Abstract
Background
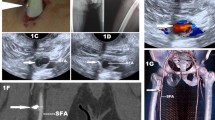
Ballistic injuries with retained foreign bodies from air guns is a relatively common problem, particularly in children and adolescents. If not removed in a timely fashion, the foreign bodies can result in complications, including pain and infection. Diagnostic methods to identify the presence of the foreign body run the entire gamut of radiology, particularly radiography, ultrasound (US) and computed tomography (CT). Removal of the foreign bodies can be performed by primary care, emergency, surgical, and radiologic clinicians, with or without imaging guidance.
Objective
To evaluate the modalities of radiologic detection and the experience of image-guided ballistic foreign body removal related to air gun injuries within the interventional radiology department of a large pediatric hospital.
Materials and methods
A database of more than 1,000 foreign bodies that were removed with imaging guidance by the interventional radiologists at our institution was searched for ballistic foreign bodies from air guns. The location, dimensions, diagnostic modality, duration, complications and imaging modality used for removal were recorded. In addition, the use of sedation and anesthesia required for the procedures was also recorded.
Results
Sixty-one patients with ballistic foreign bodies were identified. All foreign bodies were metallic BBs or pellets. The age of the patients ranged from 5 to 20 years. The initial diagnostic modality to detect the foreign bodies was primarily radiography. The primary modality to assist in removal was US, closely followed by fluoroscopy. For the procedure, 32.7% of the patients required some level of sedation. Only two patients had an active infection at the time of the removal. The foreign bodies were primarily in the soft tissues; however, successful removal was also performed from intraosseous, intraglandular and intratendinous locations. All cases resulted in successful removal without complications.
Conclusion
Image-guided removal of ballistic foreign bodies secondary to air guns is a very effective procedure that can obviate the need for open surgical procedures in children.


Similar content being viewed by others
References
Keller JE, Hindman JW, Kidd JN et al (2004) Air-gun injuries: initial evaluation and resultant morbidity. Am Surg 70:484–490
Shiels WE (2007) Soft tissue foreign bodies: sonographic diagnosis and therapeutic management. Ultrasound Clin 2:669–681
Shiels WE, Babcock DS, Wilson JL, Burch RA (1990) Localization and guided removal of soft-tissue foreign bodies with sonography. AJR Am J Roentgenol 155:1277–1281
Zhu Q, Chen Y, Zeng Q et al (2012) Percutaneous extraction of deeply embedded radiopaque foreign bodies using a less invasive technique under image guidance. J Trauma Acute Care Surg 72:302–305
Shiels WE, Young AS, Murakami JW, Coley BC (2010) Percutaneous image guided soft tissue foreign body removal: a 15-year experience. Abstract, The Radiological Society of North America Scientific Assembly and Annual Meeting, Chicago, IL
Bennett GH, Shiels WE, Young AS et al (2011) Self-embedding behavior: a new primary care challenge. Pediatrics 127:1386–1391
Rabe AJ, Shiels WE (2012) Ultrasound guided removal of an intratendinous foreign body in an adolescent. J Am Osteopath Coll Radiol 1:27–29
Acknowledgements
We would like to thank and recognize Dr. William E. Shiels for his tireless efforts in advancing the medical care of children during his lifetime. This includes his pioneering techniques in image-guided foreign body removal and his leadership role in the data collection for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Rights and permissions
About this article
Cite this article
Rothermund, J.L., Rabe, A.J., Zumberge, N.A. et al. Image-guided percutaneous removal of ballistic foreign bodies secondary to air gun injuries. Pediatr Radiol 48, 120–123 (2018). https://doi.org/10.1007/s00247-017-3977-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-017-3977-8