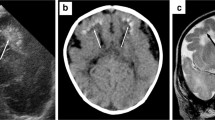
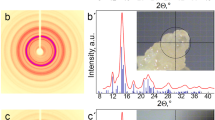
Abstract
This article is the first of a two-part series on intracranial calcification in childhood. Intracranial calcification can be either physiological or pathological. Physiological intracranial calcification is not an expected neuroimaging finding in the neonatal or infantile period but occurs, as children grow older, in the pineal gland, habenula, choroid plexus and occasionally the dura mater. Pathological intracranial calcification can be broadly divided into infectious, congenital, endocrine/metabolic, vascular and neoplastic. The main goals in Part 1 are to discuss the chief differences between physiological and pathological intracranial calcification, to discuss the histological characteristics of intracranial calcification and how intracranial calcification can be detected across neuroimaging modalities, to emphasize the importance of age at presentation and intracranial calcification location, and to propose a comprehensive neuroimaging approach toward the differential diagnosis of the causes of intracranial calcification. Finally, in Part 1 the authors discuss the most common causes of infectious intracranial calcification, especially in the neonatal period, and congenital causes of intracranial calcification. Various neuroimaging modalities have distinct utilities and sensitivities in the depiction of intracranial calcification. Age at presentation, intracranial calcification location, and associated neuroimaging findings are useful information to help narrow the differential diagnosis of intracranial calcification. Intracranial calcification can occur in isolation or in association with other neuroimaging features. Intracranial calcification in congenital infections has been associated with clastic changes, hydrocephalus, chorioretinitis, white matter abnormalities, skull changes and malformations of cortical development. Infections are common causes of intracranial calcification, especially neonatal TORCH (toxoplasmosis, other [syphilis, varicella-zoster, parvovirus B19], rubella, cytomegalovirus and herpes) infections.























Similar content being viewed by others
References
Institute of Medicine (US) Committee to Review Dietary Reference Intakes for Vitamin D and Calcium (2011) Dietary reference intakes for calcium and Vitamin D. The National Academies Press, Washington, DC
Marambaud P, Dreses-Werringloer U, Vingtdeux V (2009) Calcium signaling in neurodegeneration. Mol Neurodegener 4:20
Sama DM, Norris CM (2013) Calcium dysregulation and neuroinflammation: discrete and integrated mechanisms for age-related synaptic dysfunction. Ageing Res Rev 12:982–995
Zhivotovsky B, Orrenius S (2011) Calcium and cell death mechanisms: a perspective from the cell death community. Cell Calcium 50:211–221
Liu K, Ding L, Li Y et al (2014) Neuronal necrosis is regulated by a conserved chromatin-modifying cascade. Proc Natl Acad Sci U S A 111:13960–13965
McCartney E, Squier W (2014) Patterns and pathways of calcification in the developing brain. Dev Med Child Neurol 56:1009–1015
Kieffer SA, Gold LH (1974) Intracranial physiologic calcifications. Semin Roentgenol 9:151–162
Kıroğlu Y, Callı C, Karabulut N, Oncel C (2010) Intracranial calcifications on CT. Diagn Interv Radiol 16:263–269
Lago EG, Baldisserotto M, Hoefel Filho JR et al (2007) Agreement between ultrasonography and computed tomography in detecting intracranial calcifications in congenital toxoplasmosis. Clin Radiol 62:1004–1011
Livingston JH, Stivaros S, Warren D, Crow YJ (2014) Intracranial calcification in childhood: a review of aetiologies and recognizable phenotypes. Dev Med Child Neurol 56:612–626
Go JL, Zee CS (1998) Unique CT imaging advantages. Hemorrhage and calcification. Neuroimaging Clin N Am 8:541–558
