Abstract
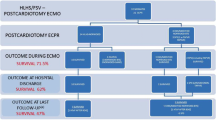
Arrhythmias account for 55 per 100,000 patient evaluations in pediatric emergency departments. Most arrhythmias in children are amenable to medical management or cardioversion. Rarely, arrhythmias lead to significant hemodynamic instability requiring extracorporeal membrane oxygenation (ECMO) support. This study seeks to evaluate children under 1 year of age with a structurally normal heart requiring ECMO for an arrhythmia. This is a retrospective review of the Extracorporeal Life Support Organization Registry. All patients less than 1 year of age between 2009 and 2019 with a diagnosis of arrhythmia and without a diagnosis of structural heart malformation were included. Demographics, clinical characteristics, and outcomes were assessed with descriptive statistics and univariate and multivariable analyses. A total of 140 eligible patients were identified from the dataset. The most common arrhythmia was supraventricular tachycardia (SVT) in 70 (50%) patients. ECMO complications occurred in 106 (76.3%) patients and survival to discharge was achieved in 120 (85.7%) patients. In-hospital mortality was associated with neuromuscular blockade prior to ECMO [aOR 10.0 (95% CI 2.95–41.56), p < 0.001], neurologic ECMO complication [aOR 28.1 (95% CI 6.6–155.1), p < 0.001], and race with white race being protective [aOR 0.13, (95% CI 0.02–0.21), p = 0.002]. Similar survival and complication rates were found in subgroup analysis of SVT arrhythmias alone. Arrhythmias necessitating ECMO support in infants without structural congenital heart disease is a rare occurrence. However, survival to hospital discharge is favorable at greater than 85%. Given the favorable survival, earlier and more aggressive utilization of ECMO may result in improved outcomes.

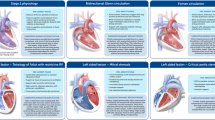
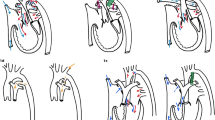
Similar content being viewed by others
Data Availability
With Extracorporeal Life Support Organization (ELSO) Registry approval.
Code Availability
At request.
References
Hanash CR, Crosson JE (2010) Emergency diagnosis and management of pediatric arrhythmias. J Emerg Trauma Shock 3(3):251–260. https://doi.org/10.4103/0974-2700.66525
Ralston MA, Knilans TK, Hannon DW, Daniels SR (1994) Use of adenosine for diagnosis and treatment of tachyarrhythmias in pediatric patients. J Pediatr 124(1):139–143. https://doi.org/10.1016/s0022-3476(94)70270-5
Sherwood MC, Lau KC, Sholler GF (1998) Adenosine in the management of supraventricular tachycardia in children. J Paediatr Child Health 34(1):53–56. https://doi.org/10.1046/j.1440-1754.1998.00153.x
Till J, Shinebourne EA, Rigby ML, Clarke B, Ward DE, Rowland E (1989) Efficacy and safety of adenosine in the treatment of supraventricular tachycardia in infants and children. Br Heart J 62(3):204–211. https://doi.org/10.1136/hrt.62.3.204
Lewis J, Arora G, Tudorascu DL, Hickey RW, Saladino RA, Manole MD (2017) Acute management of refractory and unstable pediatric supraventricular tachycardia. J Pediatr 181:177-182.e2. https://doi.org/10.1016/j.jpeds.2016.10.051
Dyamenahalli U, Tuzcu V, Fontenot E et al (2012) Extracorporeal membrane oxygenation support for intractable primary arrhythmias and complete congenital heart block in newborns and infants: Short-term and medium-term outcomes*. Pediatr Crit Care Med 13(1):47–52. https://doi.org/10.1097/PCC.0b013e3182196cb1
Ghaleb S, Thiagarajan RR, Cooper DS, Czosek RJ (2020) Outcomes of pediatric patients treated with extracorporeal membrane oxygenation for intractable supraventricular arrhythmias. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 21(8):e547–e556. https://doi.org/10.1097/PCC.0000000000002315
Extracorporeal Life Support Organization. ELSO Registry information. http://www.elso.med.umich.edu/Registry.html
R Core Team (2019) R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. https://www.R-project.org/
Bailly DK, Reeder RW, Winder M et al (2019) Development of the pediatric extracorporeal membrane oxygenation prediction model for risk-adjusting mortality. Pediatr Crit Care Med J Soc Crit Care Med World Fed Pediatr Intensive Crit Care Soc 20(5):426–434. https://doi.org/10.1097/PCC.0000000000001882
Sanaiha Y, Khoubian JJ, Williamson CG et al (2020) Trends in mortality and costs of pediatric extracorporeal life support. Pediatrics 146(3):e20193564. https://doi.org/10.1542/peds.2019-3564
Barbaro RP, Paden ML, Guner YS et al (2017) Pediatric extracorporeal life support organization registry international report 2016. ASAIO J Am Soc Artif Intern Organs 1992 63(4):456–463. https://doi.org/10.1097/MAT.0000000000000603
Saharan S, Balaji S (2015) Cardiovascular collapse during amiodarone infusion in a hemodynamically compromised child with refractory supraventricular tachycardia. Ann Pediatr Cardiol 8(1):50. https://doi.org/10.4103/0974-2069.149519
Funding
Not applicable.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declared that they have no conflict of interest.
Ethical Approval
Approval as an Exempt study with waiver of informed consent by the University of Texas at Austin IRB (IRB# 2020-03-0077).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Well, A., Fenrich, A., Shmorhun, D. et al. Arrhythmias Requiring ECMO in Infants Without Structural Congenital Heart Disease. Pediatr Cardiol 43, 914–921 (2022). https://doi.org/10.1007/s00246-021-02803-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-021-02803-x