Abstract
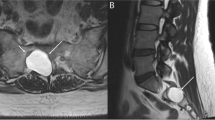
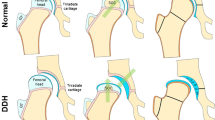
Children living with achondroplasia are at an increased risk of developing neurological complications, which may be associated with acute and life-altering events. To remediate this risk, the timely acquisition of effective neuroimaging that can help to guide clinical management is essential. We propose imaging protocols and follow-up strategies for evaluating the neuroanatomy of these children and to effectively identify potential neurological complications, including compression at the cervicomedullary junction secondary to foramen magnum stenosis, spinal deformity and spinal canal stenosis. When compiling these recommendations, emphasis has been placed on reducing scan times and avoiding unnecessary radiation exposure. Standardized imaging protocols are important to ensure that clinically useful neuroimaging is performed in children living with achondroplasia and to ensure reproducibility in future clinical trials. The members of the European Society of Pediatric Radiology (ESPR) Neuroradiology Taskforce and European Society of Neuroradiology pediatric subcommittee, together with clinicians and surgeons with specific expertise in achondroplasia, wrote this opinion paper. The research committee of the ESPR also endorsed the final draft. The rationale for these recommendations is based on currently available literature, supplemented by best practice opinion from radiologists and clinicians with subject-specific expertise.
Graphical Abstract






Similar content being viewed by others
Data availability
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
References
Pauli RM (2019) Achondroplasia: a comprehensive clinical review. Orphanet J Rare Dis 14:1. https://doi.org/10.1186/s13023-018-0972-6
Foreman PK, van Kessel F, van Hoorn R et al (2020) Birth prevalence of achondroplasia: a systematic literature review and meta-analysis. Am J Med Genet A 182:2297–2316. https://doi.org/10.1002/ajmg.a.61787
Cormier-Daire V, AlSayed M, Ben-Omran T et al (2021) The first European consensus on principles of management for achondroplasia. Orphanet J Rare Dis 16:333. https://doi.org/10.1186/s13023-021-01971-6
Kubota T, Adachi M, Kitaoka T et al (2020) Clinical practice guidelines for achondroplasia. Clin Pediatr Endocrinol 29:25–42. https://doi.org/10.1297/cpe.29.25
Savarirayan R, Ireland P, Irving M et al (2022) International Consensus Statement on the diagnosis, multidisciplinary management and lifelong care of individuals with achondroplasia. Nat Rev Endocrinol 18:173–189. https://doi.org/10.1038/s41574-021-00595-x
Rignol G, Garcia S, Authier F et al (2022) Longitudinal imaging of the skull base synchondroses demonstrate prevention of a premature ossification after recifercept treatment in mouse model of achondroplasia. JBMR PLUS 6:e10568. https://doi.org/10.1002/jbm4.10568
Antonov NK, Ruzal-Shapiro CB, Morel KD et al (2017) Feed and wrap MRI technique in infants. Clin Pediatr (Phila) 56:1095–1103. https://doi.org/10.1177/0009922816677806
D’Arco F, Mertiri L, de Graaf P et al (2022) Guidelines for magnetic resonance imaging in pediatric head and neck pathologies: a multicentre international consensus paper. Neuroradiology 64:1081–1100. https://doi.org/10.1007/s00234-022-02950-9
Avula S, Peet A, Morana G et al (2021) European Society for Paediatric Oncology (SIOPE) MRI guidelines for imaging patients with central nervous system tumours. Childs Nerv Syst 37:2497–2508. https://doi.org/10.1007/s00381-021-05199-4