Machida H, Tanaka I, Fukui R et al (2016) Dual-energy spectral CT: various clinical vascular applications. Radiographics 36:1215–1232
Nute JL, Le Roux L, Chandler AG et al (2015) Differentiation of low-attenuation intracranial hemorrhage and calcification using dual-energy computed tomography in a phantom system. Investig Radiol 50:9–16
Hu R, Daftari Besheli L, Young J et al (2016) Dual-energy head CT enables accurate distinction of intraparenchymal hemorrhage from calcification in emergency department patients. Radiology 280:177–183
American Society of Neuroradiology (2015) ACR–ASNR practice parameter for the performance of computed tomography (CT) of the brain revised 2015 (Resolution 20). https://www.asnr.org/guidelines-standards/acr-asnr-practice-parameter-for-the-performance-of-computed-tomography-ct-of-the-brain-revised-2015-resolution-20/. Accessed 27 Mar 2020
Greer M-LC (2018) Imaging of cancer predisposition syndromes. Pediatr Radiol 48:1364–1375
Sedghizadeh PP, Nguyen M, Enciso R (2012) Intracranial physiological calcifications evaluated with cone beam CT. Dentomaxillofac Radiol 41:675–678
Whitehead MT, Oh C, Raju A, Choudhri AF (2015) Physiologic pineal region, choroid plexus, and dural calcifications in the first decade of life. AJNR Am J Neuroradiol 36:575–580
Sapède D, Cau E (2013) The pineal gland from development to function. Curr Top Dev Biol 106:171–215
Kendall B, Cavanagh N (1986) Intracranial calcification in paediatric computed tomography. Neuroradiology 28:324–330
Adeeb N, Mortazavi MM, Tubbs RS, Cohen-Gadol AA (2012) The cranial dura mater: a review of its history, embryology, and anatomy. Childs Nerv Syst 28:827–837
McKinney AM (2017) Basal ganglia: physiologic calcifications. Atlas of normal imaging variations of the brain, skull, and craniocervical vasculature. Springer International Publishing, Cham, pp 427–440
Cox MA, Davis M, Voin V et al (2017) Pineal gland agenesis: review and case illustration. Cureus 9:e1314
Lun MP, Monuki ES, Lehtinen MK (2015) Development and functions of the choroid plexus-cerebrospinal fluid system. Nat Rev Neurosci 16:445–457
McKinney AM (2017) Dural calcifications: normal locations and appearances. Atlas of normal imaging variations of the brain, skull, and craniocervical vasculature. Springer International Publishing, Cham, pp 391–411
Qureshi PAAA, Qureshi MR, Rehan B (2017) Dehiscence of the lamina papyracea: MRI findings in correlation with CT appearance. Pak J Radiol 27:398–400
Pappamikail L, Rato R, Novais G, Bernardo E (2013) Chronic calcified subdural hematoma: case report and review of the literature. Surg Neurol Int 4:21
Daghighi MH, Rezaei V, Zarrintan S, Pourfathi H (2007) Intracranial physiological calcifications in adults on computed tomography in Tabriz, Iran. Folia Morphol (Warsz) 66:115–119
Murphy MJ (1979) Clinical correlations of CT scan-detected calcifications of the basal ganglia. Ann Neurol 6:507–511
Legido A, Zimmerman RA, Packer RJ et al (1988) Significance of basal ganglia calcification on computed tomography in children. Pediatr Neurosci 14:64–70
Herron J, Darrah R, Quaghebeur G (2000) Intra-cranial manifestations of the neurocutaneous syndromes. Clin Radiol 55:82–98
Randle SC (2017) Tuberous sclerosis complex: a review. Pediatr Ann 46:e166–e171
Northrup H, Krueger DA, International Tuberous Sclerosis Complex Consensus Group (2013) Tuberous sclerosis complex diagnostic criteria update: recommendations of the 2012 International Tuberous Sclerosis Complex Consensus Conference. Pediatr Neurol 49:243–254
von Ranke FM, Faria IM, Zanetti G et al (2017) Imaging of tuberous sclerosis complex: a pictorial review. Radiol Bras 50:48–54
Davis PE, Filip-Dhima R, Sideridis G et al (2017) Presentation and diagnosis of tuberous sclerosis complex in infants. Pediatrics 140:e20164040
