan Y, Hao H, Zheng X (2022) Bacteroides species differentially modulate depression-like behavior via gut-brain metabolic signaling. Brain, Behav, Immun 102:11–22. https://doi.org/10.1016/j.bbi.2022.02.007
Zhao L (2013) The gut microbiota and obesity: from correlation to causality. Nat Rev Microbiol 11(9):639–647. https://doi.org/10.1038/nrmicro3089
Acknowledgements
We are thankful to the China Scholarship Council (CSC) for supporting the doctoral student WW (CSC 201806020189).
Funding
This work was financially supported by the grant from the Beijing Natural Science Foundation (7222112) and National Natural Science Foundation of China (82101626).
Author information
Authors and Affiliations
Contributions
HL supervised this study. HL and WW conceived and designed this research. WW and ZH conducted the animal experiments and prepared the figures. WW and ZH analyzed data. WW and HL wrote the manuscript. ZW and JC conducted the light measurement and prepared the figures. ZH contributed funding acquisition. All authors have read, revised, and approved the manuscript.
Corresponding authors
Ethics declarations
Ethics approval
This experiment followed the National Institutes of Health Guide for the Care and Use of Laboratory Animals, and the protocols were approved by the Biological and Medical Ethics Committee of Beihang University.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, W., Hao, Z., Wu, Z. et al. Long-term artificial/natural daytime light affects mood, melatonin, corticosterone, and gut microbiota in rats. Appl Microbiol Biotechnol 107, 2689–2705 (2023). https://doi.org/10.1007/s00253-023-12446-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00253-023-12446-y