Watson SG, Calder AD, Offiah AC, Negus S (2015) A review of imaging protocols for suspected skeletal dysplasia and a proposal for standardisation. Pediatr Radiol 45:1733–1737. https://doi.org/10.1007/s00247-015-3381-1
Wattjes MP, Ciccarelli O, Reich DS et al (2021) 2021 MAGNIMS-CMSC-NAIMS consensus recommendations on the use of MRI in patients with multiple sclerosis. Lancet Neurol 20:653–670. https://doi.org/10.1016/S1474-4422(21)00095-8
Armstrong JA, Pacey V, Tofts LJ (2022) Medical complications in children with achondroplasia. Dev Med Child Neurol 64:989–997. https://doi.org/10.1111/dmcn.15194
Cheung MS, Irving M, Cocca A et al (2021) Achondroplasia Foramen Magnum Score: screening infants for stenosis. Arch Dis Child 106:180–184. https://doi.org/10.1136/archdischild-2020-319625
White KK, Bompadre V, Goldberg MJ et al (2016) Best practices in the evaluation and treatment of foramen magnum stenosis in achondroplasia during infancy. Am J Med Genet A 170A:42–51. https://doi.org/10.1002/ajmg.a.37394
Sanders VR, Sheldon SH, Charrow J (2019) Cervical spinal cord compression in infants with achondroplasia: should neuroimaging be routine? Genet Med 21:459–463. https://doi.org/10.1038/s41436-018-0070-0
Fornarino S, Rossi DP, Severino M et al (2017) Early impairment of somatosensory evoked potentials in very young children with achondroplasia with foramen magnum stenosis. Dev Med Child Neurol 59:192–198. https://doi.org/10.1111/dmcn.13243
Mackenzie WG, Dhawale AA, Demczko MM et al (2013) Flexion-extension cervical spine MRI in children with skeletal dysplasia: is it safe and effective? J Pediatr Orthop 33:91–98. https://doi.org/10.1097/BPO.0b013e318279c51f
Danielpour M, Wilcox WR, Alanay Y et al (2007) Dynamic cervicomedullary cord compression and alterations in cerebrospinal fluid dynamics in children with achondroplasia. Report of four cases. J Neurosurg 107:504–507. https://doi.org/10.3171/PED-07/12/504
Brühl K, Stoeter P, Wietek B et al (2001) Cerebral spinal fluid flow, venous drainage and spinal cord compression in achondroplastic children: impact of magnetic resonance findings for decompressive surgery at the cranio-cervical junction. Eur J Pediatr 160:10–20. https://doi.org/10.1007/pl00008410
Bosemani T, Orman G, Hergan B et al (2015) Achondroplasia in children: correlation of ventriculomegaly, size of foramen magnum and jugular foramina, and emissary vein enlargement. Childs Nerv Syst 31:129–133. https://doi.org/10.1007/s00381-014-2559-4
D’Arco F, Ganau M (2019) Which neuroimaging techniques are really needed in Chiari I? A short guide for radiologists and clinicians. Childs Nerv Syst 35:1801–1808. https://doi.org/10.1007/s00381-019-04210-3
Kashanian A, Stadler JA, Danielpour M (2022) Neurosurgical evaluation and management of children with achondroplasia. Neurosurg Clin N Am 33:17–23. https://doi.org/10.1016/j.nec.2021.09.003
Manikkam SA, Chetcuti K, Howell KB et al (2018) Temporal lobe malformations in achondroplasia: expanding the brain imaging phenotype associated with FGFR3-related skeletal dysplasias. AJNR Am J Neuroradiol 39:380–384. https://doi.org/10.3174/ajnr.A5468
Leiva-Gea A, Martos Lirio MF, Barreda Bonis AC et al (2022) Achondroplasia: update on diagnosis, follow-up and treatment. An Pediatr (Barc) 97:423.e1-423.e11. https://doi.org/10.1016/j.anpede.2022.10.004
Severino M, Geraldo AF, Utz N et al (2020) Definitions and classification of malformations of cortical development: practical guidelines. Brain 143:2874–2894. https://doi.org/10.1093/brain/awaa174
Jenko N, Connolly DJA, Raghavan A et al (2022) The (extended) achondroplasia foramen magnum score has good observer reliability. Pediatr Radiol 52:1512–1520. https://doi.org/10.1007/s00247-022-05348-0