Umeoka S, Koyama T, Miki Y et al (2008) Pictorial review of tuberous sclerosis in various organs. Radiographics 28:e32
Gallagher A, Madan N, Stemmer-Rachamimov A, Thiele EA (2010) Progressive calcified tuber in a young male with tuberous sclerosis complex. Dev Med Child Neurol 52:1062–1065
Martin N, de Broucker T, Cambier J et al (1987) MRI evaluation of tuberous sclerosis. Neuroradiology 29:437–443
Menor F, Martí-Bonmatí L, Mulas F et al (1992) Neuroimaging in tuberous sclerosis: a clinicoradiological evaluation in pediatric patients. Pediatr Radiol 22:485–489
Baron Y, Barkovich AJ (1999) MR imaging of tuberous sclerosis in neonates and young infants. AJNR Am J Neuroradiol 20:907–916
Koh S, Jayakar P, Dunoyer C et al (2000) Epilepsy surgery in children with tuberous sclerosis complex: presurgical evaluation and outcome. Epilepsia 41:1206–1213
Inoue Y, Nemoto Y, Murata R et al (1998) CT and MR imaging of cerebral tuberous sclerosis. Brain Dev 20:209–221
Crino PB, Nathanson KL, Henske EP (2006) The tuberous sclerosis complex. N Engl J Med 355:1345–1356
Hodgson N, Kinori M, Goldbaum MH, Robbins SL (2017) Ophthalmic manifestations of tuberous sclerosis: a review. Clin Exp Ophthalmol 45:81–86
Higueros E, Roe E, Granell E, Baselga E (2017) Sturge-Weber syndrome: a review. Actas Dermosifiliogr 108:407–417
Singh AK, Keenaghan M (2020) Sturge-Weber syndrome. StatPearls Publishing, Treasure Island
Comi AM (2007) Sturge-Weber syndrome and epilepsy: an argument for aggressive seizure management in these patients. Expert Rev Neurother 7:951–956
Akpinar E (2004) The tram-track sign: cortical calcifications. Radiology 231:515–516
Roy U, Panwar A, Mukherjee A, Biswas D (2016) Adult presentation of Dyke-Davidoff-Masson syndrome: a case report. Case Rep Neurol 8:20–26
Frantzen C, Klasson TD, Links TP, Giles RH (1993) Von Hippel-Lindau syndrome. In: Pagon RA, Adam MP, Ardinger HH et al (eds) GeneReviews. University of Washington, Seattle. http://www.ncbi.nlm.nih.gov/books/NBK1463/. Accessed 27 Mar 2020
Maher ER (1994) Von Hippel-Lindau disease. Eur J Cancer 30A:1987–1990
Chittiboina P, Lonser RR (2015) Von Hippel-Lindau disease. Handb Clin Neurol 132:139–156
Lonser RR, Glenn GM, Walther M et al (2003) von Hippel-Lindau disease. Lancet 361:2059–2067
Diaz RC, Amjad EH, Sargent EW et al (2007) Tumors and pseudotumors of the endolymphatic sac. Skull Base 17:379–393
Thalakoti S, Geller T (2015) Basal cell nevus syndrome or Gorlin syndrome. Handb Clin Neurol 132:119–128
Pino LC, Balassiano LK, Sessim M et al (2016) Basal cell nevus syndrome: clinical and molecular review and case report. Int J Dermatol 55:367–375
Kazemi M, Salehi M, Kheirollahi M (2016) Down syndrome: current status, challenges and future perspectives. Int J Mol Cell Med 5:125–133
Annus T, Wilson LR, Acosta-Cabronero J et al (2017) The down syndrome brain in the presence and absence of fibrillar β-amyloidosis. Neurobiol Aging 53:11–19
Ieshima A, Kisa T, Yoshino K et al (1984) A morphometric CT study of Down’s syndrome showing small posterior fossa and calcification of basal ganglia. Neuroradiology 26:493–498
Fink KR, Thapa MM, Ishak GE, Pruthi S (2010) Neuroimaging of pediatric central nervous system cytomegalovirus infection. Radiographics 30:1779–1796
Klase ZA, Khakhina S, Schneider ADB et al (2016) Zika fetal neuropathogenesis: etiology of a viral syndrome. PLoS Negl Trop Dis 10:e0004877
Maldonado YA, Read JS, Committee on Infectious Diseases (2017) Diagnosis, treatment, and prevention of congenital toxoplasmosis in the United States. Pediatrics 139:e20163860
Neuberger I, Garcia J, Meyers ML et al (2018) Imaging of congenital central nervous system infections. Pediatr Radiol 48:513–523
Numazaki K, Fujikawa T (2003) Intracranial calcification with congenital rubella syndrome in a mother with serologic immunity. J Child Neurol 18:296–297
