Abstract
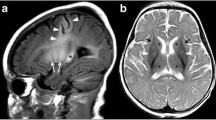
White matter changes are seen in a spectrum of disorders in children and adolescents. Understanding their distribution and appearance helps to reach diagnoses in daily radiologic practice. This pictorial essay will outline the magnetic resonance imaging (MRI) appearances of diseases with white matter changes including demyelinating diseases, dysmyelinating disorders/leukodystrophies, infections, autoimmune diseases, vascular causes, mitochondrial disorders and neurocutaneous syndromes, along with a brief overview of clinical aspects of the diseases such as typical age of presentation, etiology, symptoms and signs and treatment options. This article highlights important features in common white matter diseases in children and adolescents.




















Similar content being viewed by others
References
Branson HM (2013) Normal myelination: a practical pictorial review. Neuroimag Clin N Am 23:183–195
Barkovich AJ, Raybaud C (2012) Normal development of the neonatal and infant brain, skull, and spine. In: Pediatric neuroimaging, 5th edn. Lippincott Williams & Wilkins, Philadelphia, pp 20–80
Levine LE (2017) Physical development: the brain and the body. In: Child development: an active learning approach, 4th edn. SAGE Publications, Inc, Newbury Park, pp 177–221
Cheon J-E, Kim I-O, Hwang YS et al (2002) Leukodystrophy in children: a pictorial review of MR imaging features. Radiographics 22:461–76
van der Knaap MS, Valk J, de Neeling N, Nauta JJ (1991) Pattern recognition in magnetic resonance imaging of white matter disorders in children and young adults. Neuroradiology 33:478–493
Schiffmann R, van der Knaap MS (2009) Invited article: an MRI-based approach to the diagnosis of white matter disorders. Neurology 72:750–759
Barkovich AJ, Raybaud C (2012) Metabolic, toxic, and autoimmune/inflammatory brain disorders. Pediatric neuroimaging, 5th edn. Lippincott Williams & Wilkins, Philadelphia, pp 81–239
Lee YJ (2011) Acute disseminated encephalomyelitis in children: differential diagnosis from multiple sclerosis on the basis of clinical course. Korean J Pediatr 54:234–240
Gveric D (1999) Inflammatory cascades in the pathogenesis of multiple sclerosis lesions. Doctoral thesis, University College London
Waldman AT, Gorman MP, Rensel MR et al (2011) Management of pediatric central nervous system demyelinating disorders: consensus of United States neurologists. J Child Neurol 26:675–682
Weinshenker BG, O’Brien PC, Petterson TM et al (1999) A randomized trial of plasma exchange in acute central nervous system inflammatory demyelinating disease. Ann Neurol 46:878–886
Santosh Rai PV, Suresh BV, Bhat IG et al (2013) Childhood adrenoleukodystrophy — classic and variant — review of clinical manifestations and magnetic resonance imaging. J Pediatr Neurosci 8:192–197
Berger J, Pujol A, Aubourg P, Forss-Petter S (2010) Current and future pharmacological treatment strategies in X-linked adrenoleukodystrophy. Brain Pathol 20:845–856
Singh I, Singh AK, Contreras MA (2009) Peroxisomal dysfunction in inflammatory childhood white matter disorders: an unexpected contributor to neuropathology. J Child Neurol 24:1147–1157
Paintlia AS, Glig AG, Khan M et al (2003) Correlation of very long chain fatty acid accumulation and inflammatory disease progression in childhood X-ALD: implications for potential therapies. Neurobiol Dis 14:425–439
Barkovich AJ, Raybaud C (2012) Infections of the developing and mature nervous system. Pediatric neuroimaging, 5th edn. Lippincott Williams & Wilkins, Philadelphia, pp 954–1050
Lucignani G, Guarnera A, Rossi-Espagnet MC et al (2022) From fetal to neonatal neuroimaging in TORCH infections: a pictorial review. Children 9:1210
Diogo MC, Glatter S, Binder J et al (2020) The MRI spectrum of congenital cytomegalovirus infection. Prenat Diagn 40:110–124
Sawlani V, Shankar JJS, White C (2013) Magnetic resonance imaging findings in a case of congenital rubella encephalitis. Can J Infect Dis Med Microbiol 24:122–123
Tamura T, Morikawa A, Kikuchi K (1996) Diffuse white matter lesions associated with herpes simplex encephalitis as observed on magnetic resonance imaging. Brain Dev 18:150–152
Song Y, Li S, Xiao W et al (2021) Influenza-associated encephalopathy and acute necrotizing encephalopathy in children: a retrospective single-center study. Med Sci Monit 27:e928374
Studahl M (2003) Influenza virus and CNS manifestations. J Clin Virol 28:225–232
Bartels F, Krohn S, Nikolaus M et al (2020) Clinical and magnetic resonance imaging outcome predictors in pediatric anti-N-methyl-D-aspartate receptor encephalitis. Ann Neurol 88:148–159
Hunter JV (2002) Magnetic resonance imaging in pediatric stroke. Top Magn Reson Imaging 13:23–38
Gropman AL (2013) Neuroimaging in mitochondrial disorders. Neurotherapeutics 10:273–285
Valanne L, Ketonen L, Majander A et al (1998) Neuroradiologic findings in children with mitochondrial disorders. AJNR Am J Neuroradiol 19:369–377
Baron Y, Barkovich AJ (1999) MR imaging of tuberous sclerosis in neonates and young infants. AJNR Am J Neuroradiol 20:907–916
Willemsen MAA, Van Der Graaf M, Van Der Knaap MS et al (2004) MR imaging and proton MR spectroscopic studies in Sjögren-Larsson syndrome: characterization of the leukoencephalopathy. AJNR Am J Neuroradiol 25:649–657
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kwok, P.L., Lai, A.Y.T., Lai, B.M.H. et al. Magnetic resonance imaging of disorders with white matter changes in children and adolescents: a pictorial essay. Pediatr Radiol 53, 1188–1206 (2023). https://doi.org/10.1007/s00247-022-05580-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-022-05580-8