Goldberg AL, Kershah SM (2010) Advances in imaging of vertebral and spinal cord injury. J Spinal Cord Med 33:105–116. https://doi.org/10.1080/10790268.2010.11689685
Gürbüz MS, Berkman MZ, Ünal E et al (2015) Foramen magnum decompression and duraplasty is superior to only foramen magnum decompression in Chiari malformation type 1 associated with syringomyelia in adults. Asian Spine J 9:721–727. https://doi.org/10.4184/asj.2015.9.5.721
Bagley CA, Pindrik JA, Bookland MJ et al (2006) Cervicomedullary decompression for foramen magnum stenosis in achondroplasia. J Neurosurg 104:166–172. https://doi.org/10.3171/ped.2006.104.3.166
Vakharia VN, Smith L, Tahir Z et al (2021) Occipitocervical instrumented fixation utilising patient-specific C2 3D-printed spinal screw trajectory guides in complex paediatric skeletal dysplasia. Childs Nerv Syst 37:2643–2650. https://doi.org/10.1007/s00381-021-05260-2
Cox M, Kung D, Hurst RW et al (2019) Significance of the absent vertebral artery T2 flow void on cervical spine MRI in atraumatic patients without acute neurological symptoms. Neuroradiol J 32:154–157. https://doi.org/10.1177/1971400919839201
Blaser SI (2008) Abnormal skull shape. Pediatr Radiol 38(Suppl 3):S488–S496. https://doi.org/10.1007/s00247-008-0867-0
Moritani T, Aihara T, Oguma E et al (2006) Magnetic resonance venography of achondroplasia: correlation of venous narrowing at the jugular foramen with hydrocephalus. Clin Imaging 30:195–200. https://doi.org/10.1016/j.clinimag.2005.10.004
Offiah AC, Hall CM (2020) The radiologic diagnosis of skeletal dysplasias: past, present and future. Pediatr Radiol 50:1650–1657. https://doi.org/10.1007/s00247-019-04533-y
Rahimizadeh A, Soufiani HF, Hassani V, Rahimizadeh A (2015) Atlantoaxial subluxation due to an os odontoideum in an achondroplastic adult: report of a case and review of the literature. Case Rep Orthop 2015:142586. https://doi.org/10.1155/2015/142586
Misra SN, Morgan HW (2003) Thoracolumbar spinal deformity in achondroplasia. Neurosurg Focus 14:e4. https://doi.org/10.3171/foc.2003.14.1.5
Margalit A, McKean G, Lawing C et al (2018) Walking out of the curve: thoracolumbar kyphosis in achondroplasia. J Pediatr Orthop 38:491–497. https://doi.org/10.1097/BPO.0000000000000862
Karol LA (2012) Spinal deformity in children with achondroplasia. Spine Deform 1:107–113. https://doi.org/10.1016/j.jspd.2012.04.009
White KK, Bober MB, Cho T-J et al (2020) Best practice guidelines for management of spinal disorders in skeletal dysplasia. Orphanet J Rare Dis 15:161. https://doi.org/10.1186/s13023-020-01415-7
Matsushita M, Kitoh H, Mishima K et al (2016) Low bone mineral density in achondroplasia and hypochondroplasia. Pediatr Int 58:705–708. https://doi.org/10.1111/ped.12890
Matsushita T, Wilcox WR, Chan YY et al (2009) FGFR3 promotes synchondrosis closure and fusion of ossification centers through the MAPK pathway. Hum Mol Genet 18:227–240. https://doi.org/10.1093/hmg/ddn339
Sarioglu FC, Sarioglu O, Guleryuz H (2020) Neuroimaging and calvarial findings in achondroplasia. Pediatr Radiol 50:1669–1679. https://doi.org/10.1007/s00247-020-04841-8
Mäkitie O, Kaitila I (1993) Cartilage-hair hypoplasia–clinical manifestations in 108 Finnish patients. Eur J Pediatr 152:211–217. https://doi.org/10.1007/BF01956147
Mäkitie O, Marttinen E, Kaitila I (1992) Skeletal growth in cartilage-hair hypoplasia. A radiological study of 82 patients. Pediatr Radiol 22:434–439. https://doi.org/10.1007/BF02013505