Chantler JK, Davies MA (1987) The effect of antibody on rubella virus infection in human lymphoid cells. J Gen Virol 68:1277–1288
Tien RD, Felsberg GJ, Osumi AK (1993) Herpesvirus infections of the CNS: MR findings. AJR Am J Roentgenol 161:167–176
Noorbehesht B, Enzmann DR, Sullender W et al (1987) Neonatal herpes simplex encephalitis: correlation of clinical and CT findings. Radiology 162:813–819
Petribu NCL, Fernandes ACV, Abath MB et al (2018) Common findings on head computed tomography in neonates with confirmed congenital Zika syndrome. Radiol Bras 51:366–371
Moore CA, Staples JE, Dobyns WB et al (2017) Characterizing the pattern of anomalies in congenital Zika syndrome for pediatric clinicians. JAMA Pediatr 171:288–295
Anderson JL, Levy PT, Leonard KB et al (2014) Congenital lymphocytic choriomeningitis virus: when to consider the diagnosis. J Child Neurol 29:837–842
Deasy NP, Jarosz JM, Cox TC, Hughes E (1999) Congenital varicella syndrome: cranial MRI in a long-term survivor. Neuroradiology 41:205–207
Takayama M (1994) Reactivity of varicella-zoster virus subunit antigens in enzyme-linked immunosorbent assay to sera from varicella, zoster, and herpes simplex virus infections. Med Microbiol Immunol 183:1–11
Cheeran MC-J, Lokensgard JR, Schleiss MR (2009) Neuropathogenesis of congenital cytomegalovirus infection: disease mechanisms and prospects for intervention. Clin Microbiol Rev 22:99–126
van der Knaap MS, Vermeulen G, Barkhof F et al (2004) Pattern of white matter abnormalities at MR imaging: use of polymerase chain reaction testing of Guthrie cards to link pattern with congenital cytomegalovirus infection. Radiology 230:529–536
Barkovich AJ, Lindan CE (1994) Congenital cytomegalovirus infection of the brain: imaging analysis and embryologic considerations. AJNR Am J Neuroradiol 15:703–715
Khan K, Khan W (2018) Congenital toxoplasmosis: an overview of the neurological and ocular manifestations. Parasitol Int 67:715–721
Patel DV, Holfels EM, Vogel NP et al (1996) Resolution of intracranial calcifications in infants with treated congenital toxoplasmosis. Radiology 199:433–440
Karkhah A, Nouri HR, Javanian M et al (2018) Zika virus: epidemiology, clinical aspects, diagnosis, and control of infection. Eur J Clin Microbiol Infect Dis 37:2035–2043
Faria NR, Azevedo RDSDS, Kraemer MUG et al (2016) Zika virus in the Americas: early epidemiological and genetic findings. Science 352:345–349
de Fatima Vasco Aragao M, van der Linden V, Brainer-Lima AM et al (2016) Clinical features and neuroimaging (CT and MRI) findings in presumed Zika virus related congenital infection and microcephaly: retrospective case series study. BMJ 353:i1901
Soares de Oliveira-Szejnfeld P, Levine D, Melo AS et al (2016) Congenital brain abnormalities and Zika virus: what the radiologist can expect to see prenatally and postnatally. Radiology 281:203–218
Van Rie A, Harrington PR, Dow A, Robertson K (2007) Neurologic and neurodevelopmental manifestations of pediatric HIV/AIDS: a global perspective. Eur J Paediatr Neurol 11:1–9
George R, Andronikou S, du Plessis J et al (2009) Central nervous system manifestations of HIV infection in children. Pediatr Radiol 39:575–585
Cantey JB, Sisman J (2015) The etiology of lenticulostriate vasculopathy and the role of congenital infections. Early Hum Dev 91:427–430
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
CME activity This article has been selected as the CME activity for the current month. Please visit the SPR website at www.pedrad.org on the Education page and follow the instructions to complete this CME activity.
Rights and permissions
About this article
Cite this article
Gonçalves, F.G., Caschera, L., Teixeira, S.R. et al. Intracranial calcifications in childhood: Part 1. Pediatr Radiol 50, 1424–1447 (2020). https://doi.org/10.1007/s00247-020-04721-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-020-04721-1