Graham JM, Krakow D, Tolo VT et al (2001) Radiographic findings and Gs-alpha bioactivity studies and mutation screening in acrodysostosis indicate a different etiology from pseudohypoparathyroidism. Pediatr Radiol 31:2–9. https://doi.org/10.1007/s002470000355
Huet T, Cohen-Solal M, Laredo J-D et al (2020) Lumbar spinal stenosis and disc alterations affect the upper lumbar spine in adults with achondroplasia. Sci Rep 10:4699. https://doi.org/10.1038/s41598-020-61704-w
Calandrelli R, Pilato F, Massimi L et al (2022) Thoracolumbar stenosis and neurologic symptoms: quantitative MRI in achondroplasia. J Neuroimaging 32:884–893. https://doi.org/10.1111/jon.13015
Rossi A, Argyropoulou M, Zlatareva D et al (2023) European recommendations on practices in pediatric neuroradiology: consensus document from the European Society of Neuroradiology (ESNR), European Society of Paediatric Radiology (ESPR) and European Union of Medical Specialists Division of Neuroradiology (UEMS). Pediatr Radiol 53:159–168. https://doi.org/10.1007/s00247-022-05479-4
White ML, Zhang Y, Healey K (2011) Cervical spinal cord multiple sclerosis: evaluation with 2D multi-echo recombined gradient echo MR imaging. J Spinal Cord Med 34:93–98. https://doi.org/10.1179/107902610X12911165975025
Rekate HL (2019) Pathogenesis of hydrocephalus in achondroplastic dwarfs: a review and presentation of a case followed for 22 years. Childs Nerv Syst 35:1295–1301. https://doi.org/10.1007/s00381-019-04227-8
Kim J, Patel VJ, El Ahmadieh TY et al (2021) Hydrocephalus in achondroplasia: efficacy of endoscopic third ventriculostomy. J Neurosurg Pediatr: 1–8. https://doi.org/10.3171/2021.9.PEDS21242
Ramachandran S, Steinbok P (2019) Hydrocephalus in achondroplasia and venous hypertension. In: Cinalli G, Özek MM, Sainte-Rose C (eds) Pediatric hydrocephalus. Springer International Publishing, Cham, pp 1065–1081
King JAJ, Vachhrajani S, Drake JM, Rutka JT (2009) Neurosurgical implications of achondroplasia. J Neurosurg Pediatr 4:297–306. https://doi.org/10.3171/2009.3.PEDS08344
Schkrohowsky JG, Hoernschemeyer DG, Carson BS, Ain MC (2007) Early presentation of spinal stenosis in achondroplasia. J Pediatr Orthop 27:119–122. https://doi.org/10.1097/01.bpb.0000248570.50875.28
Afshari FT, Slator N, Fayeye O et al (2023) Spinal canal stenosis in children with achondroplasia: the role of augmentation laminoplasty-a 15-year single institution experience. Childs Nerv Syst 39:229–237. https://doi.org/10.1007/s00381-022-05566-9
McDonald EJ, De Jesus O (2023) Achondroplasia. StatPearls Publishing, Treasure Island, FL. https://www.ncbi.nlm.nih.gov/books/NBK559263/. Accessed 15 Mar 2023
Calandrelli R, Pilato F, D’Apolito G et al (2022) Airways and craniofacial assessment in children affected by achondroplasia with and without sleep-disordered breathing: quantitative magnetic resonance study. Childs Nerv Syst 38:1147–1154. https://doi.org/10.1007/s00381-022-05484-w
Forsyth R, Groves M, Sterni L, Hoover-Fong J (2021) Screening neuroimaging and polysomnography (PSG) in children <5 years of age with achondroplasia: a single multidisciplinary clinic experience. Mol Genet Metab 132:S128. https://doi.org/10.1016/S1096-7192(21)00281-X
Calandrelli R, Pilato F, Massimi L et al (2022) Impairment of motor skills in children with achondroplasia-usefulness of brain and cranio-cervical junction evaluation by quantitative magnetic resonance imaging: a case-control study. Acta Radiol 63:1703–1711. https://doi.org/10.1177/02841851211055821
Shim Y, Ko JM, Cho T-J et al (2021) Predictors of cervical myelopathy and hydrocephalus in young children with achondroplasia. Orphanet J Rare Dis 16:81. https://doi.org/10.1186/s13023-021-01725-4
Allegri AEM, Di IN, Severino M et al (2019) Foramen magnum stenosis (FMS): neuroradiological aspects before and after cervical decompression in paediatric patients with achondroplasia (ACH). BA. https://doi.org/10.1530/boneabs.7.LB10
Identification of characteristic neurological complications in infants with achondroplasia by routine MRI screening | ESPE2018 | 57th Annual ESPE | ESPE Abstracts. https://abstracts.eurospe.org/hrp/0089/hrp0089rfc2.5. Accessed 16 Mar 2023
Unger S, Bonafé L, Gouze E (2017) Current care and investigational therapies in achondroplasia. Curr Osteoporos Rep 15:53–60. https://doi.org/10.1007/s11914-017-0347-2
Calandrelli R, Panfili M, D’Apolito G et al (2017) Quantitative approach to the posterior cranial fossa and craniocervical junction in asymptomatic children with achondroplasia. Neuroradiology 59:1031–1041. https://doi.org/10.1007/s00234-017-1887-y
(2016) 25th Congress of the European Society for Pediatric Neurosurgery (ESPN) Paris-France, 8–11 May 2016. Childs Nerv Syst 32:905–1012. https://doi.org/10.1007/s00381-016-3044-z
Bosemani T, Orman G, Carson KA et al (2014) Diffusion tensor imaging of the brainstem in children with achondroplasia. Dev Med Child Neurol 56:1085–1092. https://doi.org/10.1111/dmcn.12492
Fernandes JA, Devalia KL, Moras P et al (2014) Screening for spinal stenosis in achondroplastic patients undergoing limb lengthening. J Pediatr Orthop B 23:181–186. https://doi.org/10.1097/BPB.0000000000000027
Mukherjee D, Pressman BD, Krakow D et al (2014) Dynamic cervicomedullary cord compression and alterations in cerebrospinal fluid dynamics in children with achondroplasia: review of an 11-year surgical case series. J Neurosurg Pediatr 14:238–244. https://doi.org/10.3171/2014.5.PEDS12614
Gil Z, Tauman R, Sivan J et al (2001) Neurosurgical aspects in achondroplasia: evaluation and treatment. Harefuah 140(1026–31):1118
Rollins N, Booth T, Shapiro K (2000) The use of gated cine phase contrast and MR venography in achondroplasia. Childs Nerv Syst 16:569–75. https://doi.org/10.1007/PL00007299. (discussion 575)
Keiper GL, Koch B, Crone KR (1999) Achondroplasia and cervicomedullary compression: prospective evaluation and surgical treatment. Pediatr Neurosurg 31:78–83. https://doi.org/10.1159/000028838
Kao SC, Waziri MH, Smith WL et al (1989) MR imaging of the craniovertebral junction, cranium, and brain in children with achondroplasia. AJR Am J Roentgenol 153:565–569. https://doi.org/10.2214/ajr.153.3.565
Thomas IT, Frias JL, Williams JL, Friedman WA (1988) Magnetic resonance imaging in the assessment of medullary compression in achondroplasia. Am J Dis Child 142:989–992. https://doi.org/10.1001/archpedi.1988.02150090087031
Wang H, Rosenbaum AE, Reid CS et al (1987) Pediatric patients with achondroplasia: CT evaluation of the craniocervical junction. Radiology 164:515–519. https://doi.org/10.1148/radiology.164.2.3602395
Reid CS, Pyeritz RE, Kopits SE et al (1987) Cervicomedullary compression in young patients with achondroplasia: value of comprehensive neurologic and respiratory evaluation. J Pediatr 110:522–530. https://doi.org/10.1016/s0022-3476(87)80542-5
Acknowledgements
Study collaborators and affiliations
Members of the ESPR Neuroradiology Taskforce:
Andrea Rossi1,2, Catherine Adamsbaum3, Vasileios Xydis4, Daniel Connolly5, Maarten Hans Lequin6, Volodia Dangouloff-Ros7, Luciana Porto8, Eleonora Piccirilli9,10, Jean-François Chateil11, Élida Vázquez Méndez.12
Members of the ESNR Pediatric Subcommittee:
Kshitij Mankad13, Chen Hoffmann14, Ana Filipa Geraldo.15,16
1Neuroradiology Unit, IRCCS Istituto Giannina Gaslini, Genoa, Italy.
2Department of Health Sciences (DISSAL), University of Genoa, Genoa, Italy.
3Faculty of Medicine, Paris-Saclay University, 63 Rue Gabriel Péri, 94270, Le Kremlin Bicêtre, France.
4Department of Clinical Radiology & Imaging, Medical School, University Ioannina, 45,100 Ioannina, Greece.
5Department of Neuroradiology, Sheffield Children’s Hospital, Sheffield, UK.
6Division of Imaging and Oncology, Department of Radiology UMCU Utrecht, The Netherlands.
7Service de Radiologie Pédiatrique, Hôpital Universitaire Necker Enfants Malades, Paris, France.
8Institute of Neuroradiology, Hospital of Goethe University, University Hospital Frankfurt, Schleusenweg 2 – 16, 60,528 Frankfurt am Main, Germany.
9Neuro-Oncology Unit, Department of Imaging, Bambino Gesù Children’s Hospital, Rome, Italy.
10Department of Neuroscience, Imaging and Clinical Sciences, University “G. D’Annunzio” of Chieti-Pescara, Chieti, Italy.
11Centre de Résonance Magnétique des Systèmes Biologiques, UMR5536 CNRS/Univ. Bordeaux, F-33076, Bordeaux, France.
12Pediatric Radiology, Hospital Universitari Vall d’Hebron, Vall d’Hebron Barcelona Hospital Campus, Spain.
13Department of Radiology, Great Ormond Street Hospital for Children NHS Foundation Trust, Great Ormond Street, London, UK.
14Tel Hashomer Hospital—Chaim Sheba Medical Center, Department of Radiology, Ramat-Gan, Israel.
15Diagnostic Neuroradiology Unit, Imaging department, Centro Hospitalar Vila Nova de Gaia/Espinho (CHVNG/E), Porto, Portugal.
16Clínica Universitária de Imagiologia, Faculty of Medicine of the University of Lisbon, Lisbon, Portugal.
Author information
Authors and Affiliations
Consortia
Contributions
• J.W. conceived and wrote the manuscript, researched the literature, and formatted the tables.
• F.D’A. conceived and wrote the manuscript and provided the figures.
• D.T. and M.C. conceived and wrote the manuscript.
• A.C., J.L., M.I.A., P.C.R., M.S., and O.A. participated in the first version and contacted the research board of the European Society of Pediatric Radiology (O.A.), the ESNR (M.S.), and the Neuroradiology Taskforce (M.I.A.) for endorsement.
• A.S. reviewed the images.
• All authors contributed to the process of drafting and editing the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
Rights and permissions
About this article
Cite this article
Wright, J., Cheung, M., Siddiqui, A. et al. Recommendations for neuroradiological examinations in children living with achondroplasia: a European Society of Pediatric Radiology and European Society of Neuroradiology opinion paper. Pediatr Radiol 53, 2323–2344 (2023). https://doi.org/10.1007/s00247-023-05728-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-023-05728-0